Pesticide-Related Polyneuropathy: A Case Study
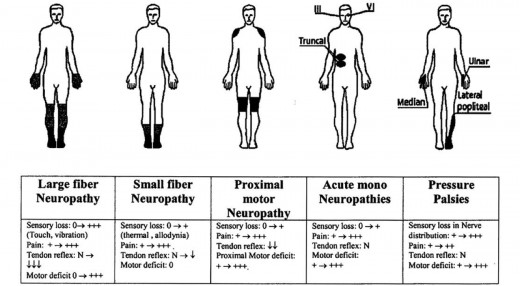
The Condition
Signals are sent through nerves in the form of current that is created by a difference in positivity and negativity on either side of the axon membrane. Myelin adds an insulating barrier between these two sides, thus creating a stronger potential in the difference of polarity across the membrane. This allows signals to reach the end of the axon. In conditions that involve demyelination, a number of axons in the nerve will not have their signals reach the synapse to either relay sensory information to the central nervous system (CNS) or relay coordinated motor signals to the muscles. This can result in numbness, tingling, or even burning sensation and difficulty with coordinated movements. This is especially true for fine motor skills such as working with one’s hands (Lundy-Ekman, 2013).
The Patient
MK is experiencing a peripheral nervous system (PNS) problem. The issue seems to be in the neurons that relay information back to the spinal cord, most likely due to absorption through the skin. If inhalation was a factor, it is likely the blood brain barrier was able to protect the CNS. Her symptoms of weakness and numbness indicate lower motor and sensory neuron damage. Any damage to the upper motor neuron tracts would result in spasticity of the muscles rather than weakness. Weakness can present with upper motor neuron damage in the first few days following the injury in a condition known as spinal shock, but since MK’s exposure happened a week ago, the hyperreflexia would have presented by now if this were the case (Aydin & Nagarsheth, 2015).
Damage to the neurons in the PNS is easier to recover from than damage to those in the CNS. PNS neurons are known to regrow and remyelinate themselves more readily and therefore are more apt to heal. Part of the reason for this is the relative lack of glial cells known as astrocytes which form scar tissue in response to injury in the CNS which blocks the growth of new neurons (Lundy-Ekman, 2013).
MK’s recovery may still be difficult depending on the extent of the damage. Her age is also a factor, as new neuron growth is declining by the late fifties. Additionally, synapses will need to be re-strengthened which will require active participation on her part. Occupational therapy is a good way to improve her coordination. As her neuronal damage does not appear to be severe and she does not have damage to muscles or ligaments, physical therapy may not be warranted. Instead, working with her on skilled tasks that may even emulate something routine for her such as gardening will help her regain the connections and myelination necessary to recover as best as is possible. The neuronal regrowth will not be exactly the same as it was before the toxicity and certain actions and sensations may not feel the same, but she should be able to return to complete functionality (Lundy-Ekman, 2013).
Treatment
Assuming MK does not further expose herself to toxins, it is likely she will be able to return to a relatively normal degree of functioning within a week to two weeks (depending on the specific severity of her case). However, it may take up to several months until she feels she is back to her normal routine and can perform all tasks without discomfort. Neurology is a very difficult area of health to predict, and thus time frames are often given in broad, cautiously optimistic ranges of time in which recovery will occur. As such, this writer feels that the timeframe of one to two weeks for self sufficient functioning and one to three months for complete routine return are accurate prognoses for the patient (Lundy-Ekman, 2013)
References
Aydin, A. & Nagarsheth, K. H. (2015). Encyclopedia of Trauma Care. New York, NY: Springer.
Lundy-Ekman, L. (2013). Neuroscience: fundamentals for rehabilitation. (4rd ed.). Philadelphia: PA: WB Saunders. ISBN: 978-1455706433.