How to Prepare for Returning to Work and Pumping Breastmilk for Your Infant
Before Giving Birth
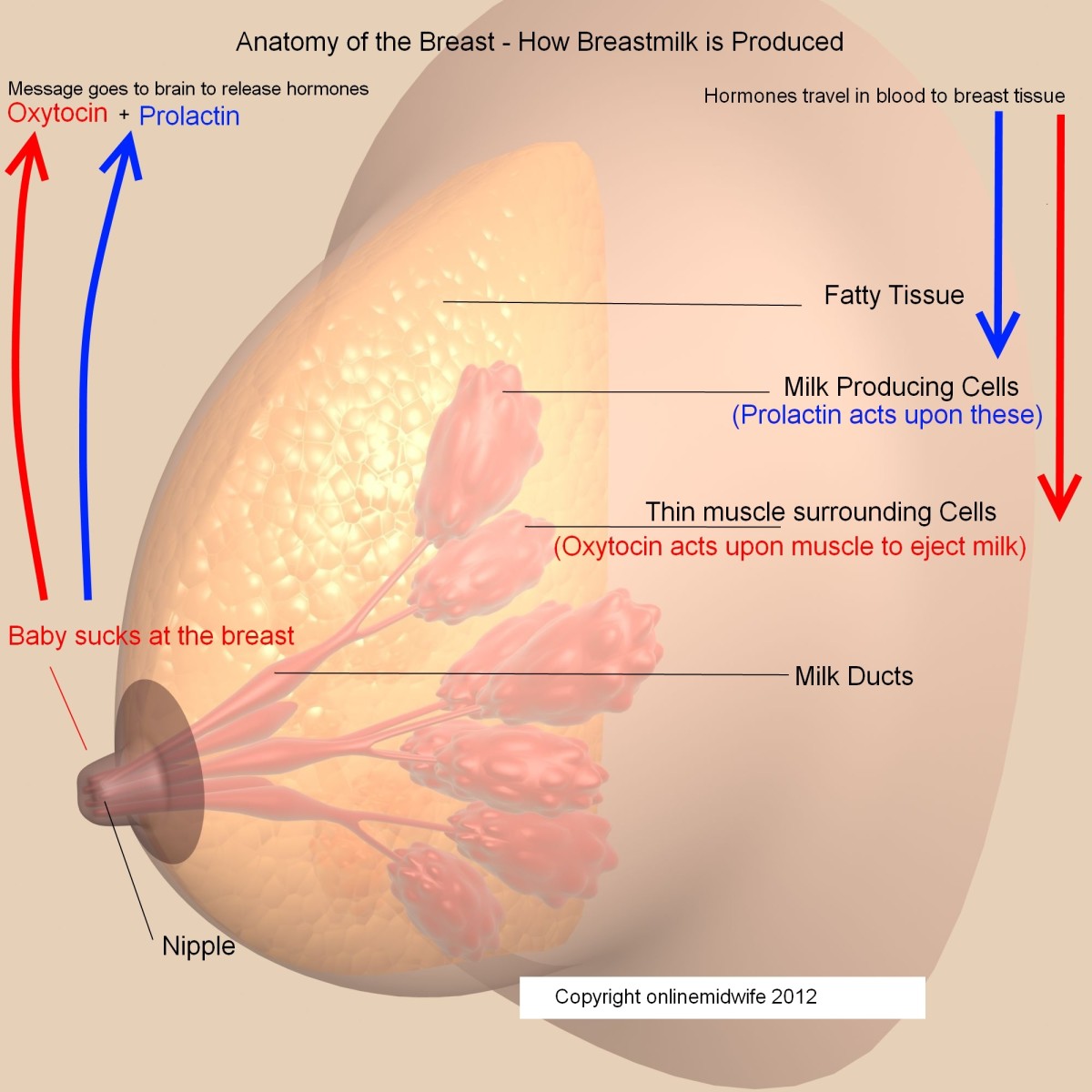
- Read up! Get familiar with nursing terminology, including detailed anatomy. Find out all the facts (including recommendations from the medical community, nutritional details of breastmilk vs. formula, etc). Read about nursing and pumping strategies.
- Mentally prepare for nursing and pumping. Like a lot of aspects of early motherhood, the most important thing to realize is that nothing can truly prepare you. There will be moments when you will feel overwhelmed. It is okay! You are not alone. Many other mothers have been there. Keeping that perspective can help you rebound more quickly after you have a meltdown.
- Get your nursing equipment (see below for recommendations). Consider including your pump in your hospital packing bag (although it is not 100% necessary). Get familiar with your equipment. Read all instruction manuals and sterilize parts according to manufacturer recommendations.
- Ignore everything you read about nipple confusion. Assuming your end-goal is to get your child to take a bottle of breastmilk while you are at work pumping - which is more important, that your child learns to nurse, or that your child learns to drink from a bottle? If you must go back to work, your baby will not have a choice - they will need to drink from something other than you. On the other hand, while you are still at home with your child, you can always pump and then feed them with a bottle. So in general, just keep in mind while reading the vast amounts of nursing guides available, most are not written with that "return to work" deadline in mind, so take all advice with a grain of salt and a dose of practicality. Most advice will err on the side of favoring nursing, whereas you need to probably do the opposite so you don't shoot yourself in the foot.
Recommended Equipment
- Breastpump
If you plan on pumping more than occasionally, these are the necessary features:
- if electric, it should be a double. If manual, purchase two. Otherwise you may find yourself pumping for for over an hour at a time due to switching to hit both sides.
- adjustable suction power is absolutely necessary. Otherwise you may end up with chafed, raw areas if the suction is too strong, and you will experience severe pain and discomfort while pumping or nursing.
- adjustable frequency in an electric pump is a nice feature, even though not absolutely necessary. It allows you to adjust how long the pump "holds" onto each pump. This can help your pump sessions become more efficient (i.e. take up less time) which becomes very important while at work!
- more about breastpumps in the next section - Storage Bottles and Vials
- early on, vials and small bottles can be extremely handy, because it's easier to measure and manage the smaller quantities of milk being expressed. Think you can save money by only purchasing 8 oz bottles? Try measuring 0.75 oz in those! Also, the smaller sizes can save in refrigerator space during the earlier months.
- do not feel like you need to use the same brand bottles and vials as your pump! Many pumps use the same size connectors - for example most Medela® bottles are compatible with Ameda® pumps and vice versa.
- conversely, ensure that your containers are compatible with your pump. For example, the Avent® pumps tend to be sized to fit their bottles, which have a wider neck. Even purchasing the same brand bottle as the pump does not guarantee compatibility.
- use the same scrutiny for any storage containers as you would for baby bottles (i.e. BPA free, etc) - Bottle to breastpump adapter (optional)
- if your bottles do not directly connect to your pump, you can sometimes find an adapter that will make them fit together properly. This can save you cleaning time and reduce the number of container transfers, which can cut down on contamination and risk of spillage.
- check to make sure the adapter fits both your pump and your bottles. For example, the BornFree® brand sells one on their website that fits "most" breastpumps and fits all BornFree® bottles. This adapter should fit at least the Ameda® and Medela® brand pumps. - pump bag
- if your pump didn't come with a bag, no worries, you just need a bag that can carry the pump, some bottles, and all the necessary accessories. Bags with antimicrobial interiors are a plus so that your parts are kept clean. - Insulated bag (optional) with ice pack
- this bag will be used to transport milk from work to home so that it is kept cool.
- if your commute is less than 15 minutes, you don't necessarily need an insulated bag, but if you plan on running occasional errands en route or picking up your little one, consider using one as an extra safeguard. - Flanges/shields
- the flanges, sometimes called shields, are the part of the pump that is directly in contact with you.
- your pump will come with a flange(s), most likely in the brand's medium size. However, not all women are the same size, so you may need to purchase separate flanges of smaller or larger sizes, and/or a reducing insert (a flange that you can insert within an existing flange to reduce the size).
- These are sized in millimeters, based on the size of your areola. Keep in mind these sizes are just guides - you may find that a larger flange works better even though your areola measures for the medium flange.
- ensure that any flanges purchased separately from the pump are compatible (most reducing inserts should be compatible across brands) - Other Pump Parts
- the exact list of parts varies according to the pump used, but typically include valves, tubes, diaphragms, tubes, etc. Your pump, if purchased new, will typically come with all necessary parts
- if your pump is second-hand or rented, replace all parts that may have had contact with milk in order to reduce risk of contamination.
- periodically replace all parts according to manufacturer's specifications or when you notice a part is failing.
- some parts are the same or similar across brands - it is recommended to bring a part into the store and compare visually for compatibility. - Breastmilk storage bags
- some mothers try to avoid purchasing these and instead use standard freezer bags. The downside to bags not made specifically for breast milk are (1) the size (2) risk of tearing, especially at the corners (3) risk of chemicals (BPA, etc) leeching into the breast milk.
- if you purchase in bulk at a good price, these will end up being less costly than standard freezer bags, anyway.
- these are useful primarily for freezer storage (using for refrigerator-only storage will prove costly and wasteful since you can just use washable storage containers)
- it's useful to keep some of these around (especially in your pump bag) just in case you end up with excess milk at some point - otherwise some breastmilk may end up down the drain due to spoilage. - Nipple cream (optional)
- nursing and/or pumping is hard on your nipples. Until your skin adjusts, keep your nipples protected with nipple cream (such as lansolin) to reduce chafing.
- most of these special creams are hypoallergenic and safe for your newborn to ingest.
More about Pumps
- Thanks to the Affordable Care Act of 2010, most insurance companies are required to pay for the cost of buying or renting a pump. Contact your insurance company directly, or use a third party such as those recommended by Babies R Us to have them coordinate with your insurance company at no additional cost to you.
- Avoid poor quality electric pumps like the plague - they can do more harm than good. A good manual pump will outperform a cheap electrical pump in speed, efficiency, and gentleness.
- Rather than purchasing a pump, consider renting a pump from the hospital. However, If you plan on pumping for more than a few months, it probably makes sense to invest in a quality pump.
- Some pumps are more appropriately designed for second-hand use than others. Any part that could be in contact with breast milk needs to be able to be sterilized and/or replaced. Take this into account when considering a second-hand pump.
- Consider purchasing an extra manual pump that can be kept with you at all times. If you ever forget part of your pump on your travels away from your baby, or if your pump breaks, you will have a back-up method. Even if you have to "pump and dump" (not save any expressed milk) you are still protecting your supply.
- Pumping should never hurt. Read the manual that came with your pump to ensure you are using it correctly.
At the Hospital
There is a lot of other stuff going on here, so you'll likely be too busy to spend time getting acquainted with your pump. However, if you're having trouble latching, or your newborn hasn't nursed for a few hours, you may want to pump (at least in order to stimulate production). If you didn't bring your pump to the hospital, the nurses will provide you with one.
Depending on the hospital staff, you may experience varying degrees of support for pumping. While most staff will be extremely supportive and knowledgeable about newborn care and breastfeeding, there are many accounts of mothers receiving mixed messages about pumping (especially early on). If you have done your research ahead of time, you can hopefully keep your head about you.
Most hospitals have lactation consultants available. Make sure to proactively ask for them if the staff does not mention it, even if you think you're doing okay with the whole breastfeeding thing. While you may not necessarily get along with them or agree with all of their opinions (some may balk at the idea of pumping at all), having hands-on (literally) guidance can be helpful. If you are having latching trouble and nobody seems to be able to help, ask for nipple shields. They are a bit of plastic/rubber (like a baby bottle) that is placed over the nipple. The shape of them can help with latching, especially for inverted, flat, or over-sized nipples.
First 1-2 Weeks at Home
By the time your new baby is 2 weeks old, he or she should be exposed to a bottle at least once most days. Most babies this young will not have a strong preference for breast vs. bottle. If they do, consider trying other bottle nipples - the shape and speed that the milk comes out, in addition to the amount of air that gets in and causes gas build-up, typically are the main factors in why a baby rejects a bottle. Introducing the bottle this early is basically to prevent a painful weaning later on. Long-term, your baby needs to be fed via bottle in order to be cared for by someone other than yourself while you are at work. Short-term, this will allow you to have someone babysit early on without too much fuss.
Within 24-48 hours after coming home, start pumping in addition to breastfeeding your baby. If you are feeding your baby exclusively breast milk, this may mean pumping the milk and then soon afterwards feeding that in a bottle to your baby. Your pumping sessions should last around 35 minutes up to 1 hour, depending on your flow and how long ago you had last nursed.
The time between let-downs (when your mammary glands release another heavy stream of milk) may be several minutes long (and even longer when you are still establishing your supply), so even if it seems like no milk is coming out, keep pumping and more milk will eventually come. You should have at least two let-downs during each pumping session; meaning, halfway through the session will probably be somewhat of an intermission in milk production. It is imperative that you pump through two full let-downs in order to stimulate proper milk production.
During this period, milk production can be pretty unpredictable. Some women will find that they produce a lot more than their baby is eating, while others will struggle to keep up. Either way, adjust habits as necessary - for those without a lot of milk, follow the section below to try to increase production; for those with what seems like too much milk to manage, read the section on milk storage (and if it seems like you have way too much milk, consider following the opposite rules for increasing supply or contacting your physician).
Tips for Increasing Supply
Take Care of Yourself
- Be patient. All methods will take some time to work for most mothers - you will feel like you are pumping just enough to keep up - but over time you will end up with excess milk.
- Make sure you are providing yourself with adequate nutrition. Pay particular attention to the amount of water ingested - don't get dehydrated! - and protein/fat intake. Consider eating more nuts, beans, oats, cheeses, etc.
- Keep tabs on your stress level. Look into relaxation techniques. Stress has a direct impact on your mammary gland's ability to produce and let-down. If you find yourself stressing about milk production, laugh at the irony and find a way to chill out - bubble bath, massage, bad television - whatever it takes.
- Related to stress levels, try to zone out while pumping. Watch a light TV show or read a book. Relaxation during pumping should yield better results.
Pumping Frequencies
- During the first month, don't go more than 6 or 7 hours overnight without emptying your breasts. During the day, don't go more than 2 hours. As your child gets older and as your milk production becomes more established, you can develop a more flexible routine that works for you and your baby while still maintaining adequate supply.
- During the period before going to work, pump one session beyond what your baby is eating. Meaning, if you produce 6 ounces of milk during each pumping and your baby ingests that much in each bottle, pump 2 times a day in addition to breastfeeding. In the case of exclusively pumping, if your baby takes in about 4 ounces of milk in each bottle and has 7 bottles a day, pump at least 4 x (7 + 1) = 32 ounces a day. Continue this even on "growth spurt" days - you may only pump 1 ounce extra or you may net a negative amount of milk on these days, but this will help increase your production during the long-term.
- Pump immediately after nursing, especially when it seems like your baby has not emptied out your breast. This should help you produce more milk during each breastfeeding or pumping session.
- Pump one breast while nursing with the other (only do this if practicing one-sided feeding). This takes a lot of juggling and practice so don't try this until you have the techniques for both activities down pat or else you will spill most of the milk.
- Find a routine for pumping. For example, pump early in the morning right after waking up and right before going to bed. This is especially useful if a loved one takes one of the nighttime feedings. Alternatively, pump when your baby takes a particularly long nap.
- Ensure you are pumping for a full session. At least two let-downs should happen - meaning the flow of milk will ebb or stop altogether for several minutes and then start up again. This will take more time earlier on (45-50 minutes or more) and then will take less time as your baby gets older (as little as 20 minutes).
Pump Hardware
- Make sure you are using your pump properly. If your nipples are chafed or tender, the pain will cause your milk production to decrease. Reduce the suction to a more comfortable level. Use nipple cream to speed up healing and reduce friction.
- Make sure your flanges are the correct size. If they are too small, your breasts and nipples will get traumatized and tender. If they are too big, your breasts will not be properly stimulated. Read the manual with your pump and flanges for more information about correct sizing.
Stimulation
- When pumping away from your baby, visual contact with your baby can help production. Look at pictures or videos of your baby. Some women even take a video of their baby nursing. If no pictures or videos are handy, just think about your baby and about nursing.
- Audio stimulation can also stimulate milk production. Record sounds of your baby nursing, or of your baby's "hungry cry" and listen to them to help get a let-down.
- Stimulate your breasts while pumping. Press and massage on parts of the breast that feel lumpy or hard (typically the lower outer edge of the breast - hook your left hand under your left breast so that the thumb is pointing up and the index finger is pointing towards the right; do the mirror image to the right breast with your right hand) - these are mammary glands that are full or possibly a little clogged. Knead these lumps towards the nipples to help push the milk forward.
Before Going Back to Work
When you first went home with your infant, you likely kept a log of how much he/she ate. If you stopped this practice, pick it up again, because you need to start figuring out how much milk to aim to pump each day and how much milk to provide your child's caregiver. When you nurse, track the start time and duration. When you bottle-feed, track the start time and ounces.
Try to simulate already going back to work by feeding your baby bottles and pumping during the day according to your future work schedule. Although this is very challenging to accomplish, because you have to pump and feed your own baby yourself (which you will not have to do once you go back to work), it will achieve several objectives:
- you can go through a trial of your schedule to see how much milk is being consumed vs. produced each day (knowing that it will fluctuate and change as your baby grows).
- you can to tweak your pumping schedule according to how it best works for your supply and work schedule, before needing to adhere to your work schedule
- you will witness how much milk is being consumed at each feeding each day so you know what to provide to your caregiver (if you nurse you do not know how many ounces your baby is taking in)
- this will help you and your baby become accustomed to your new schedule. Your baby will have to get used to exclusive bottle feeding during work hours and you will have to get used to expressing milk via pump (which does work differently, especially when pumping both sides simultaneously, so you will likely not express milk at exactly the same time as you did when nursing).
If you find that on most days your expressed milk quantities are less than the volume of consumed milk, read the section on increasing milk production. Alternatively, consider supplementing with some formula. Remember, though - a day here or there where your baby consumes extremely large quantities of milk is okay - it's just a growth spurt.
Breastmilk Storage Tips
Breastmilk can store in the freezer for up to 6 months; however it does lose some of its nutritional and immunological properties when stored in this manner (even more so than when refrigerated). Also, breastmilk's composition changes over time - it is part of evolution that our bodies produce milk with different properties that change with the needs of our babies. So, it stands to reason that milk expressed a few months ago is not as nutritionally compatible with your baby as milk expressed a few days ago. Therefore, freezer storage should mainly only be used for excess supply and refrigerator storage should be the main storage method.
Label all freezer storage clearly with an expressed date and quantity. Try to keep it in roughly chronological order so that you can more easily find the older milk more easily.
Any milk that will not be consumed in a reasonable amount of time should be frozen or otherwise donated. You can use freezer-safe reusable containers; however you will likely find it most practical to use milk storage bags that are freezer safe. If you are following the tips for increasing supply, you will have around an extra serving of milk each day (give or take). That will be the milk you freeze.
To keep your freezer supply fresh, cycle through the supply by defrosting the oldest stored milk. Defrost about one serving of milk each day to give to your baby and replace it in storage with newly expressed milk.
While Working
Block the same time(s) off of your calendar each day for pumping, clearing the break time with your manager. By U.S. federal law (the Affordable Care Act of 2010 amended the Fair Labor Standards Act, or FLSA), virtually all employers must allow unpaid breaks for purposes of expressing milk and must provide a location other than the bathroom as a place to express it, provided the employee has a child under one year of age.
Store the milk in a refrigerator before returning home, assuming one is available at your workplace. Otherwise, bring a cooler with a sufficient number of long-lasting ice packs.
In order to minimize the number of breaks needed, be sure to express milk immediately before and after work hours.
Be ready: separation from your infant goes beyond just missing someone. Your hormones and other chemical changes that have happened in your body causes a physiological connection between you and your baby. You have a biological response to being separated from them which can cause some strong emotion. It can make the first few months back to work very difficult, which are exasperated by the pumping experience.
Try to network with other mothers who are returning to work at the same time as you. They may be a coworker or another mother who uses your baby's daycare. The support and camaraderie will help.
Other References
- Breastfeeding @ womenshealth.gov
U.S. federal government-run website about women's health issues. Has breastfeeding section with some relevant information about pumping. - Breast Pumping & Bottle Feeding @ BabyCenter
BabyCenter has some generally useful information about babies and parenting and most of their content are written by actual experts. This is their section on pumping. - Medela
Although this is just a brand and contains a significant amount of product information, the Medela website also offers breastfeeding information, support and tips. - Nursing Baby: Breast Pumps @ WebMD
WebMD provides a guide to choosing an electric or manual pump, tips for getting the most out of your pump, and the basics on handling and storing pumped breast milk.