A Clinical Overview On Pneumococcal Infections With A Simple Case Study On Lobar Pneumonia
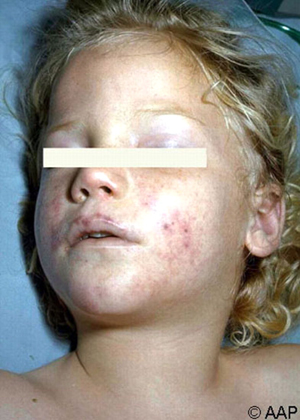
Pneumococcal Infection In A Pediatric Patient
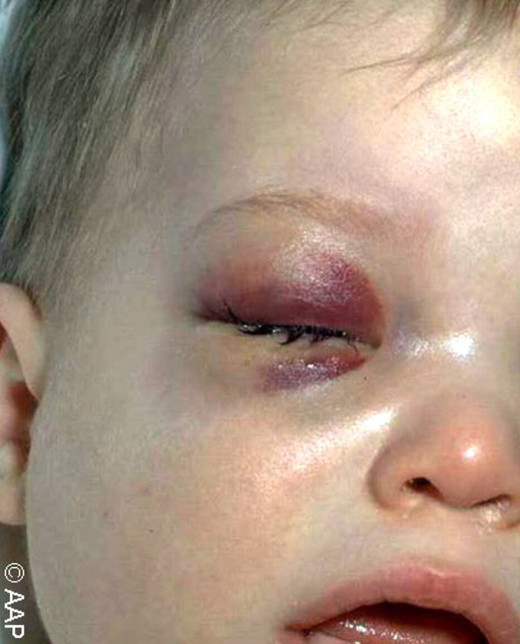
A Clinical Overview
Pneumococci are found in the upper respiratory tract. On the basis of capsular precipitation reactions using type specific antisera, about 84 serotypes have been identified. All are pathogenic to man but the most commonly encountered types are 1, 3, 4, 7, 8 and 12.
A Clinical Overview
Pneumococcal polysaccharide plays the major role in virulence and it protects the organism to some extent from phagocytosis. The polysaccharide has no toxic property. The normal respiratory tract offers adequate resistance to invasion by the penumococcus. Patients with underlying lung diseases such as bronchiectasis, carcinoma or chronic obstructive airway disease are predisposed to develop pneumonia. Aspiration of infected material, viral infections, respiratory irritants, pulmonary edema and trauma to the chest reduce the local resistance and favour the growth of pneumococci. Alcohol intoxication and anesthesia impair leucocyte migration. The mucinous secretions of the respiratory tract protect the pneumococci and these multiple and lead to further outpouring of proteinaceous fluid.
The normal defence mechanism consist of the migration of polymorphonuclear leucocytes and phagocytosis. These are enhanced by the presence of antibodies. Breakdown of these defence mechanisms result in bacteremia and the development of metastatic lesions in the meninges, joints, peritoneum or the endocardium. Recovery from infection starts with the formation of type specific antibodies in the circulation and this is clinically marked by a fall in temperature by crisis. Treatment with antimicrobials reduces the bacterial population and enhances the host defense mechanism which is still important in the elimination of bacteria. Necrosis of lung parenchyma is uncommon.
Spread of pneumococci from the nasophraynx to the adjacent structures results in the development of otitis media, mastoiditis, paranasal sinusitis or conjunctivitis.
Treating Pneumococcal Infections
Pneumococcal Pneumonia (Lobar Pneumonia)
Pneumonia is the commonst pneumococcal lesion in adults. In adults commonly the pneumonia is segmental or lobar in distribution, but in children and the aged, the lesion may be bronchopneumonic.
Pathology: Invasion of the lung by pneumococci leads to the formation of an inflammatory exudates in several alveoli and this depends upon the virulence of the organism. Segmental boundaries are not preserved and the bronchi which is relatively uninvolved, remain patent.
The inflammatory exudates contain a large number of neutrophils and red cells. In the initial stages, the alveoli are filled with red blood cells and fibrin, and the pulmonary capillaries are widely dilated (red hepatisation). In the next stage, neutrophil leucocytes predominate. They phagocytose the bacteria. The capillaries become less congested (grey hepatisation). It is uncommon for the inflammatory process to proceed to necrosis. As resolution starts, the inflammatory exudates liquefy and it is absorbed through lymphatics and removed by the alveolar macrophages. It takes considerable periods of time for complete recovery.
© 2014 Funom Theophilus Makama




