Intro to Endocrinology- Part Two
Ok, now that we are done blaming our hormones for everything in part one; let’s take a closer look at their structures. The chemical nature of a particular hormone can often give clues to how it is produced, how it travels in the body to get to its target, and how it carries out its function upon destination arrival. Another aspect of hormones that can be predicted based on their chemical structure is half-life (t1/2). A hormone’s half-life, known as a circulating or elimination half-life, is the time it takes the amount of hormone to fall to half of its initial value.
Part One
- Endocrinology-Just Blame It On Your Hormone
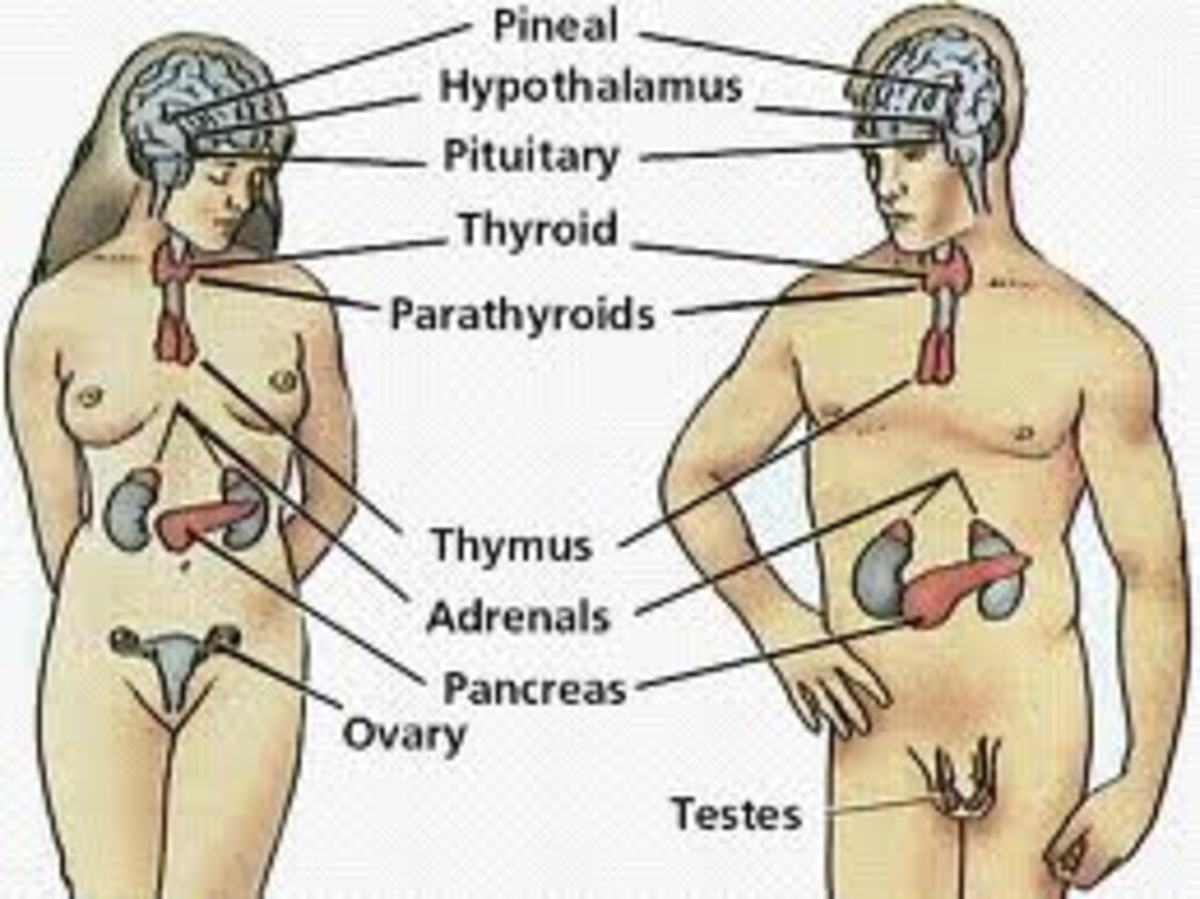
Introductory discussion of the endocrine organs and their hormones. A brief look into some of the major functions of these hormones as well.
The major biochemical categories of hormones are protein/peptides, steroids, and amines. In the case of protein/peptide hormones the difference lies in the complexity of its structure. Peptides are the building block of proteins; peptide hormones represent a simpler structure than protein hormones. A representative from the protein/peptide class is Growth Hormone (GH), produced by the anterior pituitary gland. Overall this class is relatively polar which indicates two things about the mechanism of action- 1) they can travel in the blood unbound and 2) they cannot transverse the plasma membrane of the cell. Blood is predominantly water and compatible structures such as polar protein/peptide hormones can blend in and travel freely. However when the hormone gets to its target organ, and thus target cell within the organ, it cannot make its way through the perimeter, the lipid bilayer membrane, since the membrane is mostly nonpolar. These molecules generally act by binding to a cell surface receptor. A subcategory of the protein/peptide group is glycoproteins, including LH (luteinizing), FSH (follicle-stimulating), TSH (thyroid-stimulating) and hCG-(human chorionic gonadotropin).
Chemical Nature of Hormones
Class
| Examples
|
Peptide/Protein
| Growth Hormone, Insulin
|
Steroid
| Estrogen, Cortisol
|
Amines
| Thyroxine (T4), Epinephrine
|
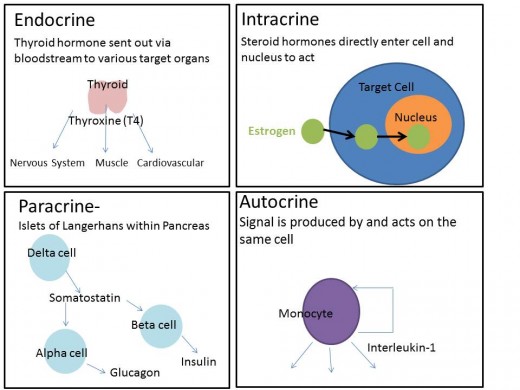
The sex hormones along with those made by the adrenal cortex are all steroids. Most steroids are non-polar so the opposite situation occurs when compared to peptide/protein class. Steroids need a carrier molecule to get them moving in the blood, but once they get to their destination they can pass through the non-polar lipid bilayer and tend to go directly through the nuclear membrane as well. Ultimately this class directly affects DNA transcription, altering production of target genes.
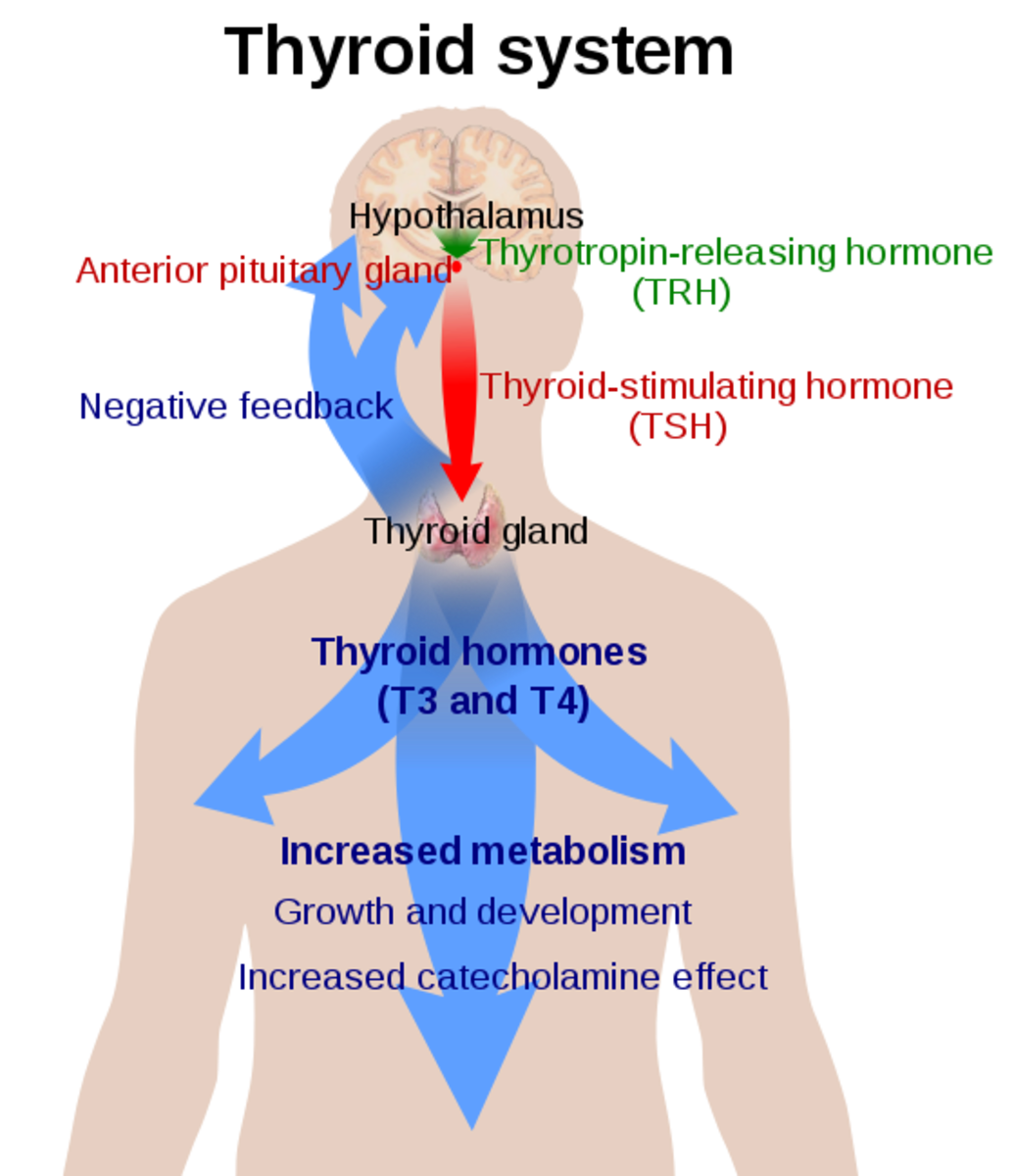
Thyroid hormones and catecholamines, as the latter’s name suggests, are both amines but their modes of action differ from each other. Thyroid hormones can cross cell membranes while catecholamines cannot. Carrier proteins are necessary for thyroid hormones’ blood travel, but not for catecholamines. Thyroid hormones, like steroids, can enter their target cells directly. While catecholamines, epinephrine and norepinephrine, have cell surface receptors similar to the peptide/protein class. Thyroid hormones have long half-lives; T4 is approximately 5 to 7 days, while T3 is 1 day, shorter than T4 but still long when compared to other hormones. Catecholamines, for example, have short half-lives. Epinephrine has a half-life of only two minutes.
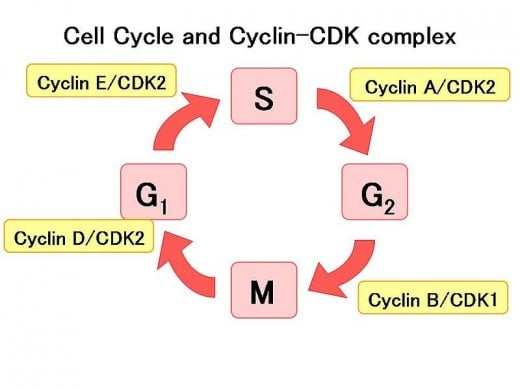
As previously mentioned hormones represent a change on the cellular level when they either bind on the cell surface or make their way into the cell. Often times these changes allow for a difference in the transcription of genes. Estrogen exerts its effect on growth and differentiation through several methods, making changes both in the nucleus on genes and through non-genetic effects. Genetic effects are mediated by the activation of transcription factors, such as AP-1 (activator protein-1) as well as non-genetic effects on Cyclin D1 and VEGF (Vascular Endothelial Growth Factor). Cyclins in general deal with mitosis; they help regulate the mitosis process along with CDK (cyclin-dependent kinase). Cyclin and CDKs represent traffic cops permitting mitosis to either go-proceed to the next stage when everything looks right, or stop- if things are not safe for the cell to proceed. VEGF signaling contributes to the production of new blood vessels, starting from scratch or made from pre-existing materials.
Several common pathways are used when hormones bind to the cell-surface receptor including the adenylyl cyclase pathway and the phosphatidylinositol pathway. Ultimately the adenylyl cyclase pathway allows for increased production of cAMP (cyclic adenosine monophosphate), a secondary messenger in many hormone cascades where the hormone represents the first messenger. In the adenylyl cyclase pathway this increase in cAMP will allow for the activation of protein kinase A, an enzyme with a role in metabolism of glycogen, sugar, and lipids. Glycoproteins mentioned above act by increasing cAMP levels. Catecholamines either increase or decrease cAMP levels depending on which receptor type they bind. Another common endocrine pathway is the phosphatidylinositol pathway. This pathway ultimately allows for calcium to be released from storage, it works as a secondary messenger allowing for a variety of effects- muscle contraction, activation of B and T cells, and neurotransmitter release. In addition calcium activates protein kinase C (PKC) which mediates a variety of functions itself including cell growth and mediation of immune response. Antidiuretic hormone (ADH) released by the posterior pituitary gland and Gonadotropin-releasing hormone (GnRH) released by the hypothalamus both utilize calcium as a secondary messenger.
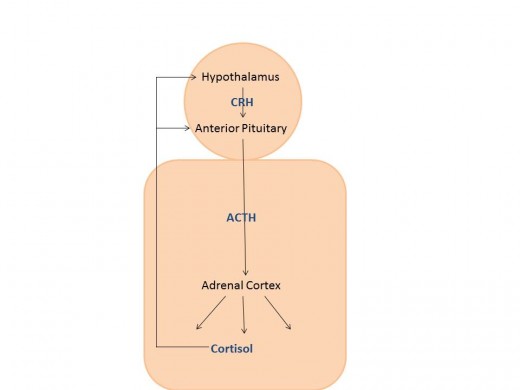
An important theme in the endocrine system is the idea of feedback. Both positive and negative feedback represent an important checks and balance system within the human body. The endocrine system has many examples of feedback but overall many systems of the body utilize feedback. Many hormones directly influence their own production through feedback mechanisms. An example of negative feedback occurs when the hormone itself causes the termination of its own production. Cortisol, a major stress-responder, is produced by the adrenal cortex and feeds back on ACTH and CRH secretion. Corticotropin-releasing hormone (CRH) production takes place in the hypothalamus; it is sent to the anterior pituitary gland in response to stress to tell the corticotropes, a fancy word for cells stimulated by CRH, to make adrenocorticotropic hormone (ACTH). ACTH will then travel through the bloodstream to the adrenal cortex, stimulating it to make all of its hormones, including cortisol. When cortisol levels reach a certain point, cortisol will attach to cell-surface receptors on both the hypothalamus and the anterior pituitary. This binding will tell them to stop making CRH and ACTH, ultimately shutting down cortisol production. Pretty cool if you ask me.
Lastly a brief note about two terms that come up in endocrinology- paracrine and autocrine, as mentioned the classic definition of a hormone is a chemical made in one part of the body and sent off to another part to function. There are, of course, always exceptions to the rule. Autocrine hormones act directly on their origin cells while paracrine hormones affect adjacent cells to their origin cells. Testosterone, in the developing male fetus, works in a paracrine fashion to allow for the development of male reproductive structures including the vas deferens and seminal vesicles. Somatostatin, a hormone not previously mentioned in this two-part introduction, functions to influence both the α and β cells which produce glucagon and insulin respectively in the Islets of Langerhans of the pancreas. Examples of autocrine action are tougher to come by when looking at strictly-defined hormones. If we look further to hormone-like substances, cytokines and eicosanoids, autocrine actions can be exemplified. Hormone-like substances function similar to the explicit hormones but vary from the traditional definition. One clear difference is where these signaling molecules are made. By definition hormones are made by endocrine organs while cytokines are made by immune organs and eicosanoids can be made in almost all cell types from precursor essential fatty acids. In a way, mentioning autocrine function in the context of endocrinology is somewhat contradictory since it precludes the traveling via the bloodstream to target organ portion of the classic hormone definition. Eicosanoids include prostaglandins, leukotrienes, and thromboxanes, among several other funny-looking named subgroups. This class of compounds can act through either cell-surface or nuclear receptors, and their major actions are through autocrine or paracrine functions. Cytokines are signaling molecules utilized by the immune system, made by a variety of cell types and act primarily through receptors. Both classes of compounds are hormone-like but not technically part of the endocrine system.