Cor Pulmonale: Its Pathophysiology And Clinical Pathology
Cor Pulmonale In A Child
Introduction
The cardiovascular changes occurring as a result of primary disease in the lung parenchyma or the pulmonary vasculature are included under this term. Cor Pulmonale may be acute or chronic.
Acute Cor Pulmonale is the result of sudden rise of pulmonary artery pressure occurring in pulmonary embolism and this leads to right-sided heart failure or shock.
Chronic Cor Pulmonale is defined as the occurrence of hypertrophy and dilatation of the right ventricle resulting from pulmonary hypertension, which occurs as a consequence of disases of the pulmonary parenchyma and/or the blood vessels between the origin of the pulmonary artery and the termination of the pulmonary veins.
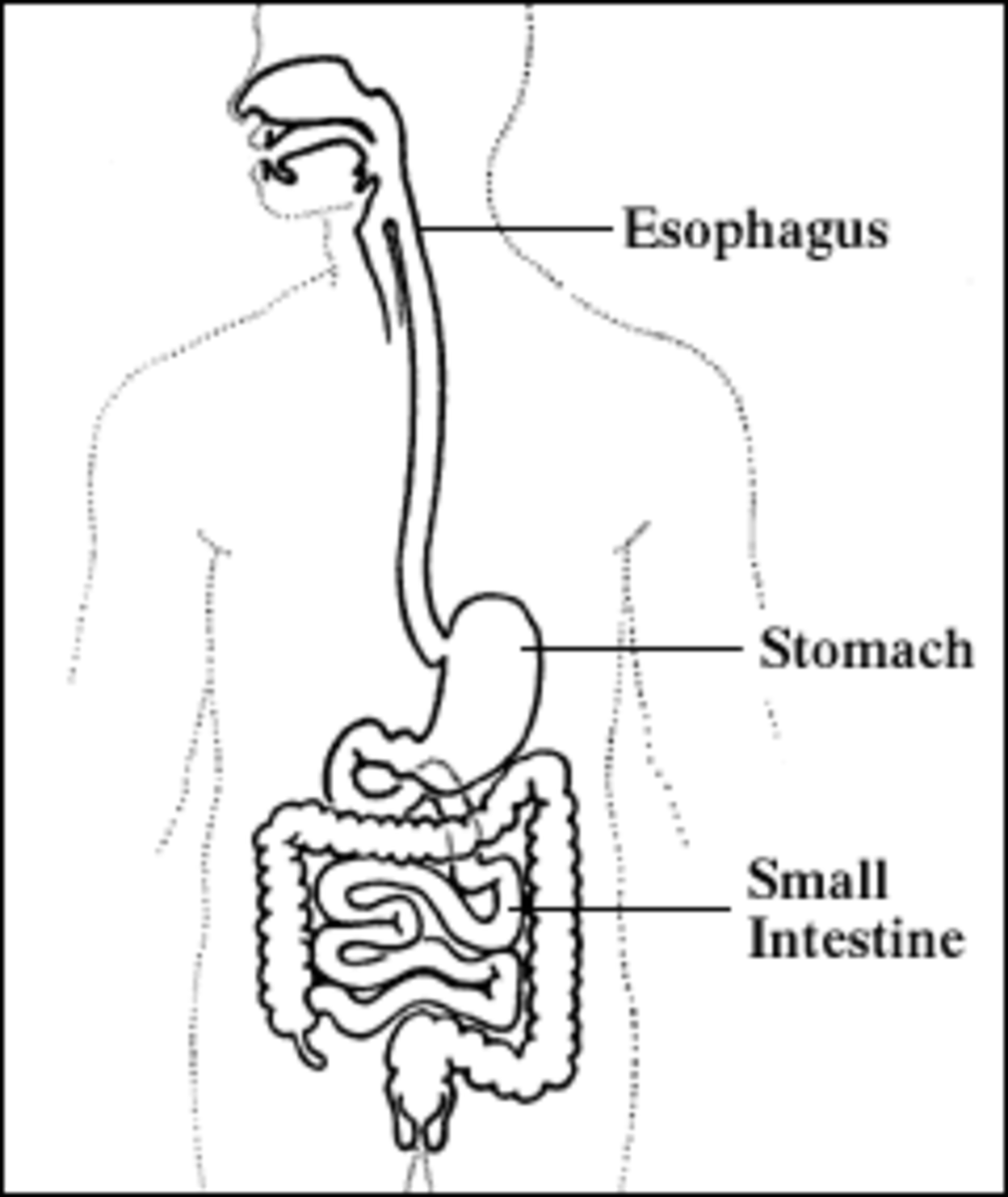
Normally, the lung is perfused by the pulmonary arteries at a low pressure (10-20mm Hg), this circulation serving the function of gas exchange. The bronchial arteries arising from the aorta supplies blood at systemic arterial pressure and supplies blood to the lung parenchyma and air passages. Normally, these two systems do not communicate directly.
Cor Pulmonary Is A Serious Clinical Issue

Pathophysiology
Pulmonary arterial tension increases when more than 50-60% of the vascular bed is obliterated. Obliteration of the pulmonary vasculature results from several causes:
- Progressive destruction of pulmonary capillaries occurs along with destruction of pulmonary parenchyma in emphysema, bronchiectasis, diffuse interstitial fibrosis and pneumoconiosis.
- Hypoxia and acidosis leads to generalized pulmonary vasoconstriction and this leads to rapid rise of pulmonary tensions.
- Persistent pulmonary hypertension arising from any cause leads to further changes in the vessels such as edema, intimal thickening, smooth muscle hypertrophy and fibrosis. All these tend to narrow the lumen further.
- Repeated minor pulmonary embolism, vasculitis and other primary disease processes occurring in the vessels (as primary pulmonary hypertension) progressively reduce the pulmonary vascular bed.
Clinical Cardiology
Pathology
As a result of factors which clinically elevate pulmonary arterial tension, the right ventricle dilates and hypertrophies. Any sudden rise in pulmonary tension resulting from factors like hypoxia tip the patient into right ventricular failure.
Chronic hypoxia gives rise to secondary polycythemia and increase in the viscosity of the blood. Peripheral vasodilatiation results from retention of carbondioxide and workload of the heart increase due to increased viscosity of blood and peripheral vasodilatation. A high output cardiac failure sets in. Severe chronic hypoxia and hypoxemia lead to dysfunction of the left ventricle as well.
© 2014 Funom Theophilus Makama