General Consideration In The Diagnosis And Treatment Of Hyperthyroidism And Goitre
Hyperthyroidism
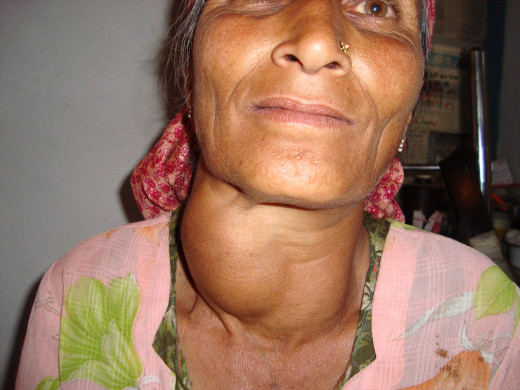
Diagnosis
In florid cases, clinical diagnosis is easy. Subclinical cases may be missed if thyrotoxicosis is not kept in mind. In all cases, it is advisable to confirm the diagnosis and establish its severity by investigations.
Differential diagnosis: When the symptoms are equivocal, hyperthyroidism may be mistaken for anxiety state, tuberculosis, diabetes or primary muscle disease. In anxiety states the palms are cold and moist, whereas in hyperthyroidism they are warm and moist.
Euthyroid Grave’s disease: This is a condition in which exophthalmos is present with or without thyroid enlargement. There may not be signs of overt hyperthyroidism. I131 uptake is increased or normal, but the uptake is not inhibited by administration of T3. Moreover, administration of TRH does not lead to elevation of TSH.
Laboratory investigations: BMR, serum, PBI, I131 uptake by the thyroid gland, levels of T4 and T3, FTI and T3RU are all increased. TSH is low and there is no increase in TSH levels when TSH is administered. Other suggestive cholesterol and raised serum creatinine.
Goiter
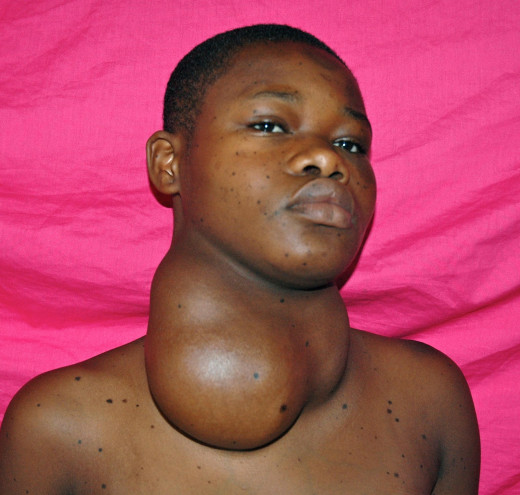
Treatment
Thyrotoxicosis may be treated with antithyroid drugs, surgery or irradiation by radioactive iodine.
Drug therapy: Drugs form the first line of management in the ordinary case. Antithyroid drugs block the synthesis of thyroid hormones. The drugs are started in a small dose, worked up to optimum response, and maintained for a period of 18 months. With improvement in the condition, the dose can be tapered and maintained at a lower level. In 50% of cases remission is obtained during drug therapy. Many cases may relapse on withdrawal of therapy. Thiocarbamides, potassium perchlorate, and Lugol’s iodine are employed as antithyroid drugs.
Thiocarbamides: The effective does of propylthiouracil is 150 mg 6 hours orally. When the toxic symptoms are controlled, the dose is reduced.
Carbimazole is most widely used on account of its efficacy and relative safety. This drug is ten times as potent as propylthiouracil. The effective dose is 10 mg/6 hours given orally. Thiocarbamides are toxic drugs and therefore close watch should be instituted when administering them. Adverse effects include fever, lymphadenopathy, splenomegaly, jaundice, leucopenia, thrombocytopenia and agranulocytosis. Generally adverse effects manifest during the early part of treatment. Reversible enlargement of the thyroid may occur during therapy and this subsides on stopping the drug.
Potassium perchlorate: In an initial dose of 800 mg daily, the drug is very effective. As the condition improves, the dose is reduced.
Lugol’s iodine: This is an effective drug in blocking the release of T4 and T3 and also the uptake of iodide by the gland. The dose is 8mg/day. It is generally administered prior to thyroidectomy since the gland becomes less vascular and friable thereby renders surgical removal easier.
Saturated solution of potassium iodide (SSKI), 1 drop containing 50 mg; may also be given instead of Lugol’s iodine. T4 has a half-life of about 1 week in the body. Therefore the effect of antithyroid drugs is not immediately evident. There is a latent period of 7-10 days before the symptoms are controlled. In order to reduce the distressing symptoms immediately, beta-adrenergic blockers like propanolol (up to 120 mg/day) should be used. These promptly control the tachycardia, palpitation, diarrhea, tremor and exertional dyspnea. Excitement and insomnia are indications for drugs like phenothiazines or diazepam.
© 2014 Funom Theophilus Makama