Foot care in Diabetes - What you need to know about your feet!
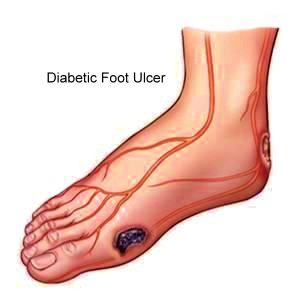
Diabetic foot disease is a less concerned entity but, 5-15% of diabetics develop foot ulcers at some stage of their disease process, leading to amputation. It is said that 85% of non traumatic lower limb amputations follow diabetic foot ulcers and foot problems are responsible for nearly 50% of all diabetes-related hospital admissions. Another important fact is that these ulcers take a long time to heal and 70% of healed diabetic ulcers are likely to recur within 5 years.
What are the causes of foot ulcers in diabetes?
There are various underlying mechanisms to cause ulcers; it can be divided into intrinsic and extrinsic causes. Extrinsic causes include diabetes related poor vision as a result of diabetic retinopathy, falls as a result of joint immobility or even oedema appearing in extremities, for example due to heart failure or renal failure. Intrinsic causes are the most important and those are direct complications of diabetes mellitus. Main causes are diabetic neuropathy, arterial disease causing Peripheral Arterial Disease (PVD) related with atherosclerosis, abnormal tissue response to trauma and sepsis.
How does diabetic neuropathy affect your feet?
In diabetic neuropathy there can be sensory involvement, motor involvement or autonomic involvement. Sensory involvement causes loss of pressure, pain, temperature and joint sense which will expose the patient into danger without being aware. Therefore the risk of trauma is high. When motor nerves get affected it causes weakness and atrophy of intrinsic muscles of foot, hence altered foot structure and leading to deformity and altered biomechanics. Also arterio-venous shunting which occurs due to autonomic neuropathy, affects maintenance of skin integrity and vascular tone so it causes a warm, dry, fissured foot.
A charcot foot is a condition which is seen in 0.2% of patients with long standing diabetic neuropathy. There are several features related with this i.e.
· Hyperaemic response
· Osteopenia
· Local fractures
· Inflammatory response
· Affected proprioception causing deformity
How can diabetic vascular disease affect your feet?
Arterial disease related with diabetes mellitus is of two types; either macrovascular or microvascular. Macrovascular disease which affects medium and large blood vessels with atherosclerosis leads to impaired blood supply to distal areas of lower limb. Here the risk of getting atherosclerotic plaques in blood vessels is 4 to 20 times high.
In Fontaine classification which describes the symptoms related to PVD; the grades are as follows;
Grade I- asymptomatic patient with absent pulse
Grade II- Symptomatic patients with intermittent claudication
Grade III- Critical ischemia with rest pain
Grade IV- Critical ischemia with tissue loss leading to ulceration, gangrene and amputation
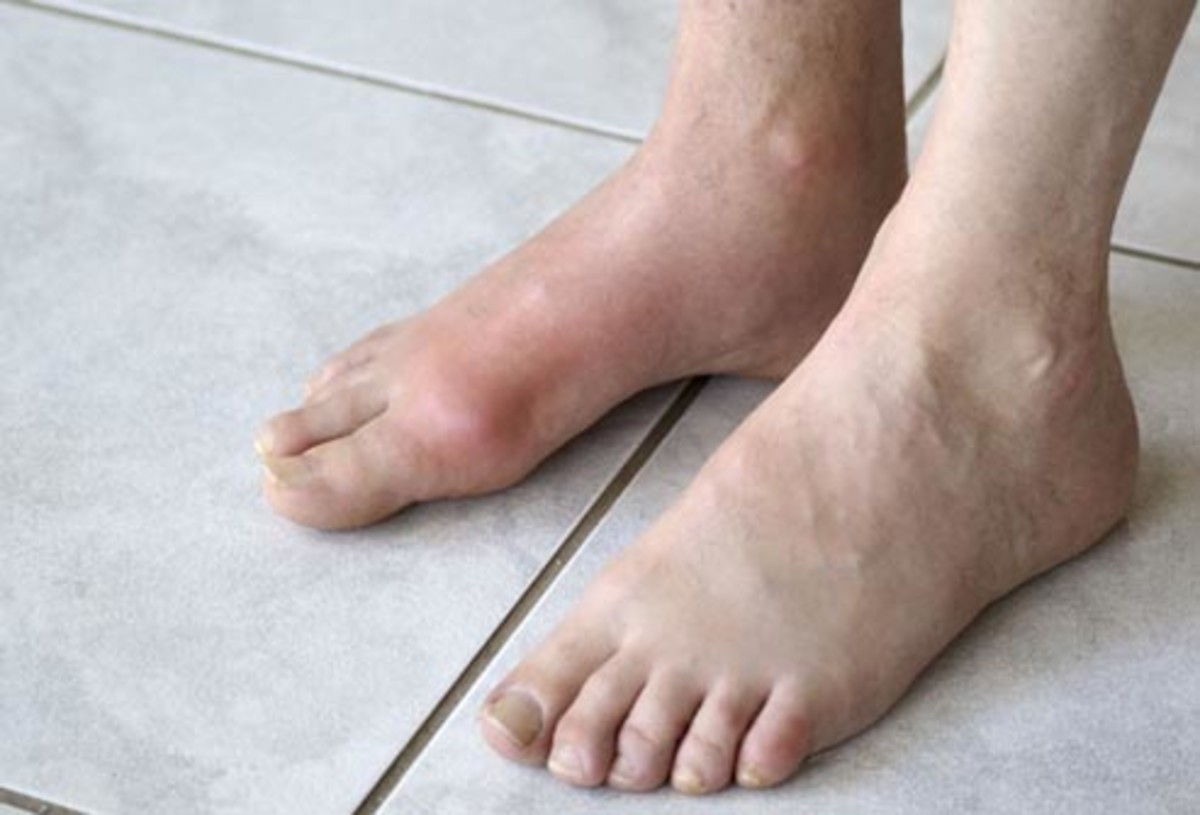
There it shows that in greater degree of arterial insufficiency, ulceration is common. These ulcers may present as painful erosions between toes or as shallow, non-healing ulcers on the dorsum of the feet, on the shins and especially around the malleoli.
Microvascular disease causes microangiopathy affecting smaller blood vessels. Early onset of micro-vascular dysfunction affects arterioles and capillaries of several organs; here basement membrane thickening may impair oxygen diffusion which results in reduced tissue response to sepsis. The results are more serious in extremities.
What happens to your feet in daibetes?
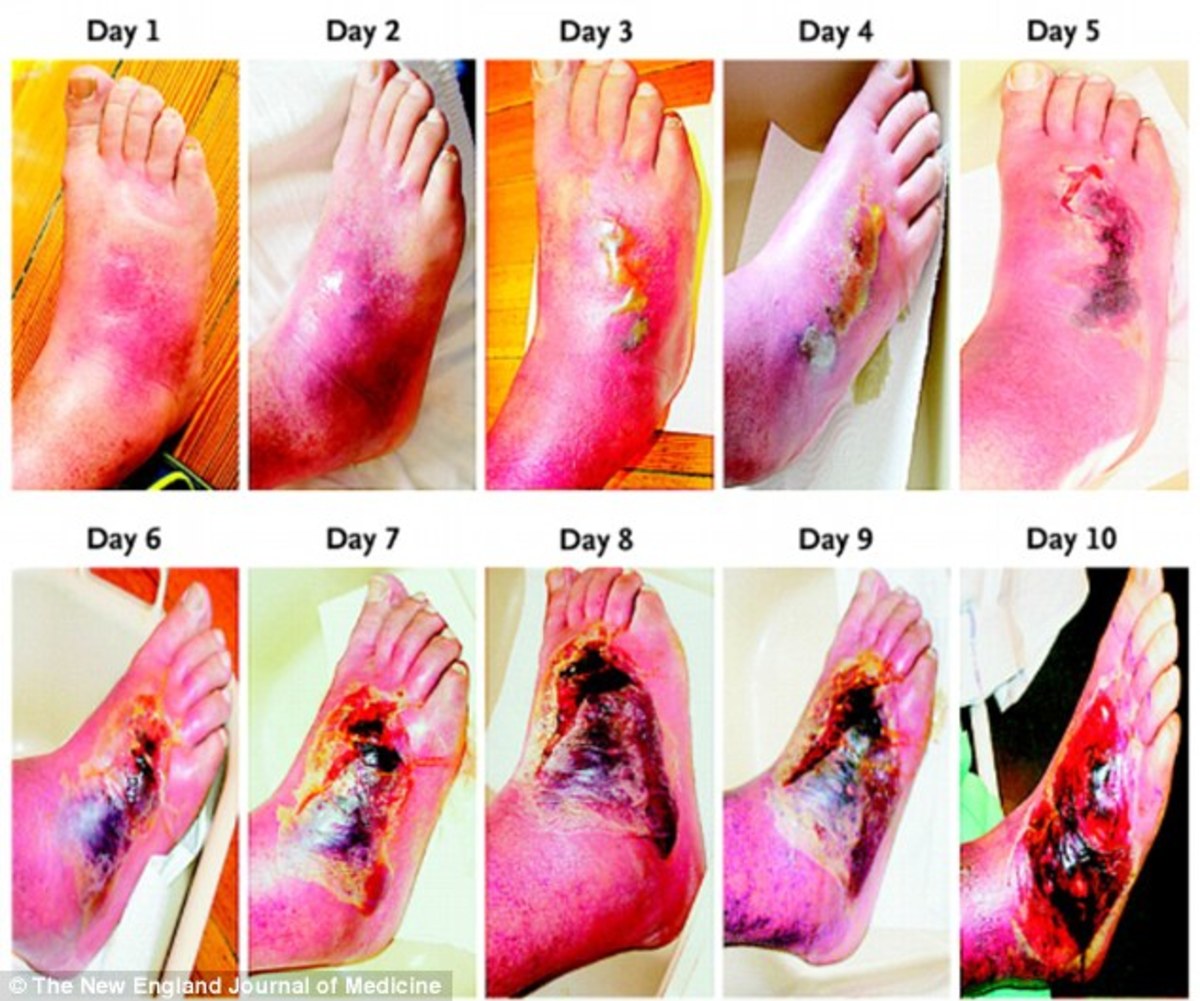
Abnormal tissue response to healing occurs in a diabetic patient. It is due to a number of postulated theories; deficiency of growth factors, impaired fibroblast response and abnormalities of extracellular matrix are among the most appreciated theories up to date. It is also said that there are alterations in neuroinflammatory response, hyperaemic response and thermoregulatory response. Apart from that, the cell mediated immunity is depressed in long standing diabetics and the phagocytic function of multinuclear leukocytes affected with affected leucocyte migration at microcirculatory level. Since patients have hyperglycaemia associated with mycotic infections the end result may be secondary bacterial infections.
Infections causes large collections of pus since immunity is altered in these patients so they get very extended infections but with little pain if the patient has neuropathy or else severe pain if it is associated with ischemia. As there is poor ability of the body to fight against infection by the time patient comes to ward there can be tracking of pus along tendon sheaths which is difficult to cure.
Wargner 1-5 a Global Severity Score is based on the severity of the ulcer as mentioned below
1. Superficial ulceration limited to dermis
2. Ulceration down to fascia or bone without abscess or osteomyelitis
3. Deep ulcers with abscess or osteomyelitis
4. Localized gangrene confined to the toes or forefoot
5. Gangrene requiring immediate major (above ankle) amputation
How to care for your feet!!
Most important part in management of diabetic foot is patient education on prevention. Many diabetic foot problems are avoidable, if patients know the principles of foot care. Following are some of the preventive measure in foot care which patients ought to practice
1. Ask not to walk barefoot
2. Inspect the feet daily
3. No hot fomentation
4. Wear correct footwear
5. Not to weight bear (unsupported) on the affected foot
6. Not to sit cross-legged
7. Not to remove footwear during traveling
8. Cut nails regularly (trim square) but they should not cut their own toe-nails
9. No home surgery
10. Clean the feet twice a day

Foot wear in diabetes.......
Patients are educated to wear mainly protective footwear which is specially designed for patients with diabetes mellitus. Features of protective footwear are
· There should be accommodation and cushioning in shoes
· Have wide toe box and extra depth
· Contain total contact insoles and rocker sole with wedging
· Heel to toe length, arch length, width measure both feet fit while weight bearing
· Check for the positioning of the first metatarsophalangeal joint
· Allow half a inch between end of the longest toe and the end of shoe
· Sniff fit around the heel
What to do if you get an ulcer!!
Proper wound care is very important to speed up the healing process. Manage the wound with deep swabbing; taking pus for culture and sensitivity test; blood transfusions if haemoglobin levels are low and expose to hyperbaric oxygen are some measures to be taken. Other measures are weight reduction; aggressive debridement and drainage of tissue space; give intravenous antibiotics like Penicillin, Co-amoxyclav , Metronidazole, Clindamycin also leukocyte colony stimulating factors.
Also rest injured area with prophylactic surgery to correct Biomechanical damage can be performed. Revascularization with angioplasty and distal venous bypass are treatment modalities for PVD. If all the treatment modalities fail amputation is the last resort. Many diabetic limb amputations could be delayed or prevented by more effective patient education and medical supervision.