Pathogenesis, Clinical Manifestations Diagnosis, Prognosis And Treatment Of Agranulocytosis
Agranulocytosis

An Overview
Severe depression of neutrophils, often associated with infection is called agranulocytosis. It is characterized by severe prostration, fever, necrotic lesions in the mouth and throat, and almost complete absence of neutrophils in peripheral blood.
Pathogenesis
In the majority of cases, neutropenia is caused by immunological mechanisms triggered on by drugs or chemicals. The granulocytes are preferentially removed by the reticuloendothelial system when they are coated by the drug-antibody complex. Two patterns are seen. Drugs like aminopyrine produce neutropenia occasionally. These act via some inherent sensitivity mechanisms against the drugs or their metabolic products. In this type, agranulocytosis may occur after intermittent administration or even the first exposure to the drug and the neutropenia develops abruptly. In the second type, exemplified by drugs like phenothiazines, prolonged administration leads to gradual reduction of neutrophils. Often this neutropenia recovers when the drug is withdrawn or the neutrophil count may get stabilized at a lower level even when the drug is continued. Probably the mechanism is one of diminished production of cells. Drugs like Sulphonamides may act by both mechanisms.
All antineoplastic drugs are capable of producing severe neutropenia if administered in sufficient dosage and this is due to direct impairment of cell production. A large number of drugs can cause agranulocytosis. The main groups are:
- Analgesics, sedatives, and anti-inflammatory drugs
- Phenothiazines and tranquilisers
- Sulphonamides
- Sulphonyl-ureas and diuretics
- Antithyroid drugs
- Anticonvulsants
- Antihistamines
- Antimicrobial agents, especially chloramphenicol
- Other drugs, eg, phenindione, procainamide, etc.
- Anticancer drugs
It is to be remembered that no drug is completely free from this form of toxic reaction. History of drug ingestion may not be forth coming in 20% of cases. When the neutrophil counts goes below 1000/cmm overwhelming infection sets in.
Gangrenous Ulceration In Agranulocytosis
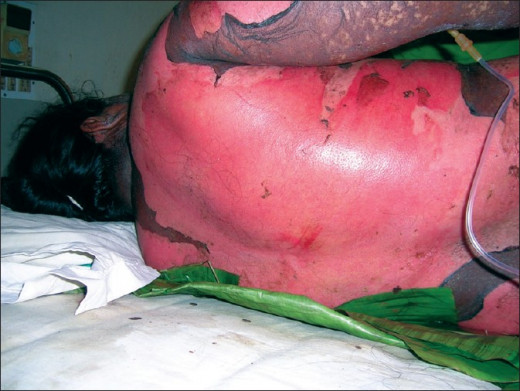
Clinical presentation
The condition ushers in with high fever, chills, sore-throat, and extreme prostration. Common sites of infections are the gums, throat, tonsils, lips, tongue, genitalia, and perianal regions. Which may show gangreneous ulceration. The ulcers are covered with grayish black, offensive exudates. The surrounding tissue is red and necrotic without any tendency to localized the lesions and the lesions tend to extend to the surroundings. Mild or moderate lymph node enlargement may be present. Systemic infection results in severe toxemia. Septic shock is not uncommon. If untreated, the vast majority of patients die in 3-9 days.
In agranulocytosis, there can be gross neutropenia. On many occasions, neutrophils may be absent in the peripheral blood smear. In the early stages, a few old neutrophils may be present, but young forms are rare. Total leukocyte count is generally below 2000/cmm and most of the leukocytes are lymphocytes. The reduction in neutrophil count bears some relationship to the severity of the condition and chances of recovery in the majority of cases. Erythrocytes and platelets are usually normal. Bone marrow shows depletion of all myeloid elements. Blood culture and material collected from the ulcerated areas show mixed organismal flora.
Leukemia Patient
Diagnosis
Clinically, the condition should be suspected whenever a patient receiving drugs develops sore throat, ulcerations of the tonsils, gums or genitalia, or develops toxemia. Strong clinical suspicion is absolutely essential to make early diagnosis.
Agranulocytosis has to be differentiated from acute aleukemic leukemia, infectious mononucleosis, vincent’s angina and thrush. In aleukemic leukemia, there is also thrombocytopenia and anemia.
At the earliest clinical suspicion, the total and differential leukocyte count should be performed and repeated after 12 hours, and all offending drugs should be withdrawn immediately.
Course and prognosis
Agranulocytosis carries a mortality of 50-60%. The type of drug, severity of neutropenia, occurrence of infection and age determine the outcome. Drugs like chloramphenicol, aminopyrine and phenylbutazone are particularly dangerous in this condition. Old age is associated with a poorer outcome.
Septic shock, pneumonia or hemorrhage from necrotic areas account for death. In those that survive young neutrophils appear in blood within days and rapidly repopulate the marrow and blood.
Symptomatology Of Agranulocytosis
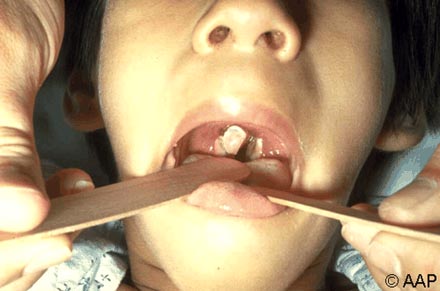
Treatment
- Prompt withdrawal of all possible causative agents and
- Prevention and control of overwhelming infection.
The patient should be isolated with reverse barrier nursing. Powerful bactericidal antibiodic combination should be started on clinical tests. Gentamicin 80 mg, 8 hourly and carbenicillin 5 g 6 hourly given through an intravenous drip gives a wide coverage against many microbes. Other drugs that can be considered are cephaloridine, 1g thrice daily intravenously and penicillin in a dose of 2 mega units intravenously is added if there is doubt of anerobic infection. When bacteriological results are available, the drugs should be suitably modified.
Corticosteriods are not employed routinely but in a rare case, when toxemia is severe, its judicious use may be beneficial.
Granulocytes transfusions in a dose of 5 X 1010 cells daily for 5 days help to tide over the crisis and this is employed in centers where facilities exist. Ideal is to select donors who are HLA and ABO compatible, but in practice, this is difficult to achieve. HLA matching is necessary since the neutrophils carry HLA-A and B antigens: III effects of granulocyte transfusions include allergic reactions and transmission of infections like hepatitis and cytomegalovirus.
Agranulocytosis is a preventable disease if it is remembered that all drugs, even apparently safe ones, are capable of producing this complication. Early detection of the disease helps in saving many lives.
© 2014 Funom Theophilus Makama