Gestational Diabetes - Symptoms and Management
Gestational diabetes is diabetes that presents during pregnancy. It is the inability of the mother’s body to convert food into energy because the body is unable to respond to insulin.
Insulin is produced by an endocrine gland, called the pancreas, and converts carbohydrates and starches into sugar (glucose). Insulin moves the glucose from the blood to the tissues and cells of the body in order to create energy.
Symptoms of Gestational Diabestes
Sometimes, there are no symptoms of gestational diabetes, or the symptoms of gestational diabetes are very mild and pose no life-threatening risks to the pregnant mother.
Symptoms may include:
--blurred vision
--fatigue
--frequent infections of the bladder, vagina, and/or skin
--increased thirst
--nausea and/or vomiting
--weight loss
Risk Factors for Gestational Diabetes
There are some health issues that contribute to a woman's risk of acquiring gestational diabetes:
--women who are 25 or older when they are pregnant
--a family history of diabetes
--giving birth to a baby weighing over nine pounds or giving birth to a baby with birth defects
--high blood pressure
--too much amniotic fluid
--an unexplained miscarriage or stillbirth
--overweight prior to being pregnant
How Gestational Diabetes is Diagnosed
Gestational diabetes often begins around the 24th week of pregnancy, and a simple blood test, called a glucose tolerance test, between weeks 24 and 28 will diagnose the disorder; however, for women diagnosed with gestational diabetes in a previous pregnancy, the test might be done as early as week 13.
The glucose tolerance test involves drinking a sweetened liquid and then having your blood tested an hour later in order to determine how your body metabolized the sugar. If the test is abnormal, an additional test will be scheduled. You will be required to fast and have your blood drawn four times, usually, within a three-hour period.
Gestational diabetes affects approximately 4% of all pregnant women. It is important to monitor blood glucose levels and control it through proper diet, exercise, and sometimes insulin therapy. If gestational diabetes is left undiagnosed or unmanaged, it can lead to pregnancy complications and may harm the baby.
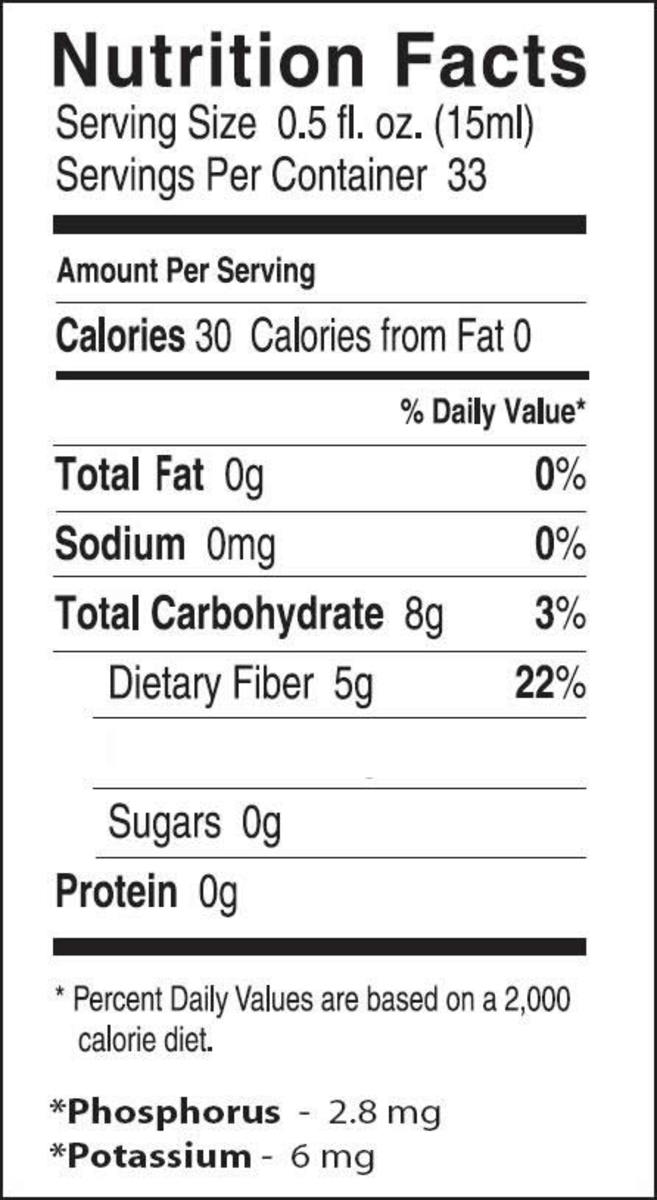
Diet for Women with Gestational Diabetes
By maintaining a healthy diet during pregnancy, gestational diabetes can be controlled. Diets should be moderate in fat and protein with controlled levels of carbohydrates and little or no foods that contain sugar. Women with gestational diabetes should eat three small meals a day that include a healthy variety of foods with a small snack in between meals, never skipping a meal.
Carbohydrates are found in foods that people often think of as the healthier foods like yogurt, corn, fruit, milk, and peas. Eating high-fiber, whole grain carbohydrates are much healthier because they are digested more slowly and include carrots, brocolli, and spinach.
Women diagnosed with gestational diabetes should utilize a cookbook aimed specifically at controlling diabetes and/or speak with their physician in order to obtain reliable and legitimate menu plans.
How Gestational Diabetes Affects The Baby
During pregnancy, the mother will pass on high blood sugar levels to her developing baby. As a result, the baby’s pancreas will work harder at producing insulin. Because the baby is receiving more energy that what is required for normal nourishment and development, the baby stores the excess energy as fat. This increases a baby’s risk for obesity and even diabetes type II as an adult.
Because the extra energy is stored as fat, there can be complications during childbirth, including shoulder damage from delivery, low blood sugar levels at birth, and breathing problems. It may also cause the need for a c-section.
Although it is unclear what causes gestational diabetes, it is thought that the placenta, while giving nourishment and providing hormones to the baby necessary for growth and development, may somehow block the action of insulin in the mother’s body.
Just because a woman has been diagnosed with gestational diabetes does not mean that she had it prior to being pregnant or that she will continue to have diabetes after her pregnancy.
By keeping to a diet for gestational diabetes, exercising and seeing a physician regularly for check-ups, a healthy, normal pregnancy and delivery of a healthy baby can be achieved.