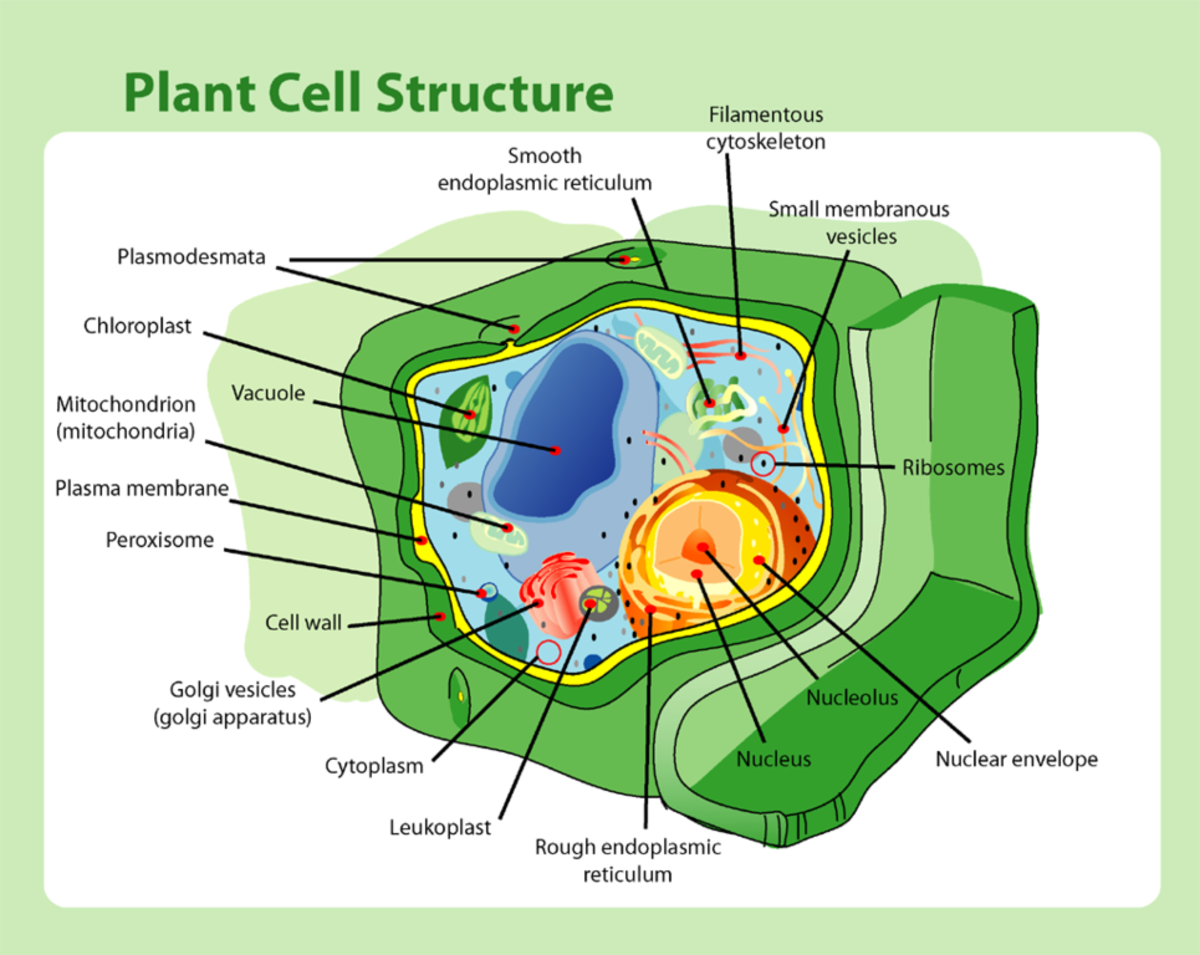
Stem Cells and Blue Light to Treat Motor Neuron Disease or Lou Gehrig's Disease
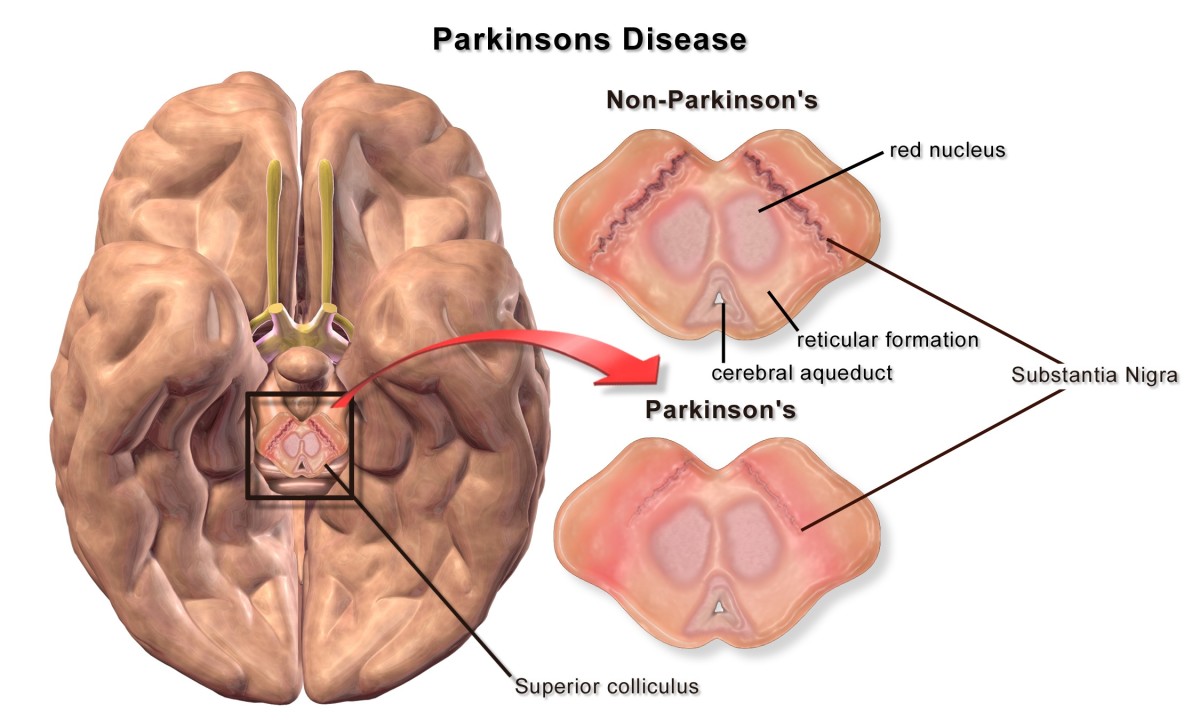
Neurons or nerves
New Hope for those Suffering from Motor Neuron Disease or Lou Gehrig's Disease
Motor neuron disease (also called amyotrophic lateral sclerosis, also called Lou Gehrig’s disease) can be treated with a method that is now being developed.
Lou Gehrig was a baseball player, presumed to be in good health, who died of motor neuron disease.
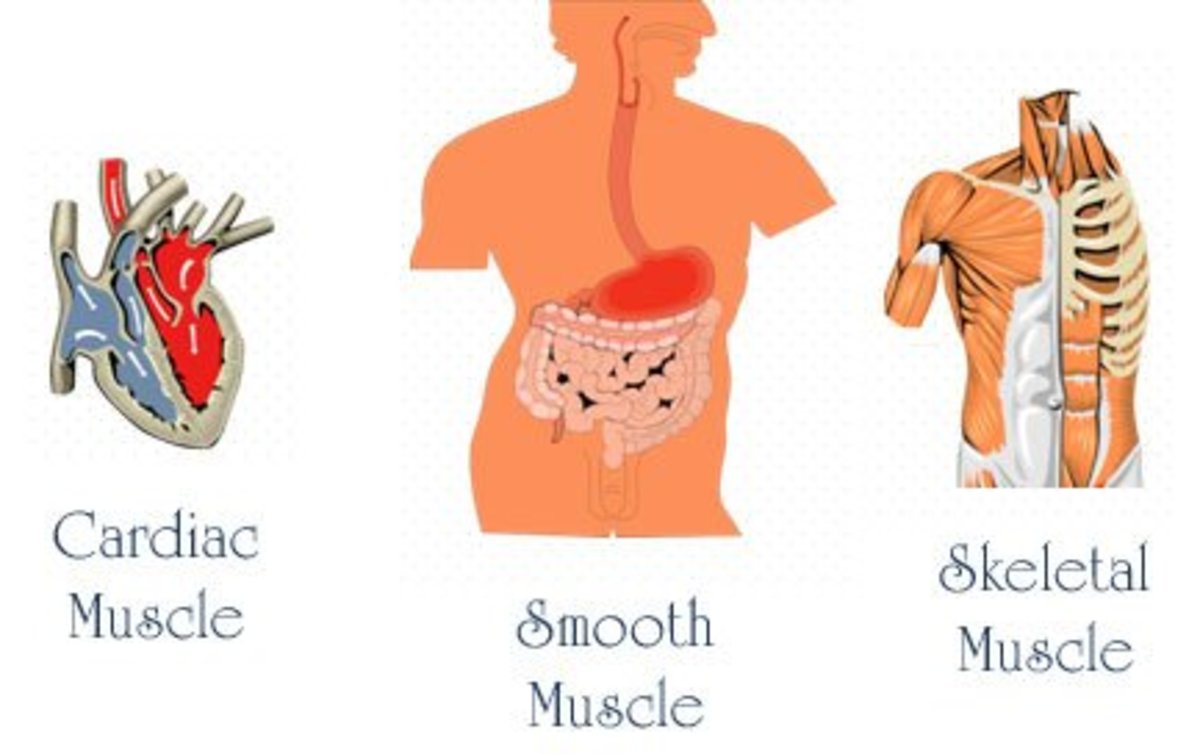
This disease consists of damaged nerves or neurons that control muscles resulting in paralysis. However, the brain remains intact. For lack of use, muscles deteriorate that may graduate into difficulty in speech, and movement. A person so afflicted needs special care and help in eating, drinking and moving to and from the wheelchair to a chair or bed. Brushing the teeth included.
Stem cells are involved in the treatment being developed. These are coaxed into special stem cells then embedded with the capability to sense blue light. Such sensitivity is enabled by providing the special stem cells with a gene that controls them. This is done by recombinant DNA technology.
Special stem cells with blue light sensitivity are then implanted to neurons of the patient suffering from Lou Gehrig’s. The sensitivity to blue light is controlled by a gadget like a heart pacemaker. Intensity, duration and frequency of blue light can be adjusted.
These special stem cells link up with neurons that had been damaged. They will grow along with the damaged neurons treating them in the process. So the functionality of the hitherto damaged neurons is restored.
This technique is being develped by scientists at UCL and King's College London.
"Following the new procedure, we saw previously paralysed leg muscles start to function," according to Professor Linda Greensmith of the MRC Centre for Neuromuscular Diseases at UCL's Institute of Neurology, co-leader of the study. Their report can also be accessed in StemCell101.com.
"This strategy has significant advantages over existing techniques that use electricity to stimulate nerves... if the existing motor neurons are lost due to injury or disease, electrical stimulation of nerves is rendered useless as these too are lost."
Causes of motor neuron disease
It is caused by free radicals and derivatives, reactive oxygen species (ROS), namely: hydroxyl radical.
This ROS mutates the gene Sod1 that controls the function of the enzyme Cu/Zn-SOD or copper/zinc superoxide dismutase. This enzyme protects the membranes of the mitochondria, the energy factory of the body.
Lou Gehrig’s “... progressively causes the degeneration of the nerve cells that control the muscles, paralyzing the body but sparing the mind....” (Swartz H.M. et al. “Free radicals and medicine.” Eaton, S.S. et al. editors. Biomedical EPR-Part A: Free Radicals, Metals, Medicine, and Physiology. 2005:25-74)
.“...The ‘gain-in-function’ of Sod 1 mutants had been postulated to arise from an increased peroxidase or hydroxyl radical activity....” (same source as above, emphasis mine).
Propagation of hydroxyl radical
Its name is a little confusing because of the ‘radical’ appendage. However, it is a ROS because it is derived from free radicals.
A free radical (atomic oxygen, molecular oxygen, ozone, superoxide) is an atom, molecule or fragment of a molecule with an unpaired electron in its outermost orbital. An orbital is a path of electrons spinning around the nucleus. For example, atomic oxygen that has eight electrons. In its second orbital, there are two unpaired electrons. Its outermost orbital is empty that makes it attractive to other elements that is why oxygen can form thousands of compounds.
Superoxide (O2-) is formed by the metabolism of glucose into energy. Note that superoxide consists of two atoms of oxygen with one unpaired electron. An unpaired electron enables superoxide to form a compound with a related molecule. Seen another way, it is destructive because it grabs an electron from another molecule. That grabbing causes an injury that results in mutation.
There are several ways by which hydroxyl radical is produced. When energy from the sun strikes water in the skin it produces hydroxyl radical.
Superoxides reacting with each other in the presence of iron results in hydroxyl radical which is more destructive than superoxide (Sharma, H., MD. Freedom From Disease. 1993).
Development of treatment protocol
Some factors involved in Lou Gehrig’s have been identified: free radicals, hydroxyl radical, neurons, blue light, blue light sensitivity gene, enzyme, mutation, and stem cells.
Free radicals provide the seeds, as it were, for hydroxyl radical. Free radicals and ROS are oxidants. The population of free radicals in the body can be controlled by built-in or native antioxidants like superoxide dismutase and the glutathione enzyme system. Elements of glutathione are found or obtained from plants, except lipoic acid which the body makes anyway. So populations of the offending factors can be mitigated with antioxidants: plants, vegetables, fruits.
Chelation therapy also neutralizes free radicals and ROS. The goal is to reduce their population, balanced with native and supplement antioxidants to prevent oxidation stress. The result is protection of neurons from damage.
If the neurons are not protected the implantation of blue-light sensitive stem cells will turn to naught because neurons are being damaged by free radicals and ROS. It is even possible that the new growth of blue-light sensitive neurons are damaged by hydroxyl radical .
Chelation therapy plays a role as an adjunct in the treatment of motor neuron disease. This therapy has been found safe and effective by the USA National Institutes of Health (HIH). HIH conducted a double blind randomized with control study called "Trials to Assess Chelation Therapy" (TACT). Results were presented at a meeting of the American Heart Association held in Los Angeles, California on November 14,2012.
I discuss TACT in a Hub "USA (National Institutes of Health) Has Announced Chelation Therapy as Safe and Effective."