Coping with Chronic Pain
We have all had pain, admittedly some more than others. (I put that in for the women readers muttering, ‘you men have no idea’). Sometimes it is mild, sometimes it is unbearable. Some are short lived and others chronic. Pain is difficult to explain as it is so subjective. It is also variable depending on the circumstances we are in. People have been known to ignore pain when focused on something else; Footballers have carried on playing with broken bones, Mountain climbers have cut their limbs off to escape when trapped.
What is chronic pain?
Pain is not just hard to define for sufferers, it is equally hard to diagnose and measure for the health professionals. For years we worked on the premise that if you cannot see any obvious cause, then pain must be imaginary. Through research, improving technology and experience, we are now much better at understanding pain than ever before. However, at the frontline, pain management, especially for those with chronic pain, is not consistently good.
Managing long standing pain (anything that lasts longer than 3 months) is based on trust. The Doctor needs to believe the pain. The patient needs to honest about the pain and its impact. The Great British tradition of ‘not moaning’ makes people suffer in silence. I have seen many patients who have never fully discussed their pain, especially when professionals couldn’t find any obvious cause. When you have your first contact with health care, there may be some investigations. When tests do not show a major cause of pain, you are often told, there’s not much ‘wrong’. This makes you go away feeling that you may be suspected of exaggerating. You may also get the same treatment from friends and family as pain is so private.
Even when the cause of the pain is well known, like an old injury, arthritis, cancer, previous surgery etc., we are not very good at getting the right treatment. We may underestimate the level of pain killers needed in these circumstances or worry about addiction and choose not to take it at all, when it is much needed.
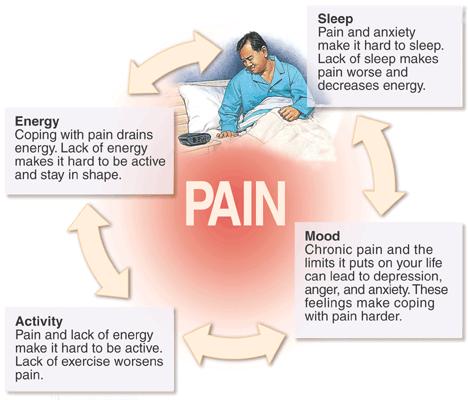
Why is it different?
The trouble with pain is the longer you leave it unsorted, the worse it can get. Sometimes the original problem that caused it may even go away, leaving the pain imprinted in your nerves. The brain and the nerves carrying the pain signals may get stuck in an endless loop, causing low moods, disability and distress. It is hard for the sufferer to know what to do. You may choose to avoid certain movements, leading to further problems. You may take over the counter or prescribed pain medication in copious amounts to try to relieve the pain. Trouble is they only work for a short period, making you take more and more. When you try and stop them, the pain or the perception of it may go worse, making you believe that you may never be off them. This causes a psychological dependence.
There are a variety of ways of managing pain.
Types of Pain
The pain itself has different components, ‘nociceptive’ which is pain from activation of the pain sensors in the tissue and ‘neuropathic’ where the pain is caused by the nerves transmitting the signals. The former can also be ‘surface’ pain from the skin and superficial tissue and ‘deep’ pain coming from muscle, ligaments, bone and in some cases deeper organs.
Managing Chronic Pain
Managing chronic pain is a difficult juggling act. It needs partnership working between the sufferer and the practitioner. Chronic pain is a case where patients exhibit heightened pain sensitivity, increased awareness of bodily symptoms, anxiety, a sense of futility and even depression. Often people may have tried some or more methods listed below in an unstructured and sporadic fashion, leading to poor results and loss of faith. This leads to multiple consultations at various portals, causing a drain for the patient and the health economy.
Multi-disciplinary approach
Chronic pain needs a multi-disciplinary team approach, involving Doctors, Nurses, Physiotherapists, Clinical Psychologists and Occupational therapists. The professionals may use a variety of interventions including drugs to help manage the pain. Before embarking on the treatment plan, it is better to give a good history and undergo a series of assessments including pain scales, mood and function.
Drug Options
The drugs we use to control pain range from simple painkillers such as paracetamol (acetaminophen) to high end drugs such as opioids including morphine & Codeine. The dosage is usually increased gradually till reasonable relief is obtained. The problem is that you may end of taking high doses of pain killers with little real relief but will be unable to stop them as the withdrawal symptoms make matters worse - this is why combination therapy is important.
Anti-inflammatory drugs such as ibuprofen and diclofenac help when tissue inflammation is involved, especially in cases of arthritis and back problems. In case of neuropathic pain drugs such as amitriptyline, pregabalin, Gabapentin and some other anti-epileptics help. Anti-depressants can also be of great value in managing chronic pain. Emerging trends is also to use skin patches to deliver the pain relief so that patients don’t have to ‘clock-watch’ waiting for their next dose.

Therapeutic Options
Massage therapy, Acupuncture, suitable Exercise, Weight management, Cognitive Behaviour Therapy, Hypnosis and TENS machines have all been found beneficial. Swimming, Tai-chi, Yoga can also help by improving posture. These should always be performed under expert guidance and support. Injections of local anaesthetic with a corticosteroid into the affected areas tend to work well in arthritis and inflamed tendons such as tennis elbow, frozen shoulder etc. These are safe and effective when administered by a trained practitioner and can be repeated after an interval. It helps to try a co-ordinated approach to the multiple interventions rather than go from one to another with long gaps in-between.
Holistic Approach
Whether newly diagnosed or established, we need to pay attention to chronic pain with a sense of immediacy due to its devastating effect on the person, their family and the nation’s economy due to disability. An empathetic understanding, shared management plan, involvement of relevant professionals, regular review and continuity of care by familiar faces, access to exercise and other therapies, quick elimination of serious problems will all help to cut short the relentless progression. This will help patients and their families to restore their faith in the Therapist and Therpaeutics.
Copyright © Mohan Kumar 2010