Serpent Worm
Rod of Asclepius
Dracunculus medinensis
Introduction
Dracunculus medinensis is classified as belonging to the class Secernetea, subclass Spiruria, order Spirurida, superfamily Dracuncluoidea, family Dracunculidae, and genus and species Drancunculus medinensis. It is commonly called Guinea worm, Medina worm, and serpent worm. It is distributed throughout Asia, Africa, Indonesia, Fiji, and Brazil though there has been a spontaneous eradication of the parasite in Brazil.
Historical
There is evidence that D. medinensis had been identified as early as 1530 BCE. It is also believed to be referenced in the Bible in Numbers as the fiery serpents set upon the Isrealites
“And they journeyed from mount Hor by the way of the Red sea, to compass the land of Edom: and the soul of the people was much discouraged because of the way. And the people spake against God, and against Moses, Wherefore have ye brought us up out of Egypt to die in the wilderness? for there is no bread, neither is there any water; and our soul loatheth this light bread. And the LORD sent fiery serpents among the people, and they bit the people; and much people of Israel died. Therefore the people came to Moses, and said, We have sinned, for we have spoken against the LORD, and against thee; pray unto the LORD, that he take away the serpents from us. And Moses prayed for the people. And the LORD said unto Moses, Make thee a fiery serpent, and set it upon a pole: and it shall come to pass, that every one that is bitten, when he looketh upon it, shall live. And Moses made a serpent of brass, and put it upon a pole, and it came to pass, that if a serpent had bitten any man, when he beheld the serpent of brass, he lived”. - Numbers 21:4-9
According to this passage, however, the fiery serpents kill many of the Isrealites and so do not seem to be the same as D. medinensis which have a low mortality rate.
It is also speculated to be a potential origin of the Staff of Life, also called the Rod of Asclepius, which is represented as a serpent wrapped around a staff. Because of the treatment for Guinea Worm Disease involves wrapping the parasite around a stick, it is thought to be related to this common medical image. Additionally it has been thought the image may be reference to pole described in the same passage in Exodus that the fiery serpents appear in.
Overview
Lifecycle
The lifecycle of D. medinensis involves an intermediate host, a copepod usually of the genus Cyclops, and the definitive host, humans. Larvae in water are digested by the copepods, called water fleas, where they develop into the infective stage after 10-14 days. Water infected with water fleas are drank by humans. Once ingested, stomach acid disintegrates the water flea, exposing the larvae. The larvae will then travel through the small intestine to the body cavity. The large female and the small male will mate in a 10-14 month time period. After mating the male, who has reached approximately 1.2-2.9 cm, dies and is absorbed by the female which, afterward, reaches 60-100cm. Now the female contains within her thousands to millions of larvae. She will migrate through the body, usually to a lower extremity, reach the surface and die. She will begin to expel from the body. When the exposed parasite comes into contact with water, larvae detach and infect the water. Perhaps because of the parasites migration from the intestinal tract to body tissue, it is thought to be an ancestral link between parasites of the digestive tract and filarial parasites of the tissue.
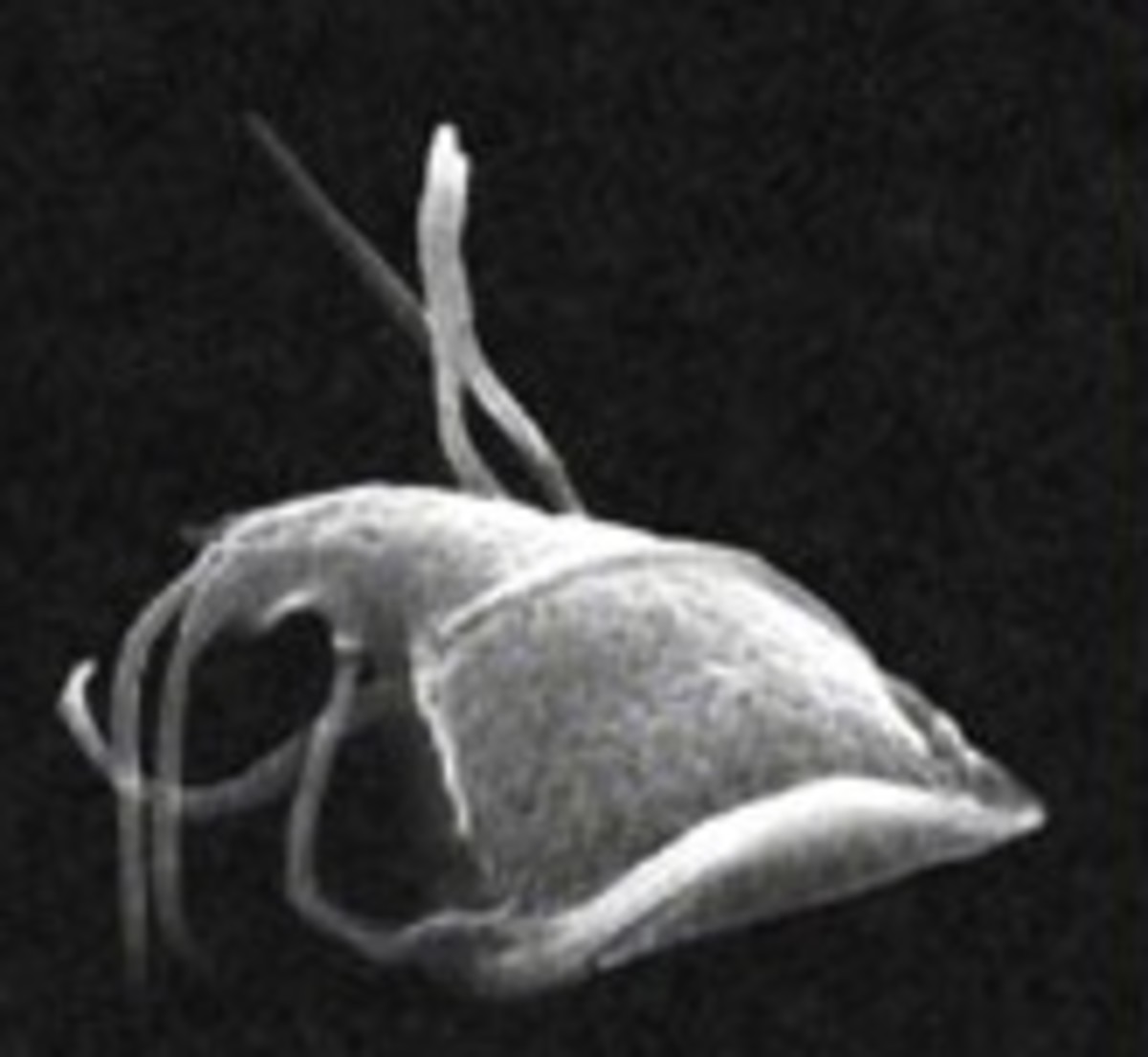
Morphology
Females range from 60-100cm long and is considered one of the larges nematodes. It is usually 1-2 mm in width. She contains a vulva in the center of her body. Unlike similar filarial parasites, a plug closes the opening and prevents larvae from exiting the body. The body cavity fully contains the uterus which extends to the posterior and may contain up to 3 million first stage larvae. The gut is nonfunctional. Males, much smaller are measured in millimeters from 12-40 mm and 0.4 mm wide.
Pathology
During most of the infection time, Guinea Worm Disease (GWD) is asymptomatic. The effects present when the parasite dies and begins to expel itself from the body approximately one year after infection. At this time, a painful blister will appear at the site. Within 24-72 hours the blister will burst and the end of the parasite will emerge. Occasionally chills and fever will coincide with the blister. Nausea, dizziness, diarrhea, and vomiting may also occur as the blister develops and breaks. If the parasite infects joints, pain may occur before the expulsion of the female. It may also cause retroplacental bleeding in pregnant patients. Some permanent injury and mild disability may happen.
“The impact of guinea worm disease does not end when the worm is out and the sufferer returns to work. A study in Ghana (88) found that, between 12 and 18 months after emergence of a worm, 34% of patients still had some difficulty performing everyday activities, usually due to pain attributable by its location and the date of onset to the episode of dracunculiasis. While this disability is not necessarily permanent, it extends beyond the incapacity occurring during worm emergence.”--Cairncross
Treatment
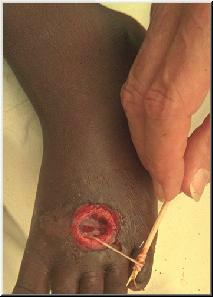
The most common treatment of GWD is to wind the parasite around a stick a few centimeters at a time. This treatment may be the origin of the Staff of Life. It will take several days to several weeks due to the long length and slow expulsion of the parasite. If the end of the parasite is broken off secondary infections are likely to result and surgical removal is immediately necessary. For some patients surgical removal occurs initially. Some antihelminthic drugs may be used, but have occasionally been found to cause the parasite to migrate to areas of the body that are more difficult to treat.
The best means of treatment is prevention and eradication. Many eradication efforts are being utilized internationally, with programs beginning in 1982, and all affected countries having eradication programs by 1995.
“At the beginning of the 20th century, guinea-worm disease, was widespread in many countries in Africa and Asia. It is estimated that there were about 50 million cases in the 1950s. Due to concentrated efforts by the international community and the endemic countries, the number of cases of guinea-worm disease was reduced to about 96 000 by 1999. Guinea-worm disease is prevalent in only 13 countries in Africa including Sudan, Nigeria, Ghana, Burkina Faso, Niger, Togo and Côte d'Ivoire. A small number of cases have also been reported in Uganda, Benin, Mali, Mauritania, Ethiopia and Chad.”—WHO
D. medinensis is considered to be an ideal parasite for eradication because of the immobility of the vector Cyclops which has highly predictable and stationary habitats, the limited carrier durations which are affected by seasonality and specificity. Decline in prevalence of D. medinensis has been very successful in most countries, with less success in the Sudan due to civil war and public unrest. For individual prevention the easiest and most effective means has been to distribute filtered drinking straws which prevent the ingestion of the water flea and to prevent contamination of water sources by infected individuals.
Current Research
Current Research for D. medinensis has been focused on reviewing eradication efforts and analyzing effective methods. It has been determined that the use of filter straws, while a very simple means, has been hugely effective in preventing ingestion of the vector. Public education efforts have been largely successful at encouraging infected people not to re-contaminate water by soaking infected limbs in drinking water sources. Due to the improved habits of the succeptible populations efforts have moved toward treating the epidemic at a community level by improving water sources and water treatment and by seeking the eradication of the vector Cyclops.
Summary
The socio-economic effect of GWD has led to attempts at eradicating D. medinensis despite its very low mortality rate at less than 0.1%. Communities are affected during growing seasons in the 15-49 year old age group, greatly reducing productivity in economically struggling communities.
“The social impact of guinea worm disease is mainly attributable to the temporary disability suffered by the patient. Two longitudinal studies in Nigeria (5, 143) found that 58 to 76% of patients were unable to leave their beds for approximately a month during and after emergence of the worm. The more severe and protracted disability is associated with secondary infection of the lesion; this occurs in roughly half the cases (124, 184).
“The impact of this temporary disability is reinforced by the seasonal pattern of worm emergence, often peaking at stages of the agricultural year when labor is in maximum demand.”--Cairncross
Means of eradication are simple and hoped to be used as a demonstration of success for other eradication projects. Disease control efforts have universally moved from treating and preventing against individual infection to community protection, prevention, and eradication.

Sources
Papers
Cairncross, Sandy; Muller, Ralph; Zagaria, Nevio. “Dracunculiasis (Guinea Worm Disease) and the Eradication Initiative” Clin Microbiol Rev. 2002 April; 15(2): 223-246.
Kelly JK MBBS and Pereira G MBBS(Hons), “The problem of water contamination with Dracunculus medinensis in southern Sudan” Journal of Rural and Tropical Public Health 5: 49-58, 2006
Sources
hhttp://www.jcu.edu.au/jrtph/vol/v05kelly.pdf
ttp://maven.smith.edu/~sawlab/fgn/pnb/dracmed.html
http://ucdnema.ucdavis.edu/imagemap/nemmap/Ent156html/nemas/dracunculusmedinensis
http://www.who.int/water_sanitation_health/diseases/guinea/en/
http://en.wikipedia.org/wiki/Dracunculiasis