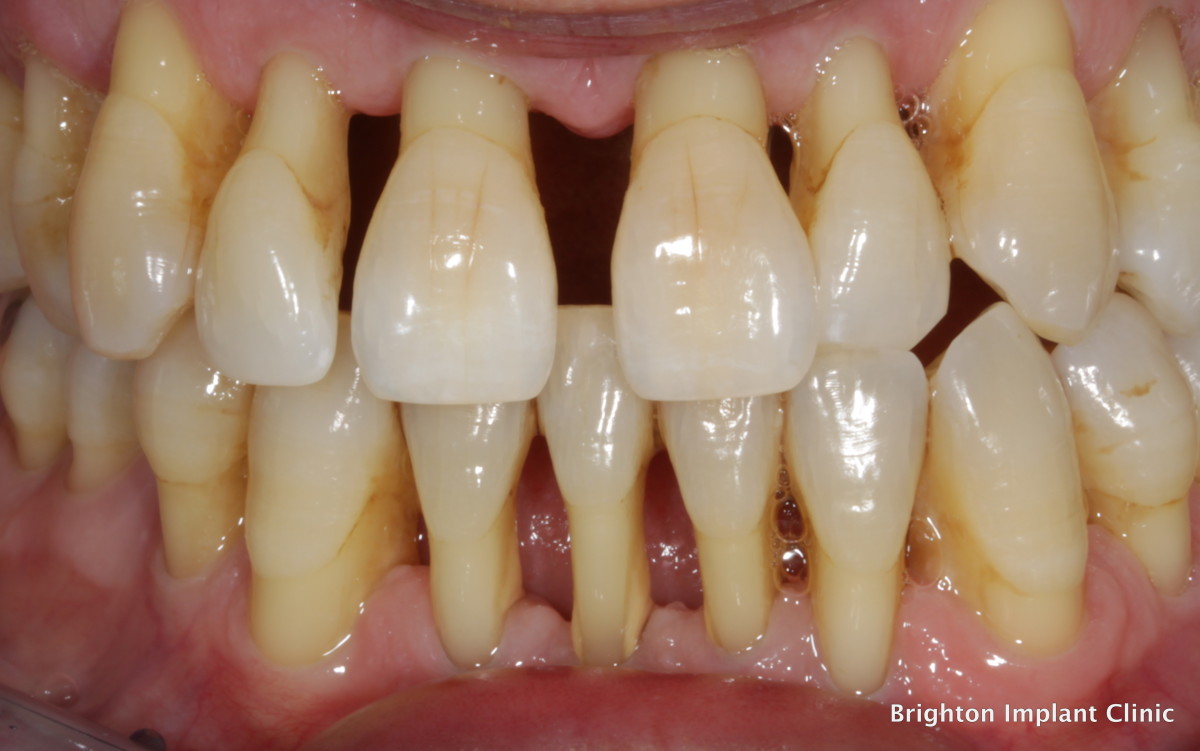
Complications after a tooth extraction

Why Become Aware of Tooth Extraction Complications?
As if getting a tooth extracted wasn't fun enough, complications after a tooth extraction is what many of us fear the most. Awareness of possible complications though can be helpful so you know what to expect and you can be prepared to face them. Your dentist most likely went over some of them or handed you a discharge paper with post-op instructions, but there may not be enough clarity about what exactly may be happening and why you should seek out help as soon as you can. This article will point out some common and not-so-common complications after a tooth extraction and what exactly causes them so you can have a better grasp on the process. Fortunately, in most cases, tooth extractions are uneventful, courtesy of our effort in following post-op instructions and the work of our amazing immune system which we often take for granted.
More Common tooth extraction complications
Despite modern advances in the dental industry, tooth extractions are still quite traumatic to tissues. Yes, these procedures are painless courtesy of the marvels of local anesthesia, but we must admit they sill involve quite an amount of pressure and damage to tissues, even though temporary. Until a magical potion is invented that makes the tooth just fall out on its own, we will need to deal with a certain level of soreness and pain in the days following the procedure. Luckily, these are normal, short-lived symptoms which can be dealt with by using pain relievers and will quickly become a memory of the past, but in some cases, tooth extraction complications can leave quite a mark. Following are some of the more common tooth extraction complications.
Bleeding excessively. Luckily, this can be easily prevented by following the many tips found in your post-op instructions. However, sometimes despite your efforts, the bleeding may be reluctant to subside. It's important to call your dentist if the bleeding appears to be excessive or prolonged. If the office is closed don't hesitate to go to the ER. Serious bleeding problems can be caused by underlying bleeding disorders or taking certain drugs that interfere with proper clotting. For more on what to do to prevent bleeding excessively and potential causes my previous article on bleeding after extractions may be helpful. Skip the first paragraphs if you are squeamish, hypochondriac or get easily anxious.
Infections. It may sound ironic how you may be pulling a tooth to prevent it from becoming infected and then you get an infection from its extraction. The truth is, anytime you are undergoing any form of surgery as little as an extraction or as big as an amputation, there are risks for bacteria to set in and cause infections. Consider though that the mouth is a place highly populated with bacteria, and that infections are quite common. Dentists may take preventive measures and prescribe antibiotics to prevent infections right after the extraction, especially in the case of surgical extractions. Generally, the first signs of an infection show up about 48 hours after the extraction. The area may appear swollen, painful and bleeding may resume.
Dry sockets. The dreaded dry socket tends to happen a few days after the extraction. The patient seemed to be doing fine when suddenly there's a surge in pain and there may be a bad taste in the mouth. The pain which was supposed to subside by the second day, instead at times can get quite excruciating, but it may be reassuring to know that while painful, a dry sockets isn't life threatening as excessive bleeding or an infection. While preventive measures may be taken to prevent its occurrence, some times no matter what it has to happen. There appears to be some evidence that women on birth control pills are more likely to get a dry socket according to Dr. Dan Peterson. Other contributing factors are smoking, sneezing, coughing, sucking from a straw or spitting in the first 24 hours after the extraction.
But what exactly is a dry socket? The socket is the hollow area remaining after the tooth has been extracted. When normal healing occurs, a blood clot forms that protects the bone and nerve endings helping the area recover. When the blood clot dislodges though, the bare bone and nerve endings are exposed to air, food and water causing pain. It typically occurs about two days or more after an extraction and may last up to 5 to 6 days. Fortunately, the dry socket resolves on its own with time, but recovery at times may be slow. According to Dr. Martin S. Spiller, studies have shown how rinsing with 0.12% chlorhexidine (Peridex) could help reduces the occurrence of dry sockets.
Swelling and Bruising. This is quite expected especially in the case of surgical extractions when gums must be cut or the bone must be drilled. In a normal situation, the swelling deriving from tissue trauma reaches a peak around the first 24 to 48 hours post extraction and then subsides afterward, according to Animated Teeth. When the swelling is prolonged or excessive and is accompanied by pain, this may indicative of an infection. Bruising is often seen in the elderly or people taking aspirin or steroids. It may take some time for it to disappear.
Excessive Pain. In normal cases, the pain is more intense in the first 24 to 48 hours and then subsides. Generally, pain meds work well to control it. Excessively severe pain or prolonged pain may be a sign of a complication such as an infection or dry socket.

More about extractions
- Can you bleed to death from a pulled tooth?
Those who fear dental procedures often have irrational fears that come to their mind. Bleeding to death from a pulled tooth is a common fear for many. Can this really happen? what are the odds? - What's the difference between simple extraction and ...
Simple extraction vs. surgical extraction, what's the difference? How can you tell the two apart and why do dentists use these two terms?
Less common tooth extraction complications
And then we have some not-so-common tooth extraction complications. While quite uncommon, it's not a bad idea to be aware of them--just in case.
Sinus perforation. It's a fact that the root of the upper back teeth tend to be close to the sinuses. A thin wall separates the two (the sniderian membrane), but in some cases, an extraction may cause the thin wall to perforate causing the mouth to communicate with sinus. Usually, dentists notice the close relation between the roots and the sinuses and will make patients aware of this risk. In small perforations, a nose bleed may be the only symptom. Fortunately, the perforation should heal as the blood clot forms. Patients will this complication will often be treated with "gelfoam" and will have prescribed an antibiotic and decongestant.
Broken jaws. In most of these cases, the dentist is not at fault. Broken jaws can happen when the bone has become excessively fragile and cannot put up with the pressure applied to extract the tooth. In most cases, the dentist will notice this on the x-ray and will make the patient aware of this potential risk. Extractions in these people aren't the only risks posed, they may as well easily fracture their jaw in a car accident or sport event.
Trismus. Also known as lockjaw, this condition causes a temporary reduced ability to open the mouth. In a dental setting, this can be caused by keeping the mouth open for too long or simply inflammation to the mastication muscles, the presence of TMJ can be a factor,. It usually occurs in extraction of lower teeth. Fortunately, its temporary and can be alleviated by following the dentist's advice.
Nerve damage. This is most common in wisdom tooth extractions It happens when nerve lies in close proximity to the wisdom tooth being extracted. What happens is that the nerve risks getting bruised or damaged. The most vulnerable nerves involved in wisdom tooth extractions are the mandibular and lingual nerves. Affected patients will feel loss of sensation on the lip, cheek or tongue areas as if there were still numbed up. Luckily, with time the area returns normal within a few days, however in rare cases it may last much longer than that and may be permanent in some cases.
Swallowing or inhaling the tooth. This is thankfully rare. The extracted tooth may slip out of the forceps and may be swallowed or inhaled by the patient. If swallowed, the patient may cough, but once it makes it down the digestive tract it usually passes uneventfully. If inhaled, emergency surgery may needed to remove the tooth from the airway or lung to prevent aspiration pneumonia or an abscess.
Bone fragments. Also known as sequestrii, these are bone fragments that are expelled weeks after the extraction and patients often believe them to pieces of tooth. These fragments are expelled by the socket in a process called "sequestration." The patient may be painful and sometimes may require the dentist to remove it when it's not expelled spontaneously.
Retained roots. We all wished teeth with all their roots would come out all in one piece and quickly, but sometimes things may get a bit complicated. When a tooth breaks in pieces, root fragments may be left behind. These can be removed by the dentists, but at times the root fragment may be strongly attached to the bone they may be very difficult to remove. At other times, they may be too close to nerves and sinuses that it isn't worth risking. The good thing is that in many cases root fragments left behind do not pose any particular problems and heal. And should the retained root fragment create problems years down the road, the socket will try to eject it and it would have loosened from the bone allowing an easier retrieval for the oral surgeon.