- HubPages»
- Health»
- Diseases, Disorders & Conditions»
- Chronic Pain
Clinical Significance Of The Diagnosis And Treatment Of Hypoparathyroidism
Hypothyroidism
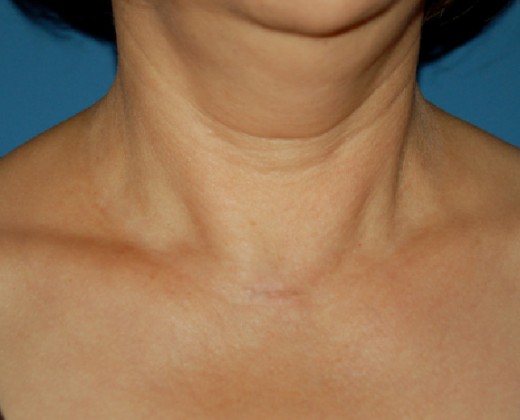
Diagnosis
Presence of hypocalcemia with hyperphosphatemia should arouse suspicion of hypoparathyroidism, if renal disease can be excluded.. Other causes of hypocalcemia are rickets, malabsorption states, hypoproteinemia, acute pancreatitis and extreme dietary deficiency of calcium. The total serum calcium is low in hypoproteinemia since the fraction bound to albumin and globulin is reduced, even though the ionized calcium is kept normal. Tetany does not occur in this condition. In acute pancreatitis transient hypocalcemia develops which is self-limiting. In rickets and osteomalacia, both calcium and phosphorus are low. Diagnosis of hypoparathyroidism can be confirmed by demonstrating low levels or absence of PTH. The response to therapeautic administration of PTH is dramatic.
Pseudohypoparathydoidism should be suspected if there is a family history of skeletal disorders and also presence of other abnormalities like dwarfism. Moniliasis and metastatic calcification are uncommon in pseudohypoparathyroidism.
Hypocalcemic tetany has to be differentiated from alkalosis and tetany occurring in hypokalemia and hypomagnesemia. When serum magnesium falls below 0.8 meq/liter, PTH secretion is depressed and this leads to secondary hypoparathyroidism. Parenteral replacement of magnesium restores parathyroid function.
Pseudopseudohypoparathyroidism
Some of the relatives of subjects with pseudohypoparathyroidism show skeletal changes, but none of the biochemical abnormalities of hypoparathyroidism. This condition is called pseudopseudohypoparathyroidism.
Treatment: Aim of treatment is to normalize serum calcium levels without increasing urinary loss. Though correction of hypocalcemia is easy, in the absence of PTH, considerably large amounts of calcium are lost in urine. Therefore even with low-normal levels of serum calcium, nephrolithiasis may develop. Intestinal absorption of calcium can be enhanced by the administration of vitamin D. This corrects hypocalcemia, but not the other metabolic abnormalities. It is desirable to keep serum calcium levels between 8.5 and 9 mg/dl by adjusting the dose of vitamin D. Several preparations are available, Vitamin D2 50,000 to 100,000 U/day or I-alpha OHD3 (1-2 ug) daily helps in improving serum calcium level. Result of vitamin D therapy is not always predictable since individual variations are common. Vitamin D preparations take a few weeks to exert their full effect. Loss of control may develop even after long periods of satisfactory control. Along with vitamin D, approximately 1.0g of elemental calcium should be provided in the diet (2.5g calcium carbonate, 3.0g calcium chloride, 8g calcium lactate or 11g of calcium gluconate). Hypomagnesemia confers resistance to vitamin D which clears up on supplementation of magnesium orally or parenterally.
Carpopedal Spasm
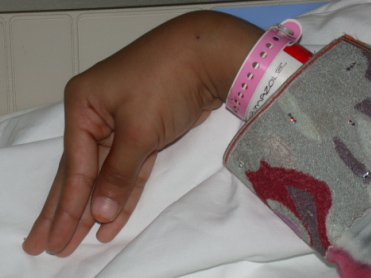
Treatment of tetany
Slow intravenous injection of 20ml of 10% calcium gluconate solution promptly relieves tetany. The relief is maintained by giving an intravenous drip containing calcium gluconate 15 mg/Kg body weight. Though intravenous calcium is generally safe, in subjects receiving digitalis thereapy, it may precipitate fatal arrhythmias like ventricular fibrillation.
In hysterical subjects who hyperventilate, alkalotic tetany may develop. This can be prevented by the inhalation of 5% carbondioxide or rebreathing into the same bag. For tetany due to metabolic alkalosis infusion of isotonic saline is the most effective measure. In alkalosis produced by the excessive administration of alkalis, relief is obtained by giving ammonium chloride orally in a dose of 2g, 6 hours.
Rugger Jersey Spine
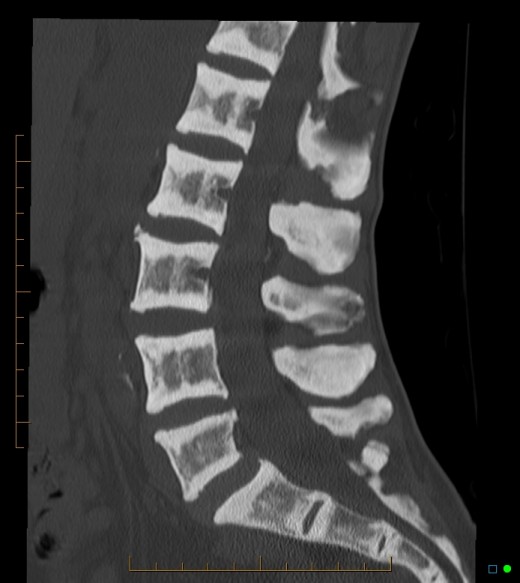
Abnormalities in the skeleton in chronic renal failure
Chronic failure gives rise to:
- Marked impairment in intestinal absorption of calcium
- Secondary hyperparathyroidism
- Progressive bone disease, and
- Soft tissue calcification.
The bony changes include osteomalacia, osteitis fibrosa, diffuse osteopenia and osteosclerosis. When the value of CaXP product is low, the tendency is to develop osteomalacia. Radiological features are subperiosteal erosions, fractures and calcification around joints and blood vessesl. The phalanges of the hands and feet, clavicles, skull, long bones and ribs show diagnostic abnormalities. Sometimes, brown tumours and marked periosteal bone formation may be seen. Osteosclerosis may develop commonly in longstanding renal failure. Horizontal bands of increased bone density develop in the vertebrae and this is known as “rugger jersey” sign. The body abnormalities of renal failure are generally resistant to therapy with vitamin D and dialysis.
© 2014 Funom Theophilus Makama