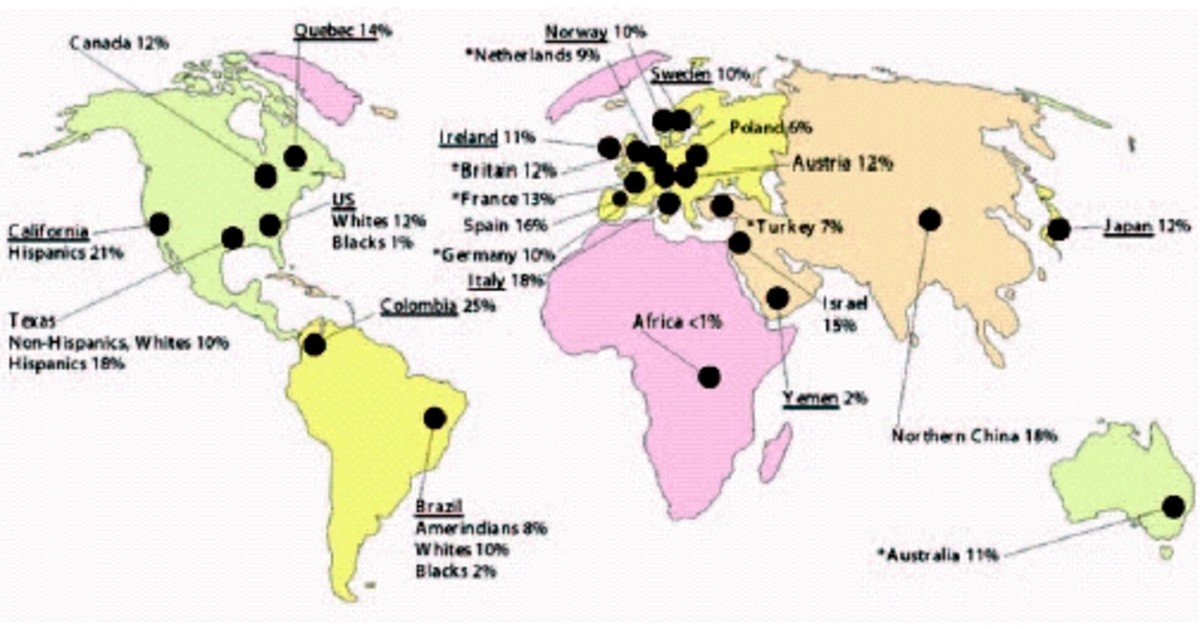
Disability and Chronic Illness: A Look at How They are Handled in Nursing

The Differences
According to LeBlanc and Jacelon (2016), one of the goals of self-care, self-management, and disease management is the “prevention of disabilities while living with chronic disease.” This statement indicates that the two terms are completely different. A disability is something that significantly impairs one’s daily functioning. AIDS is a chronic illness and may not kill an individual for many years. People living with AIDS have to alter their daily routine, but not necessarily to the point of being non-functional. They can still work, live by themselves, and transport themselves. A person living with AIDS who develops an infection in the nervous system that causes permanent damage to the point that they lose partial control over their body has a disability. Their inability to self-manage qualifies them for having a disability.
Ethics of Disability
According to LeBlanc and Jacelon (2016), access is not guaranteed. People with disabilities may have certain things that need to be prepared in order for them to avoid harm (wheelchair access, hand rails, etc). These things are not always thought of and it is ethically important as well as legally responsible for organizations to accommodate people with disabilities when needed. There is also an issue of not assuming a level of competence for a patient that is not present. While empowerment is important, it does no good to a patient to assume they are able to self-manage at a level of which they are not capable.
Ethics of Chronic Illness
There exists an assumption in health care that education is noninvasive, and therefore, does not require informed consent. Many chronic illnesses have modifiable factors such as diabetes, heart disease, chronic obstructive pulmonary disease, and HIV. These modifiable factors are an important part of nursing care and there exists an ethical obligation for the health care community to attempt to stop many of the instances of these illnesses before they start through preventative care methods such as education (Leblanc & Jaceolon, 2016).
The second ethical consideration is related to the first. Though certain conditions have modifiable factors, it is important not to blame people with chronic illnesses for their conditions. There is a point where education turns into shaming, and this serves no ethical purpose (LeBlanc & Jacelon, 2016)).
Where Nurses Come In
Education is a very important role the nurse plays. As mentioned before, it cannot be assumed that patients and family understand something. Knowledge is power, and part of empowering people living with chronic health conditions is providing them with necessary knowledge. In order for a patient and family to achieve comprehensive self-management, nurses can provide education on conditions and trainings on complicated medication and equipment which the patient may require (LeBlanc & Jacelon, 2016).
According to LeBlanc and Jacelon (2016), advanced practice RNs can facilitate group visits in primary care facilities for patients with chronic conditions. These visits are efficient since many of these patients will have the same need. Furthermore, they provide support by allowing the members of the group to share with one and other. People may learn about their conditions from other members as well as the RN running the group.
Reference
LeBlanc, R., & Jacelon, C. (2016). Self-management. In P. Larsen (Ed.), Lubkin's chronic illness: Impact and intervention (9th ed.). Retrieved from ovidsp.tx.ovid.com
© 2017 Vince