Joint Surgery for Osteoarthritis
Arthritis of the joints affects millions of Americans. As our population ages, this may become even more of a prominent heath issue, as osteoarthritis of the joints becomes more common as we get older. Arthritis causes pain, frustration and a lowered quality of life, so effective therapies are needed to treat this common disorder.
While osteoarthritis (OA) is initially managed with lifestyle changes and medication, sometimes, surgery provides the most realistic hope for a return to function and lifestyle.
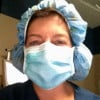
What is Osteoarthritis? Medical Definition.
Arthritis is a general term that means inflammation of a joint or joints. There are several types of arthritis. Joint inflammation is a common feature, but otherwise, they may have little else in common.
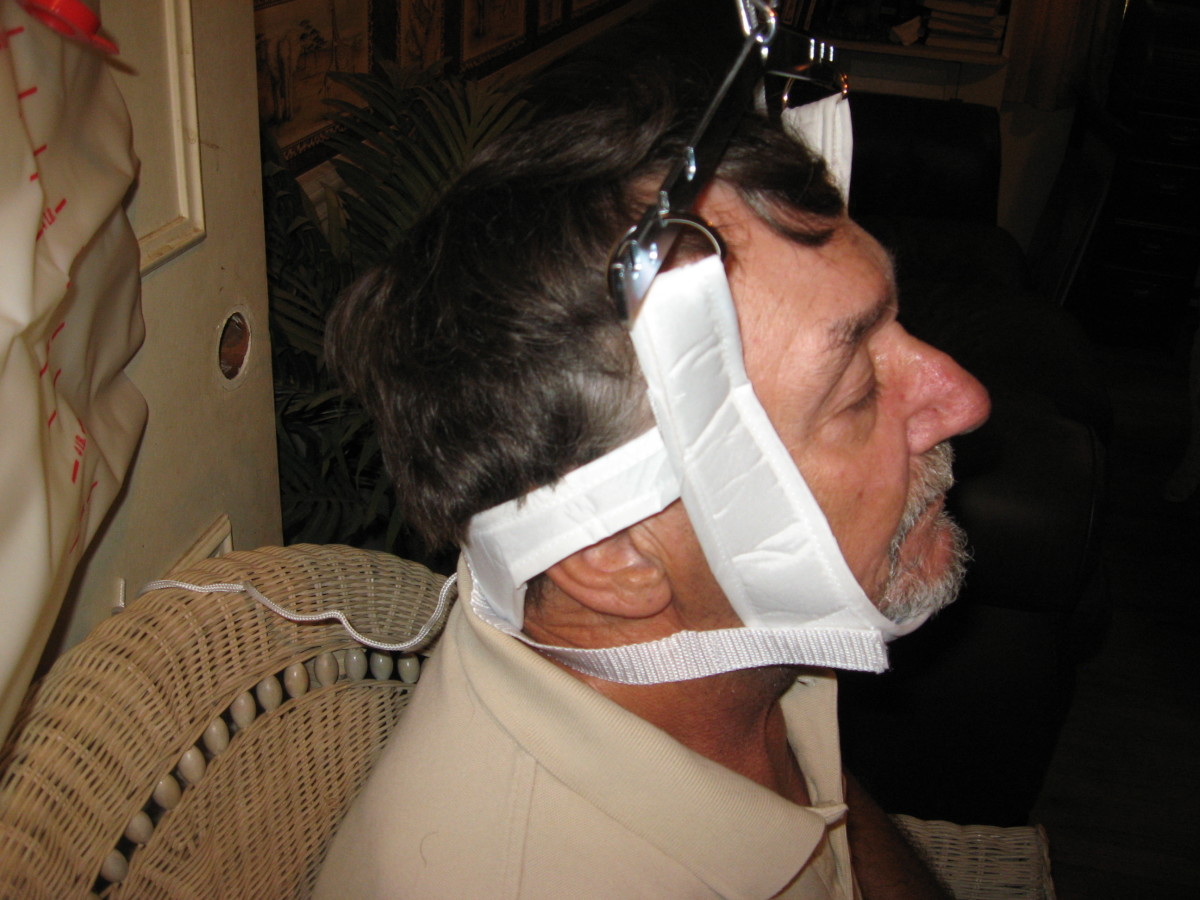
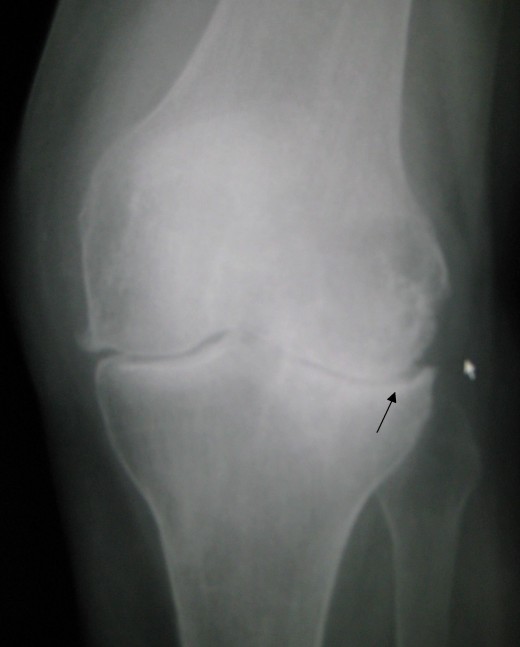
OSTEOARTHRITIS (OA) is a degenerative disease of joints caused by aging. The cartilage between bones in a joint becomes worn down, leading to pain, inflammation and dysfunction. The bones eventually get worn down, too or develop spurs that rub together and cause even more pain and limitation in movement.
Osteoarthritis is also called degenerative arthritis. Degenerative joint disease (DJD) is another term doctors may use to indicate osteoarthritis.
OA is quite different than other types of arthritis such as rheumatoid, gouty or disease-related arthritis is an autoimmune disease that affects the joints and other body parts. OA is generally a disease of aging and overuse, while the other types are related to or caused by other pathologies (such as autoimmune disease).
What is Osteoarthritis?
Have you had joint replacement surgery?
What Type of Doctor Does Surgery for Osteoarthritis?
Most people initially treat their OA symptoms with over-the-counter pain relievers and perhaps some supplements likes glucosamine. Perhaps, if symptoms continue, your primary medical doctor might prescribe a longer-acting or more potent pain reliever. Sometimes, the pain might be severe enough to require a narcotic analgesic. At this point, a referral to a specialist might be in order.
Orthopedic surgeons specialize in treatment of the bones and joints. But, just because you are referred to an orthopedic surgeon doesn't mean you are destined for surgery. There are other options to manage pain and maximize functionality. These include medication regimens, physical therapy and joint injections.
If surgery is recommended, an orthopedic surgeon is the specialist who will help you decide what type of surgery might be beneficial.
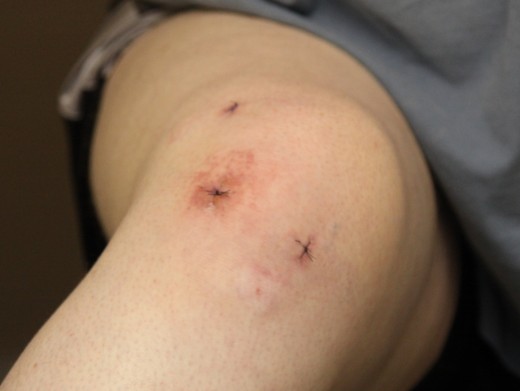
Incision sites after ARTHROSCOPIC surgery on the knee.
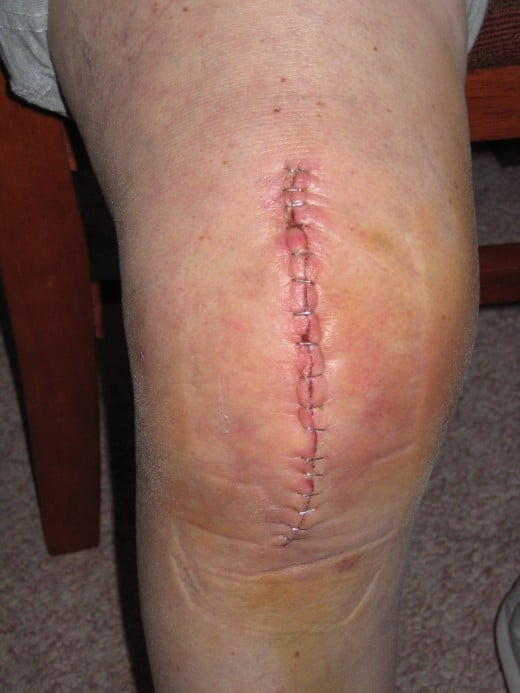
Incision after JOINT REPLACEMENT surgery on the knee.
What Types of Joint Surgery are Done for Arthritis?
Arthroscopic Surgery
Imaging studies like X-rays and MRIs are useful for visualizing the joints and their disorders. Based on your symptoms, the results of the imaging studies and a variety of other factors, your surgeon may or may not recommend surgery. If so, the first surgery done is often an arthroscopy or arthroscopic surgery. This minimally invasive procedure involves inserting cameras and instruments into the joint through small incisions. Not only does the surgeon then get a 'real-time' and accurate view of the joint and its pathology, but minor procedures can be performed at this time. Edges of cartilage that are torn can be trimmed and smoothed, for example.
Joint Replacement Surgery
When all other options have been exhausted and the symptoms of OA are not responding to more conservative therapies, surgery to replace the joint may become necessary. Knees and hips are the most common joints replaced, but shoulders and other joints can also be done.
Joint replacement surgery is a big deal. That said, it can seriously improve the lifestyle and quality of life for those that choose this route (and most patients I've talked to are VERY glad they had the surgery).
Before joint replacement can be done, a full evaluation of the joint and the patient have to be completed. This includes a medical evaluation to make sure that you are ready and healthy enough to undergo such a procedure.
Even though the surgery is limited to a 'peripheral' body part, the surgical trauma and healing process take a toll on the whole body. It is important to be in the best possible shape, physically, mentally and medically before undergoing these operations.
Most of these surgeries take at least a couple hours to complete and are done under general anesthesia (or possibly spinal anesthesia if they are on the lower extremity). Undergoing the surgery is a stress on the body. The heart and lungs, in particular have to work harder to get through the operation, the anesthesia and especially the recovery. Any issues or medical conditions with these or other organ systems should be attended to before surgery to optimize the chances of a smooth operation and recovery. Your primary medical doctor can help with this.
Total Knee Replacement- Excellent Video of the Procedure with Description
Partial and Total Joint Replacement for OA
The joint to be replaced may be worn out on both sides of the joint or just on one side. If just one side is causing most of the problems, a partial joint replacement may be possible. Usually, though, a total joint replacement surgery is needed.
During total joint replacement, and using the knee as an example, parts of both bones that come together to form the joint will be sawed off (yep) and new prostheses will be placed. Various methods are used to secure the new 'parts' in place. The artificial joint is made of special high-grade metals and plastics to allow simulation of a natural joint as closely as possible.