Risks and Dangers of Blood Transfusions



How Safe?
Many believe blood transfusions are safe. Whether they are or not is debatable. In any case, studies show, there are risks. Blood-borne diseases worry physicians and patients. Which diseases? Honestly, you cannot limit it just to one… there are many.
Danish scientist Niels Jerne, who shared the 1984 Nobel Prize for Medicine had this to say when asked why he refused a blood transfusion. "A person's blood is like his fingerprints. There are no two types of blood that are exactly alike."
When the AIDS (acquired immunodeficiency syndrome) came along in 1981 it awakened people to the danger of contracting infectious diseases from blood. Millions became infected…with a death rate of virtually 100 percent.
Admittedly, the blood industry was slow to respond, even after tests were available. Testing of donor blood finally began in 1985, but even then it was not applied to blood products already on the shelf.
Since 1977, men who have tried to donate blood have been asked if they ever had sex with another male, even if only once. Those answering in the affirmative were banned from giving blood. The reason given was these men potentially had a higher chance of transmitting the HIV virus.

Detectable Antibodies
And it was later revealed, after a person is infected, it could be months before detectable antibodies could be produced. Being unaware, someone might donate blood testing negative. People have developed AIDS after being transfused with such blood!
The Red Cross, the International Blood Association, and the America's Blood Centers suggested replacing this ban to only a year. An HIV infection can usually be detected 10 to 21 days after a person has been infected, so some feel a lifetime ban is not necessary.
HIV tests now available are very good at detecting the virus, not 100% accurate, but almost. The chance of contracting HIV from receiving blood is now said to be about 1 in 2 million.

Millions of Deaths
However, blood transfusions are given for many reasons other than AIDS. Jon Barron, a board member of the Health Sciences Institute writes "…blood cell transfusions in patients having cardiac surgery is strongly associated with both infection and ischemic postoperative morbidity, hospital stay, increased early and late mortality, and hospital costs. And significantly, the majority of those transfusions may in fact have been responsible for many millions of patient deaths over the last hundred years.”
Researchers from the University of Michigan Health System and the University of Rochester Medical Center pooled resources on this research and detailed their findings. There statistics showed women received more blood transfusions than men undergoing similar surgeries. So basically, the more blood transfusions done, the greater the risk for complications.

Safe as Scientifically Possible
Blood transfusions have been made as safe as scientifically possible. Nevertheless, receiving someone else's blood always carries some risks. When a blood transfusion is determined necessary, researchers recommend patients use blood having had the white cells removed (leukoreduction.) It is believed this process lowers the chance of developing an infection.
"For 100 years we've assumed blood transfusions are good for people, but most of these clinical practices grew before we had the research to support it," said Neil Blumberg, M.D., professor of Pathology and Laboratory Medicine and director of Transfusion Medicine at the University of Rochester Medical Center.
And The Boston Globe Magazine reports blood specialist Dr. Charles Huggins believes blood “…must be considered unavoidably non-safe.” He describes blood as “the most dangerous substance we use in medicine.”
This is backed up by a New South Wales press release, in which the statement was made "There is now increasing evidence for immunomodulatory effects following transfusion. We can no longer ignore the facts about blood and blood transfusion". (Blood Myths,Clinical Excellence Commission NSW 23/01/2008.)
There are many myths and misconceptions floating around about blood transfusions. such as blood is now safer than ever. Bacterial contamination, incompatibility reaction and transfusion related acute lung injury (TRALI,) are still common, dangerous complications.
Some believe blood transfusions will shorten a hospital stay. There is new evidence indicating transfused patients have longer hospital stays and more infections following their release.
Another myth is blood transfusions improve a patients healing process. Emerging evidence reveals patients who receive blood transfusions are at greater risk for infection, kidney failure or even death.
There are those who ask, since blood has been donated freely, why are people charged for it? The exact cost of blood transfusion is yet to be determined but it is at least $200 per unit to process.
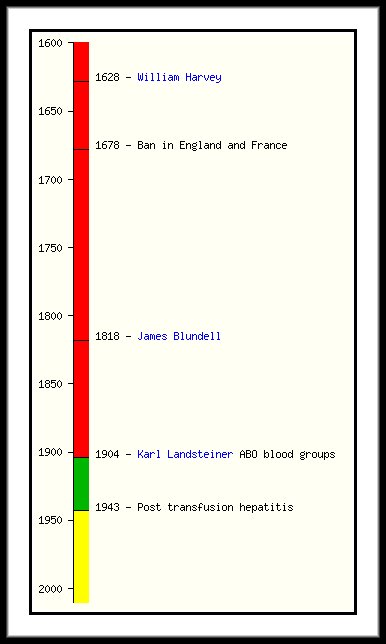
It was in 1628 William Harvey postulated the concept of blood circulation. From that point, it was just a matter of time before someone would conceive the concept of transfusing blood. They did…but in addition to human blood, several other substances were administered, including animal blood. However, at that time physicians had no concept of blood groups and cross matching processes. Therefore, an estimated 1 out of 3 human transfusions would have resulted in incompatibility.
By 1678 the practice was prohibited in France and England for well over a century until London obstetrician James Blundell announced only human blood should be used. Blundell conducted several transfusion experiments, but without the yet to be discovered knowledge of blood groups there were bound to be fatalities. The discovery of ABO blood groups and use of saline didn’t occur until the early 1900’s.
This practice continued along with some even more hazardous practices. In its’ infancy, animal to human transfusions were done with dire consequences. This still continued, but in addition there were also attempts to transfuse animal milk and even human milk. It was thought at the time fat particles in milk could be converted into blood cells.
Even after the discovery of blood grouping, improvements in blood transfusion techniques took many years to become established. There were problems with clotting and collection methods. Anti-coagulation procedures came of age in World War I, but it was during World War II blood banks were formed. Further developments, especially the use of plastics were a great boon.
As early as 1943, it was observed some patients developed hepatitis following a transfusion. Although not much was known about causative agents then, blood from paid donors was soon linked to the situation. This was not surprising, as many paid donors included high risk groups such as intravenous drug users. Therefore, blood transfusion was made purely voluntary in most parts of the world.
Unfortunately the identification of hepatitis viruses in the 1970’s and 80’s came too late to prevent many patients from becoming infected with blood borne contaminated pathogens.
It has been seen throughout the history of blood transfusions, every time its’ been thought safe, another discovery comes along to prove otherwise. Only time will tell what dangers are actually lurking in our blood supplies.The unknown may be more cause for concern than the known.