Diabetes Mellitus: Clinical Relevance In The Complications Of Insulin Therapy And Their Management (Hypoglycemia)
Upgoing Plantar Responses: Effect Of Insulin Overdose
Clinical Presentation
The major complication of Insulin therapy is over- administration, leading to decrease level of blood glucose. This situation is known as hypoglycemia.
Hypoglycemia: This occurs under the following circumstances:
- Excessive dosage of insulin
- Reduction in food intake
- Vomiting or diarrhea
- Unaccustomed exercise
- Concurrent administration of drugs like chloropropamide
The onset of symptoms depends on the type of insulin and the dose. In general, the onset of hypoglycemia coincides with the duration of peak action.
Clinical Manifestations
The onset is abrupt with a sense of anxiety, feeling of emptiness in the epigastrium, sweating and palpitation. As the condition progresses, the patient may become comatose and convulsive. Examination reveals cold clammy skin, excessive sweating, full volume bounding pulse, tachycardia, elevated blood pressure, exaggerated tendon reflexes, and upgoing plantar responses. If untreated, the condition may end fatally. Diagnosis is confirmed by demonstrating blood sugar values below 60 mg/dl. A simple bed side test is to give 50 ml of 25% glucose intravenously which dramatically allays symptoms and restores consciousness within minutes. Hypoglycemia which develops after the use of short- acting insulins tends to be transiet. But if hypoglycemia is the result of long-acting insulins or a long-acting hypoglycemic agent, it tends to be persistent. In such cases, an intravenous infusion of 5% glucose has to be started and continued till the condition of detecting the cases and adjusting the dosage of insulin. When monocomponent insulins are used, their doses have to be smaller, compared to other conventional preparations (usually in the range of 5- 10 units instead of 20- 40 units). In atherosclerotic individuals, hypoglycemia may precipitate myocardial and cerebral ischemia.
Allergy may manifest in various forms, change in type of insulin is often helpful. Sometimes, insulin may have to be continued under cover of antihistamines.
Insulin Injection
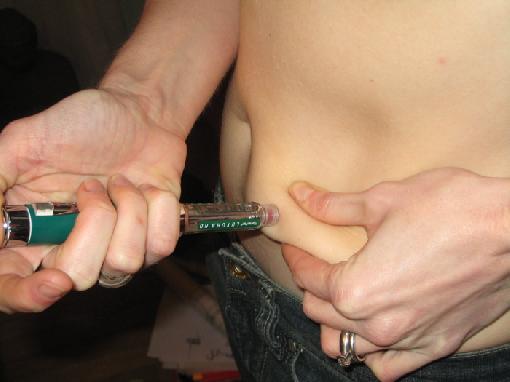
Insulin Resistance
In some individuals, the effect of insulin wanes and 200 units or more may be required daily. The development of antibodies which neutralize insulin or the presence of impurities in the insulin cause this condition. Apart from these, complications like ketoacidosis and infection confer temporary insulin resistance. Gross fluctuation in insulin requirement demands careful search to eliminate the underlying cause. Monocomponent insulins are of value in cases where antibodies to conventional insulins are present.
Insulin lipoartrophy is seen at the site of repeated injections as disciples. The fat recovers on stopping the injection. Administration of monocomponent insulin at these sites helps to restore the fat in most cases. In some cases, the fat may even hypertrophy.
Newer insulin delivery systems: Since intermittent injections do not achieve perfect control of blood sugar, concentration, automatic continuous or intermittent delivery systems have been developed. Further refinements have incorporated glucose sensors which automatically regulate the delivery of insulin. The control of blood sugar levels can be monitored through the blood sugar estimation, or the glycosylated hemoglobin estimation tests.
Glycosylated Hemoglobin: Levels of glycosylated hemoglobin (HbA1c) reflect the blood glucose concentrations over a period of about 6 to 10 weeks, prior to the test. In the presence of hyperglycemia, glucose is attached (glycosylation) non-enzymatically to the N-terminal of Hb A and the percentage of glycosylated hemoglobin increases. Levels of glycosylated hemoglobin do not fluctuate within short periods. The normal level of Hb Al c in most of the laboratories ranges around 6%. In uncontrolled diabetes this may exceed 10- 12%.
Duration of Insulin therapy: In the majority of patients dependent on insulin, it may have to be continued for long periods. In some, insulin can be withdrawn if the diabetic state stabilizes. During periods of stress or infections, the insulin requirement may actually go up. Withdrawal of insulin under such conditions leads to the development of ketosis and coma. This risk should be made known to all patients receiving insulin.
© 2014 Funom Theophilus Makama