Clinical Manifestations Of Pericarditis And Pericardial Effusions, Its Complications And Treatments
Pericarditis On Chest X-ray
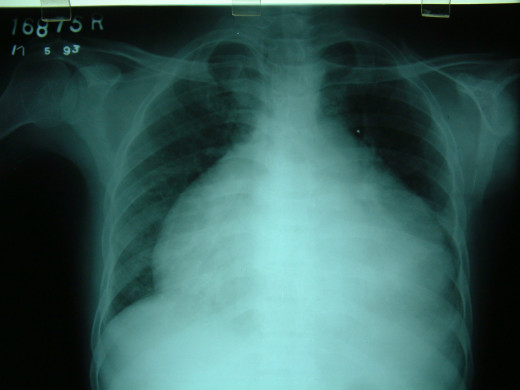
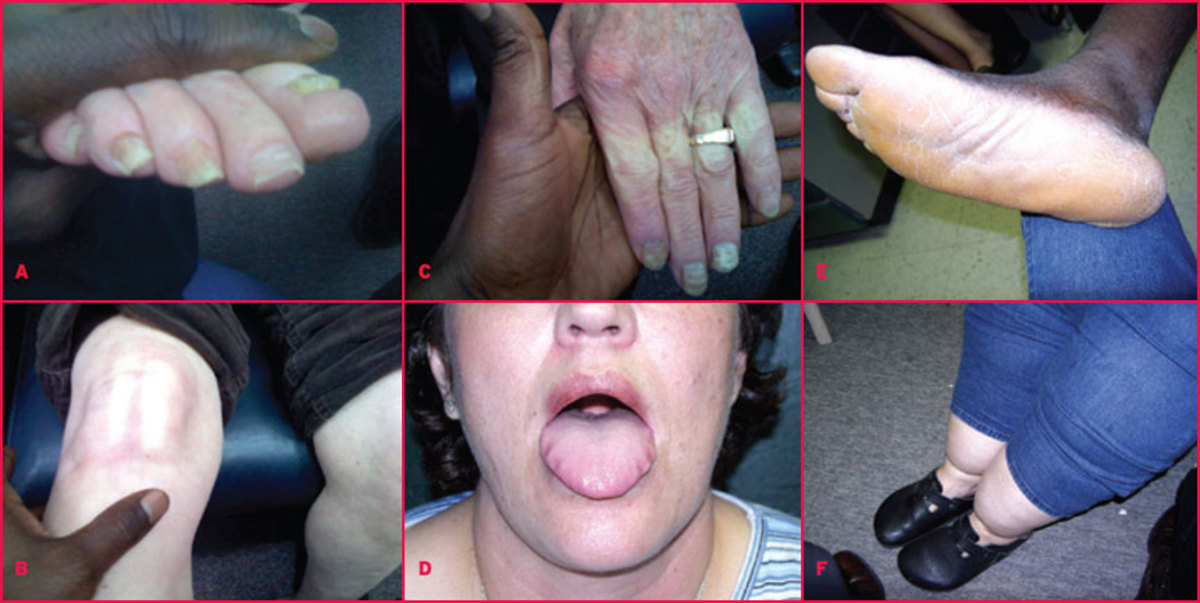
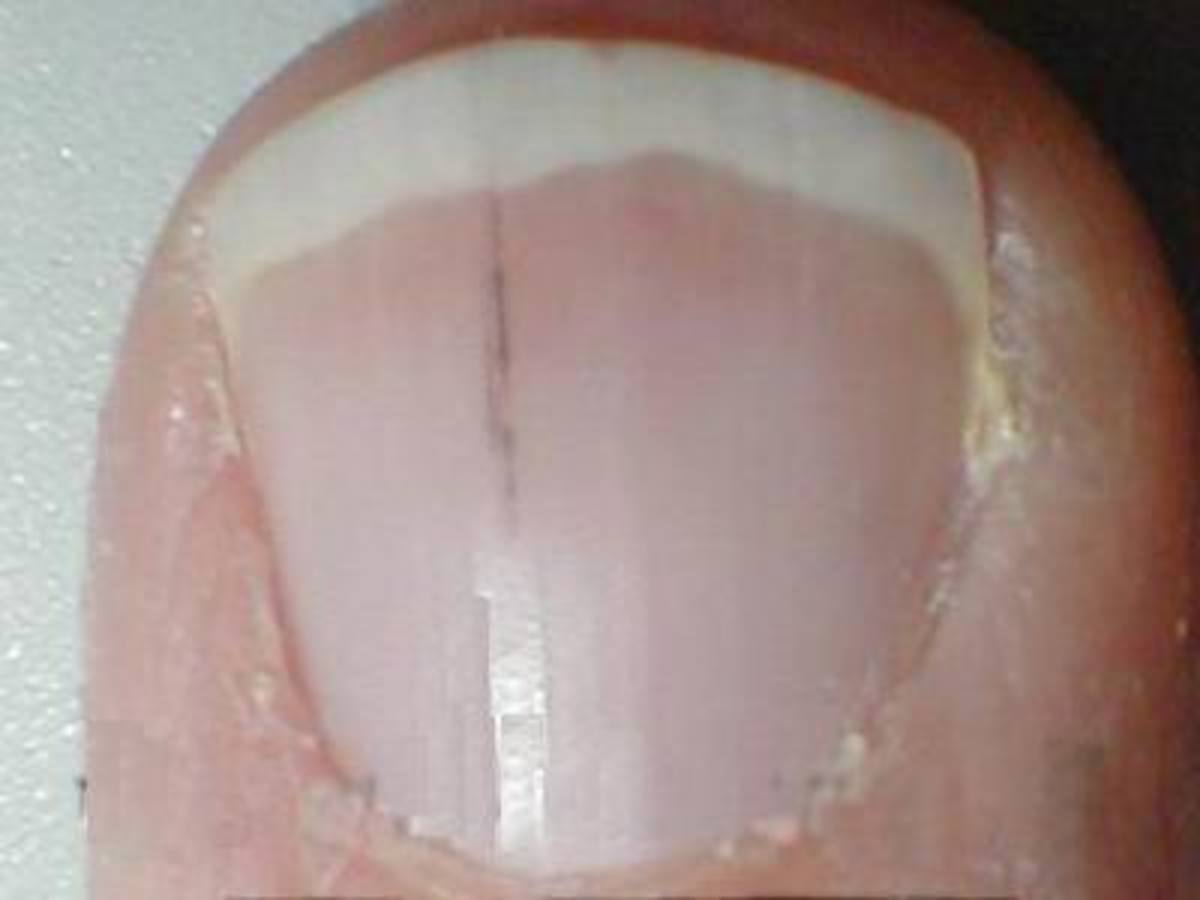
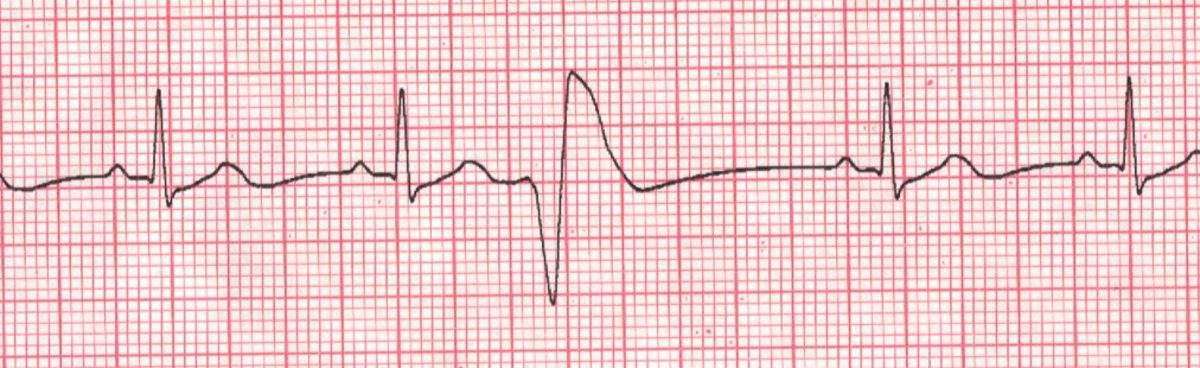
Clinical Manifestation
Inflammation of the pericardium is pericarditis. Pericarditis starts as inflammation of both layers of the pericardium, but soon fluid accumulates in the pericardial cavity, giving rise to pericarditis with effusion.
Clinical features
Acute pericarditis starts off with chest pain felt in the precordium. The pain may be dull or acute and it may be aggravated by deep inspiration, swallowing or movements of the chest. In many cases, there is mild or moderate fever. Auscultation over the upper part of the precordium reveals a pericardial friction rub. The rub is an adventitious sound which is of superficial rubbing quality, heard both during systole and diastole. It is heard better, when the patient is made to sit up, lean forward and the stethoscope is held firm on the chest. Sometimes, the pleura also may be involved and then a pleuropericardial rub is heard. A Pleuropericardial rub increases during inspiration and diminishes during expiration.
Pericardial Effusion And Pulmonary Edema
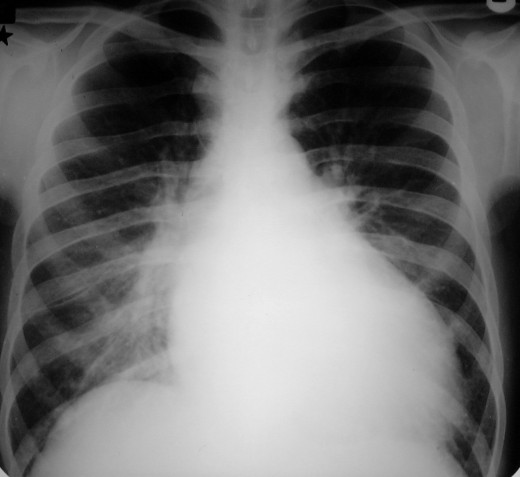
Pericardial Effusion
When fluid accumulates in the pericardium, it causes restriction of cardiac filling during diastole, thereby leading to fall in cardiac output. Right-sided chambers being thinner, are affected more. Gradual effusion produces much less symptoms and the patient may not come up for treatment for several months or even years.
Clinical features
Inspection reveals signs of right-sided heart failure such as engorged jugular vein and dependent edema. The jugular venous pulsations may be weak in severe effusion but in may cases, they show further distension during inspiration (KUSSMAUL’S sign). Sudden diastolic collapse may be seen (Frederick’s Sign). The X and Y descends may be abrupt and prominent.
The apex beat is usually not palpable or only weakly felt. Percussion reveals cardiomegaly. The left border of the heart is made out lateral to the apex beat. The cardiac dullness changes, when percussed in different positions. The pulse is rapid and of low volume. It shows further diminution of volume during inspiration (Paradoxical pulse). Heart sounds are heard feebly, or distantly. Often the pericardial rub disappears when effusion occurs. Pericardial knock which is an additional early diastolic sound may be heard in some cases. Unlike the third heart sound which is low-pitched, pericardial knock is high-pitched.
When accumulation of fluid in the pericardium is rapid, intra-pericardial tension rises abruptly. This leads to gross diminution of ventricular filling, fall in cardiac output and reduction in pulse volume and pulse pressure.. In severe cases, shock supervenes. These constitute cardiac tamponade.
Treating Complications Of Pericarditis
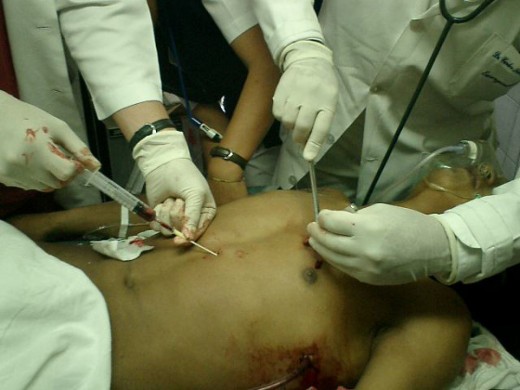
Treatment
When the pericardium is the seat of chronic inflammatory processes, it undergoes fibrosis and calcification.
Complications include cardiac tamponade, constrictive pericarditis, cardiac cirrhosis and atrial fibrillation. Acute pericarditis generally subsides. The prognosis depends upon the cause. Cardiac tamponade may be fatal, if unrecognized in time. Timely diagnosis and relief by pericardial effusion and constrictive pericarditis run a protracted course over several years, leading to chronic right-sided heart failure and cardiac cirrhosis and finally ending in death.
Treatment
Acute Pericarditis: Symptomatic measures include analgesics, antipyretics and sedatives. Viral pericarditis and those complicating myocardial infarction, pneumonia and pleurisy subside uneventfully when the underlying condition is treated. Tuberculous pericarditis should be treated with antituberculosis drugs. Early treatment leads to complete resolution. Addition of prednisolone 20-40 mg/day in the initial phases of therapy accelerates resolution and probably prevents delayed complications. Uremic pericarditis subsides with dialysis or renal transplantation when the blood urea levels are brought down. In predialysis days, uremic pericarditis was considered to be a terminal phenomenon portending death.
Pericardiocentesis
Pericardiocentesis
Aspiration of the pericardium is done for diagnostic purposes, to examine the fluid or therapeutically to relieve the tension and to hasten resolution. Sites of aspiration are:
- Fourth left intercostals space 2.5cm from the sternum;
- Between the cardiac apex and left border of the heart made out by percussion; and
- Transdiaphragmatically through the epigastrium.
The last one is preferable on account of its safety. Complications of aspiration include shock, arrhythmias, injury to the myocardium and coronary vessels, and bleeding into the pericardium. If cardiac tamponade develops, emergency aspiration or pericardiotomy may have to be done. Pericardial aspiration should be done only in centers properly equipped for cardiac resuscitation.
Constrictive pericarditis is not amenable to medical therapy. Surgical treatment (pericardiectomy) is done to relieve the constriction. This surgery carries a significant mortality.
Adherent Pericarditis
This is the condition where the two layers of the pericardium become adherent and this may extend to extracardiac tissues. Systolic retraction of the left side and back of the chest wall occurring in this condition is called “Broadbent’s sign”.
If not treated with all seriousness, Pericarditis can prove fatal.
© 2014 Funom Theophilus Makama