ACCESSORY ORGANS
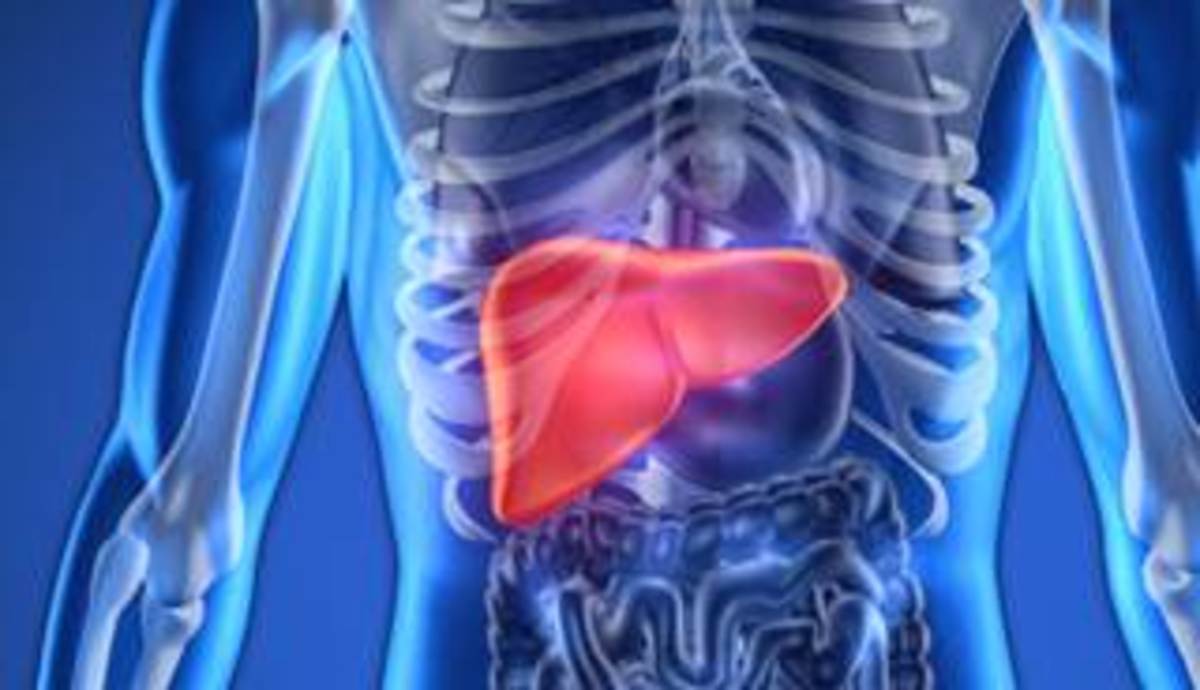
Diseases of the liver
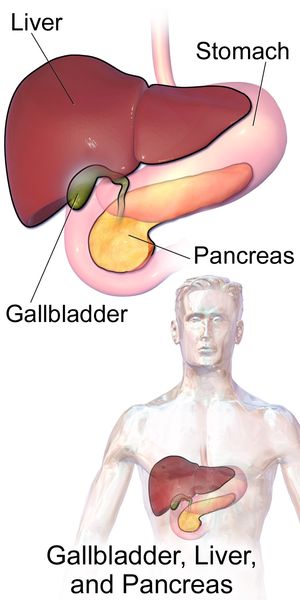
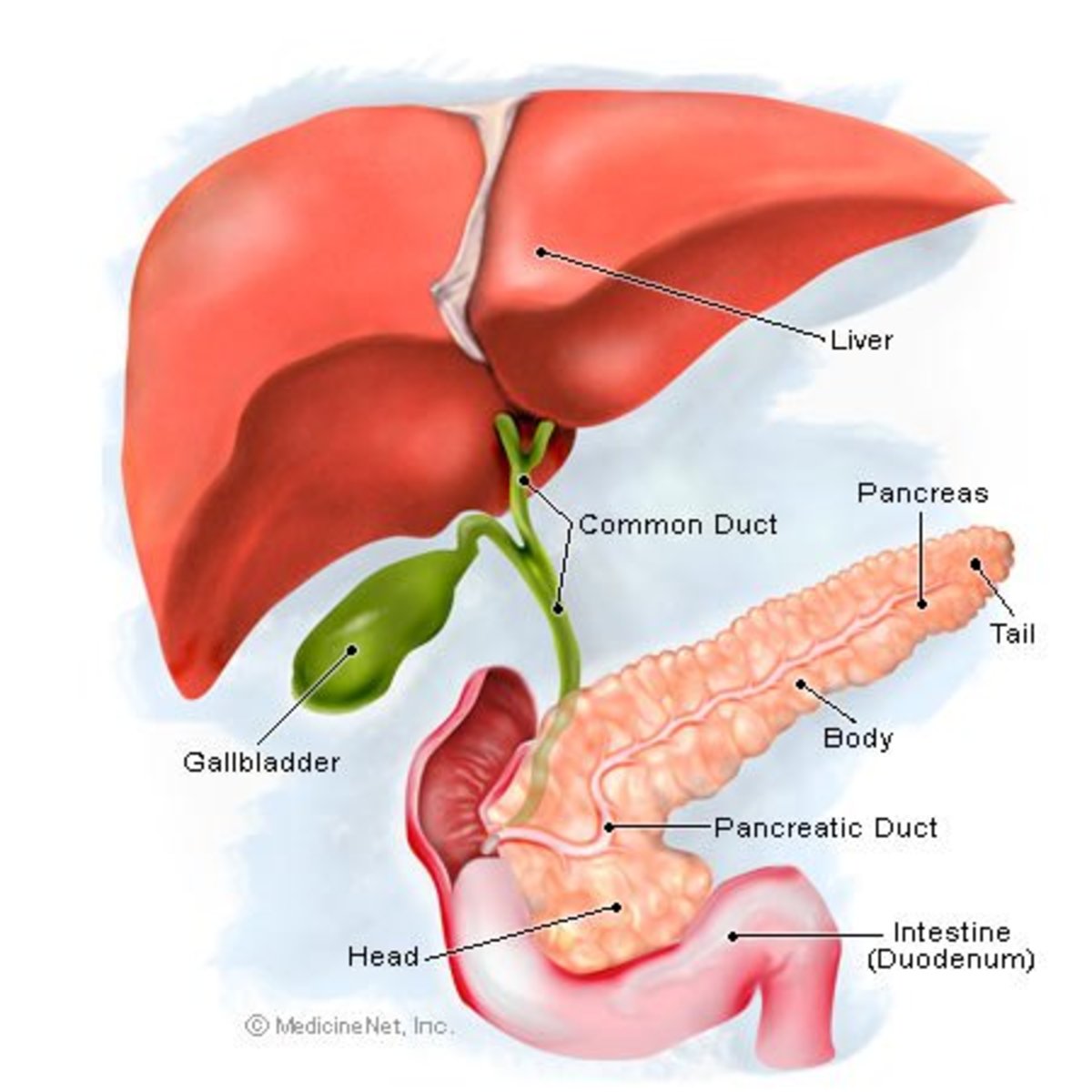
Three major accessory organs lie adjacent to the gastrointestinal tract and produce important digestive agents that enter the intestine and aid in the handling of food substances. Specific enzymes are produced for each of the major nutrients, and bile is added to assist in the digestion of fats. These three organs are the liver, gallbladder, and pancrease. Diseases in each of these organs, therefore, can easily affect gastrointestinal function and cause problems of interference with the normal handling of specific types of food.
Diseases of the liver
Hepatitis. The exact organism responsible for hepatitis is not clearly defined. It is probably one of a group of related viruses. In infectious hepatitis the viral agent is transmitted by the oral-fecal route, a common one in many epidemic diseases. Thus the usual entry is through contaminated food or water. In serum hepatitis the organism is usually transmitted in infected blood by transfusions or by contaminated instruments such as syringes and needles.
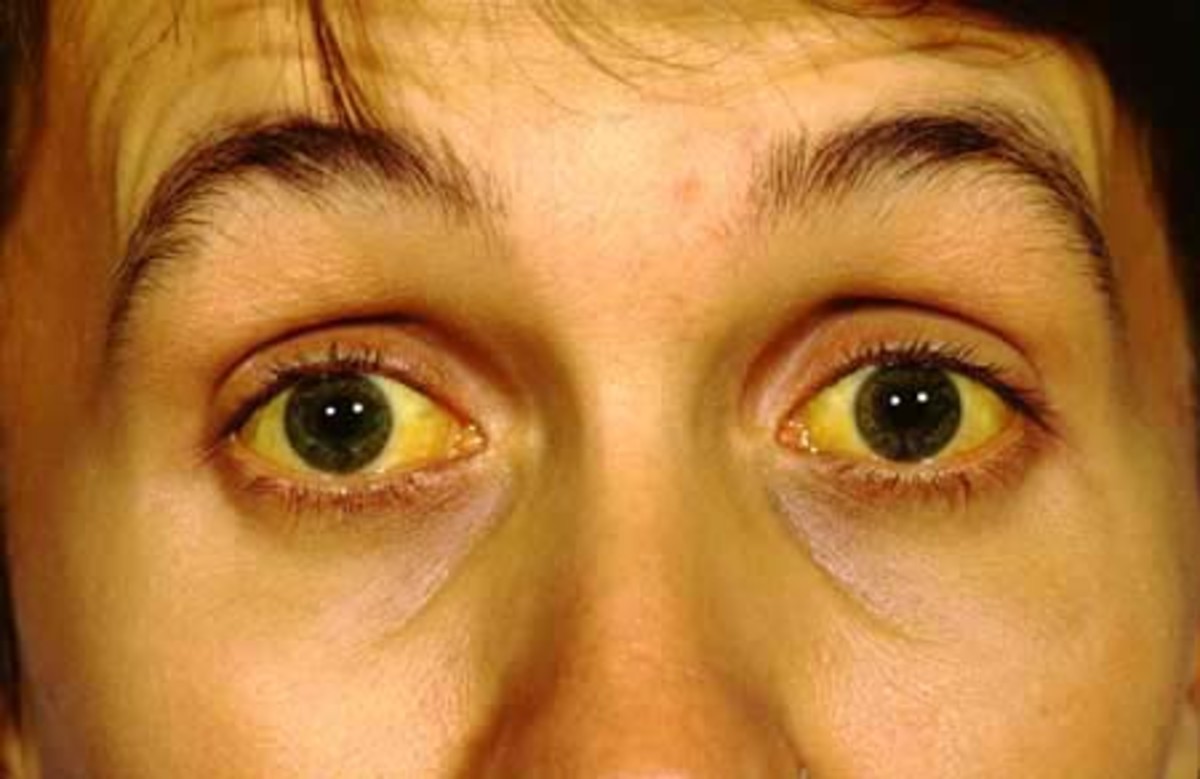
CLINICAL SYMPTOMS. The viral agents of hepatitis produce diffuse injury to liver cells. In milder cases the tissue injury is largely reversible, but with increasing severity more extensive damage occurs. Massive damage in some cases may lead to liver failure and death. Thus varying clinical symptoms appear, depending on the degree of liver injury. Jaundice is a common symptom and the most obvious one. Other symptoms include general malaise, loss of appetite, diarrhea, headache, fever, enlarged and tender liver, and enlarged spleen.
TREATMENT. The importance of bed rest in the treatment of acute hepatitis has been clearly demonstrated. Physical exercise increases both severity and duration of the disease. A daily intake of 3,000 to 3,500ml. Of fluids guards against dehydration and gives a general sense of well-being and improved appetite. Optimum nutrition provides the foundation for recovery of the injured liver cells and overall return of strength. It is the major therapy. The principles of diet therapy relate to the liver’s function in the metabolism of each of the major nutrients.
PRINCIPLES OF DIET THERAPY
High protein. Protein is essential for liver cell regeneration. It also provides lip tropic agents for the conversion of fats to lipoproteins and their removal from the liver, thus preventing fatty infiltration. The diet should supply from 75 to 100gm. Of protein daily.
High carbohydrate. Sufficient available glucose must be provided to restore protective glycogen reserves in the liver and meet the energy demands resulting from the disease process. Also an adequate amount of glucose ensures the use of protein for vital tissue building. This is an application of the protein-sparing action of carbohydrate. The diet should supply from 300 to 400gm. of carbohydrate daily.
Moderate fat. An adequate amount of fat in the diet makes the food more palatable, and hence the patient with poor appetite will be encouraged to eat. Former liver disease diets limited the fat on the rationale of preventing fat accumulations in the diseased liver. However, values of better overall nutrition for improved food intake outweigh these concerns, and a moderate amount of easily utilized fat, such as that in whole milk, cream, butter, margarine, and vegetable oil, is beneficial. The diet should incorporate from 100 to 150 gm. of such fat daily.
High calorie. From 2,500 to 3,000 calories are needed daily to fulfill energy demands of the tissue-building process, to compensate for losses because of fever and general debilitation, and to renew strength and recuperative powers.
Meals and interval feedings. The problem of supplying a diet adequate to meet the increasing nutritive demands of a patient whose illness makes food seem almost repelant to him is a delicate one. It calls for creative ideas and supportive encouragement. The food may have to be in liquid form at first, using concentrated formulas for frequent feedings. As the patient can better tolerate solid food, every effort should be made to prepare and serve it in an appetizing and attractive manner. Nutritional therapy is the key to recovery. Therefore a major responsibility is the devising of ways to encourage optimal food intake. The diet should include approximately the amounts shown below.
Cirrhosis. Liver disease may advance to the chronic state of cirrhosis. The French physician Laennec first named the disease from the Greek work kirrhos, meaning orange, because the cirrhotic liver was a firm, fibrous mass with orange-colored nodules projecting from its surface. Another name given to such a cirrhotic liver is a “hobnail” liver, referring to its rough, nodular surface, similar to that of the bottom of a boot. The nutritional or alcoholic form of cirrhosis bears his name, Laennec’s cirrhosis.
The most common problem is fatty cirrhosis associated with malnutrition. The associated malnutrition may develop from other causes, but it usually is the result of a long history of alcoholism. The fatty liver and early cirrhosis may appear within 5 years of the onset of the alcoholism, but more often 10 to 15 years is required. Increasingly poor food intake as the excessive drinking continues leads to multiple nutritional deficiencies. Damage to the liver cells occurs as fatty infiltration, causing cell destruction and fibrotic tissue changes.
CLINICAL SYMPTOMS. Early signs include gastrointestinal disturbances such as nausea, vomiting, loss of appetite, distention, and epigastric pain. In time jaundice may appear. There is increasing weakness, edema, ascites, and anemia from gastrointestinal bleeding, iron deficiency, or hemorrhage. A specific anemia from folic acid deficiency is also frequently observed.
Essentially the major symptoms are due to a basic protein deficiency and its multiple metabolic problems. As the disease a progress, fibrous scar tissue increasingly impairs blood circulation through the liver, and portal hypertension develops. Contributing further to the problem is ascites, an accumulation of fluid within the peritoneal cavity. The impaired portal circulation with increasing venous pressure may lead to esophageal varices, with the danger of rupture and fatal massive hemorrhage.
TREATMENT. Treatment is difficult when alcoholism is the underlying problem. Each patient requires individual supportive care and approach. Usually therapy is aimed at correction of fluid and electrolyte problems and nutritional support to encourage healing of the liver tissue as soon and insofar as possible.
Diseases of the liver