Treatments for Scuba Diving Decompression Sickness

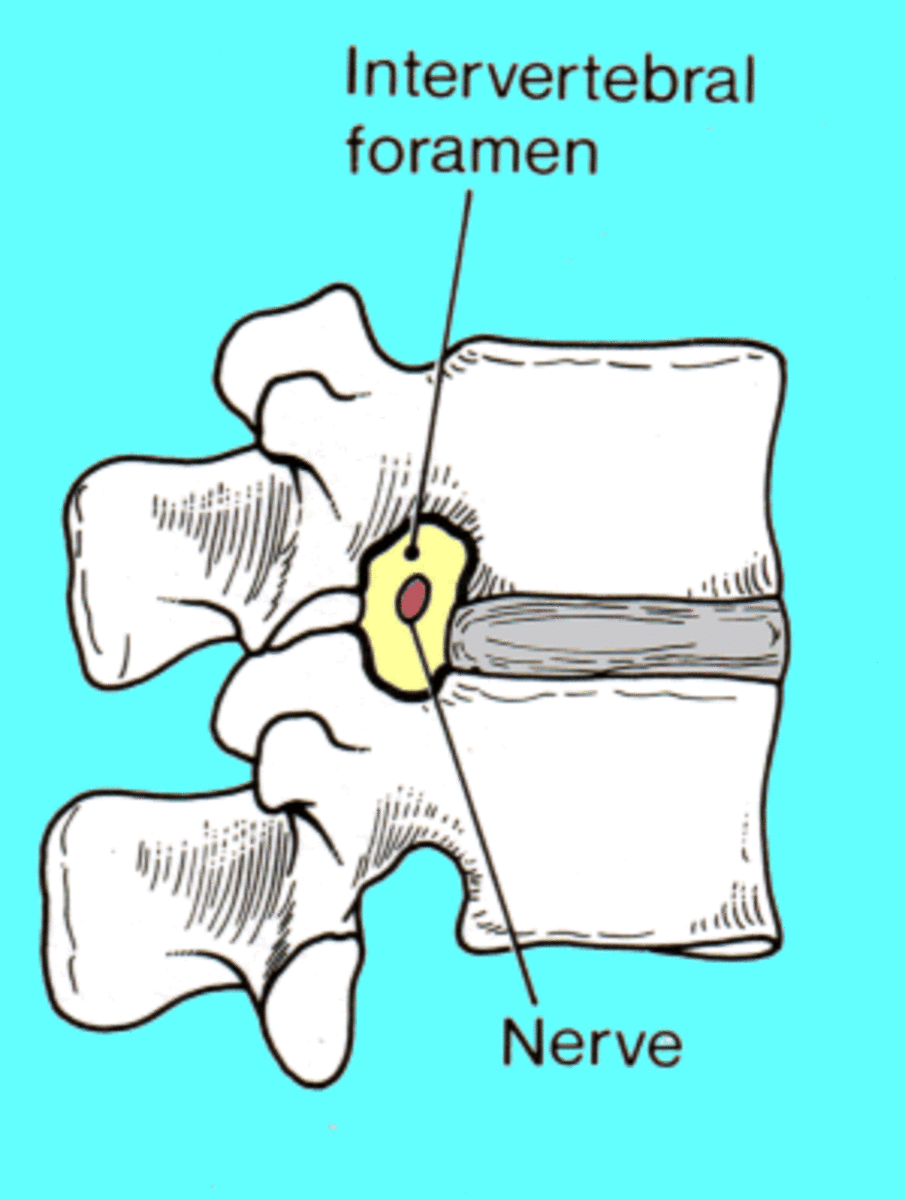
The main danger scuba divers face is Diving Decompression Sickness (DCS). It occurs when divers spend a great deal of time at great depths then rise back up to surface too quickly. The sudden change in pressure can cause painful, even life-threatening, symptoms. The deeper the dive, the greater the risk to the diver.
What Is Decompression Sickness (DCS)?
DCS is defined as a sudden reduction of pressure on the body resulting in the formation of nitrogen bubbles in the blood, tissues, and joints. It can happen when divers rise too quickly following extended periods at greater underwater depths or when fighter pilots or astronauts ascend too quickly to higher elevations above sea level. Other names for DCS include divers’ disease, the bends, and caisson disease.
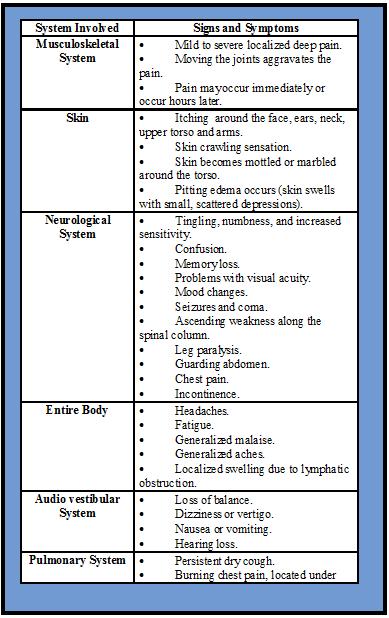
Symptoms of Decompression Sickness
Symptoms of DCS (as shown in the table above) range from joint pain to paralysis and death. The severity of symptoms vary from one day to the next and from one person to the next. Symptom type and severity may be affected by the person’s physical condition, whether they’ve been sick, whether they have been diving recently, or even whether they’ve had alcohol to drink within 24 hours of diving. Symptoms may occur anywhere from one hour to 48 hours after coming up from a dive
Treatments for Decompression Sickness
The best treatment is prevention. Prevention includes:
· Limiting ascent rates to about 33 feet per minute, with a decompression schedule that fits the circumstances of the dive (diver’s height and weight, depth, length of the dive time).
· The diver should be in good health before going on a dive.
· Diver should have proper scuba training.
· Divers should never dive alone, but work on a buddy system.
· Scuba equipment should be in good working order.
· Divers should have a list of emergency numbers and contact information on all dives.
· Divers should avoid flying or mountain climbing within 24 hours of a dive.
Once symptoms start, they should be treated in an emergency room, beginning with oxygen therapy and ranging anywhere from symptomatic relief to hyperbaric chamber treatments. Physicians will begin with a basic history and physical exam to ascertain the parameters of the dive and the divers’ symptoms and their current physical condition. This will determine the course of treatment. Treatments include:
· Blood pressure, heart and respiratory rate, and temperature.
· Blood oxygen levels will be determined using a finger or earlobe sensor.
· Patients will be given oxygen through a mask, beginning with 100% O2, dropping it as the patient’s condition improves.
· Patient’s will be given intravenous fluids to keep them hydrated and prevent their systems from shutting down.
· Patient’s may be given recompression therapy (hyperbaric chamber treatments) to help the break down the nitrogen bubbles and help them reabsorb into the blood and get naturally processed by the body.
· Pain medication may also be given to help make patients comfortable.
· Nausea medication may be given for those suffering from nausea and medication.
And of course, patients will usually require a follow up exam to make sure there are no lingering effects of the DCS and to determine if he or she is okay to dive again in the future.
Resources
Wikipedia. Decompression Sickness.
http://en.wikipedia.org/wiki/Decompression_sickness
e-Medicine. Scuba Diving: Barotrauma and Decompression Sickness.
http://www.emedicinehealth.com/barotraumadecompression_sickness/article_em.htm
Divers Alert Network. Decompression Illness: What Is It and What Is the Treatment?
Bookspan, Jolie, PhD. Scuba Doc. Decompression Sickness.
http://www.scuba-doc.com/dcsprbs.html
US Navy Dive Manual, Operational Medicine. Diving Disorders Requiring Recompression Therapy.
http://www.operationalmedicine.org/TextbookFiles/USNDiveManual/Chap20.pdf