Dermatomyositis: Clinical Significance, Pathology, Clinical Presentations, Diagnosis And Management
Dermatomyositis
A General Overview
Dermatomyositis is the least common among the connective tissue disorders. It consists of inflammatory and degenerative lesions involving the striated muscle, skin and other connective tissues in varying combinations. The clinical types are:
Type I: Typical polymyositis
Type II: Typical dermatomyositis
Type III: Dermatomyositis associated with malignancy
Type IV: Childhood dermatomyositis
Type V: Dermatomyositis or polymyositis associated with other collagen diseases as part of an overlap syndrome.
Pathology: The muscles show fragmentation, loss of cross striation, cellular infiltration of interstitial connective tissue, increase in sarcolemmal nuclei and rarely calcification. Perivascular inflammatory changes are present. Skin shows swelling and edema of dermal collage, atrophy of epidermis and flattening of rete pegs.
Clinical Features
Dermatomyositis is more common in the second, fifth and sixth decades. Women are more affected than men. A wide spectrum of clinical severity ranging from an acute, extensive rapidly fatal paralytic syndrome to a very slowly progressive muscle disease closely resembling a muscular dystrophy may be seen. Proximal muscles are affected more than others in the early stages. Muscle tenderness is prominent in the acute stage. Eventually, fibrosis and contractures occur. The muscles are hyporeflexic. Though in a third, the esophageal and pharyngeal muscles are affected, the ocular muscles are spared. Muscle enzymes are increased. The EMG shows myopathic pattern.
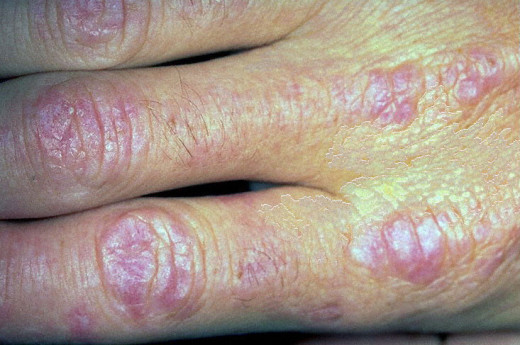
The diagnostic skin lesion is a heliotrope eruption on the face associated with periorbital edema. Skin lesions may precede, coexist or follow the muscular involvement. Cutaneous lesions may ulcerated and leave behind depressed scars. Subcutaneous and periarticular calcification may be seen. Around 35% of cases show a non-erosive arthritis.
Physical Presentations
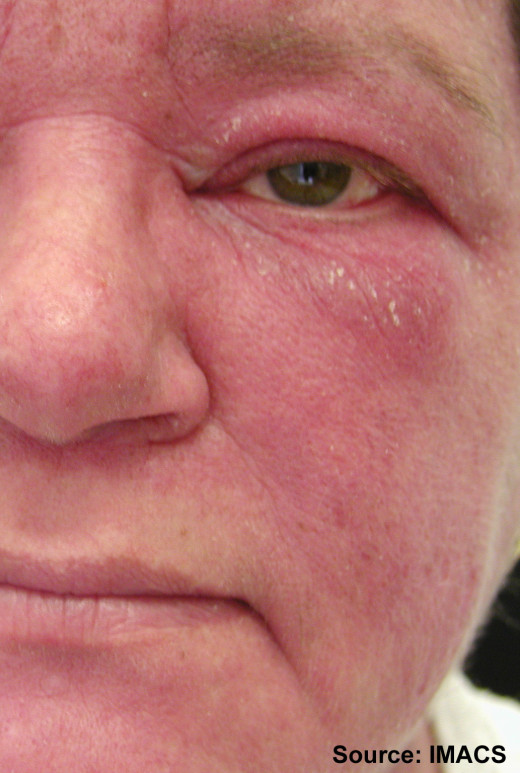
Dermatomyositis
Diagnosis And Management
Diagnosis: The diagnosis is made on clinical grounds, electromyography, raised levels of creatine phosphokinase, aldolase, SGOT and lactic dehydrogenase and muscle biosy. Rheumatoid factor is present in many cases and antinuclear factor in 30%.
The course is variable. In some, it is rapidly progressive and fatal due to cardia, renal or pulmonary complications. Many follow a slowly progressive course extending over 10-25 years leading to muscle weakness, contractures, and deformities. Spontaneous remission is seen in some cases. In the course of other connective tissue disorders like rheumatic fever, rheumatoid disease, sjogren’s syndrome, scleroderma or lupus erythematosus, a picture of dermatomyositis may occur. In such cases, the occurrence of muscle weakness out of proportion to the primary condition should suggest the possibility of superadded dermatomyositis.
Management: Prednisolone in a degree of 1- 2 mg/Kg/day to start with and subsequently tapered off is effective in the majority of cases. Immunosuppressive agents are indicated when the response to corticosteroids is unsatisfactory. Physiotherapy is indicated to prevent disuse atrophy and contractures.
Since dermatomyositis may occur as a paraneoplastic phenomenon, an underlying malignancy should be excluded in all cases. The usual primaries are the breasts, lungs, ovaries, prostate and stomach. Removal of the tumour brings about remission.
© 2014 Funom Theophilus Makama