Measuring Mental Status Using the MMSE

What is Mental Status and What is the MMSE?
Mental capacity, mental status and cognitive functioning are terms used to describe the mental skills people use in their every day lives. Mental capacity includes memory, attention, concentration and ability to calculate. A full mental status assessment is completed by a trained professional, and would include other aspects of a person’s mental health such as mood, feelings, behavior, attitudes, perceptions, thoughts, and more. One part of the complete assessment is a test called the mini mental status exam or MMSE. The MMSE focuses on measuring a person’s cognitive functioning. The MMSE can be completed by anyone who knows how to administer and score it. It can be used to get a quick sense of a person’s mental state or to understand the extent of a person’s deficits.
A person’s mental capacity is affected by a number of factors. Age is often associated with some mental decline, especially in memory. Change in mental capacity due to age alone is not typically sudden or extreme. A sudden and severe decline can indicate illness or disease requiring medical attention. A number of factors can contribute to mental decline, such as poor nutrition and vitamin deficiencies, depression, and drug interactions. Mental decline in these instances can often be treated and reversed.
The MMSE was designed in 1975 by M. Folstein, and is sometimes called the folstein test. It was designed to assess the cognitive functioning of older adults. It assesses orientation (a person’s awareness of time, place and person), attention, recall, language and ability to follow directions. The current form of the exam hasn’t changed much since 1975. If every question on the MMSE is answered correctly, the maximum score is 30. The MMSE can be completed in 5-10 minutes, and the results are consistent with other more time consuming tests of cognitive functioning.
The MMSE is the most widely used tool to assess cognitive functioning. It is cited in most research related to cognitive functioning or patient responses to treatments and interventions. It is required to be completed when determining if a person is an appropriate candidate for some medications, such as Aricept and Excelon. The MMSE is used to assist with the diagnosis of dementia, but it is not used alone to diagnose dementia. It is part of a full diagnostic work up.
The primary reason to use the MMSE is to get a measure of a person’s cognitive functioning, and then use the result or score to assist with the person’s treatment and care planning. For example, if a person scores low on time orientation, caregivers can ensure that calendars and clocks are available to help with time orientation. The MMSE is typically repeated following a treatment episode or changes in circumstances, in order to record any changes in response to treatment, intervention or changed circumstances.
Administer and Score the MMSE
There are guidelines for administering and scoring the MMSE. Following the guidelines can improve the usefulness of the results. There are also certain materials that will need to be prepared and available before beginning to administer the MMSE. One of the strengths of the MMSE is that the required materials are readily available or easy to get.
Materials and Testing Conditions
- Watch, pencil, eraser, blank piece of paper
- Piece of paper with CLOSE YOUR EYES written in large letters.
- A drawing of two five sided figures that make a four sided figure when lines intersect. (see diagrams below)
- Complete questionnaire.
- Ensure hearing or visual aids are available and in good working condition
- Ensure setting is comfortable with good lighting and ventilation
- Establish rapport with examinee and explain the nature of questions to be asked
- Refer to the MMSE as a standard questionnaire and avoid using “memory test.”
- Allow the examinees to answer questions themselves without prompting.
- Make sure any prompts are removed such as calendars or a newspaper with a date on it.
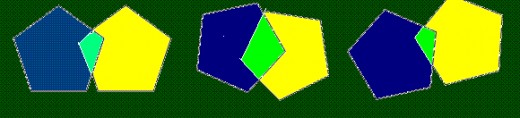
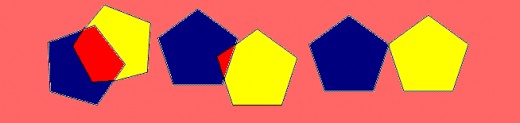
Instructions for administering and scoring the MMSE are available when the MMSE is purchased from Psychological Assessment Resources, Inc. There are 11 questionnaire items. In general, one point is scored for each correct response. Some of the questionnaire items contain several responses. For example, a person might be asked to repeat the name of three objects and a point is scored for each object named. A person is asked to spell a word backwards and is awarded a point for each letter in the correct order. Incorrect answers earn 0 points. A question can be asked a maximum of three times. If a person does not respond, a score of 0 is recorded. The highest possible score is 30.
Interpreting the Results
Note: Contact the person's doctor if there is a score of less than 24/30 or a significant decrease from a previous score.
Score
| Cognitive Functioning
|
|---|---|
24-30
| normal range
|
20-23
| mild cognitive impairment
|
10-19
| moderate cognitive impairment
|
0-9
| severe cognitive impairment
|
Results are not considered valid if the person being tested does not speak English or has poor language skills. Likewise, the results are not valid if the person tested has problems with vision or hearing, is very ill or in pain, or has a tremor.
Decline in cognitive functioning is a normal part of aging, but individual scores can vary according to a person’s level of education. A person with a 4th grade education might have a high score of 22 at age 50 and a low score of 20 at age 80. A college graduate might score 29 at age 50 and 27 at age 80.
The MMSE score relates to cognitive functioning, not a person’s functional ability. A person with a score of 20 or less might struggle with managing finances and medications, driving, shopping and preparing meals. They may still be able to manage hygiene, grooming, dressing and eating. When cognitive and functional declines occur gradually over a number of years, the changes may not be noticed by a family member or caregiver who interacts with the person daily.
Condition/Disorder
| Deficits Revealed in MMSE
|
|---|---|
Dementia
| People with dementia may not complain of memory problems. They might continue to try to get the correct answers, and not be bothered by incorrect answers.
|
Alzheimer's
| Usually the first deficit is in short term memory/recall, as measured by difficulty recalling the three items in Q5. Orientation to time is lost first, followed by loss of orientation to place. Language deficits appear later.
|
Vascular
| Deficits are “patchy.” May have speech/language problems earlier than in Alzheimer’s.
|
Delirium
| Clouding of consciousness might be apparent with difficulties concentrating and irritability. It may difficult to keep the person’s attention long enough to complete the testing. Visual hallucinations may be present. They may be drifting in and out of consciousness and alertness. The MMSE should be repeated once the delirium has resolved, as the score obtained while the person is delirious is not a true assessment of their cognitive functioning.
|
Depression
| A person with depression is more likely to be concerned about and complain of problems with memory and concentration, but their scores do not reveal difficulties in memory and concentration. Their scores are within normal range on the MMSE. A person with depression may take longer to answer questions, may answer, “I don’t know,” or may not attempt to answer. They may be concerned about their performance and incorrect answers, or give up on a task. In conversation, they may not show obvious short term memory loss or difficulty finding words.
|
Using the Results in Treatment and Care
The results of the MMSE can help with planning care. If the person had problems following three stage commands in question 8, then commands can be given in single steps. A person who has difficulty with time orientation can be prompted to use guides available in the environment; calendars, clocks, etc. A person who has difficulty understanding a written command, may need to have rules, instructions, reminders, etc communicated differently.
The MMSE, in summary, is a fast and reliable way to measure cognitive functioning. It can help with diagnosis of cognitive conditions and can be useful in identifying health issues. The results of the MMSE can help with planning treatment and care.
Purchase the MMSE
SAGE - The Self Administered Gero-cognitive Exam
- SAGE - A Test to Measure Thinking Abilities
Contact information Douglas W. Scharre, MD Director, Division of Cognitive Neurology The Ohio State University Wexner Medical Center (614) 293-4969 scharre.1@osu.edu