Trauma Flap
Indications
• Elevated intracranial pressure (ICP) is one of the most common causes of death and disability following severe traumatic brain injury and ischemic stroke.
• There have been no new medical treatments for elevated ICP in more than 90 years. A decompressive craniectomy may be a useful surgical option in ICP that is refractory to medical treatment. Decompressive craniectomy is also performed as a prophylactic measure in the emergency setting during evacuation of a traumatic subdural or epidural mass lesion when the bone is not replaced in anticipation of postoperative elevated ICP as predicted by computed tomography (CT) scan or the appearance of the brain at surgery.
• Decompressive craniectomy, when performed correctly, can reduce ICP and prevent cerebral herniation and death. Successful decompressive craniectomy allows the brain to swell, reducing the risk of neurologic injury from elevated ICP. In most instances, decompressive craniectomy also reduces the intensity of medical management in the intensive care unit.
Contraindications
• Decompressive craniectomy is most often performed in the setting of life-threatening, impending cerebral herniation. It is important that the surgical and critical care teams and the family members know the dire prognosis of many of these cases to avoid unrealistic expectations. Decompressive craniectomy is well established to treat elevated ICP, but it is less certain which patients are most likely to benefit from this procedure.
• Older patients and patients with limited brainstem reflexes and a low Glasgow Coma Scale score from the time of injury may be at greatest risk for a poor outcome.
Planning and positioning
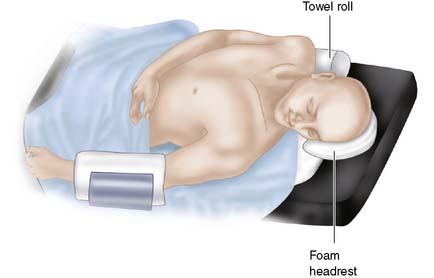
Trauma Flap 12-1: For unilateral decompressive craniectomy, the patient is positioned supine with a small towel roll under the ipsilateral shoulder and the head turned to the contralateral side. In the setting of trauma, it is important to position the patient with cervical spine precautions. Care should be taken not to compress the jugular veins, which can lead to decreased venous return and further increase in ICP. The head can be rested on a foam headrest; this allows for repositioning of the head intraoperatively if venous outflow obstruction is suspected. We generally prefer not to use a rigid head holder with pins unless we are certain that there are no skull fractures.
Procedure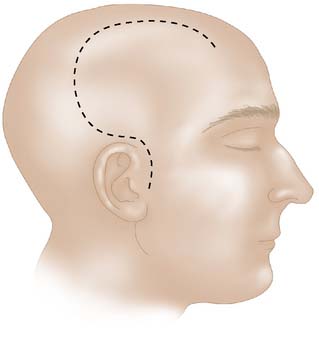
Trauma Flap 12-2: Skin incision. After the head is shaved and prepared, a large reverse question mark incision is made, beginning at the zygoma extending far behind the ear, then curving a few centimeters lateral to the sagittal suture, anteriorly to the hairline. If possible, the superficial temporal artery should be protected to preserve the blood supply to the flap.
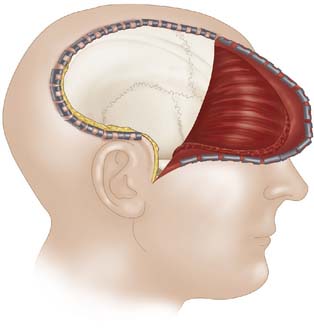
Trauma Flap 12-3: Muscle and soft tissue dissection. The incision is carried through the subcutaneous tissue, including the temporalis, down to the cranium. The musculocutaneus flap is reflected anteriorly and fixed with scalp hooks. Ideally, this muscle dissection extends down to the root of1 the zygoma and as far below the keyhole as possible, to maximize the temporal decompression achieved.
Read more Trauma Flap Part 2