How to Become an Anesthesiologist: The Anesthesia Residency
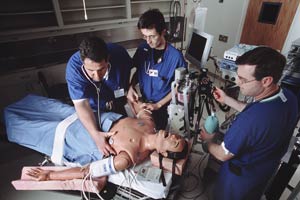
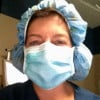
Are anesthesiologists the same as CRNAs?
No, an anesthesiologist is a medical doctor and has learned anesthesia through that pathway. They have four years of medical school (to obtain an MD degree) and four years of intensive residency training after college.
Nurse anesthetists (CRNAs) are nurses who completed nursing school, have at least one year of critical care nursing experience and then continued their education in CRNA school. This two to three year program is considered to be graduate level education in nursing, with the equivalent of a master's degree upon graduation.
Sometimes, physician anesthesiologists and nurse anesthetists work together and sometimes independently of each other, depending on the care setting and model utilized by their practices and the laws of the states in which they practice. The American Association of Nurse Anesthetists believes that CRNAs should be allowed to provide anesthesia to patients without supervision by a physician.
Are Anesthesiologists Doctors?
As an anesthesiologist, I get this question, or some variation of it, a lot.
Yes, anesthesiologists are doctors with an M.D. (or D.O. degree if they went to osteopathic medical school).
So, anesthesiologists are physicians who specialize in anesthesiology during residency. Anesthesiologists have gone through medical school and residency training, just like physicians who chose other specialites.
Medical school has the same requirements for everyone. By the end of medical school, each student has selected a specialty. He or she will have participated in the "match" to be placed in a residency spot. Before anesthesia residency, the new doctor must first complete a yearlong internship, usually in general medicine or surgery. The next three years are spent in the anesthesia residency program.
The path to board certification starts with the written board exam. Once this is passed and you have graduated from anesthesia residency, you can sit for the oral board exam. This is a face-to-face question and answer assessment of your knowledge, skills and attitude with senior anesthesiologists. When this is passed, you are considered "board-certified". You will then have yearly requirements for continuing education, practice assessments and so on. Every ten years, you will take a written exam. All of these things are required to maintain your status as "board-certified."
This article has and will address "you" as if you are considering a residency in anesthesiology. It is written, however, for anyone who is just more curious about the training of an anesthesiologist.
Miller's Anesthesiology is the comprehensive, 'gold-standard', reference text for anesthesia.
Barash's text is quite "readable" for anesthesia residents on a day-to-day basis
Anesthesia Residency Training
Anesthesia residency is structured like other post-graduate medical training programs. Residents start learning their specialty under the careful guidance of more experienced residents and attending physicians.
Each month and each year, the resident in anesthesia is given measured, and more, independence and responsibilty. These include duties in patient care, research, teaching of other residents while still under the guidance of attending physicians, themselves.
Attendance at lectures, completion of required reading, oral case presentations and self-study are expected and required during residency, as well.
Overview of Skills Learned by Anesthesiology Residents
General anesthesia
Sedation and local anesthesia
Epidurals and Spinals
Mangagment of the pregnant patient for delivery and surgeries
Anesthetic care of children
Anesthetic care of newborns (including premature babies)
Care of babies and children with congenital heart defects during surgery
Anesthetic decision making, planning and administration for patients with severe or rare diseases
Anesthesia for trauma patients
Procedures such as nerve blocks
Pain management medications and procedures
Anesthesia Residency Requirements
All anesthesia residents, before becoming eligible for board certification, are expected to demonstrate competence in basic and advanced anesthesia techniques.
Through your training as an anesthesiologist, you will become an expert in peri-operative medicine. This includes care of the patient before, during and after surgery. You will be helped by a strong background in general medicine, and many medical specialties such as cardiology, pulmonology and neurology. The basic science fields of anatomy, pharmacology and especially physiology and pathophysiology will be the foundation of your education.
In addition to learning how to provide safe and effective anesthesia, there are many other skills that you will master during your residency.
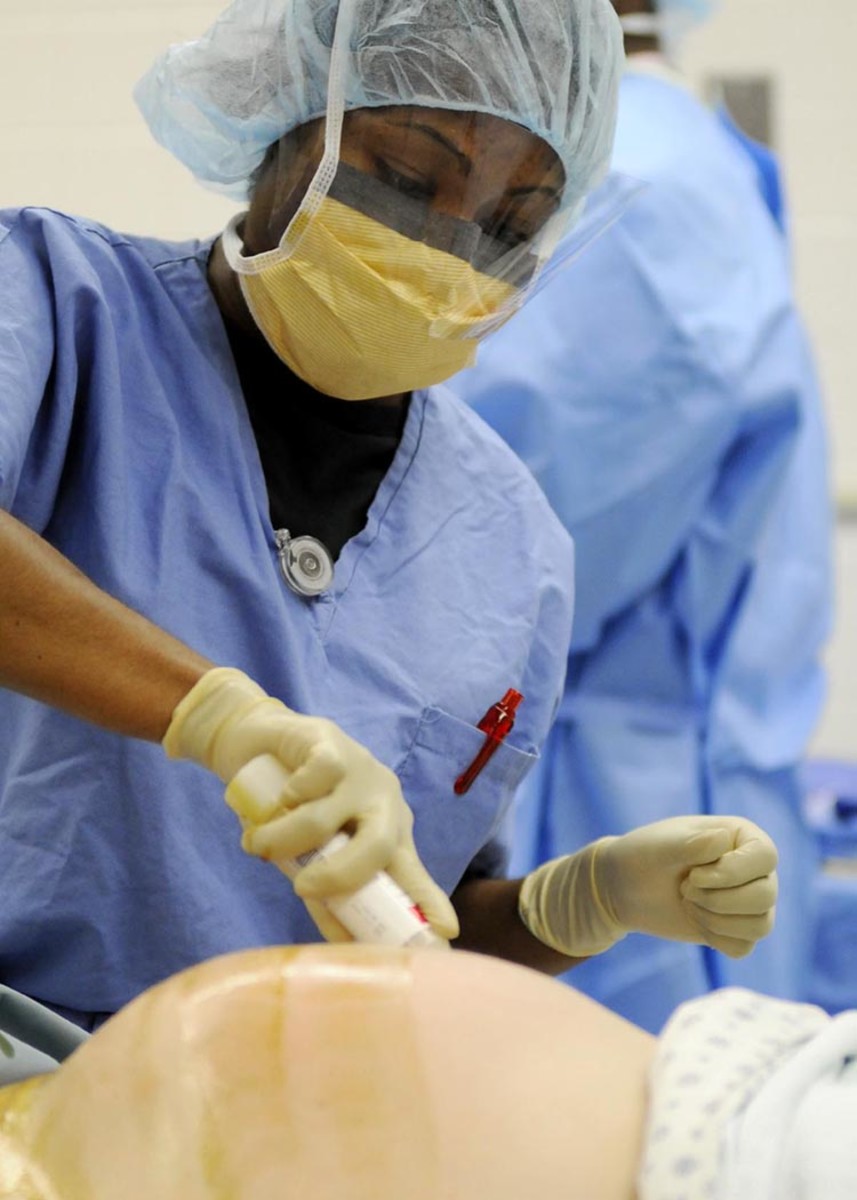
You will become an expert in airway management. In life-threatening situations, you will be responsible for accessing the airway (nose, mouth, pharynx, larynx, windpipe, lungs) to make sure oxygen is delivered to the lungs and to the body. Usually, this is done with placement of a breathing tube.
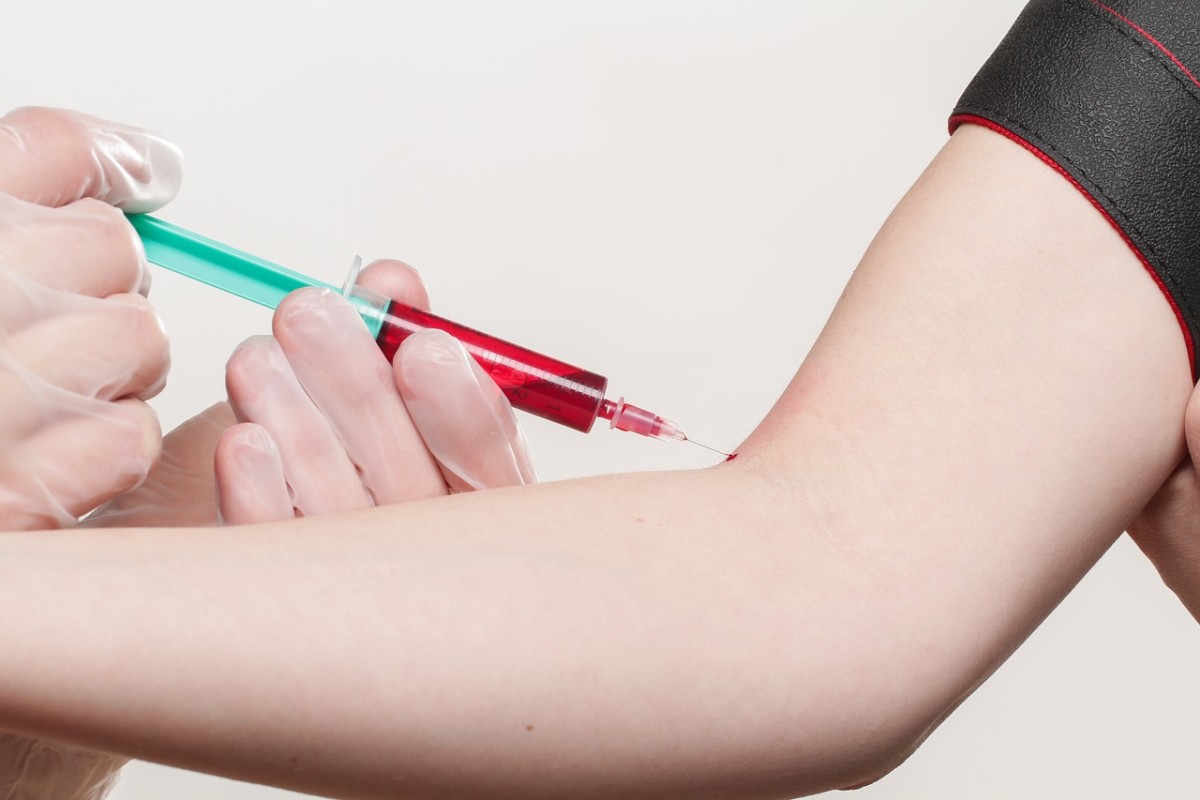
The anesthesiologist, in many hospitals, is the "go-to" person, not just for airway management throughout the hospital, but also the expert in IV placement. You are the person to be called if no one else is able to place an IV, so you will spend a lot of time learning this skill during residency.

What is Residency in Anesthesiology Really Like? A few thoughts from someone who has been there.
Like most residency training programs, anesthesiology residency is grueling and stressful. It is also very interesting and rewarding. The biggest surprise might be the amount of responsibility you have. Although you realize before going in that there is a lot more to the job than most people realize, the impact hits you hard when you really start begin responsible for patients.
EXAMPLES OF A FEW UNIQUE STRESSES FOR ANESTHESIA RESIDENTS
The medications at your disposal and in your syringes are fatal. Unlike other doctors, you do not write an order on a chart for the nurse to send to pharmacy, for the pharmacist to fill and the nurse to get back and administer. Those steps all provide opportunities for another person to check and confirm that the medication, dosage and timing of administration are safe and adequate. In anesthesia, you don't have that luxury. You decide what medicine should be given, you grab the vial, fill the syringe and inject the medicine, sometimes in life-threatening, urgent, stressful situations. There's no room for error, no time to 'think it through'. You must be decisive, careful, focused and vigilant.
You intentionally give people medicine that make them stop breathing. Then you, and you alone, are responsible for making them start again, and for getting oxygen in them until they do. You must have (correctly) assessed that you would be able to manage the airway and then you MUST do it before the oxygen level drops. This is usually routine and standard. During residency, you will encounter many times when this is difficult or nearly impossible. And, you will learn how to manage this.
You have no control over the surgeries. When the unexpected happens, you must be ready and able to adapt. You control the vital functions of the patient while they are asleep. It is a very big responsibility. You don't get to have "bad days" at work.
Residency hours are long. Sleep can be rare at times. The demands of learning the tons of information can be overwhelming. But, it is your job for the years you are there. You owe it to your patients and future patients to do what you need to do so you are competent to practice independently at the end of residency.