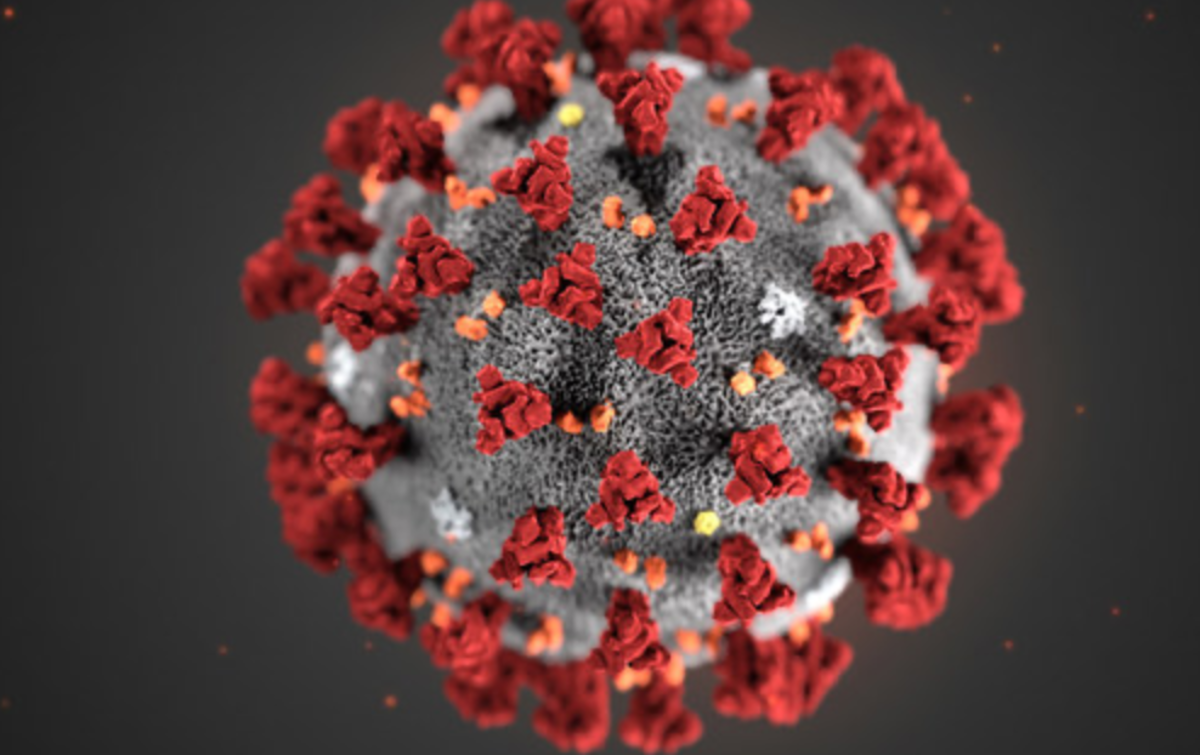
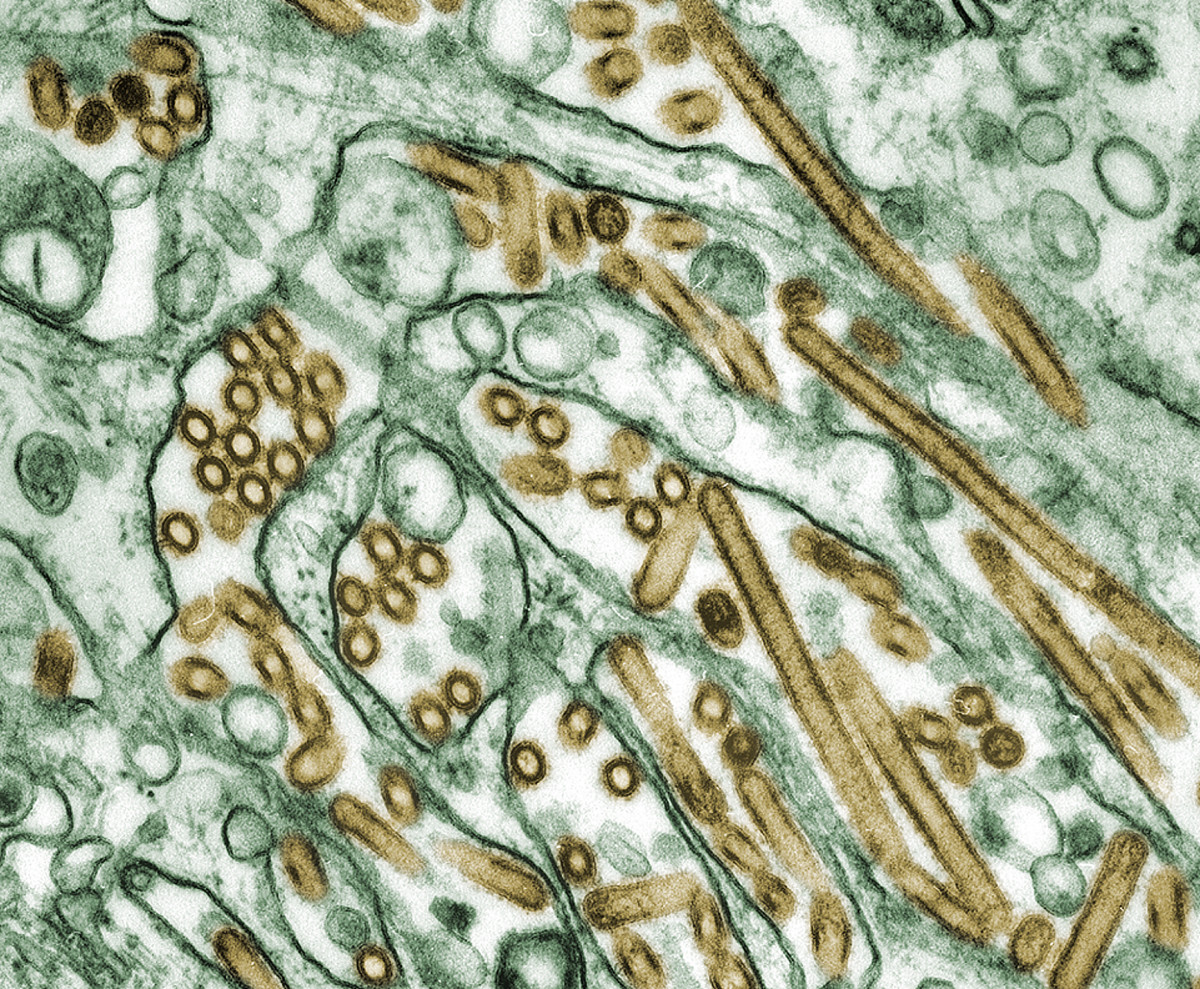
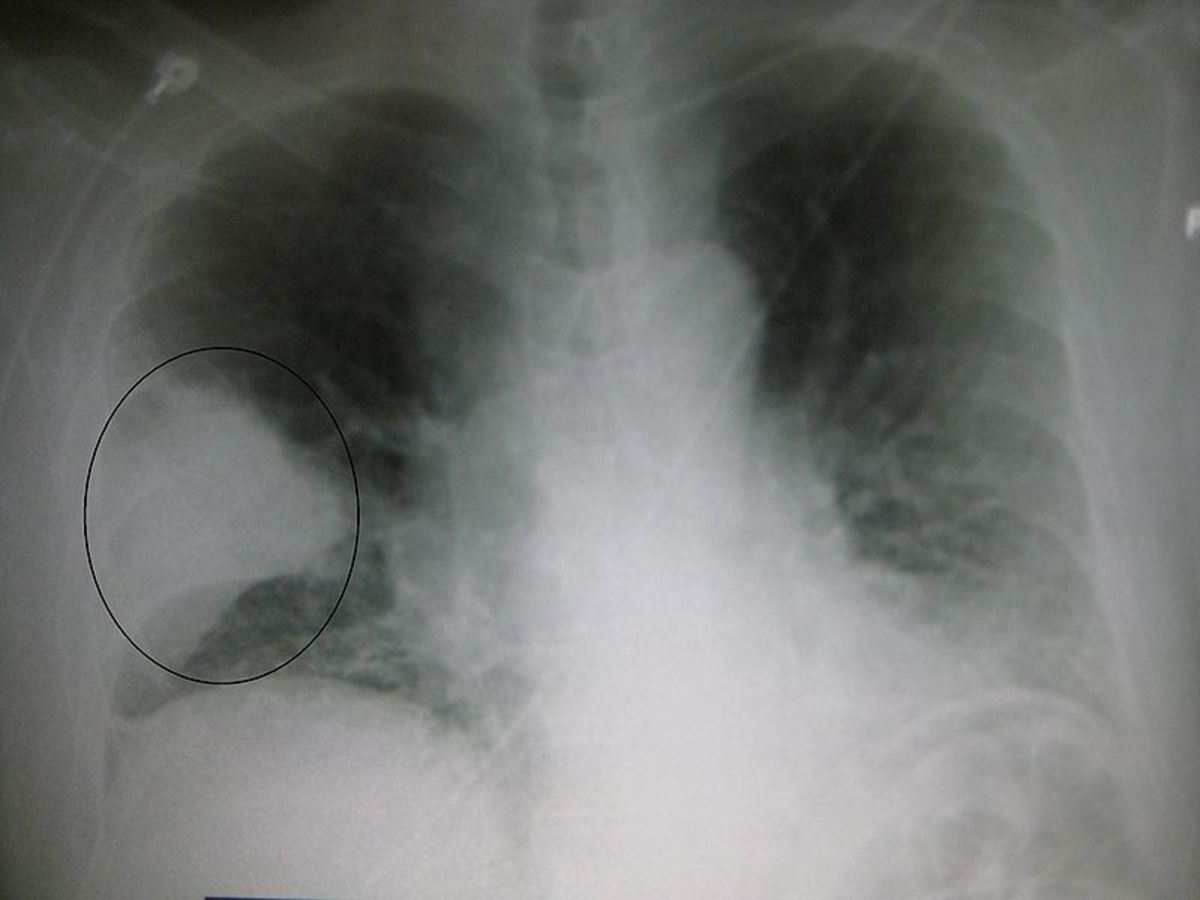
Where Did Severe Acute Respiratory Syndrome (Sars) Originate From?
Severe Acute Respiratory Syndrome (SARS) is a respiratory condition that originates from the zoonotic disease. Among the first symptoms of the disease are flue, fever, lethargy symptoms, myalgia, sore throat, cough and other nonspecific symptoms. High fever and influenza are the only symptoms that are common to most patients. The fever exceeds 38 °C (100 °F). Shortness of the breath may also occur later. Another initial symptom is influenza. The condition was first recognized in 2003. An infection with the SARS causing virus may result to respiratory distress or severe breathing problems and in other times, death. The World Health Organization first identified the disease in 2003. The first SARS case was noted in a 48-year-old man who had travelled from the Guangdong province in China, through Hong Kong, Hanoi, and Vietnam. Both the old man and the health practitioner who had diagnosed the illness died from the condition (Abraham, 2005, 4).
The pandemic was significantly controlled by the affected governments in collaboration with WHO in 2003. During that year, airline passengers in affected countries were thoroughly screened at the particular airports. However, in 2004, another SARS outbreak was again reported in China. Unlike the first one, this one was not caused by human interactions, but from the contact of a laboratory virus sample (Huang, 2011, 23). Despite intense measures taken by governments and world health institutions, the disease remains to be present in animals and human beings because of its ability to mutate. Currently, the disease is spreading at a faster rate and infecting many people in almost all parts of the world.
SARS as a Zoonotic disease
Zoonotic diseases are contagious ailments that are transmitted by animals and human beings. The main causes for these types of diseases are parasites, viruses and fungi. Either animals or insects are carriers of these diseases. Examples may include dengue, anthrax, Ebola, SARS, Lyme disease, Escherichia coli infection, Plague, Malaria, Rocky Mountain spotted fever, West Nile virus infection, and salmonellosis.
The history of Zoonotic disease is long. For example, the bible and ancient Greeks mentions the plague as a form of contagious disease. Today, there are high numbers of Zoonotic diseases that are existing in the world. SARS is among the most notorious of Zoonic diseases in the world today. In addition to other diseases we just mentioned, there are also Lyme disease, ringworms, and many other diseases that are threatening humanity. A zoonotic disease is risky to any human exposed to an infected individual, animal or disease vector. A vector refers to a disease career which transmits the disease from an infected animal to unaffected one. Some of the more risk victims are small children and infants. These groups of people are risky because of the immaturity of their immune systems and poor hygiene associated with them. Other groups of vulnerable people are pregnant women and the elderly. This is because their immune system is more susceptible with more added fetal hazards. The elderly are also immune-compromised individuals and include those with Aids, cancer and health care practitioners.
SARS is one of the zoonotic pathogens, which are transmitted to the human population by another human career, or an intermediate host such as the palm civet. In preventing the development of SARS-CoV virus and ensuing transmission into human populations, heterologous disease models have been incorporated in testing the efficiency of therapies and vaccines on human and Zoonic isolates. (Isolates are SARS careers; there are human and Zoonic/animal careers). Rockx and Feldmann (2011), show that the zoonotic SARS-CoV strains (this is a type of virus) infect the cynomolgus macaques, and results in histopathological and radiological changes that are noted in mild human cases. Viral replications are higher in animals that are infected with a human phase isolate that comes later in relation to a Zoonotic isolate. There are significant variations in the number of host genes which are differentially regulated. The major functions and pathways were found to be similar and appear in the time of infection with the majority of genes that related to interferon signaling pathways.
SARS-CoV is a zoonotic pathogen that emanated from bats and either directly penetrated into the human population or recycled through raccoon dogs or civets as intermediate hosts. Old age was related significantly with increased SARS-related pathogens and deaths because of the rapid progression in the respiratory compromise. Based on epidemiological research, SARS-CoV epidemic is characterized through different phases. These include the early phase, the Zoonotic phase, middle and the late phase. The Zoonic phase is in turn characterized by isolated strains from the raccoon dogs and palm civets that thrive in animal markets. The early phase was featured by various independent human cases, which are mostly related to Zoonotic transmission. The middle phase is characterized by initial human-to-human transmission. The late phase on the other hand, is characterized by effective human-to-human transmission as well as the widespread global transmission in over 30 countries.
The SARS-CoV spike (S) glycoprotein has been noted as being the main mediator for virus penetration and host range by binding it to its receptor angiotensin 1, which is converted to enzyme 2 (ACE-2). A high rate of mutation of the S glycoprotein was noted between the various isolates from both the humans, and animals and several changes to amino acids. These were being identified as being critical for the transition and transmission among human beings. Presently, there are various animal models for SARS CoV that are in extant. These include hamsters, mice, non-human primates, and ferrets. Whereas these models have been employed for studies in pathogenesis and vaccine development, majority of such studies were focused on isolates from the late stage to the eventual outbreak. The heterogonous challenge of mice after vaccination against the late phase S glycoprotein provided only partial protection.
Both the early and late human phase viruses replicated to high level in human ciliated airway epithelial cultures especially where the Zoonotic isolate did not exist. Interesting, the early zoonic and human phase isolates were lethal in older mouse models which results in extreme lung infection which progresses in an early organizing phase of ARDS and death (Rockx, 2007, 7423).
Before emergence of SARS, coronavirus had been detected in both livestock and human populations. However, all the previously known human coronaviruses only resulted to mild respiratory symptoms and have never been related with severe human disease. This is actually what has made the SARS disease unique. These aspects also made the search for the particular cause of the disease to be a complicated affair. It should be noted that corononaviruses had not been extensively studied before, and its origin was even made more complex. Initial evidence indicated that SARS coronavirus had a likelihood of being an animal virus, which had caused the species barrier into the human population. A research carried out by an international team discovered that bats were the potential reservoir host for SARS.
SARS as a World Pandemic
The outbreak of (SARS) was considered as one of the most serious pandemics in the present world perspective. The disease was found to have been caused by a member of the coronavirus family and another kind of virus in the Middle East. It originated from the Southern parts of China to other parts of the world, infecting over 8,000 humans and causing more than 800 deaths. In essence, SARS has caused pain in the global community for various reasons. At first, many people did not know what the condition was or where it originated from. Suddenly, the virus gradually diminished, but again re-emerged back in the Middle East. The SARS virus has continued to cause a consistent outbreak of respiratory diseases. Due to the easiness of the modern travel, SARS has continued to spread from Saudi Arabia, Qatar, Jordan, United Arab Emirates, German, United Kingdom, France, Tunisia, and Italy among other states in the world. SARS has become a potential issue of national security in the affected countries such as China. It has also become a threat to not only the health sector, but also businesses (Duffin, 2006. 27).
On March 2003, the World Health organization issued an international warning, which was followed by the health warning issued by the Center for the Disease Control and Prevention (CDC) in America concerning SARS. Regional SARS transmissions occurred in such places as Ottawa, Toronto, San Francisco, Manila, Ulan Bator, Singapore, Hanoi, Taiwan, and Hongkong among other states. Similar warning was also issued by China, which were directed at the most affected cities as Hebei, Shaanxi, Jilin, Guangdong, Inner Mongolia, Tianjin, Shanxi, and Jiangsu among others (Kleinman and Watson, 2006, 78). Between 2002 - 2003, more than 8,600 cases of infected people and 774 human deaths caused by SARS had been confirmed. This was a case-fatality rate of 9.7%) as listed in the World Health Organization's (WHO) 2004 report. The disease was transferred very fast within very few weeks from the Guangdong province in China to more than 38 other nations in various parts of the world.
Based on more complete and detailed data, the WHO has estimated the case fatality of ratios that range to be from 0% to 50% depending on the age of those affected. The overall estimate of case fatality is 14% to 15%. The probability of dying from SARS in a particular region has been indicated to be depending on the profile of such cases. This includes the age group that had been adversely affected plus the presence of the underlying disease. A report by the WHO articulates the race fatality ratio to be less than 1% among people with less than 24 years. The fatality ratio for people within the age bracket of 25-44 years was 6 percent while for those aged 45-64, it was 15 percent. However, for those with 65 years and above, the fatality ratio was more than 50%. This means that older people had a higher probability of dying from the disease in comparison to others (World Health Organization, 2013).
In essence, SARS infections have been considered as being risky to global health. These necessitated many governments to initiate various programs aimed at preventing wider spreading of the epidemic. However, the threat to the new mutant virus goes on and SARS has been a wakeup call to the global community. There is also a danger that if SARS becomes fully established in developing and very poor nations, and those that harbors few facilities for diagnosis, contract tracing, isolation or treatment, then it could be risk of the disease spreading like bush fire. Further, the disease could be compared with the 1918-1919 flu, which infected more than 400 million people out of which 30 million died. The death rate for SARS is higher in comparison to Spanish flu (WHO, 2003, 1).
SARS and Public Health Campaigns
Many governments have urgently raced against time in preventing the risk of future spread of SARS pandemic. In some places, the number of SARS cases has more than doubled with more than 10% mortality rate. This is an increase of 50%, especially with people with more than 65 years. The poorest nations are more prone to SARS compared to developed nations. It happens that the massive efforts in dealing with the SARS condition have actually paid off. In addition, there is a probability of SARS being eliminated, although the risk has remained to be in existence. SARS prevention and management has remained to be the concern of the World Health Organization, many governments and leading virologists around the globe. It is also the reason why such steps have continued to be considered as an attempt to stamp out the SARS infection (Anderson, 2007, 389).
Presently, the situation is radically different from a few years or months ago where governments were more secretive and reluctant. For instance, six months after the emergence of SARS disease in China, the Chinese government had not disclosed the prevalence and statistics concerning the disease. However, the increasing pressure from the domestic and international community mandated the Chinese government to disclose this condition to the domestic and international community. The official attitudes for many governments are now very different from the past, with SARS cases reported in a transparent manner. There are also various national responses at most national levels. If the Chinese for instance, had continued the official delay and silence for another couple of weeks, the world would have faced challenges that are far more serious. We however need to identify that the massive turnaround in China and the affected countries have been realized at a high social cost, with severe draconian measures, restriction of liberties and other difficult steps (Huang, 2011, 23).
If things had simply continued the way they initially were that is with denial, delay, confusion, bad decisions, ignorance, poor data gathering , incompetence, paralysis in official decision making, secrecy, concealment and the government apathy, then the pandemic would have spread more far and its impact more worse. It is apparent that just one missed SARS case may lead to a closure of an entire hospital, or spark a new epidemic, fill intensive care units and place more than 7,000 in a quarantine or isolation. Places such as Toronto have been able to manage local SARS outbreaks. This is attributed to the fact that such places are backed by best facilities. However, it cannot be expected that the most poor part of the world may be able to effectively cope with the spread in the same way as other countries. An approximate of 3 billion people are surviving on a less than $2 a day, coupled with limited healthcare. In essence, such communities are vulnerable to the spread of SARS and similar viruses to the influence of significant similar cases (McIntosh and Perlman, 2009, 155).
Many countries started delivering strict health advisories and warnings to travelers. For instance, Australia informed its citizens to avoid travelling to Canada and other parts that were affected in the Far East. In China, Japan and Hong Kong, travelers saw citizens covering makeshift pieces of cotton or medical masks as a measure of avoiding contradicting the disease. Canada declared SARS a national disaster and initiated legal measures that were aimed at removing personal autonomy for the affected individuals as a measure of preventing the spread. On the other hand, Taiwan issued a decree of SARS as being an infectious disease, which necessitated enaction of laws banning visits by public servants to affected areas, including Vietnam, China, and Hongkong.
Conclusion
SARS offers a dramatic example of how fast the world is travelling and spreading the disease. It is also an example of how faster the connected health system and governments could respond to a new health threat. SARS has actually altered the way in which the world responds to infectious diseases at a time of increased globalization and international travel.