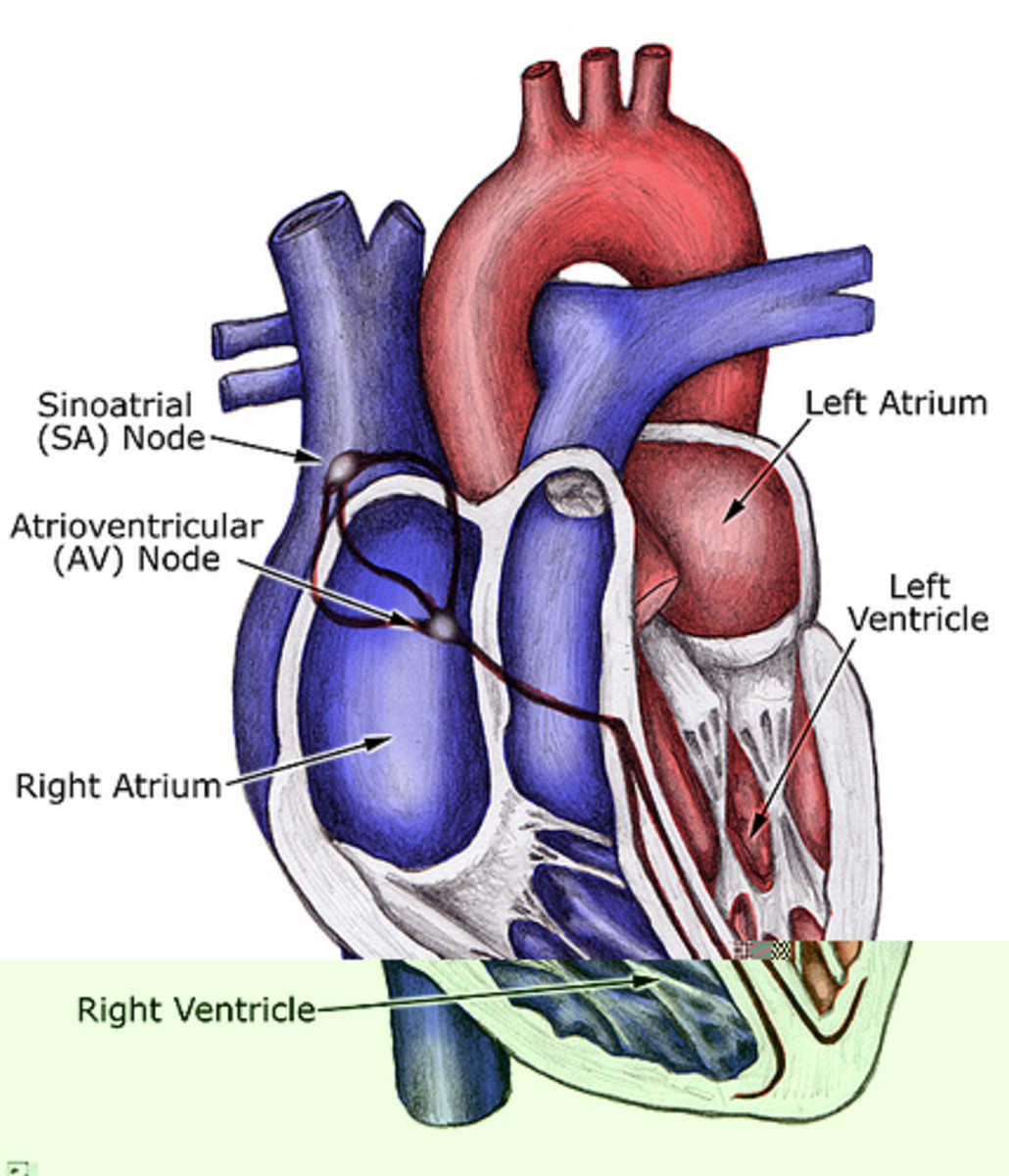
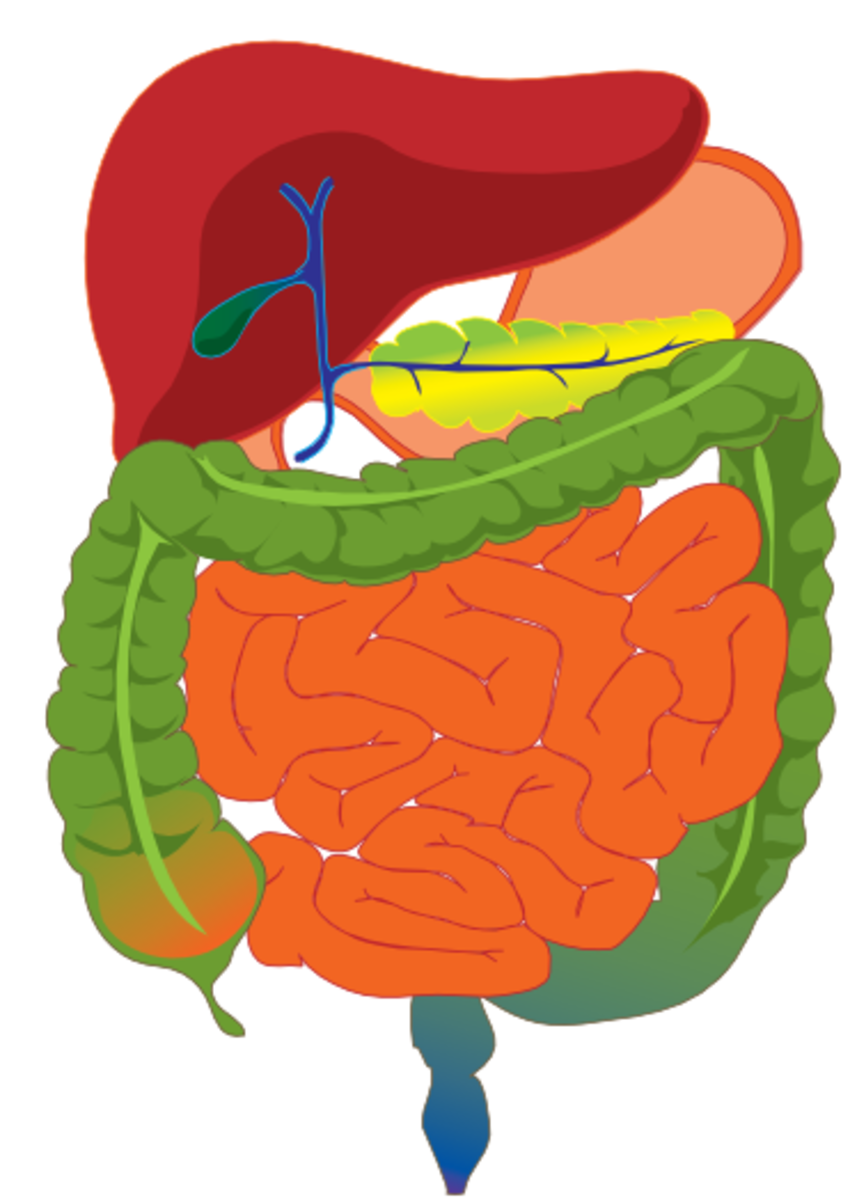
Acute Intermittent Porphyria - an Inherited Blood Disorder
What is Acute Intermittent Porphyria?
Acute Intermittent Porphyria (AIP) is one of several diseases that affect the digestive tract, skin and nervous system because of the buildup of toxins related to the creation of hemoglobin in your blood. People with porphyria have an enzyme that is reduced or operating incorrectly. Some medical historians believe that King George III of England had AIP, which caused his bouts of psychological symptoms. The movie Madness of King George described his battle with the disease. Other forms of porphyria that affect the skin when exposed to sunlight have been offered as the source for vampire mythology. AIP, however, does not affect the skin in the same way. Most symptoms of AIP involve abdominal pain and psychiatric / neurological issues.
How is porphyria inherited or acquired?
Porphyria is almost always inherited. AIP in particular is autosomal dominant, which means that children of someone with AIP or who is a carrier for the gene has a 50% chance of inheriting it regardless of if the other parent has it or not.
How is porphyria diagnosed?
Porphyria is very rare (approximately 1 in 50,000 among all the types together). Therefore, most people with porphyric attacks go misdiagnosed if only because doctors don't consider it or see it as being so rare that more obvious and frequent diseases such as irritable bowel syndrome or major depression are more likely to be the culprit.
What are the symptoms of porphyria?
AIP comes in attacks which can be as infrequent as once in a lifetime or seemingly constant. Significant abdominal pain is the most frequent complaint. Many case studies exist that describe patients who have had their appendix and gallbladder removed before doctors eventually realize the symptoms are really porphyria. Attacks can last between hours to weeks.
People suffering from porphyria frequently also have neurological symptoms such as dizziness, hallucinations, memory loss or even coma.
The name “Porphyria” comes from the greek word for 'Purple' because patients' urine during attacks tend to be very dark and turn red or purple when exposed to sunlight. This happens because the porphyrins that build up in the urine break down into red colored toxins in light.
How is porphyria treated?
Acute Intermittent Porphyria does not have a cure. Attacks can be lessened or possibly prevented by avoiding diet and drug triggers. Barbiturates, seizure medications and other drugs can trigger attacks. Foods such as broccoli, alcohol and high-sulfite foods can also trigger attacks. Carefully avoiding known triggers can help. Crash dieting and low-carb diets such as Atkins are definitely out.
For severe attacks, IV infusions of glucose or a drug called Panhemetin can stop symptoms.
What is the prognosis for people with porphyria?
Once a patient knows he or she has AIP and makes doctors aware of it, they frequently can live normal life expectancies. Most deaths and long-lasting effects come from improperly prescribing extremely porphyrigenic drugs. However, even diet and stress triggers can cause so many and so severe attacks that the toxins build up and damage the liver until the patient eventually needs a liver transplant. For reasons that aren't fully understood, some people are merely carriers of the AIP gene and never become symptomatic. However, once a family is known to carry the AIP gene, members should make sure family members are aware in case offspring eventually become symptomatic. They can make sure their doctors are aware of the history and consider an AIP attack for abdominal and neurological symptoms.
People with Porphyria are up against the fact that this rare disease is poorly publicized, and there are few support groups for them. However, new porphyria support and information sites are being formed to provide that sense of community.
How can porphyria attacks be prevented?
People who know they are carriers of the gene or have had attacks in the past should wear a MedicAlert bracelet or similar way of informing health providers that they should not be prescribed attack-generating drugs.