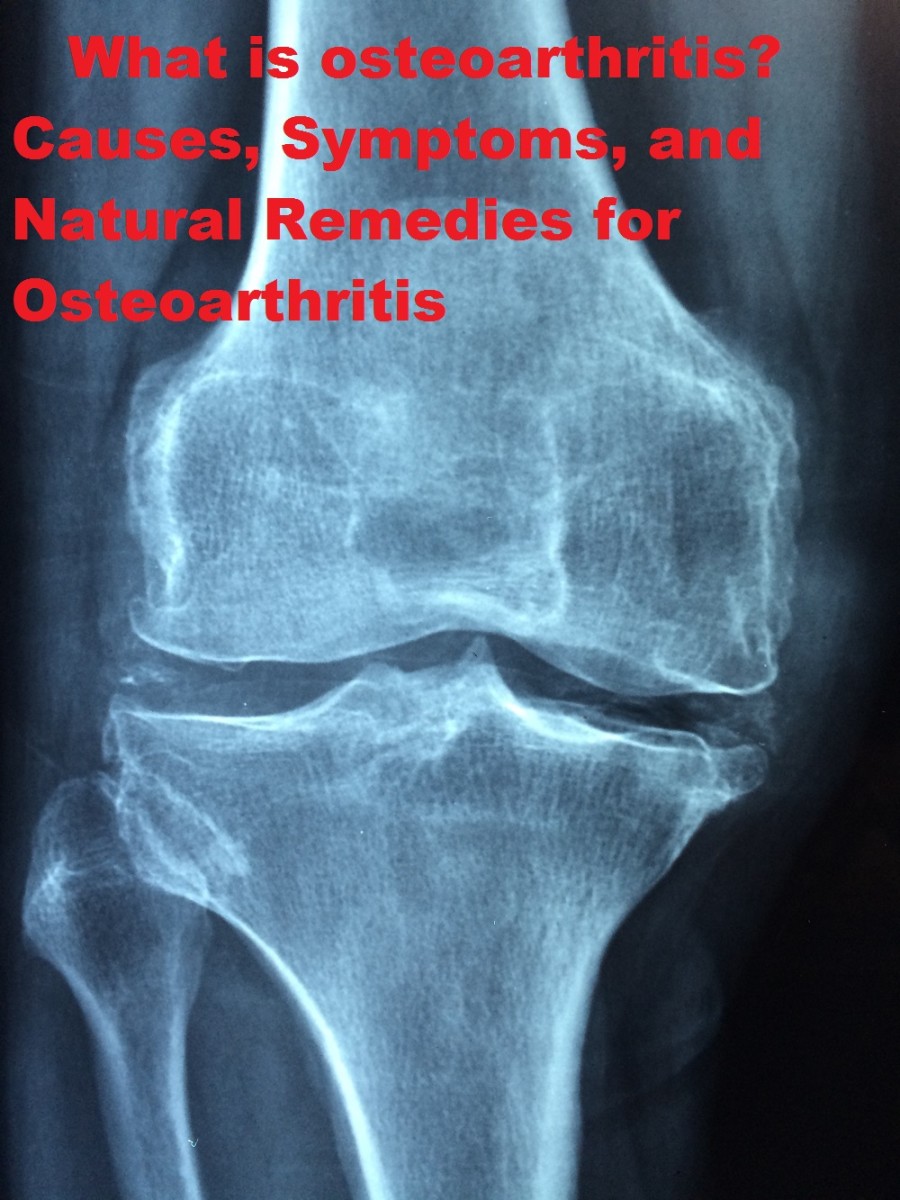
Hip Osteoarthritis (OA)

What is Hip Osteoarthritis?
Arthritis of the hip causes a great deal of disability, especially among older people. Hip arthritis causes pain and dysfunction. This makes it more difficult to lead an active and fulfilling life, which, in turn can contribute to depression and cognitive and physical decline. Pain with walking also makes the risk of falling more likely. Hip fractures that result from a fall are a leading cause of physical and mental decline in older people.
Osteoarthritis of the hip refers to the degeneration of the cartilage hip joint. Osteoarthritis may also be referred to as degenerative joint disease. Cartilage lines and protects joints and can be thought of as a type of shock absorber. As the cartilage thins and wears away, the joint becomes inflamed. Pain and difficulty with movement result.
Hip Osteoarthritis Causes
Osteoarthritis (OA) is largely considered to be the result of age and use. Degeneration of the cartilage in joints happens over time. A joint that experiences higher than average use or has had previous injuries may degenerate more rapidly. For example, long-distance runners may have more knee and hip degeneration. Hip degeneration may be more prevalent in high level track-and-field runners and basketball players, as well.
- Hip osteoarthritis is seen more frequently in older people.
- Some high level athletes are at risk for hip OA due to significant overuse of the joint.
- Being overweight is a more likely risk factor for hip OA than is athletic activity.
- Genetics may play a role in the rate of cartilage degeneration.
- Previous injury is a risk factor for degenerative joint disease.
Summary of Symptoms of Osteoarthritis of a Joint
Joint discomfort or pain
Joint stiffness or limitation of movement
Joint swelling
Pain gets worse with activity, especially weight-bearing activity
Pain improves with rest
Joint seems to "catch" or "give out"
Symptoms progress over time
Symptoms of Hip OA
Hip osteoarthritis causes discomfort early in the process. This evolves into more significant pain and stiffness as time goes on. Swelling (although difficult to detect around the hip) and dysfunction of the joint also begin to be more noticeable. As more cartilage wears away, there is less padding between the bones.
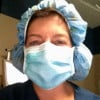
The top of the femur (upper leg bone) has a ball on the end of it. This ball fits into a socket on the side of the pelvis to form the hip joint. As the cartilage between these bones erodes, the pain gets even worse with activity and movement. Catching, clicking, "giving out", sharp pains and limitation of movement further indicate disease progression. When there is bone to bone contact due to complete erosion of the cartilage, the pain and dysfunction may be debilitating and limit the ability to walk.
The pain of degenerative joint disease of the hip may be felt in the front of the hip, the back of the hip, the groin, the front of the thigh or the buttocks. Because of the varied presentation, the diagnosis may not be made right away.
Anatomy of the Hip Joint & Description of Osteoarthritis of the Hip
What about Glucosamine/Chondroitin?
Once osteoarthritis of the joint develops, many people will try over-the-counter supplements to treat the disease or the symptoms. Glucosamine and chondroitin remedies are among the most popular for OA. They are not harmful, but are they helpful?
Well, the results are mixed. In one study called GAIT, a small subset of participants did get significant relief with the combo of the two supplements together. There is some question as to whether the sample size is large enough to be valid and further studies were recommended. And, while symptoms were improved, there was no evidence on X-ray or other studies that the rate of cartilage loss was slowed when compared to placebo.
More recent studies do not corroborate the finding of better pain relief with glucosamine with or without chondroitin.
Overall, it is thought that these supplements do not provide significant benefit for the majority of osteoarthritis patients. And, while there are some concerns about side effects and complications in lab studies, none of significance have been found in actual human trials.
So, they may not be harmful, but aren't likely to be of real benefit, either.
A good summary of these findings can be found here:
GAIT STUDY: http://nccam.nih.gov/research/results/gait/qa.htm
OTHER INFO: http://www.quackwatch.com/01QuackeryRelatedTopics/DSH/glucosamine.html
What do you think?
If you have taken a glucosamine/chondroitin supplement for OA, did it help you?
Treatment of OA of the Hip
Once the damage is done from osteoarthritis of the hip, it cannot be reversed. The cartilage will not regenerate to any significant degree.
The purpose of treatment in the early stages of the disease is to relieve symptoms and to slow or stop further degeneration. To achieve this, it is recommended that you:
- Rest your joint when pain occurs.
- Don't participate excessively in weight-bearing activities such as running or basketball.
- Do exercise to strengthen the muscles around the joint. Swimming and biking are excellent choices for hip arthritis.
- Lose weight and maintain a healthy weight.
- Treat pain and inflammation with NSAIDS (non-steroidal anti-inflammatory drugs) such as ibuprofen.
- Follow up with your doctor if symptoms worsen or change. Ask if injections will help you.
- Consider formal physical therapy to learn how to care for a hip joint with OA
SURGICAL TREATMENT:
If you have severe degeneration, the above measures will not significantly improve your pain or your lifestyle. In that case, surgery to replace the hip joint could be considered. This is major surgery and creates physiologic stress on the whole body, so discuss this option thoroughly with an orthopedic surgeon AND your primary medical doctor to make sure you are a good candidate for hip replacement surgery.
As expected, surgery is reserved as a last resort therapy. It does make a significant impact on pain and improving lifestyle and activity for people who are good candidates for the surgery.