Meningitis: Is your Child at Risk?
Meningitis, is a disease which causes an inflammatory response of the meninges of the brain. It may affect persons of from all ages, but is very dreaded for children and young infants. The diseases may be caused by several entities, most common of which is by an infection -- of which case will be presented in this article.
What are the tell-tale signs of this condition? What are the warning signs to watch out for? What do you need to know about seizure events?

The Case of Baby E
In order to analyze the disease, we follow the case of Baby E. He is a 13 month old infant who initially consulted because of history of 1 week of coughing. This progressed to difficulty of breathing later on which culminated in several episode of vomiting which prompted his mother to bring him to the clinic. Also, the mother reported that Baby E. has suddenly developed convulsions with accompanying change in skin color to a bluish tinge. This lasted for a few minutes.

Initial Symptoms of the Baby E.
- Fever
- Cough
- Vomiting
- Seizures
Approach 101: Define the Manifestations
As readers can see, there are several signs and symptoms presented by Baby E. Most of which are very vague and non-specific. In order to analyze this, each of the manifestations should be correlated and analyzed.
For the diagnosis of this case, several hinge signs and symptoms could elaborate the condition seen in the patient. Since the temporal profile (sequence on how the manifestations presented) of the patient has a noticeable continuous chain of events, the connection between these can elucidate the pathophysiological mechanisms of his underlying condition. These include the early onset cough, worsening and progressive later on developing with difficulty of breathing. Secondly, there was the fever which developed at the middle part of the disease process. Third, is the abdominal pain and vomiting which happened during the day and a few hours prior to admission. Lastly, are the seizure episodes that necessitated the emergency consultation.
Of all the known manifestations, one should first focus the attention on the most specific and hard to manage without elaborate medical care – the seizures. In this types of cases, vivid characterization of the convulsion episode is very important. The details of which are explained further in this discussion.
Seizures and Convulsions – What readers need to know
Before actually labelling the patient’s manifestation as a ‘seizure’, it is important to note that there are several seizure-like conditions that are common in this age group. Non-epileptic seizures contribute to an approximated amount of 20% of patients diagnosed with first onset seizure. Some of which include apneic syncope, paroxysmal movement disorders, sleep disorders, and other psychological disorders. It is very difficult to differentiate a true seizure from a non-seizure event and there is no single sign, symptom, or test that can clearly draw a line between them. In the case presented, the patient was not reported to have been diagnosed with these conditions before. There are no associated signs related to these disorders such as impairment in cognition, mental retardation, chronic movement changes, and uncontrolled sleep or psychological problems. Hence, although we cannot fully rule-out these are possible causes, it is more prudent to consider the convulsion as a true seizure until other signs prove otherwise. Now, we move on to the categorization of the seizure episode.
In the assessment of the seizure episode encountered by the patient, it is important to characterize it primarily since seizures are very common in this age group. Hence, the etiologies are greatly varied so entertaining several causes may prove to be too difficult. Seizure is defined as “transient, involuntary alteration of consciousness, behavior, motor activity, sensation, or autonomic function caused by an excessive rate and hypersynchrony of discharges from a group of cerebral neurons.” Considering this definition, it is still very broad and therefore can be further differentiated based on the manifestation experienced by the patient. First, it is notable that this is his first time to develop this condition so we could lean towards the acute causes first before considering the recurrent causes. Nonetheless as noted earlier, seizures are very common in this age group, not only those which are acute; but this may spell a first time manifestation of recurring types such as epilepsy.
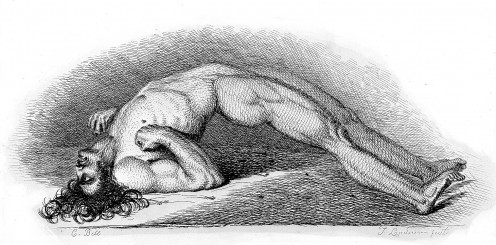
“During the initial tonic phase, the child becomes pale, with dilation of the pupils, deviation of the eyes, and sustained contraction of muscles with progressive rigidity.”
Diving In Deeper to the Case of Baby E
The motor activity manifested is one of the key characteristics that may elucidate the etiology of convulsions. It was reported that the patient had minimal activity during the seizure event. The watcher was unable to fully document the event but it was notable that there was sudden contraction of the patient’s limbs with not much jerking movement noted. The patient also had rolling of his eyeballs. Since the patient was an infant, he is unable to report if there were any aura, or associated symptoms noted. This type of seizure may be noted to be similar to the one described as an initial tonic phase. This is characterized as: “During the initial tonic phase, the child becomes pale, with dilation of the pupils, deviation of the eyes, and sustained contraction of muscles with progressive rigidity.” The rolling of eyeballs may be important in defining this as a true seizure event. It is seen in patients that closure of the eyes indicates psudoseizure, while a fixed gaze, rolling of eyeballs, or lateral gaze may indicated temporal or extratemporal lobe seizure, respectively. The other descriptions for partial, complex partial or absence seizures do not fully characterize the case presented by the patient.
Notable associated symptoms with the onset of seizures is the onset of febrile condition. As stated by the watcher, the patient had a temperature of approximately 39 C during the initial event 9 hours prior to admission. In this case, we could start to consider that the febrile condition may either be a (1) cause, or (2) separate manifestation of the same disease process, (3) contributory as both a cause and a similar manifestation. In aid with this, we should define one type of seizure pertinent in the case of the patient. “A febrile seizure is defined as a convulsion that occurs in association with a febrile illness in children between 6 months and 5 years of age. A simple febrile seizure is single, brief (<15 minutes), and generalized.” The patient has also presented with generalized weakness and inactivity as reported by the watcher, later on the child has gradually regained his activity. This is parallel with those experiencing the post-ictal state of this kind of seizure. The definition does cover the manifestation of the child’s convulsion based on its presentation. For the specificity of type of febrile seizure presented, further assessment is needed. It was reported that a good proportion of patients simply have febrile seizures mainly due to fever, and not due to any primary neurologic cause. Furthermore, there is great variability in terms of manifestations of the most usual causes such as meningitis. Hence, assessment is necessary in order to further delineate the classification of the patient.
All Roads Converge to Bacterial Meningitis
In delineating the common cause of the fever, associated with the febrile seizure, it is important to note that the febrile seizure may be solely due to the fever, independent to any primary neurological origin This may however be due to 2 conditions predisposing to each other. Bacterial meningitis is the likely candidate for ruling in since it may explain most of the symptoms of the patient. Also, it fits the temporal profile. The patient was also reported to have several bouts of vomiting. This may be due to increase in Intracranial pressure whenever the meninges of the patient is inflamed.
The most common cause of bacterial meningitis in children include haematogenous spread (through the bloodstream) or direct extension. In children of this age, it is commonly due to respiratory tract infection which may lead to direct colonization of the bacteria to the meninges. In the case of the patient, this is a very likely outcome of the patient’s longstanding infection. It was reported that he had a respiratory tract infection that was initially not managed by the parents. It was reported that this later progressed to productive cough, and even caused difficulty of breathing the latter end of the week since the initial manifestations. This is parallel with the usual manifestations such as fever, and onset of mental status changes.
The mother did not report any occurrence of noticeable meningeal irritation. However, it is only usually seen in 5% of patients and it does not rule out meningitis.
The correlation between simple febrile seizure and bacterial meningitis has varied results based on literature review. There are no prospective studies fully supporting the direct associative correlation between these two. In one large prospective study, it was estimated that 23% of patients with bacterial meningitis had seizures.
Group A meningococcus accounts for an estimated 80–85% of all cases in the meningitis belt, with epidemics occurring at intervals of 7–14 years. In the 2009 epidemic season, 14 African countries implementing enhanced surveillance, reported 88 199 suspected cases, including 5352 deaths, the largest number since a 1996 epidemic.
— World Health Organization, November 2012What laboratory procedures are used for diagnosis of meningitis?
The use of lumbar puncture if highly useful for this case since it may directly detect the presence of bacteria. Analysis of the CSF and gram stain and cultures may show the exact organism that is responsible. Even though there is no growth in culture, the WBC count, differential and both glucose and protein concentrations may indicate the presence of infection in the CNS. This points to the direction why many of the signs and symptoms presented in the case such as the fever, seizures, and sequale of the respiratory tract infection.
The use of routine neuroimaging in children is not really supported by literature, it was recommended that it must be performed when the child has suffered from head trauma, or is suffering from post-ictal focal neurologic deficit. However, it is not really recommended for those proved by fever as the first line of workup.
Other useful tests include Complete Blood Count (CBC) for the determination of White Blood Cell (WBC) differentials. This is needed for the supportive diagnosis in case of increased Neutrophil count.
Arterial Blood Gas (ABG) may be requested in case of continuous respiratory distress. This assess the degree and adequacy of oxygenation.

Have you (your family members) been vaccinated against meningitis?
The Treatment for Meningitis
The patient presents with seizures during the visit in the Emergency room. In these cases, the most important thing is the maintenance of airway, breathing and circulation. It was reported that the patient was cyanotic on several occasions. This may be due to the period of apnea because of the clonic event, associated with the massive impairment of the oxygenation of the patient due to the respiratory tract infection.
It is the priority to maintain a patent airway in cases that the patient will start to seize. Insertion of a tongue guard may be done it the seizure activity can be predicted. This will ensure that the patient will not cause his tongue to block the air passages. Then, management of the respiratory tract infection is paramount. Symptomatic relief with the use of nebulization and mucolytic in cases of massive mucus trapping may be done at first. This will ensure a patent airway and good areas for gas exchange leaving less likelihood of cyanosis episodes from occurring again. Oxygen support may be initiated in cases of severe dyspnea, this may be done through administration of low-flow oxygen via face-mask.
Pharmacologically, during interval episodes, the patient should be given anticonvulsants to avoid onset of seizures. Also, the patient can be started with empirical antibiotics during the presentation in the emergency room. The choice of antibiotic depends on the most likely etiologic agent. In this case, it may be due to Streptococcus spp., or Haemophilus spp., or Neisseria spp. being the most common in this age group.
For the readers information, there is also preventive measures such as vaccination that help protect oneself from contracting this disease. Boosting the immune system has also been helpful against the viral forms.
Closing the Curtain
After two weeks of stay in the hospital and laborious monitoring and treatment, Baby E was finally sent home medicating with an oral antibiotics at home. He was generally well and the meningitis storm has passed.
In summary, children are very vulnerable with this condition since their body lack the capacity to fend of infections similar to adults. It is very important to recognize the early signs, and seek appropriate help from a medical professional.
Works Cited and Further Reading
- Adams, S. M., & Knowles, P. D. (2007). Evaluation of a first seizure. American Family Physician, 75(9), 1342–7. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/17508528
- Ansari, I., & Pokhrel, Y. (n.d.). Culture proven bacterial meningitis in children: agents, clinical profile and outcome. Kathmandu University Medical Journal (KUMJ), 9(33), 36–40. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/22610807
- Berkley, J. a, Versteeg, A. C., Mwangi, I., Lowe, B. S., & Newton, C. R. J. C. (2004). Indicators of acute bacterial meningitis in children at a rural Kenyan district hospital. Pediatrics, 114(6), e713–9. doi:10.1542/peds.2004-0007
- Chávez-Bueno, S., & McCracken, G. H. (2005). Bacterial meningitis in children. Pediatric Clinics of North America, 52(3), 795–810, vii. doi:10.1016/j.pcl.2005.02.011
- Curtis, S., Stobart, K., Vandermeer, B., Simel, D. L., & Klassen, T. (2010). Clinical features suggestive of meningitis in children: a systematic review of prospective data. Pediatrics, 126(5), 952–60. doi:10.1542/peds.2010-0277
- Elger, C. E., & Schmidt, D. (2008). Modern management of epilepsy: a practical approach. Epilepsy & Behavior : E&B, 12(4), 501–39. doi:10.1016/j.yebeh.2008.01.003
- Friedman, M. J., & Sharieff, G. Q. (2006). Seizures in children. Pediatric Clinics of North America, 53(2), 257–77. doi:10.1016/j.pcl.2005.09.010
- Gates, J. R. (2002). Nonepileptic Seizures: Classification, Coexistence with Epilepsy, Diagnosis, Therapeutic Approaches, and Consensus. Epilepsy & Behavior, 3(1), 28–33. doi:10.1006/ebeh.2001.0310
- Hampers, L. C., & Spina, L. a. (2011). Evaluation and management of pediatric febrile seizures in the emergency department. Emergency Medicine Clinics of North America, 29(1), 83–93. doi:10.1016/j.emc.2010.08.008
© 2015 LM Gutierrez