Pathogenesis, Diagnosis, Management And Principles Of Therapy Of Acute Nephritis Syndrome
Managing Acute Nephritic Syndrome
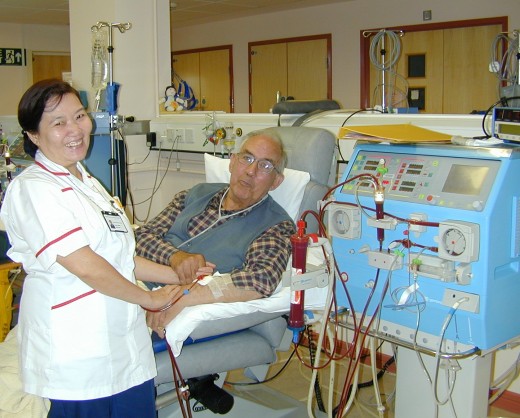
Clinical Manifestations
Acute nephritic syndrome is characterized by hematuria, red blood cell casts, proteinuria, oliguria, hypertension, fluid retention and sometimes renal failure.
Common causes
The following are the common causes of this syndrome:
- Poststreptococcal acute glomerulonephritis
- Other postinfective acute nephritic syndromes- following staphylococcal, pneumococcal and viral infections;
- Focal glomerulonephritis
- Collagen disorders-systemic lupus erythematosus and polyarteritis nodosa; and
- Miscellaneous groups- Henoch- Schonlein syndrome, infective endocarditis, hypersensitivity angitis, hemolytic uremic syndrome, and early stages of Goodpasture’s syndrome.
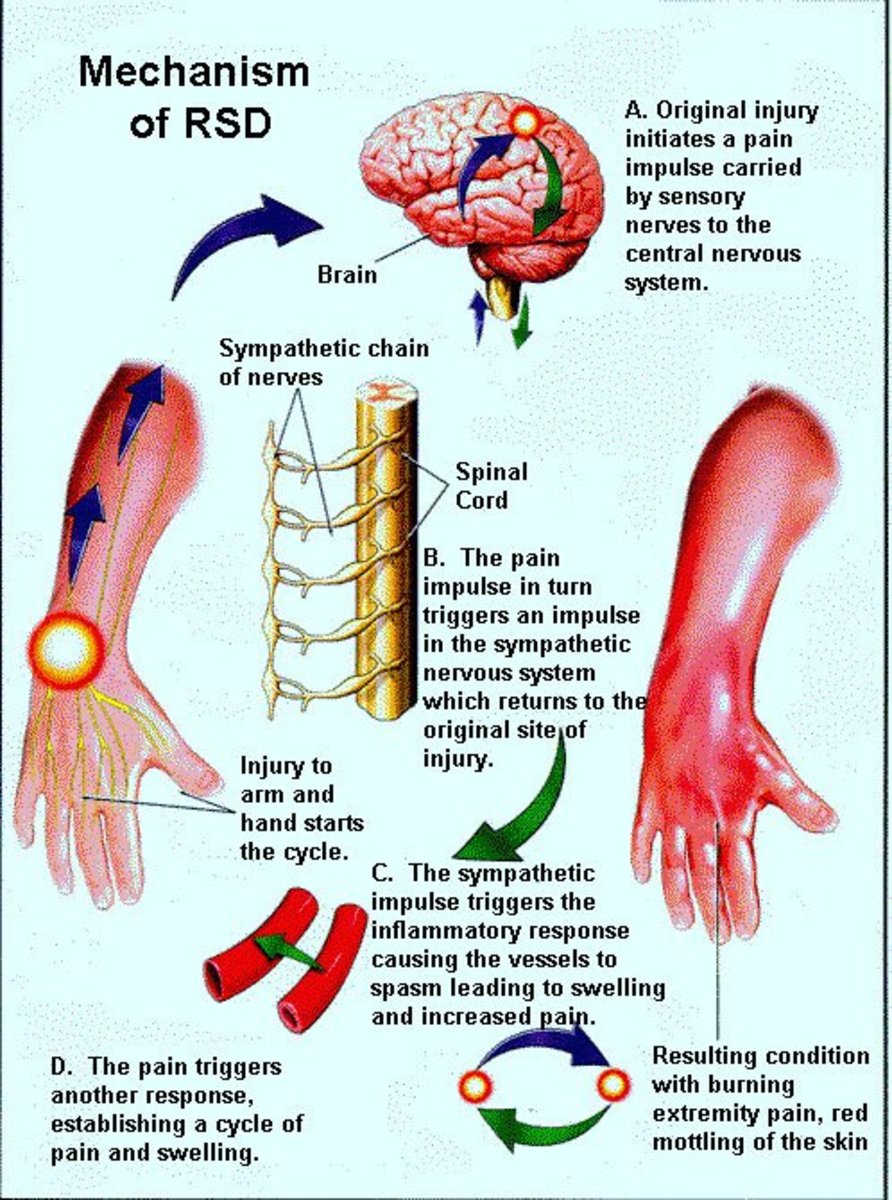
Pathogenesis and pathology
Poststreptococcal acute glomerulonephritis is the most common form. It is an example of immune-complex mediated glomerulonephritis. Following streptococcal infection, the streptococcal antigens stimulate the production of antibodies. The antigens and antibodies combine to form immune complexes. These get deposited in tissues, particularly in the kidney and initiate acute inflammatory reaction in the glomerulus. The kidneys are enlarged. The glomeruli are swollen and show proliferation of the endothelial cells. Glomerular ruft is infiltrated by polymorphonuclear cells. In addition to the proliferation, electron dense deposits are seen under electron microscopy. These are the immune complex deposits. Immunofluorescence microscopy shows a granular pattern of distribution of immune complexes in the glomeruli.
Clinical feautures
The illness starts about 2-3 weeks after streptococcal infection of the skin, throat or respiratory tract. It is more common in children but can occur at any age. Both sexes are affected. The onset is often abrupt with puffiness of the face, oliguria, reddish smoky urine, hypertension and edema. Severity of the disease is variable. Mild cases may go unnoticed (subclinical type). Severe cases present with life-threatening complications like hypertensive encephalopathy, acute left ventricular failure or uremia.
Urine examination
The urine volume is reduced, it is reddish-brown and contains protein. At this stage, the specific gravity is normal or raised. Numerous red cells are seen. The presence of red cell casts indicate active glomerulonephritis. The blood chemistry is altered depending on the severity of the disease. The antistreptolysin I (ASO) titer is significantly elevated and this suggests recent streptococcal infection. The serum complement levels are reduced during the active stage of the disease. During the oliguric phase, biochemical features of acute renal failure may be evident.
After a variable period, the activity of the disease ceases and the urine output and renal functions improve. Urinary abnormalities also clear up. Though erythrocytes and casts disappear promptly, proteinuria may persist for up to 6 months. The blood pressure promptly returns to normal in most cases with recovery.
Prognosis
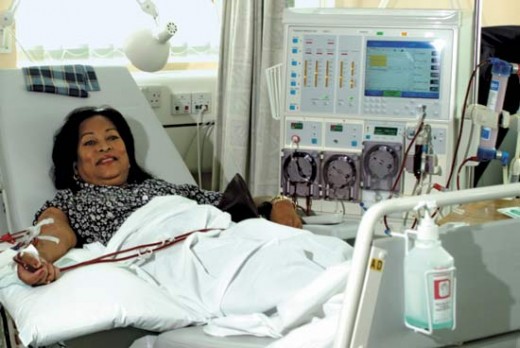
Nephrology
Diagnosis And Management
Any patient presenting with puffiness of the face, oliguria, hematuria, hypertension and edema should be investigated to exclude acute nephritic syndrome.
Differential diagnosis
Angioneurotic edema involving the face may occur in children. This may superficially resemble acute glomerulonephritis. In angioneurotic edema, puffiness is asymmetrical. Often there is pruritus and other signs of allergy. The blood pressure is not elevated and urine is normal. Nephrotic syndrome may present with edema of the face, though edema is more prominent in the dependent parts. The long duration, less dramatic onset and urinary findings should suggest the diagnosis. The blood pressure is normal in the majority of cases of nephrotic syndrome.
Diagnosis should be confirmed by urinary findings and biochemical examination of blood. Etiological diagnosis is made by estimating serum complement levels, isolation of the organisms, estimation of ASO titer and renal histology. Reduction in serum complement levels and demonstration of immune complexes in histological specimens by immunofluoresence microscopy are diagnostic of immune complex nephritis.
Renal biopsy is not routinely indicated in all cases of acute postreptococcal glomerulonephritis, especially in children. It is indicated under the following conditions:
- Failure to recover promptly;
- Presence of hypertension, azotemia and hematuria; and
- Possibility of systemic diseases like vasculitis and collagen diseases.
Course and Prognosis
In 90% of children, the recovery is uneventful and complete. The proteinuria and microscopic hematuria may persist for a few weeks or months. Some children develop nephrotic syndrome or chronic glomerulonephritis. Advanced irreversible renal failure may develop in 2-5% of cases in the acute phase. During recovery, any intercurrent infection may precipitate transient exacerbation of the clinical and urinary abnormalities. In adults, uneventful recovery occurs only in 50% of subjects. Many develop renal failure, hypertension, nephrotic syndrome or chronic glomerulonephritis slowly progressing to renal failure.
Management
Since in the vast majority of patients, acute nephritic syndrome is self limiting, only fluid restriction and close observation are required. As in the case of acute renal failure, bed rest, maintenance of fluid and electrolyte balance and adequate nutrition with carbohydrate and fat calories form the basic principles of therapy.
© 2014 Funom Theophilus Makama