A Guide to Atrial Fibrillation
atrial fibrillation complications and overview
My husband has had two episodes of atrial fibrillation in the past year. As a result, I’ve done extensive research on the condition, as well as on the complications of atrial fibrillation, by reading everything I could get my hands on and by talking to numerous doctors, nurses, and other health care professionals. As you might imagine, I was more concerned with the possible complications of atrial fibrillation than I was with the causes.
What is atrial fibrillation?
Atrial fibrillation, also called “a-fib” or “atrial fib,” is an irregular heart rhythm. In fact, a-fib is the most common cardiac arrhythmia. With this condition, the top two chambers of the heart – the atria – don’t contract properly. Instead of strong, regular contractions, the atria quiver, sometimes with as many as 600 beats per minute.
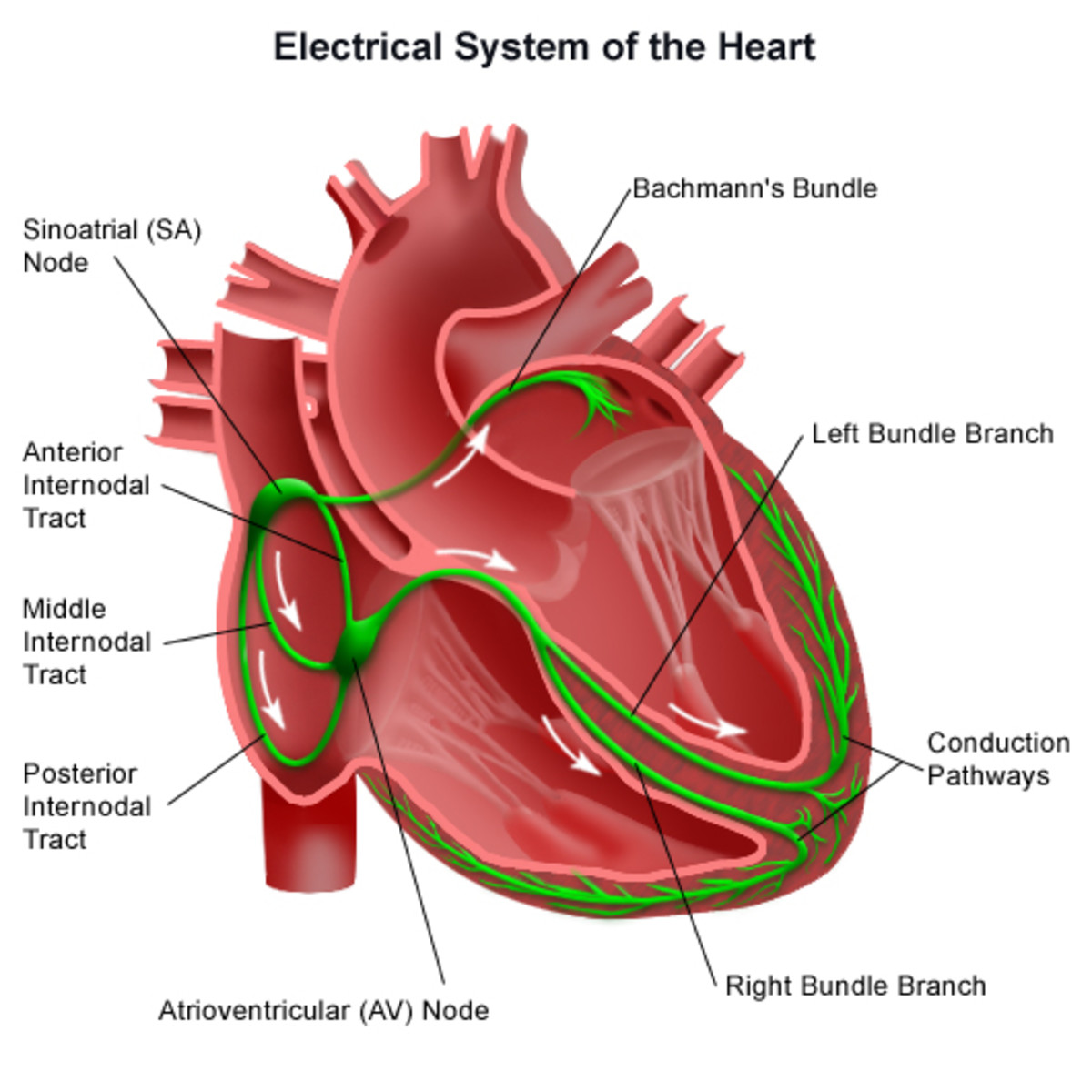
The heart has four chambers – the two atria at the top, along with two ventricles at the bottom. The sinus node is what makes the heart beat. Each heartbeat begins in the right atrium, when the SA node sends the signal to that part of the heart. The heart rate depends on how much oxygenated blood the body needs at the time, with a faster rate for exercise and a slower rate for rest. When this electrical impulse is sent, it makes both atria contract, which pumps blood into the ventricles.
The signal then passes through the AV junction to the ventricles, signaling them to contract. This pumping action forces blood out of the heart. The blood from the left ventricle goes to the body, while the blood from the right ventricle goes to the lungs.
With atrial fibrillation, the atria are bombarded by faulty signals, making them beat rapidly, irregularly, and inefficiently – blood is not effectively pumped into the ventricles. Only a percentage of these chaotic beats ever make it to the ventricles, however. Even so, the rapid beats of the atria will produce an overall heartbeat that is often irregular and much faster than in a normal heart rhythm.
A-fib often begins as a paroxysmal condition. In other words, it might come and go, lasting for just a few minutes to several days. Many people don’t even realize that they have a-fib, so it’s often untreated at this point. This could result in more frequent and longer lasting episodes, making a-fib a chronic condition.
Symptoms of atrial fibrillation
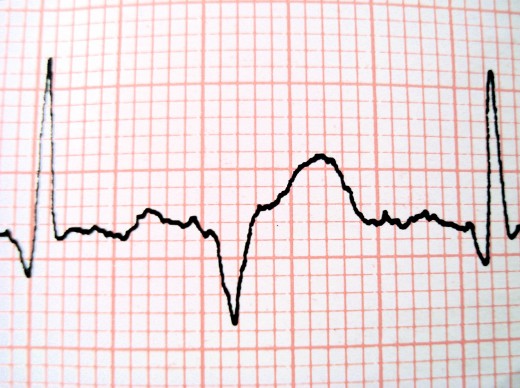
Some people have atrial fibrillation and don’t even realize it until they have a routine ECG. Most people, however, experience shortness of breath, fatigue, dizziness, and/or chest discomfort or pain. Patients might also feel their heart “racing” or feel like they’re going to faint.
My husband never experienced any chest pains, but he did have some of the other symptoms. He felt very tired for a couple of weeks, and one day as he was walking up a slight incline, he couldn’t catch his breath and had to sit on the ground for a few minutes. He felt fine the next day, but later, he began feeling light-headed. He still tried to ignore the symptoms. When it got to the point that he was having difficulty breathing even at rest, he finally went to the doctor.
What causes atrial fibrillation?
Cardiologists aren’t always sure what causes atrial fibrillation. Things that might contribute to a-fib include sleep apnea, heavy drinking, caffeine use, hypertension, obesity, smoking, lung disease, hyperthyroidism, stress, diabetes, serious infections, electrolyte imbalances, and genetic factors.
In some patients, there’s an underlying heart disease or condition, but in others, the heart is otherwise healthy. Some of the conditions that might cause a-fib include pericarditis, cardiomyopathy, coronary artery disease, heart valve disease, and a blood clot in the lungs.
How is atrial fibrillation diagnosed?
A-fib will show up on an ECG, an electrocardiogram. So if you’re having atrial fibrillation while you’re getting an ECG, it will be revealed. If, however, your bouts of a-fib come and go, you might not be having an episode at the exact time you have an ECG. In that case, your doctor might prescribe a Holter monitor.
A Holter monitor is like a mini-ECG machine that you wear for a short period, ranging from 24 hours to three days. During the time you wear the monitor, your heart’s rhythm and electrical impulses are recorded and stored on the device. When you return the monitor to your health care team, the information stored will be retrieved and read.
If you and your physician think that you’re having episodes of a-fib that occur too infrequently to be recorded on a Holter monitor, you might be asked to wear a portable event monitor. Instead of recording information 24/7, as with a Holter, the portable event monitor is patient-activated. You turn it on when you’re having symptoms. Most patients who use a portable event monitor wear the device for several weeks.
How is atrial fibrillation treated?
With my husband’s first bout with a-fib, his heart rate was 150. He was placed immediately in our local ICU, where several IV drugs were administered. He was given Cardizem, which slows the heart rate and prevents the ventricles from beating too fast. He was also given sotalol, which is an antiarrhythmic that helps the heart maintain a normal rhythm.
Since blood clots are a major complication with a-fib, patients are also given “blood thinning” antiplatelet or anticoagulant medications to decrease the chance of stroke. In my husband’s case, Coumadin was administered.
By the time my husband left the hospital, his heart rate was slower, but he was still in a-fib. He was prescribed oral medications to take at home, including Coumadin. Because he was on Coumadin, he had to go to a clinic once a week to check his blood, in order to make sure it wasn’t too thick or too thin.
One option that is often effective for treating a-fib is cardioversion, when the heart is “shocked” back into rhythm. A side effect of cardioversion is blood clots. As a result, our cardiologist wanted hubby to be on Coumadin for a month before he underwent cardioversion. Fortunately, his heart rhythm had returned to normal on its own by that time, so he didn’t have to be converted.
Hubby’s second bout with a-fib occurred just recently. Again, he began to have trouble breathing and had no energy. He thought he had bronchitis at the time, so he went in for a breathing treatment and found out he was in a-fib again. He stayed in ICU for seven days. At home, he continued taking Coumadin every night and sotalol twice a day. When he went in for his checkup on this past Wednesday, the ECG revealed that he was still in a-fib, so cardioversion was scheduled.
Hubby just had the cardioversion this morning, and I was amazed that it only took about five minutes! He was sedated, so doesn’t remember a thing about the procedure. His heart is now in normal rhythm, and he’s already feeling better. As a matter of fact, we’re going out with friends tonight.
Cardioversion works about 90% of the time, according to our cardiologist. It’s not always a permanent solution, however. If you’ve had more than one bout with a-fib, the chances are that you’ll have it again, even after being converted.
A longer term cure for atrial fibrillation is ablation. With this procedure, a catheter is inserted into the groin and threaded up and into the heart, near the pulmonary veins. The tissue around the pulmonary veins is cauterized, separating them from the left atrium. Because of this separation, the rest of the heart cannot be affected by the chaotic electrical signals. This procedure has about a 70% success rate, with these patients no longer needing to remain on antiarrhythmic drugs. In about 85% of patients who have the procedure, their atrial fibrillation will be at least greatly reduced.
If hubby goes into a-fib again, the cardioversion might not work. In that case, he’ll most likely undergo atrial fib ablation to hopefully correct the problem once and for all. For us, this will mean a trip to Atlanta.
Complications of atrial fibrillation
In most cases, atrial fibrillation is not immediately life-threatening. People live for years with a-fib. The biggest complications of atrial fibrillation are the formations of blood clots, resulting in strokes.
If a-fib is left untreated and is not brought under control, the heart is weakened over time. Because your heart doesn’t pump blood effectively, there won’t be enough to meet your body’s demands. This could lead to one of the major complications of atrial fibrillation - heart failure.
Read more about health:
- Atrial Fibrillation Complications
If you have a-fib, you're concerned about atrial fibrillation complications. My husband suffers from this condition, along with several of its symptoms. In his case, they include fatigue, dizziness,... - Primary Peritoneal Cancer: Symptoms, Diagnosis, Treatment, and Clinical Trials
Primary peritoneal cancer, or PPC, is a rare type of cancer that attacks primarily women and is often considered to be a gynecologic cancer. It's a very aggressive type of cancer and can spread quickly to... - Avoid knee surgery with synovial fluid injections - video included
If you have knee pain and stiffness from arthritis or injury and are considering knee replacement, you might be able to avoid surgery with injection therapy. Many doctors, especially orthopedic surgeons, are... - Night Sweats: Causes and Treatment, with Helpful Videos
Sometimes I wake up in the middle of the night sweating, even in the winter. And we keep our house cold, so I dont think its because Im overheating. Its a strange feeling and difficult to explain.... - How to Recognize the Symptoms of Alzheimer's
Alzheimers is a terrible disease. In fact, Im convinced that its just about the worst fate that can befall a human being. Not only is Alzheimers tragic for the person who suffers from it ...