I have Fibromyalgia, now what?
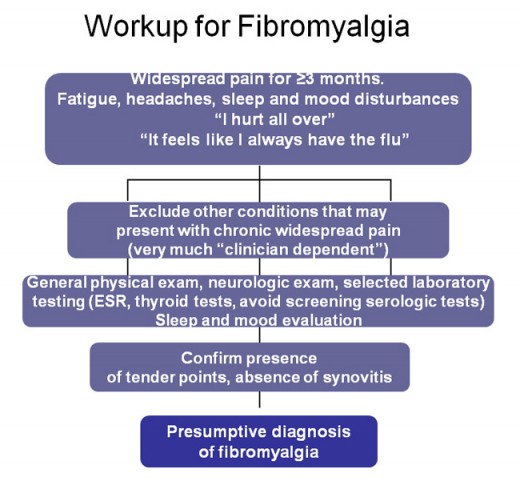
What is Fibromyalgia?
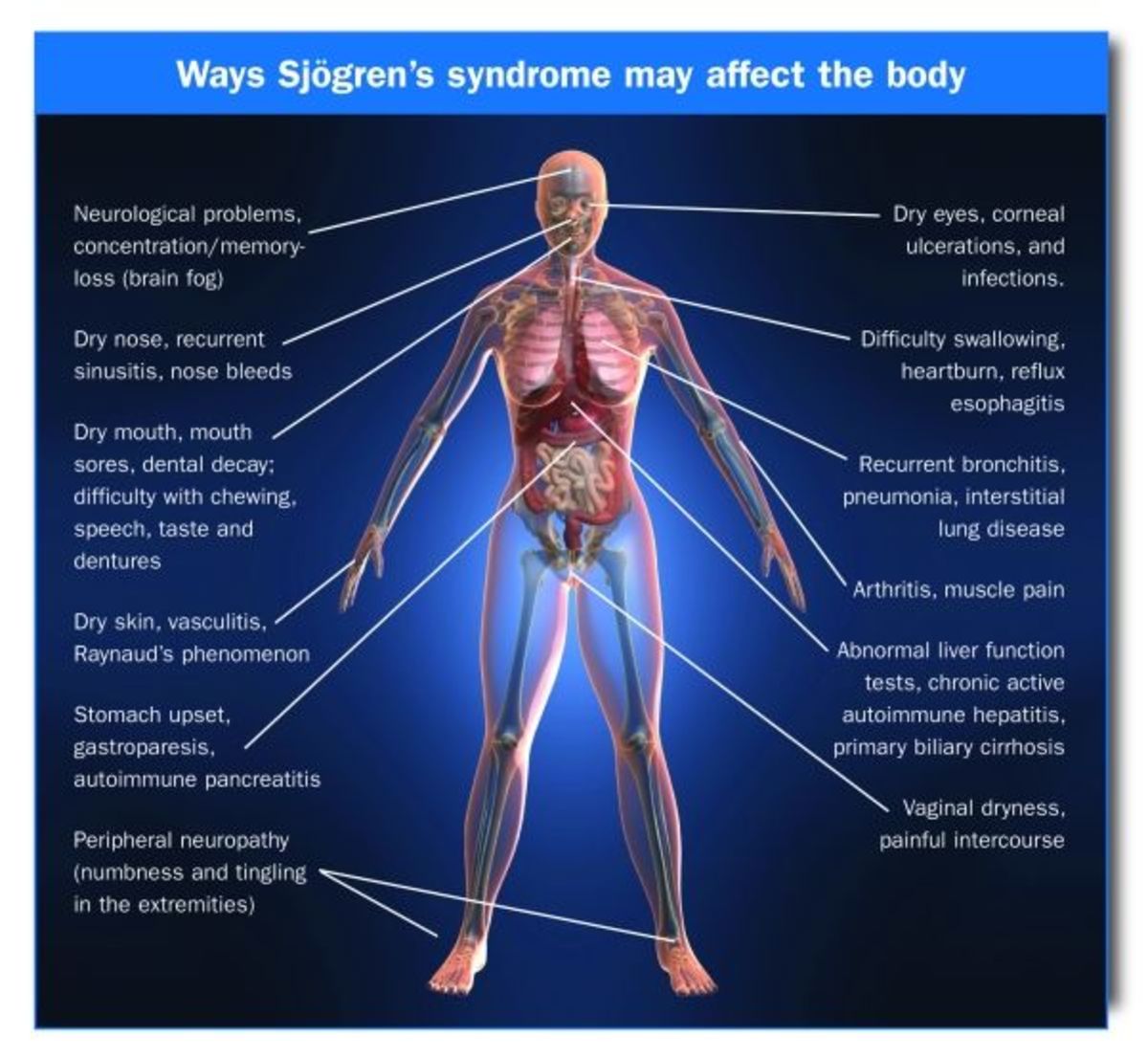
Fibromyalgia, according to the Mayo Clinic (Mayo Clinic), is “a disorder characterized by widespread musculoskeletal pain accompanied by fatigue, sleep, memory and mood issues…that amplifies painful sensations by affecting the way your brain processes pain signals.” It isn’t known at this time exactly what causes Fibromyalgia, and there is no cure at the current time. Fibromyalgia is also referred to as fibromyalgia syndrome , fibromyositis, and fibrositis (National Fibromyalgia Association). Fibromyalgia can range from mild to debilitating, and can interfere with even the most basic of daily tasks.
Fibromyalgia: What it is not
At this point, researchers claim to have ruled out auto-immune disease as the cause of Fibromyalgia. This syndrome is not contagious, but does appear to have possible genetic ties (Mayo Clinic). Fibromyalgia and Chronic Fatigue Syndrome are often comparable conditions, but are two separate conditions and should be treated differently.
Signs & Symptoms of Fibromyalgia Syndrome (FMS)
Pain: Widespread, unexplained, chronic pain is the most common complaint from patients diagnosed with FMS (National Fibromyalgia Association). The pain can migrate to all parts of the body, and often occurs most at “tender points” throughout the body. Many patients also complain of numbness, tingling, burning, and stiffness, as well as citing that the pain may be better or worse based upon outside factors such as weather, altitude, physical activity, and stress.
Fatigue and sleep disturbances: Many people who suffer from Fibromyalgia also have sleep disorders such as Restless Leg Syndrome, Sleep Apnea, or may simply have fatigue due to restless sleep disturbed by pain and stiffness. Patients with Fibromyalgia have been found in laboratory studies to have a higher than average amount of “non-restorative” sleep, where the stage 4 deep sleep is never achieved (James, 1994). The fatigue experienced by Fibromyalgia patients is more of an exhaustion which affects occupational, personal, social, and/or educational activities.
Mental/Memory disruptions: Many people with Fibromyalgia report having issues with recalling information and concentration. This phenomenon is often referred to as “fibro fog”.
Do you have Fibromyalgia?
Have you been, or do you suspect you should be, diagnosed with Fibromyalgia?
Co-existing Conditions
There are several conditions that people with Fibromyalgia may also have. Some of the most common co-existing conditions of Fibromyalgia sufferers include fatigue, anxiety, depression, irritable bowel syndrome (IBS), endometriosis, headaches (tension and/or migraine are most common), bipolar disorder, lupus, arthritis, and Raynaud’s Syndrome. Not everyone with FMS will have all of these conditions, and not everyone with these conditions will have Fibromyalgia, but often times they do coincide, though the exact link is not known at this time.
Risk Factors
Risk factors for developing FMS can include your gender, genetics, history of rheumatic diseases, and physiological abnormalities. This list is not all inclusive, as research into the causes and contributing factors for this syndrome are still very much in their infancy.
Research has shown that 80-90% of those diagnosed with Fibromyalgia are women (What is Fibromyalgia, 2011). This disorder also appears to be seen in families, among siblings or mothers and their children (National Fibromylagia Association).
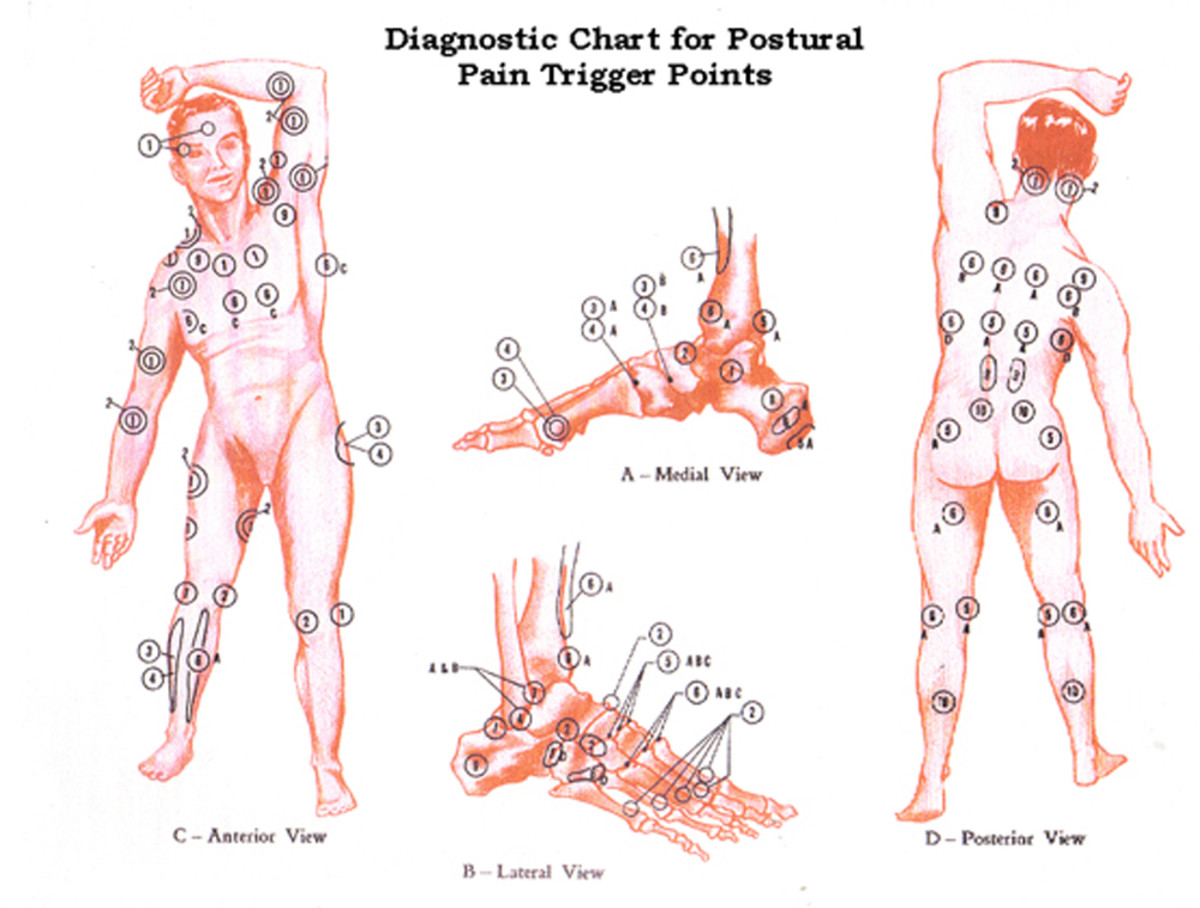
Fibromyalgia Tender Points Chart
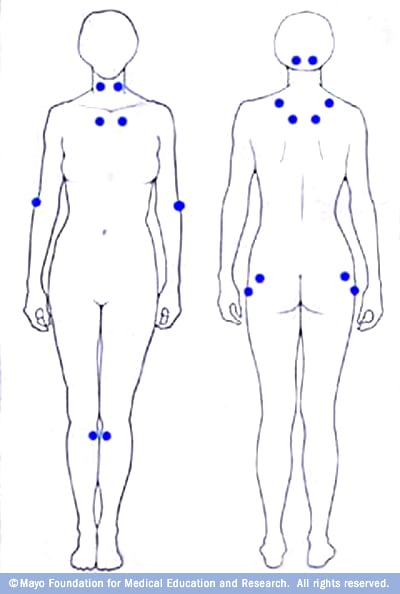
Tests and Diagnosis
While there are currently no tests that can be ordered to diagnose Fibromyalgia, in 1990 the American College of Rheumatology established two criteria for diagnosing FMS: Widespread pain lasting at least 3 months, and at least 11 positive tender points out of a possible of 18 (Mayo Clinic). While these are the main guidelines, adopted by the World Health Organization in 1992, there are newer criteria to consider as well, such as no other underlying conditions that could be the cause of the pain.
Doctors will most likely order blood tests in an effort to rule out other conditions with similar symptoms. Some of the blood tests that may be included are a complete blood count (CBC), Erythrocyte sedimentation rate, and Thyroid function tests. It is possible to have thyroid disorders and Fibromyalgia, but ruling out these as primary causes of the symptoms is helpful in proving your condition to be FMS.
Treatment
There is unfortunately no one treatment for Fibromyalgia that will work for everyone. Clinical trials are still being conducted to test pharmaceuticals, as well as group studies on the effects of sleep management and physical activity levels on pain and other symptoms. While there is no one miracle treatment for this condition, many people do see some improvement with managed care.
Currently, the U.S. Food and Drug Administration (FDA) has approved medications such as Lyrica, Cymbalta, and Savella for the treatment of FMS. Pain may be managed through non-narcotic pain relievers such as Tramadol, or low doses of antidepressant medications. Lidocaine or “Trigger Point Injections” may be used to alleviate localized areas of pain. Stretching and light, regular exercise is also highly recommended.