Why You Should Donate Platelets

Thrombocytopenia, a low platelet count, can occur in response to an injury but also radiation and chemotherapy. Pro-death Bcl-2 family members target megakaryocytes and thus diminish the platelet population. This link confirms the need for platelet donation in chemotherapy and radation-treated cancer patients.
For the past 15 years, my dad has gone into the local Children’s Hospital and donated his platelets. He began donating whole blood in the 1980s and made the switch after some time to platelet donation. Donating platelets is somewhat more involved than donating blood as a whole. The donor is hooked up to a machine and the blood is taken out of the body, spun down, the platelets are removed, and the remainder of the blood is put back into the patient. Platelet donation takes about an hour and a half to two hours whereas whole blood donation takes less time.
So why donate platelets? Well, for starters, according to the American Red Cross website, it’s a lot more bang for your buck. One donation of platelets can provide a single therapeutic dose for a patient, where building a platelet dose from whole blood could take as many as four to six donations. The benefit of getting a full dose from a platelet donation is two-fold since it is also best for the recipient to receive platelets from one donor instead of multiple donors. This cuts down on the chance of cross-reactivity between the donor and recipient’s blood. Platelet donations are critical for patients undergoing chemotherapy, those with immune deficiencies, and those undergoing organ transplants and open heart surgery.
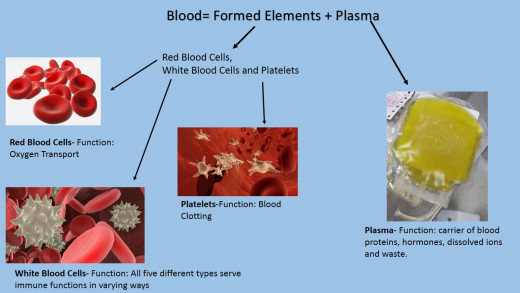
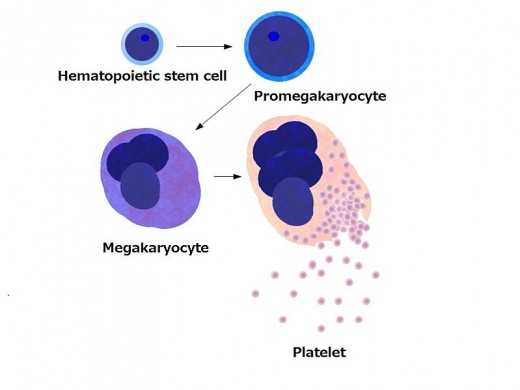
Platelets are one of three formed elements present in blood. A little bit more detail about blood is present in the above pictorial. Platelets, or thrombocytes, are not whole cells but instead cell fragments from megakaryocytes. Megakaryocytes are large, multinuclear cells created in the bone marrow where the fragments of these cells, platelets, contain no nuclei. Most people know to associate platelets with their function in blood clotting.
For more on blood...
- The Basics of Blood and Blood Typing
An accompanying article to 'Why You Should Donate Platelets', this hub introduces the major components of blood and their functions. As well a look at blood typing, the Rh antigen and HLA typing.
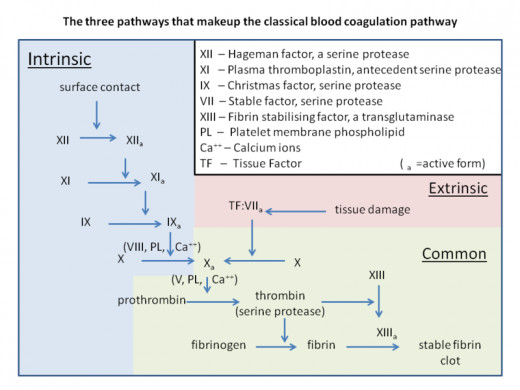
Blood clotting, or coagulation, allows for a self-sealing material to form a plug in our vessels in the event of injury as to not bleed out. Overall platelet formation is a very complex process involving many clotting factors. In the simplest terms, in addition to platelets there are two key players in coagulation: thrombin and fibrin. These clotting factors are the last components in a long cascade which is initiated by the binding of platelets to the damaged site- the exposed connective tissue of the injured blood vessel. Initiating factors are released from intracellular platelet compartments, granules, as well platelets contain receptors on their cell surface that allow for adhesion. The environment as a whole contributes to the adhesion and aggregation properties of the group. This includes not only the platelets but also the damaged cells and the plasma at the site. Ultimately these clotting factors convert prothrombin to thrombin; it will then bind to platelet’s cell surface and allows for fibrinogen to be converted to fibrin. (Fibrinogen and prothrombin are the inactive forms, respectively, of these two proteins). When prothrombin is converted to its active form thrombin, it allows for the conversion of fibrinogen to fibrin. Platelets form the plug, while fibrin, a clotting factor, forms cross-links between platelets to form the clot. Also involved in the system are several anticoagulation factors. As with many systems in the body, there is an equal and opposite system to remove the clot after the incident is over. The thrombolytic system involves the conversion of plasminogen to plasmin, which functions to break down the clot by deconstructing the fibrin polymer. There are also anticoagulation factors, a group of inhibitors of the clotting factors.
Burn victims, bone marrow transplant patients, and patients with Aplastic Anemia also may require platelet donations.
The process of separating out a particular component of the blood from donation is known as apheresis. Platelet apheresis is sometimes referred to as plateletpheresis or simply platelet separation. The process can be done manually or by a machine. Overall the same procedure is followed but going the machine route gives a sterile environment. This not only benefits the intended recipient but also the donor as the blood components not wanted for donation can be safely delivered back to the donor.

The platelet apheresis machine contains either a single or double needle system; a series of sterile tubing, and a single-use centrifuge collection system . The blood is taken from the donor, passed through the tubing and into the centrifuge to be separated. Centrifugation works by establishing a density gradient, where in the case of blood the plasma has the lightest density and goes to the top, the red blood cells form a dense pellet at the bottom of the centrifuge and the buffy coat which contains the white blood cells is found in between the two layers. The donor’s blood is treated with an anti-coagulant before it is spun down to prevent the platelets from clotting. The plasma is rich in the platelets and is usually the desired layer, although the buffy coat also contains platelets so it depends on the specific laboratory’s technique which layer is taken. The unwanted blood is delivered back to the patient either in a separate needle going into the other arm, if the system is a double needle system, or through the same needle and arm the blood was taken out. In the case of the latter the process is repeated until there are enough platelets to make up a unit, while in the case of the former the process is continuous.
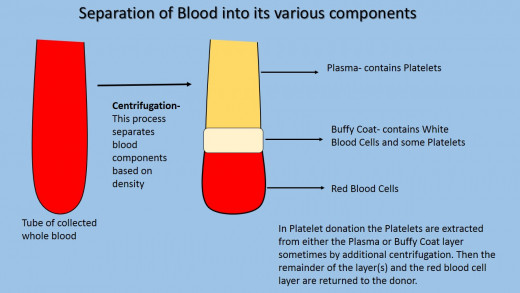
Since the platelets are most often taken from the plasma layer of spun down blood, saline can be given back to the donor to replace the volume. The platelet-rich plasma can be spun down further to separate out the plasma from the platelets. Cross-reactivity can occur if non-compatible donations of platelets in plasma occurred, antibodies for blood antigens are present in plasma. Spinning down the platelet-rich plasma reduces the overall volume of plasma for the donation, potentially minimizing the antibody amount for reactivity. The donor’s body replaces the absence platelets within one to two days of donation.
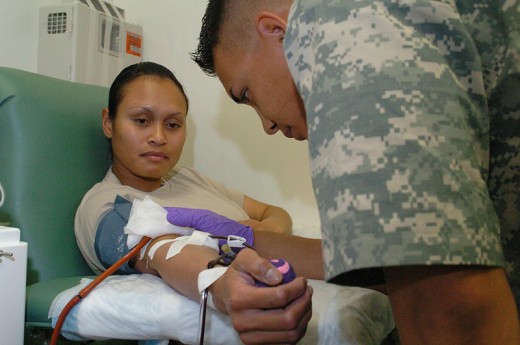
The donor may experience side effects when the anti-coagulant is introduced to the body with the unwanted blood components, as well general feelings of nausea and dizziness may be present. Platelets can only be stored for 5 days after donation, one of the reasons they are always in demand. Donors are required to go through a physical examination, as well as a platelet count and blood typing before donating. The platelet count estimate indicates the amount of blood that must be taken and spun down to yield a full dose. A brief physical exam is done each time to make sure the donor is in good health to donate. Potential donors may be excluded if they take certain medications known to interfere with platelet function. The blood typing is only done once and is done to avoid cross-reactivity of antibody/antigen combinations in the donor and recipient’s blood.
Donating platelets over whole blood is definitely a time commitment, but it is the best way to give platelets. Whole blood donations are separated out into the different components, but platelets represent a small fraction of a donation. Due to the brief lifespan of a platelet donation, as well as the many different reasons a patient needs platelets it is easy to see why this type of donation is in high demand. Donors must be in good health, at least 110 pounds, and have good veins in order to donate. My dad goes into the city every other Sunday morning to give his platelet donation until he hits his 24 donations for a given year. He enjoys chit-chatting with the donation center employees and watching DVDs while he is there. Seeing young patients throughout the hospital on his way to and from the donation center is reason enough for him to continue on.
Comparison of Platelet to Whole Blood Donation
Platelet Donation
| Whole Blood Donation
| |
|---|---|---|
Approximate time it takes to Donate
| Up to a few hours
| Up to 30 minutes
|
Benefits
| For Patient-Single Donor
| |
Downsides
| For Donor-Side effects after donation
| For patient-if used for Platelets, may require multiple donors
|
Donation Schedule
| Once a week, up to 24 times in a given year
| 6 times a year
|








