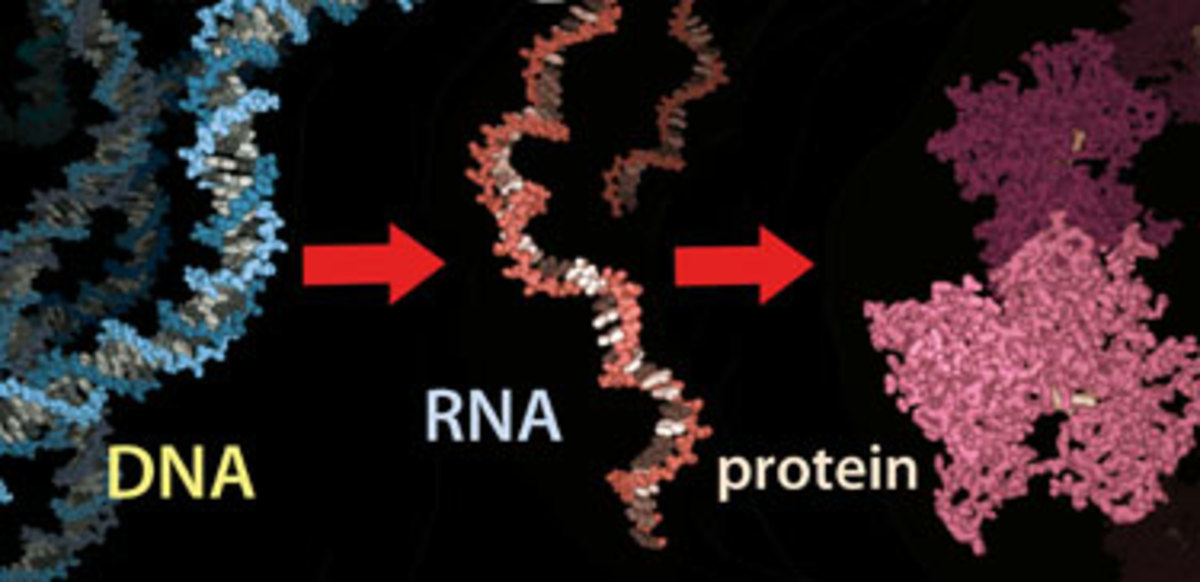
What Are Stem Cells?
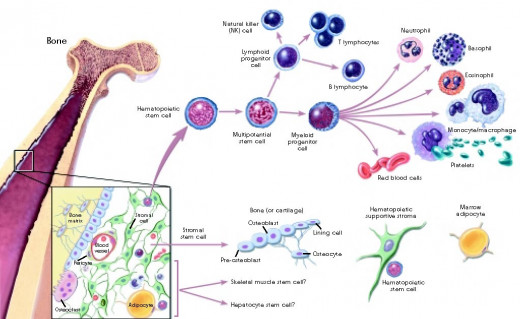
Stem Cell Differentiation
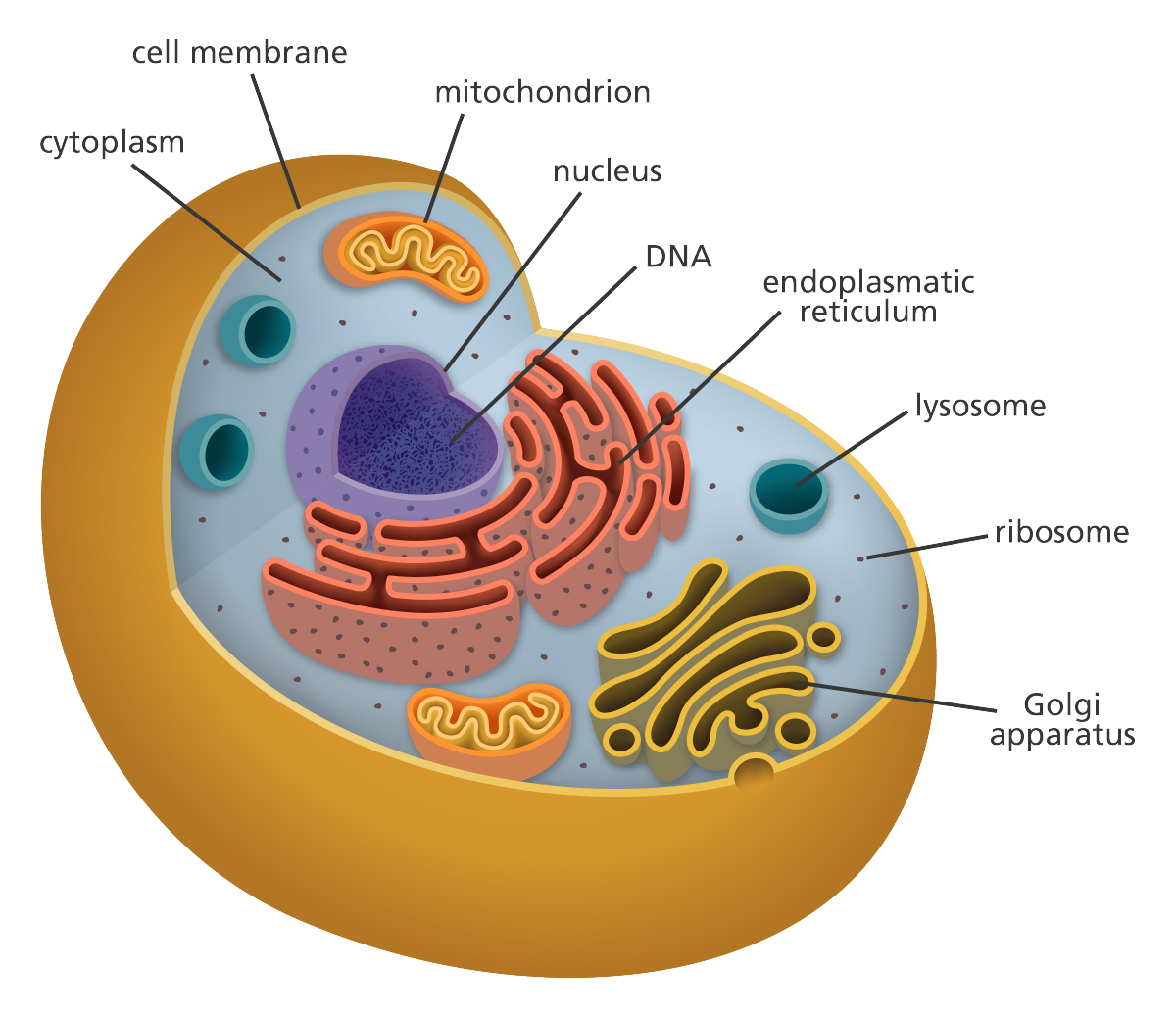
Types of Cells
The human body (and every other multi-cellular organism) has millions of cells, which perform different functions within the body. The cells in the liver are different from the cells in the brain, and both of these cell types are different from the cells that form bone. These cells are differentiated, which means they are specific to the function they need to perform.
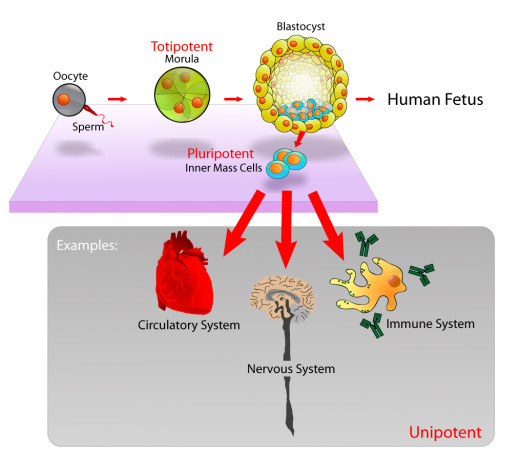
Early in development, however, cells are not differentiated: the cells in a very early embryo (called a blastocyst) can become any cell type. These cells are pluripotent, with the potential to become a bone cell, cardiac cell, or any other cell within the body. Stem cells are pluripotent cells, and occur in embryos and in some adult tissues (namely, skin and blood).
Embryonic Stem Cells
Where Are Stem Cells Found?
Embryonic Stem Cells are found in early embryos, before cellular differentiation has begun. Early embryos are usually obtained from in-vitro fertilization, with the donor’s consent. The cells are grown in a nutrient rich broth called a culture medium. Cells that grow successfully and do not have any genetic defects, mutations, or signs of differentiation become an embryonic stem cell line.
Cord Blood Stem Cells are stem cells circulating through a baby’s blood system at the time of birth. Blood is taken from the infant’s umbilical cord to harvest these cells. While not as pluripotent as embryonic stem cells, the cells found in an umbilical cord are more flexible than adult stem cells. These “cord blood derived embryonic-like stem cells” (CBEs) can be induced to form many different tissue types, and are easier to grow than adult stem cells.
Adult Stem Cells are found in many different tissues. Stem cells have been found in skin, bone marrow, muscle, the intestinal tract, and in many other organs. These stem cells reside in what is called a stem cell niche, and are very difficult to grow outside the human body. Once identified, the cells are grown in cell culture media, and scientists try to induce them to differentiate into the tissue they were derived from. If successful, these induced stem cells can be used to treat diseases like Type I Diabetes (pancreatic cells) or injuries. For example, burns may be treated with the use of skin stem cells, which grow new skin over the patient’s wounds.
Some scientists are working on inducing adult stem cells to turn into a tissue that differs from the “parent” tissue – this is called transdifferentiation. Genetic modification is used to program these cells to differentiate into a new tissue type – in this case, a neural stem cell might be induced to become a hematopoietic stem cell. Another method for transdifferentiation is programming the adult stem cells to return to an embryonic stem cell state – a process known as Induced Pluripotent Stem Cells (iPSCs).
Types of Adult Stem Cells
Cell Type
| Gives Rise to These Tissues
| Potential Therapies
|
|---|---|---|
Hematopoietic
| red blood cells, macrophages, lymphocytes, eosinophils, basophils, monocytes
| Transplants for leukemia and multiple myeloma
|
Mesenchymal
| fat cells, bone cells, cartilage cells
| Reconstruction of damaged bone and vascular tissue
|
Neural
| astrocytes, oligodendrocytes, and neurons
| Treatment of ALS, strokes, and spinal cord injuries
|
Epithelial
| cells lining the intestinal tract: goblet cells, absorptive cells, endocrine cells, and paneth cells
| Treatment of ectodermal dysplasias, burn wounds, and ulcers
|
Skin
| hair and skin
| Wound treatment from burns, baldness
|
Stem Cell Controversy
There is little controversy over the use of cord blood stem cells or adult stem cells, but the use of embryonic stem cells has generated a significant ethical debate. The acquisition of embryonic stem cells from donated embryos requires the destruction of that embryo. For some, this is the same situation as infanticide. For others, the early stage embryos have no moral status at all. The basic beliefs about the use of embryonic cells are:
No Moral Status
There are those who believe the embryonic cells have absolutely no moral status, as they have no thoughts, expectations, or beliefs.
Full Moral Status at Fertilization
For some, the early embryos are viewed as "persons," with the same rights and protections as any other member of society. Since the development from zygote (fertilized egg) to infant is a continuous process, a single point of time for becoming a "person" cannot be established. The embryo will become a person and should be protected as such from the moment of conception.
Moral Status at 14 Days
Prior to 14 days post-fertilization, an embryo may still split into twins (or more), has no central nervous system, and cells are undifferentiated. Some believe this is the cut-off point for the use of embryonic stem cells: once the primitive streak appears to form the central nervous system, full moral status should be granted to the embryo.
Embryonic Stem Cell Poll
When should an embryo be considered a person?
Gradual Onset of Moral Status
As a developing embryo goes through many "milestones" of development, there are a number of stages where increasing moral status could be granted. Some milestones include:
- Six days after fertilization, the embryo implants into the uterine wall. This is approximately the timea pregnancy test would turn positive.
- 14 days after fertilization, the embryo develops the beginning stages of the central nervous system.
- Four weeks after fertilization, when the embryo develops a heart beat.
- 8 weeks after fertilization, when the fetus has detectable brain waves.
- 21-22 weeks after fertilization, the limit of viability outside the womb (with intensive care).
- 38 weeks after fertilization, or birth.
Pluripotent Stem Cells
Induced Pluripotent Stem Cells
Due to the controversy surrounding the use of embryonic cells, there has been an emphasis on creating "embryonic-like" cells from adult stem cells. These cells are called induced pluripotent stem cells (iPSCs), and are often difficult to discern from embryonic stem cells by genetic analysis. Since the iPSCs have been reprogrammed to behave like embryonic cells, there may be sporadic "errors" in some of the clones. Careful selection and evaluation must be used when selecting cells for use in medical applications.
The very first iPSCs were created from mouse cells in 2006 - by 2007, the same feat was accomplished in human cells. Four critical genes (Oct3/4, Sox2, klf4, and c-Myc) were introduced into the adult stem cells using a retrovirus. These genes are master transcriptional regulators, and induce the cells to become pluripotent.
Adult Stem Cells to Heal Burns
Stem Cell Research and Therapies
There are many clinical trials currently underway to create treatments for genetic diseases with stem cells. Lou Gehrig's Disease, or Amyotrophic Lateral Sclerosis (ALS) is one such disease currently in the clinical trial phase. Neural stem cells are injected into different areas of the spinal cord, in the hope that they will form new, healthy nerve cells, preserving the functionality of the diaphragm (allowing the patient to keep breathing, since respiratory failure is a fatal complication of this disease).
Stem cells may also treat victims of traumatic injuries and burns. A "skin gun" was developed by Dr. Jörg Gerlach as a way to apply skin stem cells to burn victims. Skin stem cells are isolated from an area of healthy skin on the patient, grown in a bioreactor, and then sprayed on the burn area with the specialized spray gun. The skin will regrow over the burned area in a matter of days, much faster than traditional skin graft methods. In addition, since the skin comes from the patient's own skin cells, there is no chance of rejection by the immune system. The skin cells simply grow and cover the burned area, preventing infection and other complications. This treatment is not a future possibility, but a real, current treatment option at the Berlin Burn Center in Germany.