How Must Public Health Change to Support the Paradigm Shift of Healthcare?
Public Health

Health Educators Must Overcome Challenges
When facing modern health problems, health educators are challenged with many barriers. Glanz, Rimer, and Viswanath (2008) mention that research findings are slow to be included in interventions for populations that need them most. The authors further reveal that health educators must examine an increasing amount of literature which also slows the incorporation of best practices. While the collection of research and literature continues to grow, the incorporation and adoption of the plethora of findings has proved challenging for those working in the health education and promotion.
Health educators working on the health problems of tobacco use, obesity, and physical inactivity are also confronted with racial and economic disparities that hinder their success. Glanz et al. (2008) states that disparities remain in health information seeking between those with high and low economic status. Glanz et al. (2008) further elaborates that clinical prevention and behavioral interventions are not universally available nor equally accessible across race and social economic status.
Technology, while improving communication in many aspects, also has disadvantages that challenge health educators. New communication products have not equally reached affluent and more disadvantaged populations (Glanz et al., 2008). Health educators must adequately account for a population’s resources when choosing new technological methods. Also with technology, the risk for inaccurate information dissemination and a weakened patient-provider relationship is present (Glanz et al., 2008). Close attention must be given to these factors when faced with addressing important health problems.
Use the Social Determinant Approach
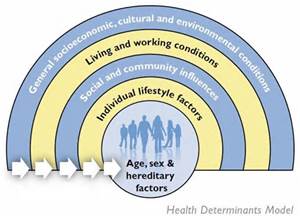
The U.S. Department of Health and Human Services (2012) mentions that the social determinant approach aims to identify methods to improve social and physical environments that promote healthy choices. Negative social factors, such as education level, are analyzed and understood as contributing factors to health. Riley (2010) states “better educated people have more opportunity to make healthier decisions” (p. 4).
Collaboration is necessary not only within the health sector when using the social determinant approach, but also with education, business, law, media, community planning and agriculture to make improvements in social environments which impact population health. Partnerships are embraced between federal, state, and local agencies to emphasize the public health initiatives (U.S. Department of Health and Human Services, 2012). Riley (2010) elaborates stating “eight times more lives can be saved with education than with medical advances” (p. 4).
Focus on the Young
Focusing on young populations to instill knowledge and further prevention efforts is an important public health concept that embraces primary prevention. Primary prevention efforts aimed at young populations are beneficial to the entire country. Cohen and Chehimi (n.d.) mention that the U.S. spends twice the amount per person on healthcare than other industrialized countries; a cost that will continue to rise unless disease and injury incidences decrease. “Health promotion and disease prevention could reduce outright the burden of illness, acute events, injury, and their sequelae” (Cohen & Chehimi, n.d.). Starting on the very young and embedding health promotion skills and education will assist in the initiative to have a healthy country.
Glanz, Rimer, and Viswanath (2008) explain that health education has become a tool for social change as public health activities are now including policy, advocacy, and organizational change. While many social change efforts aim to change health behaviors of adults, many also seek to prevent unhealthy behaviors in children, which will change the social norm. To assist with the endeavor, multiple levels of influence such as individual, interpersonal, institutional, community, and policy are all considered when developing interventions for health education programs (Glanz et al., 2008). Cohen and Chehimi (n.d.) suggest growing knowledge and skills, using word of mouth to spread information and resources, and educating providers such as public servants to assist with changing norms. The authors further explain that networking, changing organizational practices, and influencing policies will assist with transforming norms which in turn change behaviors.
Social Determinants Model
Utilize Partnerships
Utilizing community partnerships is a valuable method to increase effectiveness of health education and prevention efforts. Cohen and Chehimi (n.d.) mention that primary prevention strategies are a natural complement to medical care and treatment. Steps are being taken towards primary prevention efforts in the U.S., but efforts must focus on communities and populations instead of individuals. Quality community prevention efforts must be emphasized while targeting the environments where behaviors occur (Cohen & Chehimi., n.d.).
Glanz, Rimer, and Viswanath (2008) explain that the health education scope and teaching methods have changed to become more diversified. Partnerships between organizations such as local health departments, hospitals, senior living and activity centers, and the media play an important part in health promotion programs. These agencies work side by side to implement clinics, screenings, and community education while developing a rapport with community members. Constant collaboration between the community, health agencies, and government bodies will assist in achieving positive outcomes at the community level. Mullen and others (1995) suggest that health education settings provide channels for delivering programs, access to specific populations and gatekeepers, usually have existing methods for dispersal of programs, and facilitate organizational change to support positive health practices” (as cited in Glanz et al., 2008).
What Do You Think?
Which concept is the most effective change to public health?
Future Public Health Focus
In the next decade, the baby boomers will continue to increase the ill elderly population while the young obesity stricken population will begin to observe the negative effects of their disparity. Health education and promotion will be key to address and prevent the further decline in the nation’s health. The future focus of public health professionals should not lie with one such disparity, but instead focus on bridging the gap between health education, health promotion, and positive health behaviors. Glanz et al. (2008) suggests that health educators implement methods grounded in theory, merging theory and research to improve population health.
Health Promotion

References
Cohen, L. & Chehimi, S. (n.d.). The imperative for primary prevention. In Prevention is primary (chapter 1). Retrieved from http://media.wiley.com/product_data/excerpt/53/04705509/0470550953.pdf
Glanz, K., Rimer, B. K., & Viswanath, K. (2008). Health behavior and health education: Theory, research, and practice. San Francisco, CA: Jossey-Bass.
Riley, R. W. (2010). Health starts where we learn. Retrieved from http://www.rwjf.org/content/dam/farm/articles/articles/2010/rwjf69396
U.S. Department of Health and Human Services. (2012). Social determinants of health. Retrieved from http://www.healthypeople.gov/2020/topicsobjectives2020/overview.aspx?topicid=39