Giant Cell Arteritis (Temporal Arteritis, Cranial Arteritis) And Miscellaneous Connective Tissue Syndromes
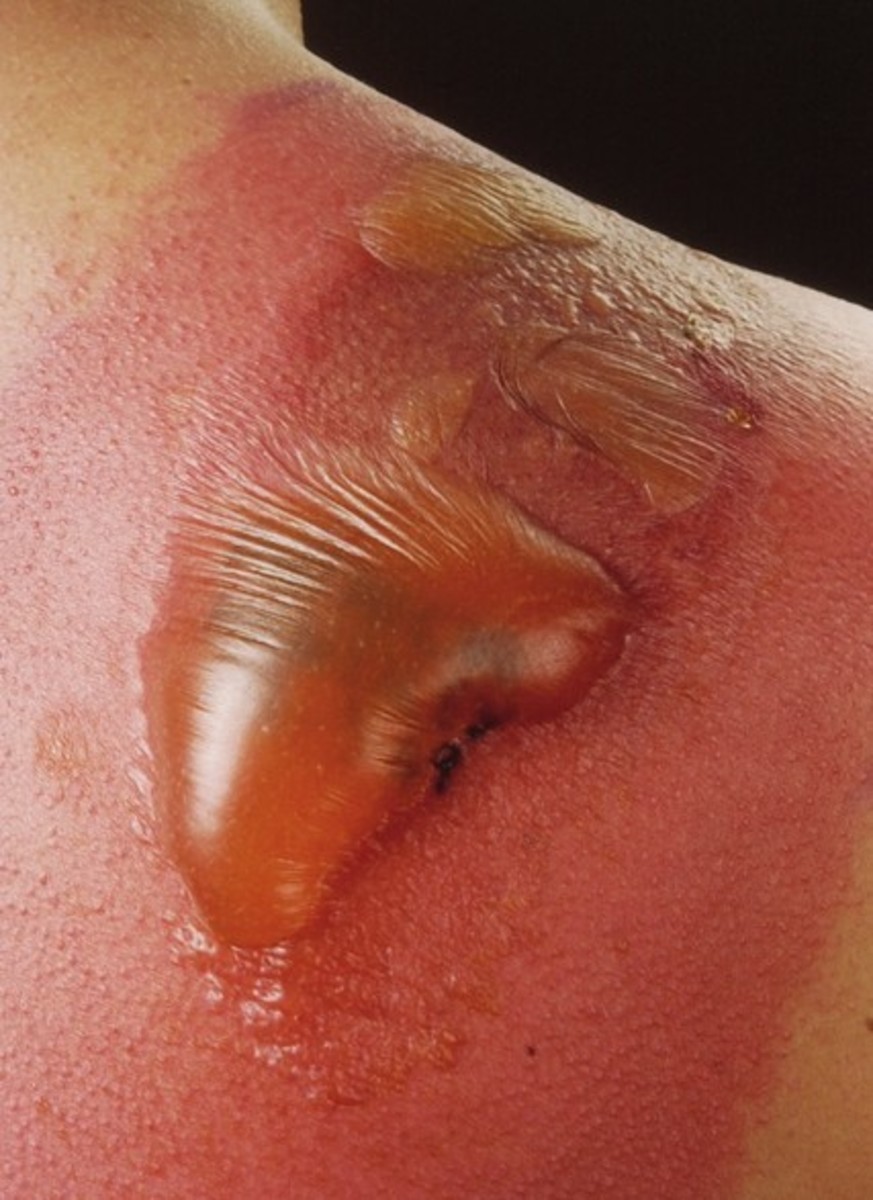
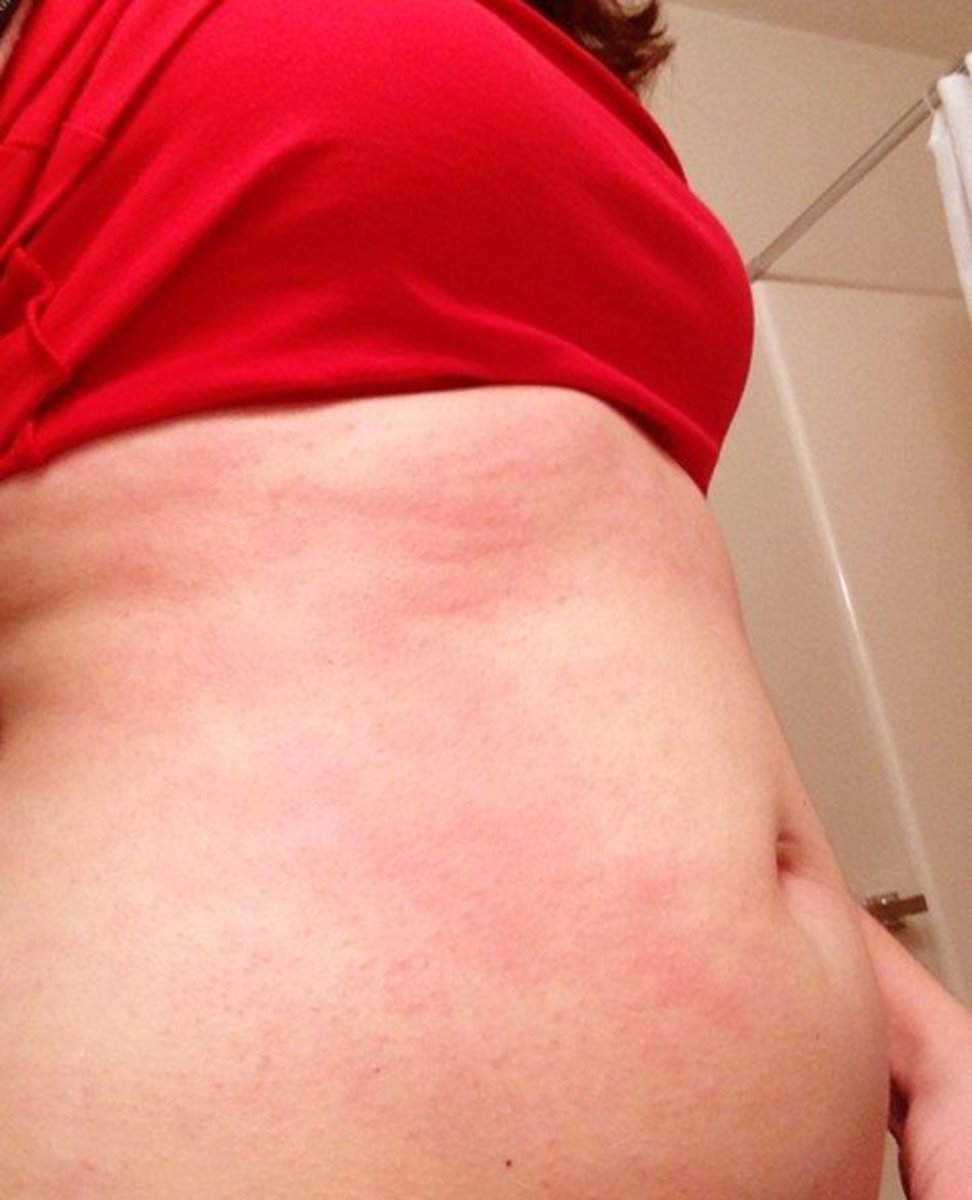
Giant Cell Arteritis Ulceration
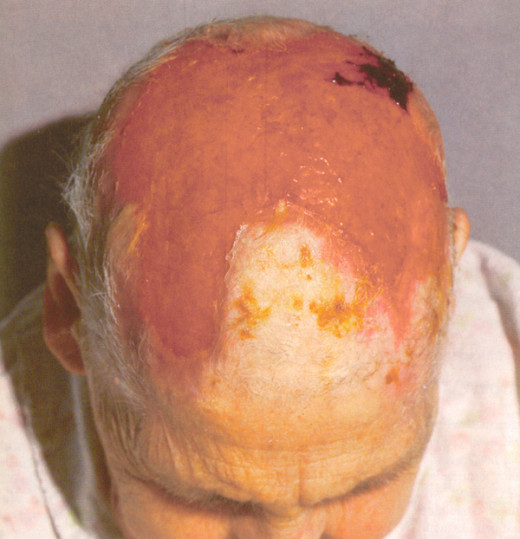
Giant Cell Arteritis
This is form of systemic connective tissue disease occurs in the elderly, in the sixth and seventh decades. It is characterized by a panarteritis with giant cell infiltration, predominantly affecting the cranial vessels. The etiology is not established.
Pathology: The larger arteries such as the internal and external carotids, temporal, occipital and ophthalmic arteries are usually involved, though any other artery may show lesions. The lesions are segmental with intervening normal areas. The media of the artery is infiltrated by round cells and giant cells. The vessels may be occluded by thrombi which recanalise later.
Clinical features: Both sexes are equally affected. Onset is with severe, unilateral or bilateral headache in the temporal or less commonly in the occipital regions, associated with vomiting. Diagnostic feature is the palpably thickened, tender and non-pulsatile temporal arteries.
Loss of vision due to occlusion of the ophthalmic artery is a dreaded complication. Rarely, patients present as facial neuralgia with jaw claudication on chewing, deafness, necrosis of the tongue, or an associated widespread necrotizing arteritis of small vessels which presents as peripheral neuropathy.
Laboratory diagnosis: The ESR often exceeds 100 mm/hr and all immunoglobulin fractions are elevated. Temporal artery biopsy which reveals the characteristic histology is diagnostic. However, a negative biopsy does not rule out the diagnosis, since the lesions may occur segmentally.
Treatment: Corticosteroids are indicated in high doses. Prednisolone (50- 60 mg/day) may be started initially and tapered off slowly to the minimum maintenance dose required to keep the ESR down. This treatment must be continued for at least one year.
Once blindness occurs, it is irreversible and it has to be prevented by early diagnosis and institution of steroid treatment.
Tendinitis
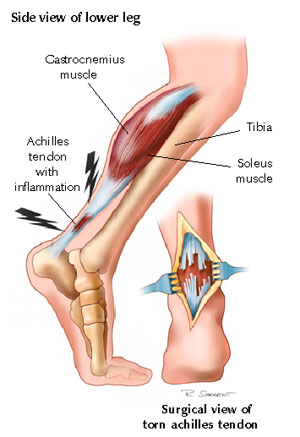
Miscellaneous Connective Tissue
In may musculoskeletal syndromes, no definite disorders of bone, cartilage or connective tissue may be demonstrable. They present with pain and varying grades of disability due to local inflammatory changes but follow a self-limiting course. Such are as follows:
- Lumbago-Sciatica syndrome: Pain is vaguely located in the low back, it may radiate to the lower limbs. Signs of nerve-root compression do not occur.
- Supraspinatus tendinitis
- Sub-acromial bursitis
- Bicipital tendinitis
- Frozen Shoulder: This is a condition of painful limitation of movement of the shoulder. In the initial stages, the shoulder is tender and painful, but later on it becomes painless. It is more probably caused by lesions of the rotator cuff. Myocardial infacrtion, hemiplegia, herpes zoster or surgery on the chest wall may be followed by the syndrome of “frozen shoulder”.
- Shoulder hand syndrome: This is a condition in which shoulder movements are restricted and it is associated with pain and swelling of the hand. Conditions which lead to frozen should also may give rise to this syndrome. The incidence is more in epileptics and those on barbiturates and antituberculosis drugs. Treatment consists in the judicious administration of analgesics, anti-inflammatory drugs, corticosteroids, local short wave diathermy and manipulation. In some cases, sympathetic nerve block may be required.
- Tennis elbow: This condition is caused by the traumatic rupture of the common origin of the extensor tendons at the lateral epicondyle.
- Golfer’s elbow: This condition is caused by the rupture of the common flexor tendon from the medial epicondyle.
Precipitating factors include exposure to inclement weather, unaccustomed exercise, infections, faulty postures, and mild trauma. These disorders are more common in the older age groups.
© 2014 Funom Theophilus Makama