Blood Types to Remember, ABO, Especially Type Rh
Antibodies of Rh- mother pass thru placenta, get to Rh+ fetus and destroy latter's red blood cells (Illustration from "Rh Blood Type," Internet, Aug. 9,2014

Siblings of father with DD gene and of mother with dd gene are all Rh+

Siblings of father with Dd gene and of mother with dd gene: half is Rh+ and half is Rh-

Blood types are an important factor in blood transfusion and pregnancy
Type A, type B and type O are the common blood types to remember.
My blood type is O. It was first determined when I was about to go under the knife for a partial nephrectomy. That is kidney operation where part of my right kidney was cut out. The stones were still the size of corn kernel. This kidney is still working that I have virtually two kidneys.
Blood typing was necessary in case I needed a blood transfusion during the operation. Fortunately, I am not a bleeder that I did not need a blood transfusion.
My doctors said I am not a good patient insofar as blood transfusion is concerned. The reason is that my blood is type O. That means I cannot have a transfusion of type A or type B. Incompatibility of blood types bring on agglutination or clumping.
Clumping is clotting
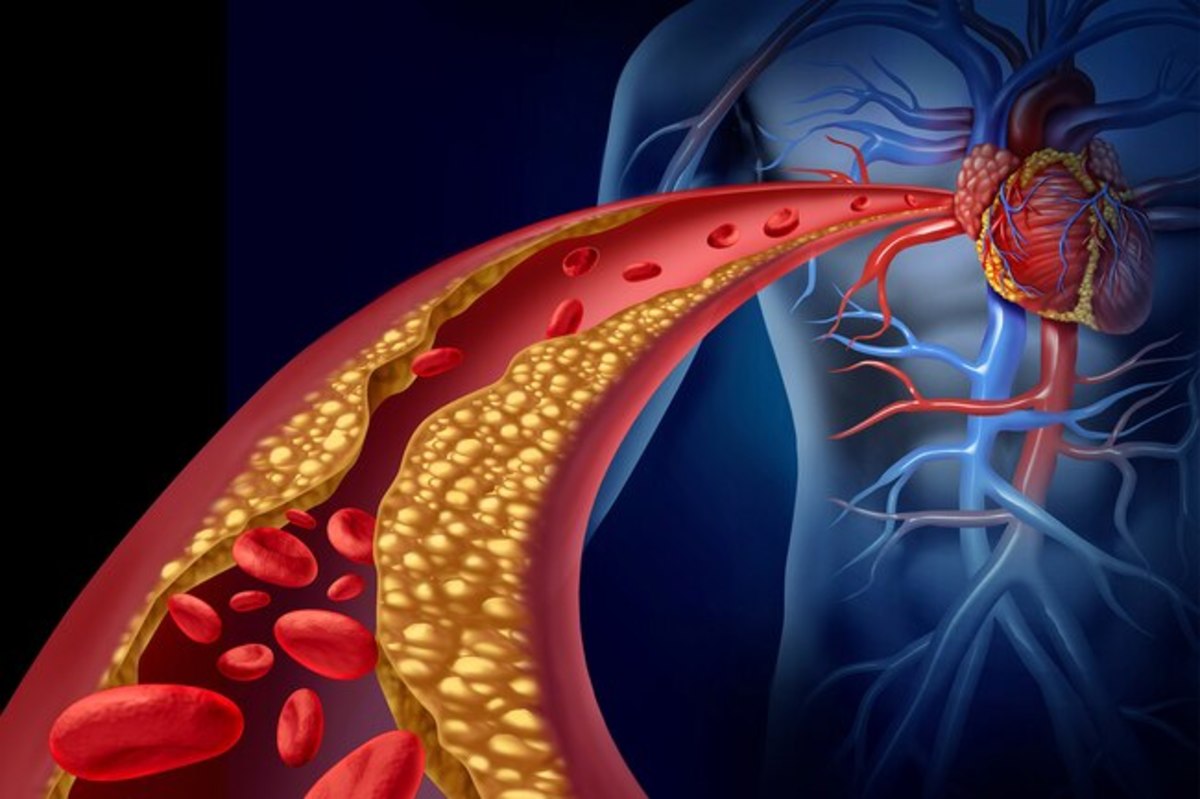
This can bring on a stroke or heart attack. A blood clot blocks flow of blood through an artery like carotid artery that delivers blood to the brain; like coronary artery that delivers blood to heart muscles.
A type A blood produces antigen H in the first layer of its surface. This antigen will reject a blood transfused that is not type A. Blood type B has two layers in its surface, the first one produces antigen H and the second one produces antigen B. These antigens reject blood type other than type B in transfusion.
Who discovered blood types? Karl Landsteiner discovered the ABO blood groups.
Rh Blood type
There is no mysticism in the letters Rh. They are derived from rhesus monkey whose antiserum was used in blood typing.
If your red blood cells agglutinate or clump when mixed with antiserum, your blood type is Rh+. If your red blood cells do not clump in antiserum, your blood type is Rh-. That is, your red blood cells do not produce Rh antigens.
Blood Rh is much more complicated than type A or type B or type O. The reason is that Rh blood produces 45 antigens.
Of course, Rh+ blood type is heritable. Individuals pass on their blood type to offspring with a partner who also has Rh blood type. Rh is controlled by a genes that has alleles, D and d. D is dominant and d is recessive. A gene is a heredity material that comprise a chromosome. The inheritance patterns are shown in tables above.(Tables are adopted from "Rh Blood Types." Internet, Aug. 9,2014).
In the first table, the father is homozygous dominant in having DD. The Mother is homozygous recessive in dd. Children (whose genes are indicated by letters in bold type) born from these parents are all Rh+ in blood type.
In the second table, the father is heterozygous in having Dd. The mother is homozygous recessive in dd. Half of children (whose genes are indicated by letters in bold type) born from these parents are Rh+, half are Rh-.
Mother-fetus incompatibility
When the mother is Rh- and her fetus is Rh+ there is incompatibility between mother and fetus. An antigen provokes the production of antibody that is a protection against the antigen. An antibody destroys blood cells. The antibodies of the mother can cross the placenta and destroy the red blood cells of the fetus. The first pregnancy can be easily remedied. But risks increase in every pregnancy. Europeans are susceptible at about 13%.
There is less risk in blood transfusion than in mother-fetus incompatibility.
Karl Landsteiner and Alexander Wiener discovered Rh blood types in 1940.
Anemia owing to Rh-
Antibodies of Rh- mother clump red blood cells of the fetus. This results in lack of oxygen. Thus the newborn baby may have life-threatening anemia called erythroblastosis fetalis.
This anemia can be remedied while the fetus is still in the womb or after birth of baby. A massive transfusion of Rh- blood is done, at the same time draining blood to flush our Rh+ antibodies from the mother. The fetal Rh+ will be replaced with Rh-. This will be eventually replaced by the baby’s Rh+. Since the baby does not produce Rh+, the Rh+ antibodies from the mother will leave the baby.
This anemia can be remedied by administering the serum Rho-GAM into the mother in about 28 weeks of pregnancy. This treatment is 99% effective.