Reentry Supraventricular tachycardia
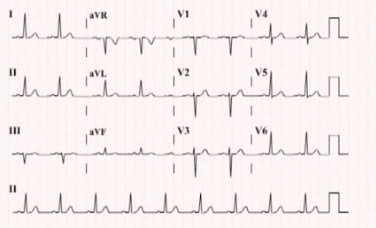
SVT or Supraventricular tachycardia is a term used to refer to a class of rapid heart arrhythmias that begin in the atrial cardiac chambers. Reentry supraventricular tachycardia is characterized by the sudden onset of rapid cardiac arrhythmias or anomalous heartbeat, due to the presence of additional electrical connections in the heart.There are many forms of supraventricular tachycardia and the symptoms elicited by each of them are almost the same, but their treatment however differs.
Most patients with SVT have an additional electrical connection in the cardiac system from birth. Such extra connections can sporadically disturb the normal electrical activity of the heart leading to SVT. Such type of SVTs are referred to as reentry supraventricular tachycardia.
Supraventricular tachycardia is broadly classified into reentrant or reentry supraventricular tachycardia and automatic supraventricular tachycardia. Reentrant or reentry tachycardia is further classified into supraventricular tachycardia, ventricular fibrillation, and ventricular tachycardia.The anomalous electrical connections associated with SVT are congenital and hence can be observed in young, healthy people. Reentry supraventricular tachycardia can result in major symptoms, but is normally almost never life-threatening.
The abnormal connections related to SVT can produce an electrical circuit not occurring in healthy hearts. In just the right conditions, a reentry supraventricular tachycardia may develop when one of the cardiac electrical impulses get ‘captured’ inside this anomalous circuit. The electrical impulse then starts to spin around the circuit, continuously. Each lap around the circuits causes the impulse to create a heartbeat. This in turn causes the heart to beat rapidly eventually leading to reentry supraventricular tachycardia.
The most common types of reentry supraventricular tachycardia include atrioventricular reciprocating tachycardia/AVRT, atrioventricular nodal reentrant tachycardia/AVNRT, intraatrial reentrant tachycardia/ IART, and sinus nodal reentrant tachycardia or SNRT.
The names of each type of reentry supraventricular tachycardia often cause confusion. It is however important to note that each of the names indicate the location of the additional cardiac electrical connection.
Treatment for each of these types of reentry supraventricular tachycardia include medications as well as ablation procedures. The best treatment option is however dependent on the kind of reentry SVT affecting the patient.
Common types of reentry supraventricular tachycardia
- Atrioventricular nodal reentrant tachycardia: It is the most common kind of reentry supraventricular tachycardia. It accounts for nearly 60 percent of the cases.
- In AVNRT patients, the extra cardiac electrical connection is congenital, and the complete reentrant circuit is situated in the tiny atrioventricular node.
- Symptoms of AVNRT include lightheadedness, unexpected palpitations, and dizziness. The bouts may persist for some minutes to many hours.
- The AV node is abundantly supplied by the vagus nerve. Hence, AVNRT episodes can usually be stopped by immersing face in water for a few seconds, the Valsalva maneuver, or other options that elevate the vagus nerve tone. Doctors may prescribe antiarrhythmic medications to prevent this type of reentry supraventricular tachycardia. Ablation therapy can usually cure the condition.
- Atrioventricular reciprocating tachycardia: It is the second most common kind of reentry supraventricular tachycardia. It accounts for around 30 percent of the cases.
- In patients with AVRT, the congenital abnormal cardiac electrical connection connects one of the upper cardiac chambers to the lower cardiac chambers. The additional connection is also referred to as an accessory pathway. Some patients may suffer from electrical impulses in both directions, i.e. from atria to ventricles and vice versa, while others may experience this abnormality in only one direction.
- If the abnormal electrical impulses travel from the atria to the ventricle, then affected patients are said to have the Wolff-Parkinson-White syndrome, which has additional clinical anomalies.
- The reentrant circuit in AVRT-type reentry supraventricular tachycardia is quite big. The anomalous electrical impulse passes across the AV node down to the ventricles, and comes back to the atria via the accessory pathway, then returns to AV node. This repeats continuously.
- Symptoms include dizziness, palpitations, and/or lightheadedness. The bouts may persist for some minutes to many hours.
- AVRT is also associated with the vagus nerve. Hence, acute episodes of AVRT can be stopped as discussed above. Antiarrhythmic drug therapy is moderately effective in treating AVRT, while ablation therapy can cure it and prevent new episodes.
- Sinus nodal reentrant tachycardia: It is not a very common kind of reentry supraventricular tachycardia and accounts for only about 5 percent of the cases.
- The abnormal additional cardiac electrical connection, which occurs from birth, as well as the complete reentrant circuit is present inside the tiny sinus node.
- SNRT-type reentry supraventricular tachycardia is dissimilar from IST/inappropriate sinus tachycardia. SNRT episodes start and stop abruptly, and the heart rhythm and rate remain normal during normal times. However, IST associated abnormal heartbeat slowly speeds up and slowly decelerates. Also, the heart rate is slightly increased even during normal times.
- SNRT is also associated with the vagus nerve. Hence, acute episodes can be stopped as discussed above. Antiarrhythmic drug therapy that includes calcium channel blockers and beta blockers is quite effective. Ablation therapy is not suggested as it can harm the rest of the sinus node.
- Intra-atrial reentrant tachycardia: It is also a rare form of reentry supraventricular tachycardia. The anomalous electrical connection is situated in any one atria.
Episodes involving palpitations, dizziness, and/or lightheadedness may last for some minutes or many hours. It is not associated with the vagus nerve. Episodes can be stopped with antiarrhythmic medications. Recurrent episodes can be prevented with ablation therapy.