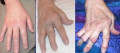
Juvenile idiopathic arthritis treatment

Juvenile idiopathic arthritis treatment
Juvenile idiopathic arthritis (or juvenile rheumatoid arthritis) is a painful condition affecting children. The treatment options for juvenile arthritis often include medications and interventions from a variety of health professionals. Treatment may include several types of medications along with advice or treatment from physical therapists, occupational therapists, dietitians, psychologists and podiatrists among others. It is important that an appropriate treatment plan is administered as soon as possible after the condition is diagnosed to maximize the chance of a good prognosis. This page will outline and discuss common interventions for the treatment of juvenile idiopathic arthritis.
Family doctor or general practitioner (GP)
The family doctor (GP) is usually a good first contact person. They will be able to take a full history, conduct a physical examination and decide on the best immediate course of action. If juvenile idiopathic arthritis is suspected, and diagnosis has not yet been made, it is likely that a referral to a rheumatologist will be provided. Additionally, some lab tests and imaging investigations (e.g. x-rays etc.) are also like to be requested by either the GP or rheumatologist. It is also likely that medications will be prescribed along with a referral to one or more health professionals who may be able to assist with treatment.
Medications for juvenile idiopathic arthritis
There are several types of medications for juvenile arthritis. In general terms most of these medications can usually be classified as one of four broad categories of drugs. These categories are pain relievers, non-steroidal anti-inflammatory drugs (NSAIDs), steroidal anti-inflammatory drugs, and disease modifying anti-rheumatic drugs (DMARDs). The purpose of these four medication types are described below.
- Pain relieving medications – This category includes medications that have a primary influence on one or more steps in pain sensation, but no major influence on underlying condition or inflammation. These medications can be useful to allow someone with juvenile arthritis to get on with certain activities that they need to do without being burdened by pain (this includes sleeping)! However, it is true that all medications used in the treatment of juvenile idiopathic arthritis are intended to reduce pain in one way or another.
- Non-steroidal anti-inflammatory drugs (NSAIDS) –The purpose of NSAIDs is to reduce inflammation in and around the affected joints. In other words, NSAIDs help reduce the swelling and inflammatory mediators that cause pain and discomfort. Medications in this category are not steroids. NSAIDs tend to have fewer side effects with ongoing use than steroid based drugs.
- Steroidal anti-inflammatory drugs (SAIDs or steroids) – The general purpose of steroids in the treatment of juvenile idiopathic arthritis is to cause a rapid reduction in symptoms. Steroids have a similar effect to NSAIDs, but the effect may be stronger and more immediate (e.g. if injected directly into the joint). Unfortunately steroids have more undesirable side effects than NSAIDs, particularly with ongoing use.
- Disease modifying anti-rheumatic drugs (DMARDs) – Unlike medications in the first three categories, disease modifying anti-rheumatic drugs are designed to address the underlying cause of the condition. Drugs in the other three categories tend to treat symptoms directly, but do not stop the primary tissue damage from occurring. Disease modifying anti-rheumatic drugs include a range of medications with a variety of possible side effects. These side effects can be substantial and discussed with a doctor or pharmacist.
It can be a useful exercise to discuss any medications with a qualified pharmacist. Pharmacists have an excellent understanding of the role of each medication, dosage levels, interaction effects when more than one medication are taken at a time and possible side effects.
Physical therapy and occupational therapy
Joint range of motion and muscle strength can be severely reduced amongst children with juvenile arthritis. Targeted exercises can help prevent the loss of joint range and muscle function. These targeted exercises also help to regain lost joint range and muscle strength once the condition is under control or in remission.
Physical therapists are experts in educating, designing and prescribing exercises for this purpose. They can provide a personalized exercise / activity program for children with juvenile arthritis tailored for their specific ability levels and symptoms. This helps to maximize physical functioning. In addition to exercise prescription physical therapists may also use other interventions to reduce symptoms and help children with juvenile arthritis.
Occupational therapy can also be very helpful for children with juvenile arthritis. Occupational therapists use a variety of interventions to help children to function independently. This may involve a variety of treatments including advice, education, exercises, splinting (if appropriate) among other things. Occupational therapists are also skilled in identifying assistive devices that may be useful for children with juvenile arthritis. These assistive devices may include things like built up handles and grips for utensils or pens, raised toilet seats, shower or bathtub chairs, dressing aids (like a shoe horn) etc.
Although occupational therapists and physical therapists have different areas of expertise, there may be some overlap in their scope of treatment for children with juvenile arthritis. For this reason, therapists treating the same child will often look to discuss their intervention plans. This allows them to avoid treatment overlap and permit the child to receive a well rounded treatment protocol. For example a physical therapist may end up focusing their interventions on the larger joints and muscle groups (such as the hips and knees) to improve walking ability while on the same child an occupational therapist may focus their treatment on the small joints in the hand (for writing, dressing, etc.).

Podiatry treatment
Podiatrists can assist children with juvenile idiopathic arthritis affecting their feet and ankles. Podiatrists are able to make custom foot orthotics that can alleviate pain. Additionally, the custom foot orthotics may also help with shock absorbing and walking. It is usually possible to see a podiatrist without a doctor’s referral. However, a doctor’s referral may assist with communication between the podiatrist and the doctor to ensure any pertinent information is reported to each other.
Dietician treatment
Diet may not be the first thing that springs to mind when considering treatment options for children with juvenile arthritis. However, several factors may lead to nutritional impairment amongst these children. Reduced or altered food intake may occur as a result of reduced appetite or difficulty eating. This may be due to physical difficulties while trying to eat or as a side effect of medications. Nutritional impairment may contribute to reduced functioning, growth and development. In the long term it could lead to a short stature, osteoporosis or anemia. Dieticians are skilled in assessing the nutritional requirements for children. They can assess whether these requirements are being met. If a child’s dietary intake is not currently sufficient for their body to function and develop properly, they can provide advice or supplements to overcome any shortfall in the diet.

Psychology / psychologist treatment
Life as a child can be difficult. Unfortunately children with juvenile idiopathic arthritis face additional struggles. This may affect their mental health and put them at risk of depression and anxiety among other mental health conditions. Psychologists can help children dealing with depression, anxiety or other mental health issues. They can also assist children to develop positive coping strategies and promote desirable emotional development.
Other health professionals can help too…
This is not a comprehensive list of health professional that may be required in the management of juvenile arthritis. For example:
- Social workers may assist children and families to cope with the changes in lifestyle and educational adjustments. They may also be able to provide a variety of useful resources.
- Children who have their hands or temporo-mandibular joint (TMJ or jaw joint) affected by the arthritis may benefit from a visit to a dentist familiar with the condition who can help overcome difficulty with teeth brushing and flossing.
- Children who suffer from symptoms in their eyes (such as uveitis) will likely benefit from treatments offered by an ophthalmologist or optometrist.
There are no doubt other health professionals that may be able to assist in the treatment of juvenile idiopathic arthritis.
Summary
In summary there are a variety of health professionals and treatments that can help children with juvenile idiopathic arthritis. Juvenile idiopathic arthritis is a complex condition with symptoms affecting many aspects in a child’s life. The family doctor (GP) is a good first contact person for advice about the treatments that are required for any individual child.
Recommended pages
- Juvenile idiopathic arthritis overview
Juvenile idiopathic arthritis is a condition that is characterized by pain, swelling and heat in one or more joints. This article gives an overview of the condition including causes and diagnosis... - Juvenile rheumatoid arthritis prognosis
A diagnosis of juvenile rheumatoid arthritis (also called juvenile idiopathic arthritis) can be confusing and concerning. This article will outline what the latest research can tell us about juvenile rheumatoid arthritis prognosis amongst children... - Dangerous Eye Complication of Juvenile Arthritis: Uveitis
All parents whose children have been diagnosed with juvenile arthritis need to be aware that eye pain or reduced vision requires prompt treatment... - Supraspinatus tendon tear
Supraspinatus tendon tears are the most common tendon tear in the shoulder region. Tears of the supraspinatus tendon can be painful. They usually present at a sharp pain at the outside or front of the shoulder, particularly with...