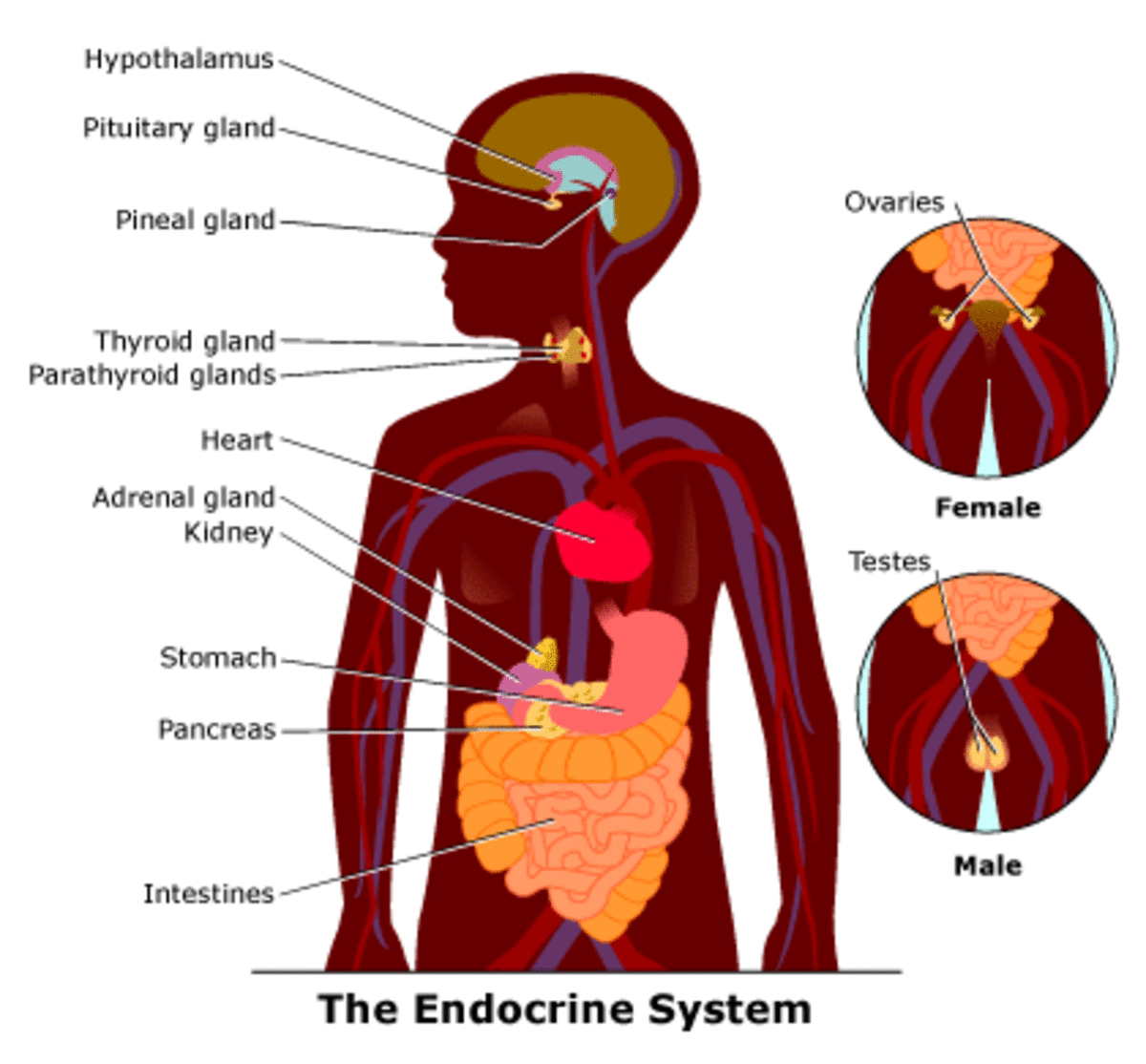
Physical And Objective Examination Of Patients With Cardiovascular Diseases:
Cardiac Lateral Auscultation
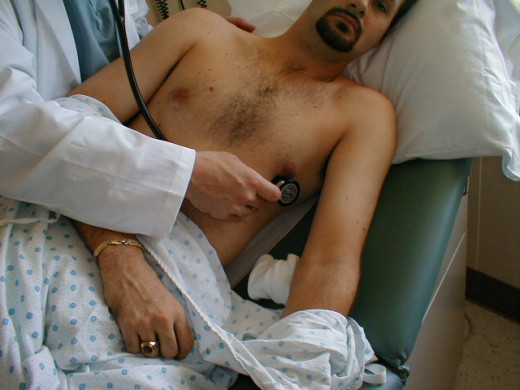
Introduction
Our previous discussion was centered on pathological symptoms of cardiology such as Precordial pain, palpitation and syncope, so we will move on to physical examination of cardiovascular cases.
Findings that may point to disease of the cardovascular system are cyanosis, digital clubbing and dependent edema. other general findings like anemia, skin rashes, pyrexia and obesity may have relevance in the final analysis.
Central Cyanosis

Cyanosis & Edema
Cyanosis
Congenital heart disease gives rise to central cyanosis due to mixing of arterial and venous blood within the heart or outside it. In central cyanosis due to cardiac cause, the extremities and tongue are all cyanosed, the periphery is warm and the cyanosis is not abolished by breathing 100% oxygen.
Low Cardiac output states may give rise to peripheral cyanosis in which there is stagnation of blood in the capillaries and over-extraction of oxygen by tissues resulting in cyanosis. The limbs are cold to feel and only the periphery is affected, the central parts like tongue are not cyanosed.
Edema: Careful search for edema and its distribution is essential in all cases.
Feeling the Limbs
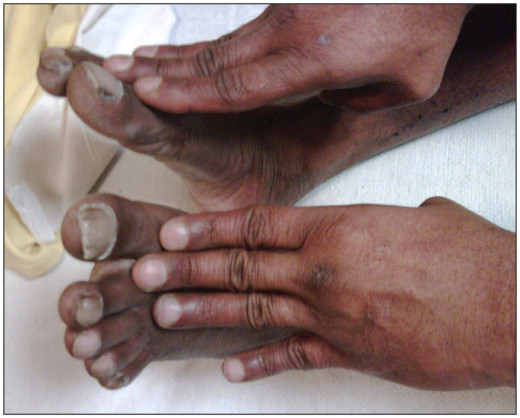
Temperature of Limbs
This depends on the state of arterial circulation. In low cardiac output states, peripheral vasoconstriction gives rise to coldness of the palms and feet. In high cardiac output states (e.g thyrotoxicosis), the limbs are warm and the arterial pulsations may become prominent.
Pulse Evaluation
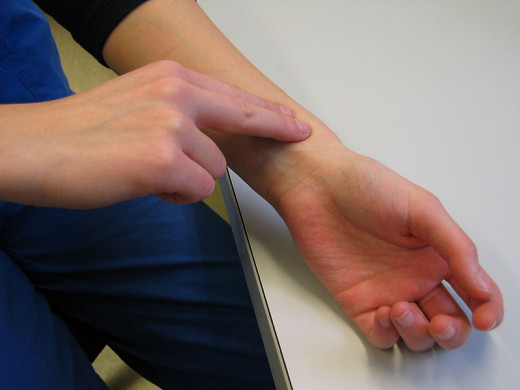
Arterial Pulse
The radial artery is generally taken up for examining the pulse. The rate, rhythm, volume and character of the pulse and nature of the arterial wall are noted. Pulse is of large volume in high cardiac output states such as thyrotoxicosis and anemia and in conditions where the stroke volume is high as in aortic incompetence. Small volume pulse (Pulsus parvus) occurs in low cardiac output states such as mitrial stenosis. When there is anatomical obstruction to the outward flow of blood as in aortic stenosis, the pulse is small in volume and slow rising (slow rising pulse or pulsus parvuset tardus).
The pulse is jerky in hypertrophic subaortic stenosis. When the stroke volume is large and there is vasodilatation, the pulse is of high volume and low tension, such a pulse is called "collapsing pulse" or "corrigan's pulse". This occurs classically in aortic incompetence and some cases of patent ductus arteriosus. The term "bisferiens pulse" is used, when the pulse wave shows two upstrokes. This is seen when there is a combination of aortic stenosis and incompetence or sometimes even in pure aortic incompentence. Pulsus bisferiens may be more clearly identified over the carotid artery. In normal subjects, during inspiration, the pulse volume falls slightly, but this is often not noticeable.
Marked fall of pulse volume and pulse pressure during inspiration is called "Pulsus paradoxus". This is seen in pericardial effusion and constrictive pericarditis. "Pulsus alternans" is the condition in which alternate beats are weak. This difference may be palpable in most cases. When in doubt, this abnormality can be brought out using the sphygmomanometer. The difference between the stronger and weaker beats may be up to 40 mmHg. Presence of pulsus alterans signifies gross impairment of left ventricular function.
Mockeberg's sclerosis in the elderly
Monckeberg's Sclerosis
Examination of the arterial wall for thicknening, nodularity and calcification reveals several abnormalities. When the medium-sized arteries like the radials are nodular and thickened, it suggests medial sclerosis (Mockeberg's sclerosis), which is generally seen with advancing age.
All major arteries should be palpated to assess whether they are patent or occluded. Generally, the carotid, axillary brachial, radial, femoral, popliteal, dorsalis pedis and posterior tibials are examined. Simultaneous palpation of the radial and ipsilateral femoral artery helps in detecting occlusion of the aorta. Normally, the femoral pulse precedes the radial pulse by 0.005s. The femoral pulse is delayed in coarctation of the aorta and aortoarteritis. Ausculatation over the arteries may reveal bruit. Bruit may be the result of narrowing of the lumen (e.g carotid stenosis and renal artery stenosis) or may arise from increased blood flow through the artery (e.g carotid artery opposite to the side of carotid occlusion, thyroid arteries in Grave's disease).
Clinical skills: Examination
© 2013 Funom Theophilus Makama