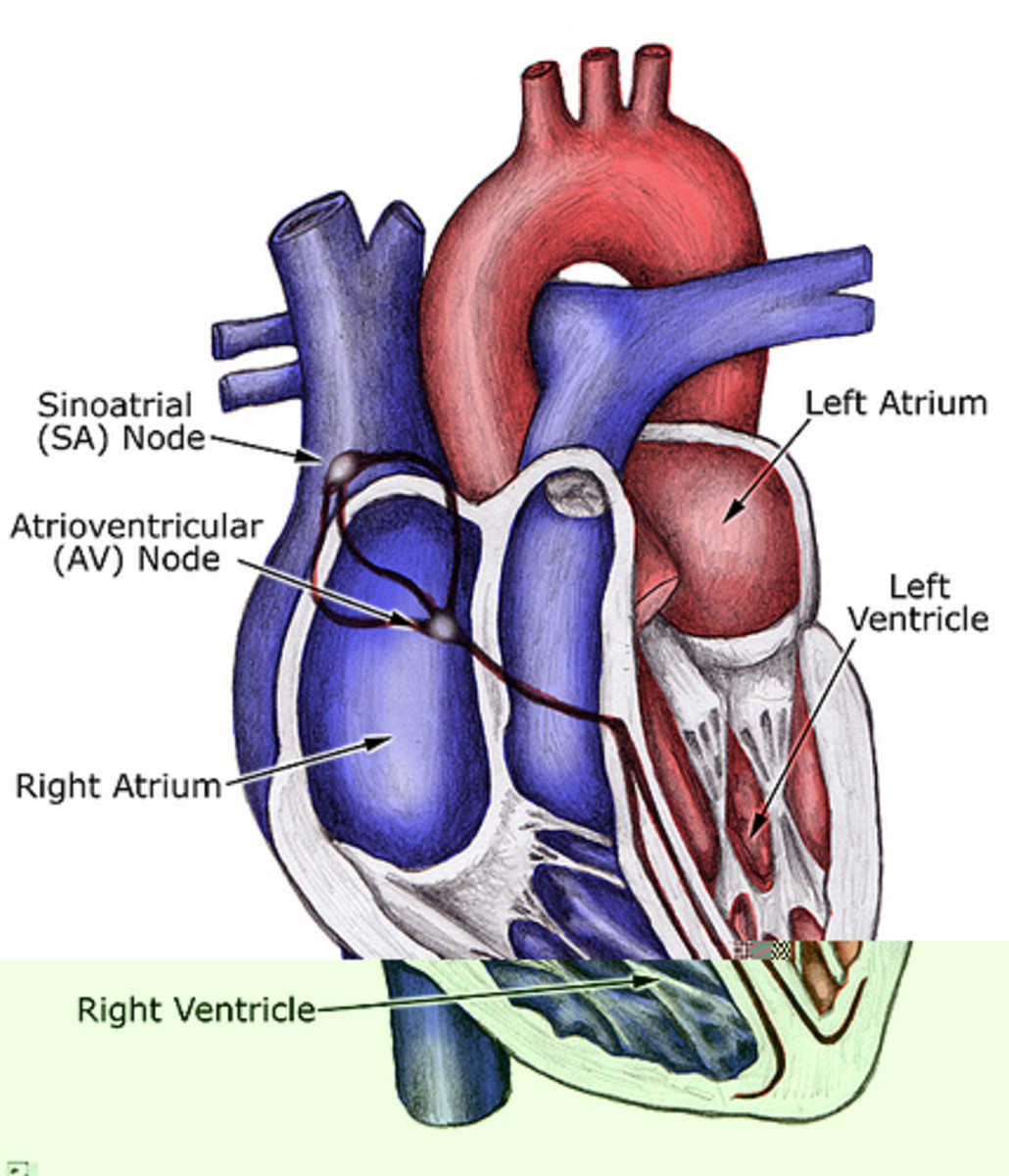
The Braden scale tool used by patients suffering from heart failure
Abstract
This paper seeks to expound on the research undertaken to inform my patient who is suffering from heart failure about the Braden scale assessment. The Braden scale is a tool used for assessment during the determination of patient’s risk levels for contracting skin breakdown. It has been tried in long-term and acute care settings. It is based on items developed following expert consensus. Sensitizing the patient on the Braden scale and encouraging the patient to do a range of motion (ROM) exercises, coupled to therapy will provide an optimal level of health. The Braden scale evaluates skin breakdown in six aspects; sensory discernment, moisture, activity, mobility, nutrition and overall friction, including wear and tear. Higher scores on the Braden scale signify a better prognosis whereas a score lower than 16 is suggested as an indication of those at a higher risk of developing a pressure sore.
Braden scale risk assessment

Introduction
PICOT question;
P: The patient population is an elderly female with heart failure, incontinence, impaired, inability and impaired nutrition.
I: The use of Braden Scale to determine the risk of the pressure sore.
C: use of the Braden Scale compared.
O: useful by reducing the risk of pressure sores development.
T: no new pressure sores in 60 days.
For a patient with heart failure and post left hip replacement in ICU setting(P), does the use of Braden scale assessment (I)reduce the future risk of pressure sores(O) compared with not using the Braden scale assessment(C)in 60 days (T)?
Mrs. A is a 72-year-old Asian-American woman height 5’9”, she weighed 140lbs and was admitted to the Intensive Care Unit (ICU) as a result of heart failure. She is a retired military officer who lives by alone. She suffers from orthopnea and dyspnea, which have gradually worsened over the last five years. Her health history includes having a myocardial infarction two years ago. She also has a history of hypertension for which she is being treated with Verapamil 80 mg daily. She has multiple medical conditions and is slowly becoming feeble. Her other diagnoses are status post left hip replacement. She has fallen several times, which resulted in the left hip fracture. As she was admitted to the ICU, her medications were adjusted due to her current condition. She is alert but appears anxious. Her current physical assessment reveals that her lungs sounds are clear to auscultation, her abdomen is flat, and bowel sounds are present in all four quadrants. She has muscular atrophy and weakness in all extremities, and there is 2+ pitting edema in both feet and ankles. During hospitalization, Physical Therapy (PT) and Occupational Therapy (OT) were ordered for ROM and activities of daily living (ADL) training. But she refused therapy and said, “I don’t want to do anything and just want to lie in bed.” However, she consumes an average of 50 % of each meal. She can feed herself if the tray is set up. She is incontinent of urine and stool. When the caregivers turn her, they occasionally find her wet. The morning shift nurse reported that there was a 2 cm X 1 cm non-branch able reddened area noted on her coccyx. Ms. A was turned and repositioned every 2 hours to keep the pressure from bony prominences including coccyx area. By using Braden Scale, nursing staff concluded that she was at risk for developing pressure sores. The nurse explained her condition to her and discussed the likelihood of her developing pressure sore according to the Braden scale. The patient stated “I don’t believe in this Braden Scale. Is this scale even valid for assessment?”
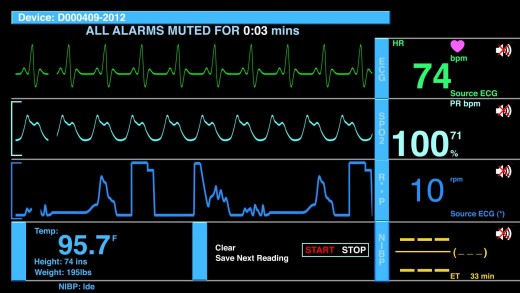
Author’s objective
• To identify risk assessment scales for pressure sores that have been applied in Intensive Care Units
• To determine, based on the available facts, the effectiveness of the Braden Scale in reducing the occurrence of pressure sores in an elderly female patient.
• To keep the patient’s body free from any skin tear.
• To provide client teaching, since this is an integral part of the nursing process
• To sensitize the patient on the importance of the Braden scale in minimizing the magnitude of her pressure sores.
Search process
Outline
A methodical review of the current scientific literature on pressure sore risk analysis scales for Intensive Care units.
Search method
The search was done on the following databases: CUIDEN Plus (Fundación Index Spain), Spanish Medical Index (Índice Médico Español – IME), MEDLINE, Latin American and Caribbean Center on Health Sciences (LILACS), Cumulative Index to Nursing and Allied Health Literature (CINAHL), The Cochran Library, InterSciencia (Wiley), Centre for Reviews and Dissemination of the University of York, Current Contents, EBSCO Online, ScienceDirect, Springer, Pascal, ProQuest. A detailed search approach was conducted tailored to each database, including at least the following parameters: “pressure ulcer” or “decubitus ulcer” or “pressure sores” or “risk assessment” and “bed sores”. No language restrictions were applied for the investigation and in the closing selection articles available in English, Spanish, French, Portuguese, Italian and German were used. Furthermore, a reverse exploration was done grounded on the bibliographical references of the studies chosen. When required, the authors of the articles were directly reached to ask for extra validation data. The evaluation incorporated studies published in the period between 1962 and December 2009 that fulfilled the following requirements: the articles had to include a mechanism to evaluate pressure sore risk, with a clinical test or potential study plan, together with patient follow-up, presenting the results of clinical validation indicators or calculating these if possible. The following were excluded: expressive studies, unpublished articles, exposition or cross-sectional studies and probable studies with a percentage of loss to follow-up over 25% together with studies relating to patients with pressure sores on admission.

Criteria used for the search
Data was obtained by a researcher and scrutinized by another autonomously to preempt errors. The data was collected on an ad hoc sheet that contained the following variables:
• For all studies: study citation (author and year of publication), scale and cut-off point, type of facility, sampling method utilized, sample size, number of patients lost, average age, follow-up period, lowest category of ulcers included and whether the study analyzed predictive validity and/or capacity and/or reliability.
• Predictive validity analysis: number of valid samples, pressure ulcer incidence, sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV), effectiveness or correct percentage and area under the ROC curve.
• Predictive capacity analysis: relative risk (including a CI of 95%).
• Reliability analysis: correlation (Pearson’s index or Intra-class correlation coefficient) and agreement between authors.
Data synthesis: An aggregated breakdown was done on the scales with two or more applicable studies using the indiscriminate effects mock-up. Heterogeneity was calculated by the use of the Q statistic and was complemented by calculating the values
Overall effectiveness of interventions and statistical significance
Interventions
Interventions for the patient included;
i. Total skin assessment. A halogen light can be used to search for any difference in skin color. This may be purple hues or any other discolorations depending on the patient’s skin tone.
ii. Assessment of internal and external risk factors. Note Risk assessment scores and execute prevention procedures based on the score, lowest sub scores, and in-depth assessment for any other risk factors.
iii. Application of the Braden risk analysis. This involved the Braden scale which is a standardized tool for undertaking a risk assessment. It involves documenting risk assessment scores and implementing prevention strategies based on the overall scores.
iv. Employing the three-group risk assessment tool. This involves regularly assessing the skin.
v. Qualitative analysis and the classification of skin tears based on the Payne-Martin system. Lubricants, protective dressings, and the correct lifting procedures to preempt injury when moving the patient.
Statistical studies for the interventions
These studies identified risk evaluation scales particularly intended for ICUs. The characteristics of these scales are revealed above. Most of the critical-care scales were designed in the United States or the United Kingdom; however, some were also designed in Germany, Spain, and Japan. 62.5% were designed for adults. Half of them were built with designs based on previous sales,
18.75% was grounded on clinical exploration, 12.5% based on varied methods including; research and prior sales and the rest grounded on risk factors (6.25%), experts (6.25%) or no data was availed in this regard. Most (43.75%) are reverse scales, with a higher score and lower risk, followed by straight score scales of a higher score and greater risk (31.25%), whereas the rest (25%) are numerical functions. Half of the scales did not characterize terms; a quarter had reasonably defined terms, and the rest had explicitly defined terms.
Similarities and differences of effects
Similarities
The BM Choi Song scale exemplifies the greatest sensitivity and NPV; however, it has only been tried in very insignificant samples of patients. It also exemplifies the best RR value. Its lofty heterogeneity means that it cannot be taken into consideration. Two scales are very comparable, regardless of being long considered to be the same scale. These are the Cubbin-Jackson and Jackson-Cubbin scales, the latter being an adjustment of the former designed in 1999 by Christine Jackson. Both have equal sensitivity and NPV. They have an increased efficiency than the first scale. The first adaptation also has a superior RR value, but its confidence interval is too broad. Both scales have been tried in very few patients to be declared adequate. The Norton scale presents comparable results to the original scales, giving excellent sensitivity and NPV, excellent RR values although with a very broad confidence interval. It has also been tried in a negligible number of subjects. The Braden Scale has gone through a complete corroboration procedure in the ICU environment. It strikes a good poise between sensitivity, NPV, efficiency and RR with a rigid confidence interval. It also has a superior RR value; it has been tried in a satisfactory number of subjects and presents firm confidence intervals.
Differences
Unlike other approaches such as the assessment of internal and external factors and the total body assessment, the Braden scale analysis for pressure sore largely depended on the medical practitioner administering the analysis.
Evaluation
Consistency has mostly been calculated using Pearson’s R statistic. This is not a good technique for estimating inter-observer dependability because it fails to consider instances of arbitrary concurrence, prompting elevated correlation values and forcing researchers to employ the weighted Kappa index as a tolerable estimator or the Intra-class correlation interval to correct this indiscriminate effect. Dependability data could not be aggregated owing to the lack of studies. The Waterlow scale once again offers the least parameters. Reliability studies have been tried in very few patients.