Understanding Osteomalacia and Managing It Successfully
Osteomalacia is a disorder where the bones become soft and weak, typically caused due to a severe vitamin D deficiency.
Softening of Bones in Osteomalacia
How Does Osteomalacia Present Itself?
- Fracturing of bones is the commonest symptom, especially in adults and old individuals.
- Children show a characteristic bowing of the legs.
- Another important symptom is muscle weakness. Impairment at the site where the muscle attaches to the bone is the cause for muscular weakness. Consequently, walking is difficult and you will develop a waddling gait.
- Pain in the bones, mainly in the hips, is rather common too. the pain is dull and aching pain and radiates from the hips to the pelvis, legs, and ribs.
Etiological Factors for Osteomalacia
Osteomalacia occurs due to an insufficiency of vitamin D. Vitamin D is a very vital nutrient which facilitates the absorption of calcium in the gut.
The vitamin also maintains adequate levels of calcium and phosphate for normal bone formation. Vitamin D is manufactured in the skin from exposure to the sun’s ultraviolet rays. It is absorbed from foods such as dairy products and fish.
If you have low levels of vitamin D in your body, then it fails to process the calcium that your bones require for normal growth and strength. Vitamin D deficiency results due to a poor diet which is lacking in this vital element, no sun exposure, or a disorder in the GI tract.
If you have had a surgery to excise segments of the stomach or small intestine, you will have trouble absorbing vitamin D as well as breaking the food down to release it.
Conditions which impact D3 levels in your body:
- Celiac disease can impair the mucus membrane of the GI tract and consequently hamper the absorption of vitamin D.
- Liver and kidney disorders affect the metabolism of D3.
- A diet deficient in phosphates triggers phosphate reduction, and this leads to osteomalacia.
- Anti-seizure medications - phenytoin and phenobarbital are known to cause osteomalacia.
- Malignancies get in the way of vitamin D processing.
Osteomalacia during Pregnancy
When pregnant, your caloric requirements increase. During the 1st trimester, you require an extra 150 calories daily to support fetal development. Alongside, the requirement for other vital nutrients increases too, and your OB/GYN will advocate taking a vitamin supplement everyday. Ensure that your diet is rich in folic acid, iron calcium, protein, vitamin B12 and vitamin D to avoid deficiencies.
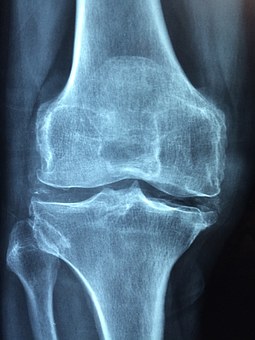
Osteomalacia Radiology and Investigations
- X-rays: Cracks are seen in the bones which are characteristic of osteomalacia.
- Blood and urine tests: Help assess levels of vitamin D, calcium and phosphorus.
- Bone biopsy: A needle is inserted through the skin, into your pelvic bone to excise a tiny piece of bone. Bone biopsy is an accurate way of detecting osteomalacia, on the other hand, it is seldom needed to make the diagnosis.
Supplementation

Osteomalacia Natural Treatment
- Your health care provider will prescribe oral vitamin D, calcium, and phosphate supplements.
- In some cases, you may be given vitamin D intravenously.
- You need spend some time outdoors in sunlight so that your body can make adequate amounts of vitamin D within the skin.
- In case of underlying conditions which affect vitamin D metabolism, they must be managed. Liver cirrhosis and kidney failure need to be treated.
- You may also be prescribed calcium and / or phosphorus supplements.
Soak up the Early Morning Sun

Osteomalacia Diet
Foods Rich in Vitamin D
Consuming foods rich in vitamin D can supply you with all the vitamin D you need to support strong bones. Good dietary sources are – salmon, eggs, cod liver oil, mackerel, tuna, and yogurt. Certain foods are also fortified with vitamin D – milk, orange juice and breakfast cereals.
Foods Rich in Calcium
99 % of calcium in the body is present in the bones and calcium in conjunction with vitamin D and phosphorous is necessary to prevent and manage osteomalacia. Foods rich in calcium are - milk, yogurt and cheese and green leafy vegetables such as kale and spinach
Foods Rich in Phosphorous
Good dietary sources of phosphorous are – milk, yogurt and cheese, eggs, salmon, beef, chicken and turkey.
Step Up Your Intake of Milk, Eggs and Salmon