Women's Health: Reproductive Cancers
Cancer is a collective term that describes a group of diseases that are caused by an abnormal growth of tissues or cells. This abnormal growth usually creates a lump or mass called a tumor. Tumors can be cancerous (malignant), or noncancerous (benign). Benign tumors are not generally dangerous. However, malignant tumors will continue to grow and may break off and spread to other parts of the body, or metastasize. The growth and spread of malignant or cancerous tumors interrupt normal body functions and rob the body of vital nutrients and oxygen.
There is much to be learned about cancer. However, it is known that certain risk factors increase a person's chance of getting certain cancers. For example, skin cancers are more common in those who have had a lot of sun exposures and smoking increases one's risk of lung cancer. Therefore, much of the cancer prevention efforts are aimed at identifying and reducing one's individual risk factors.
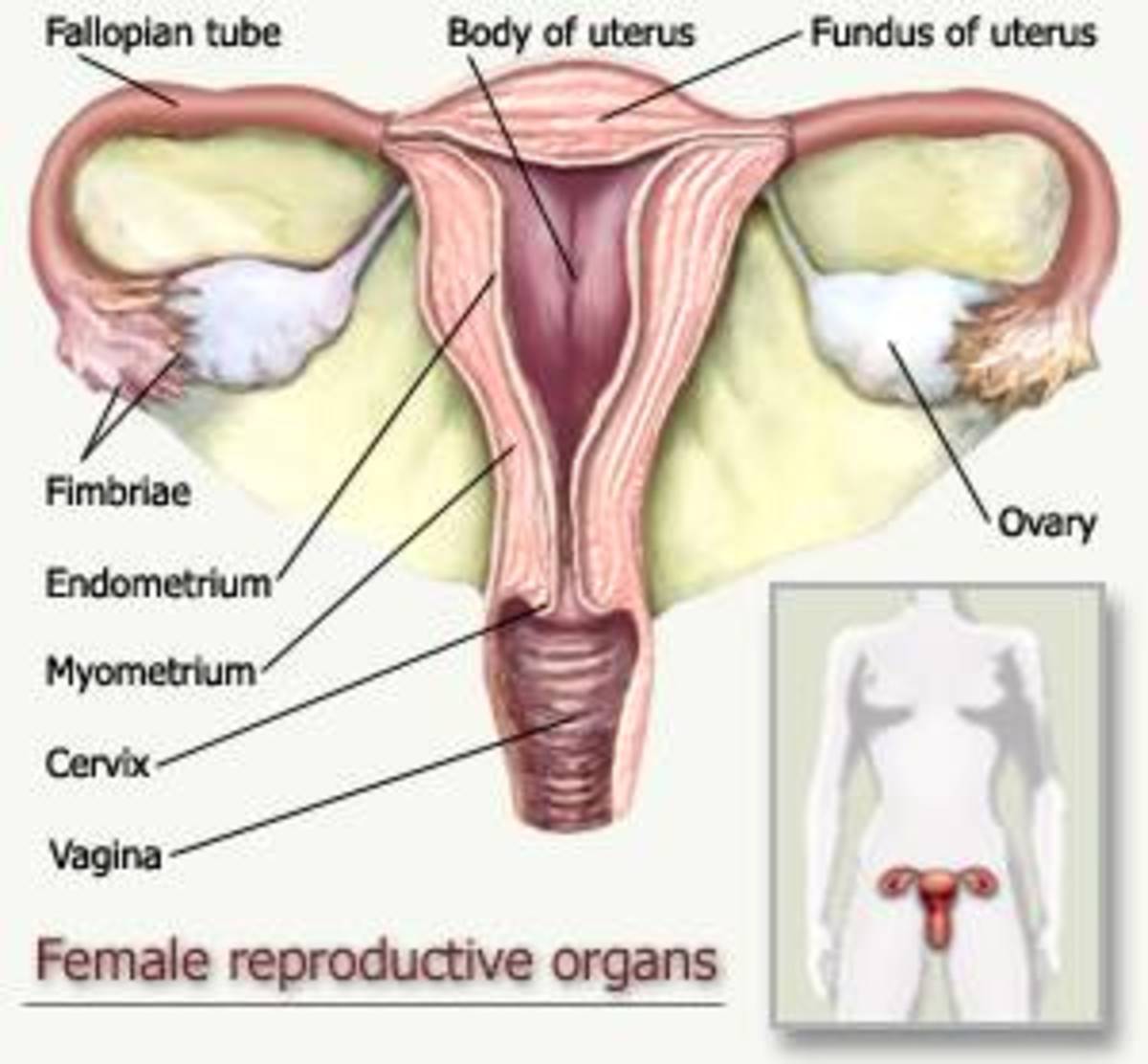
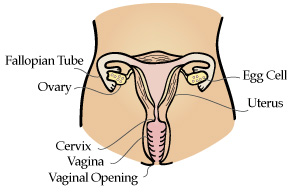
In women, a very important part of maintaining reproductive health and reducing cancer risk involves having periodic pelvic exams and Pap tests, in addition to monthly breast self exams. These simple and inexpensive checkups can detect infections of the breasts, v^gin^, cervix, uterus, or fallopian tubes as well as, cysts or tumors of the ovary and cancer of the cervix. Women should consult with the health care practitioner to determine the best schedule for the routine exams.
Often, reproductive cancers are 'silent,' not producing symptoms until they have grown considerably. A diagnosis of a reproductive cancer can be a surprise to most women. Routine screening is one way to help guard your health and identify cancer early.
In general, all women should have their initial exam and Pap smear when they begin having sex or at the age of 18. Exams and Pap tests are then done at regular intervals for life. It may be suggested that the exams and Pap tests be done annually for those at high risk of cancers or other reproductive problems. Women who have no reproductive problems and low risk for cancer may get by with less frequent exams.
In addition to the Pap test, the pelvic exam can provide some valuable information about the health of your reproductive system. In this exam, the doctor or practitioner will do a gentle exploration with one hand pressing on the abdominal area from the outside while one or two gloved fingers from the other hand are placed in the vagina.
Learning to perform breast self exams, in addition to annual physicals and, after age 40, mammography can assist women in detecting breast lumps early. The key to successful cancer treatment is early detection.
This is done to check the size, consistency, shape and location of the cervix and uterus. Then they will gently touch both sides of the abdomen to locate the ovaries and to inspect for masses or tender areas. Be sure to speak up if you feel any pain or tenderness!
Cancers are generally named after the part of the body where the cancer first starts. The most common cancers of the reproductive system include cervical cancer (cancer of the cervix), ovarian cancer (cancer of the ovary) and uterine cancer (cancer of the uterus).
Cervical Cancer
Cervical cancer is most likely to occur between the ages of 30 and 55. It begins in the lining of the cervix, which is the lower part of the uterus where it joins the vagina. Cancers of the cervix usually form slowly and initiate with cell changes that are called 'precancerous'. For some women, precancerous changes may go away without any treatment. More often, they need to be treated to keep them from changing into cancer. Thanks to Pap smear screening, most precancerous changes are readily detected and treated. Consequently, the death rate from cervical cancer has fallen by 70 percent since the 1940s.
Am I at Risk?
A sexually transmitted infection, called the human papillomavirus (HPV), is thought to be responsible for nearly all cases of cervical cancer. However, it's important to note that there are many types of HPV, and not all of them result in cervical cancer. There are over 70 different papillomaviruses, some which cause the common wart (papilloma) and others which cause genital warts and precancerous changes on the cervix.
HPV, the most common sexually transmitted infection, can be passed from person to person with any skin-to-skin contact with any HPV-infected area of the body. The HPV infection does not always produce warts or other symptoms, so a person may be infected with, and pass on, HPV without knowing it. Although HPV can develop in anyone, it is more likely to develop in women who become sexually active early in life (before 18 years of age) or those who have multiple sexual partners.
The Pap test can provide early detection of cervical changes associated with HPV infection. Women whose Pap tests report a mild cellular abnormality called atypical squamous cells of undetermined significance (ASCUS) should undergo further testing by colposcopy (viewing the cervix through a binocular magnifying instrument).
Currently, there is no cure for HPV. However, there are a variety of medical interventions that help to slow the growth of the virus. In many cases, a woman's own immune system will successfully control the virus so that it remains dormant.
Whether or not a woman with HPV will develop cancer depends on a variety of factors that act together with HPVs. These factors include smoking, decreased resistance to infection, and infection with other viruses, such as human immunodeficiency virus (HIV).
For those with HPV infection, frequent Pap tests and careful medical follow-up, with tissue biopsies and treatment if necessary, can help ensure that the mild abnormalities in the cervix caused by HPV infection do not develop into cancer.
Symptoms
In its early stages, cervical cancer causes no pain or other symptoms. Therefore, the only way to detect early cervical cancer is through regular exams and Pap tests. The symptoms below may be a sign of infection or early cervical cancer and warrants a call to your healthcare provider.
- Watery or bloody vaginal discharge, sometimes heavy and foul-smelling.
- Vaginal bleeding after intercourse, between menstrual periods or after menopause.
- Menstrual periods that are heavier and last longer than normal.
Cervical Cancer Diagnosis and Treatment
Cervical cancer usually develops slowly over time. Initially, healthy cervical cells enter an abnormal phase called dysplasia; which are not cancerous, but can become so. If the dysplastic cells become malignant (cancerous), it is called carcinoma in situ. Carcinoma in situ, is a term used to describe any cancer that is confined to a localized area, rather than spread through other regions of the body. If the cancer cells are not arrested at this point, they will multiply and can invade the lining of the cervix itself, spread to nearby tissue or enter the bloodstream.
Women with genital warts and mild dysplasia usually require no immediate treatment, but should be followed closely with regular exams and Pap tests. Carcinoma in situ and severe dysplasia usually require some type of surgery. Early, carcinoma in situ may be treated with a laser beam, controlled freezing, burning the cancerous tissue with cauterization or sometimes radiation therapy. If the cancer has spread deep into the cervix or into neighboring organs, a hysterectomy (removal of the cervix, uterus and possibly other organs) is usually needed. Radiation therapy and perhaps chemotherapy may be suggested if cancer is more extensive.
Common Cervical Cancer Surgeries
Laser surgery
| A laser beam is used to destroy cells or to remove a small piece of tissue for laboratory analysis. This treatment is for early cervical cancer only.
|
|---|---|
Cone biopsy
| A cone-shaped piece of tissue is removed from the cervix.
|
Simple hysterectomy
| Only the uterus is removed. Pregnancy is not possible following this procedure.
|
Radical hysterectomy
| The uterus as well as tissues next to the uterus, the upper part of the vagina, and sometimes the lymph nodes from the pelvis are removed.
|
Ovarian Cancer
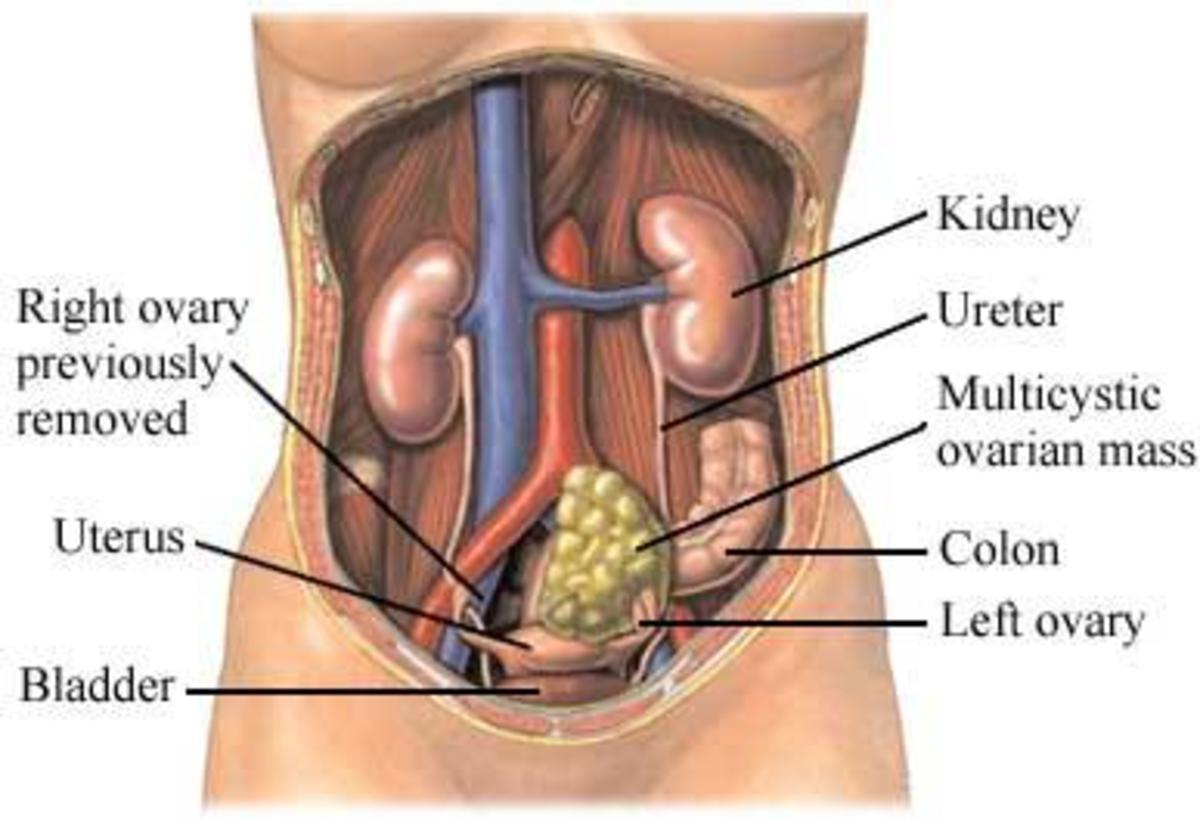
The ovaries are two almond shaped organs on either side of the uterus that produce estrogen and release eggs each month during menstruation. Cancer of the ovary is the second most common gynecologic cancer and the fourth leading cause of cancer deaths among women.
Risk Factors for Ovarian Cancer
Age
| The incidence of ovarian cancer rises with age. Half of all cases are detected in women older than 65, and most are diagnosed after age 60. Experts generally recommend annual pelvic exams for all women over age 40 to increase the chances of early detection.
|
|---|---|
Menopause
| Ovarian cancer is more likely to develop after menopause.
|
Reproductive history
| Risks are greater for women who have never had children, or have delayed childbearing until after age 35. Ovarian cancer is also more common in women who begin menstruating before age 12 or reach menopause after age 50.
|
Genetic predisposition
| About 7 percent of ovarian cancer cases are linked to a genetic predisposition for the disease. Researchers have discovered that women who have a BRCA1 (short for BReast CAncer 1) gene mutation, not only have an increased risk for breast cancer, but also have a 40 percent to 60 percent increased risk for ovarian cancer.
|
Fertility drugs
| A number of studies have reported a link between the use of fertility drugs and ovarian cancer. The results of these studies have been disputed and more research is needed for conclusive evidence.
|
History of other cancers
| Women with a history of breast or endometrial cancer have an increased risk of developing ovarian cancer.
|
Can I Reduce My Risk
Some factors such as the long-term use of oral contraceptives, having children, breast feeding, and undergoing a hysterectomy, are associated with a reduced risk of ovarian cancer. However, the most important steps you can take to reduce your risk are to have yearly pelvic exams and Pap tests, and discuss any concerns or unusual symptoms with your physician.
Symptoms
Ovarian cancer is elusive and may be hard to detect until it is in the advanced stages. Women should always contact their health care provider if they experience any of the following.
- Pain during intercourse
- Abnormal vaginal bleeding
- Discomfort in the pelvic region
- Persistent indigestion, gas, or bloating
- Pain and swelling in the abdomen
Diagnosis and Treatment
Routine pelvic exams may detect ovarian enlargement that may be associated with ovarian cancer. In addition, two tests that hold promise in aiding early diagnosis are ultrasound and a blood test for a protein called CA 125. Abnormalities of the ovaries, such as enlargement, can be detected early through the use of a special imaging device called an ultrasound. The CA 125 is a protein marker that becomes abnormally high in people with cancer.
If ovarian cancer is suspected, several steps may be taken to confirm the diagnosis. An ultrasound or magnetic resonance imaging (MRI) may be ordered to see if there is evidence of a tumor on the ovaries. If a tumor is visualized, then a surgical procedure called a laparoscopy must be done to positively diagnose cancer. If cancer is present, further surgery to remove all evidence of cancer is done. The type and extent of this surgery is dependent on the extent of the cancer. Following surgery, chemotherapy is started to destroy any cancer cells that may be remaining after surgery. Unlike many other cancers, radiation therapy is not routinely used for ovarian cancer.
Uterine or Endometrial Cancer
Cancer of the uterus or endometrium usually strikes women at or past menopause and is the most common gynecological cancer. Most cancers of the uterus occur in the endometrium, which is the lining of the uterus. Cancer of the endometrium is more likely in women who have the characteristics below.
Risk Factors for Uterine or Endometrial Cancer
- Are infertile.
- Began menstruating at an early age.
- Don't have children.
- Have menstrual problems.
- Go through menopause at a later age.
- Are obese.
- Have adult onset diabetes.
- Have high blood pressure.
- Use of estrogen .
- An increased risk may also be seen in those with gallbladder disease and thyroid disease.
Symptoms
The most common symptom of cancer of the endometrium is abnormal vaginal bleeding or discharge. Since uterine cancer often occurs in women around the age of menopause, many mistake the symptoms of vaginal bleeding for a menstrual period. Therefore, women past menopause should always see their health care provider for any vaginal bleeding or discharge.
Diagnosis and Treatment
Diagnosis and preliminary treatment involves evaluation of a sample of endometrial tissue (biopsy), x-rays of the pelvis and endoscopic exams of the colon and bladder. If the biopsy indicates cancer, a hysterectomy will be performed to remove the uterus and ovaries. Depending on the extent of the cancer other tissue may also be removed surgically. Radiation treatments to halt cancer growth and shrink tumor size, may be done before and possibly after surgery.