Ailments causing Bronchial obstruction- Especially, Chronic Obstructive Pulmonary Diseases (COPD)
clinical findings of Bronchial obstruction
Bronchial Obstruction
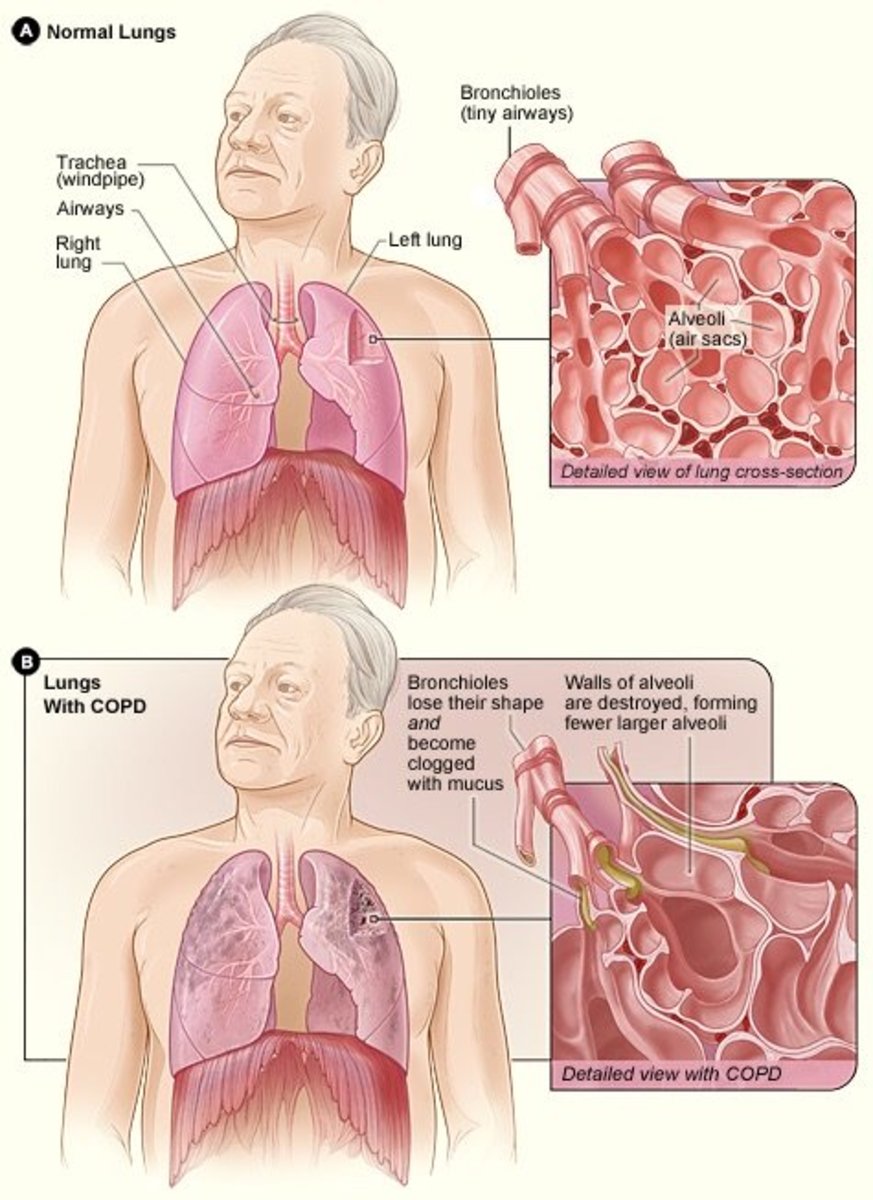
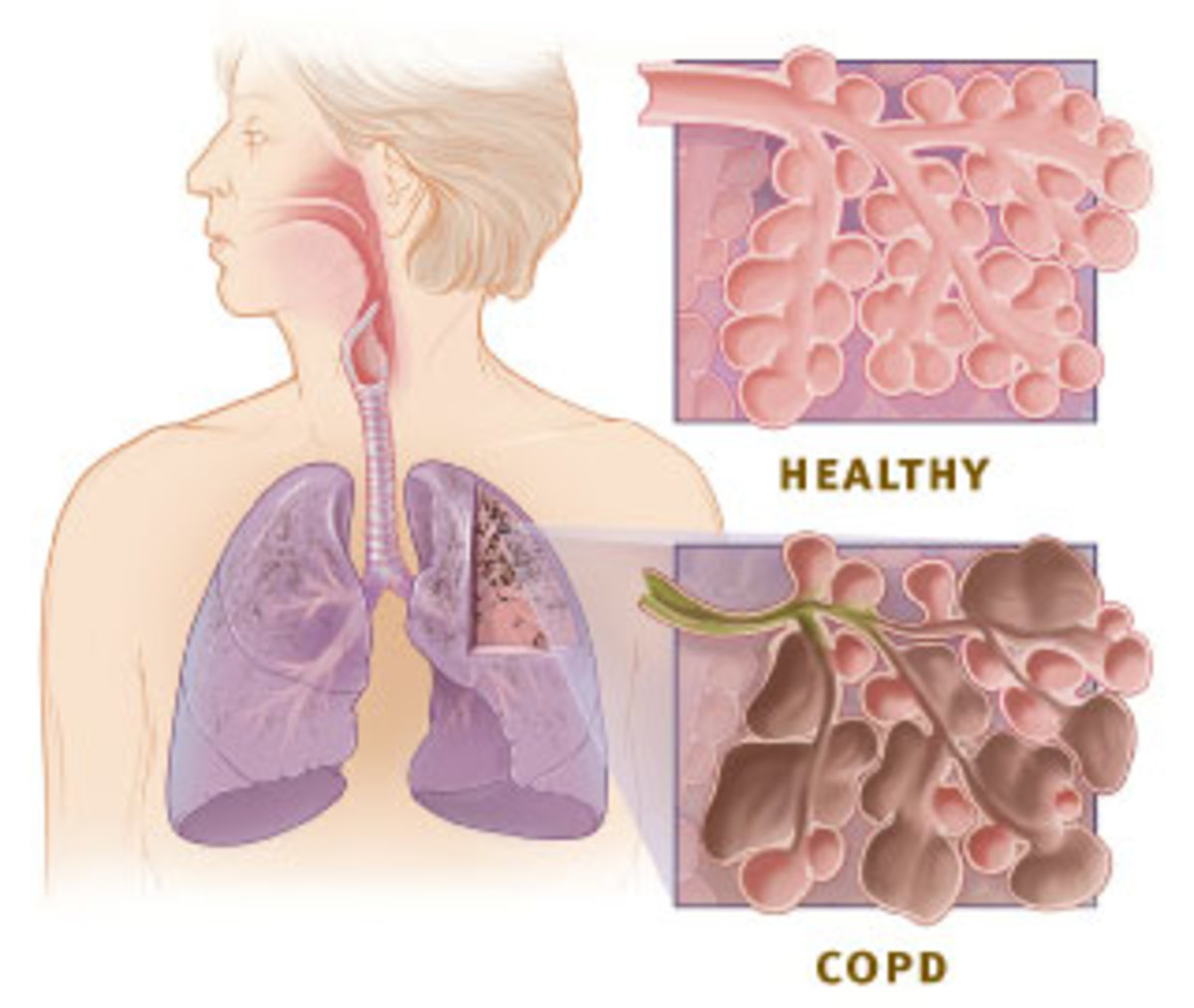
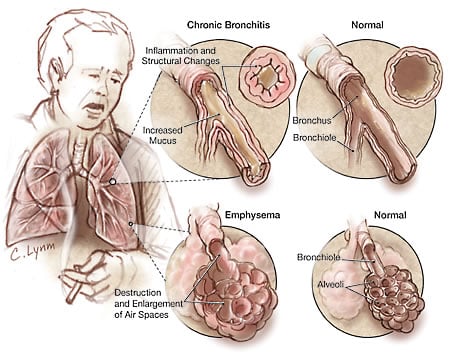
COPD and Bronchial Asthma are the most common diseases of the Lungs in which 4-10% of Adults in the world are ill of COPD. In Europe, 7.4% of people have COPD and mortality of such patients is 10%. According to Gold (Global initiative for Chronic Obstructive Lung Disease), COPD is a disease which is characterized by combination of clinical signs of chronic obstructive bronchitis (inflammation and narrowing of bronchi) and emphysema (changes of Lung tissue structure)
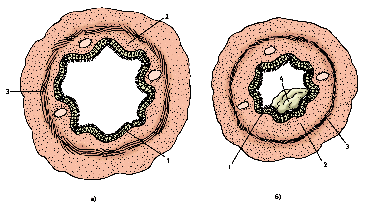
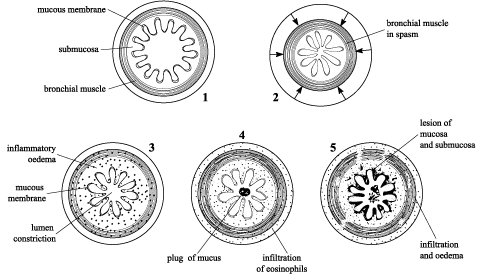
Etiology of bronchial obstruction: a) spasm; b) mucous odema; c) hypersecretion; d) scar narrowing: e) endobronchial tumor; f) external pressuring of bronchus.
Airways obstruction is mainly caused by: Chronic bronchitis, Emphysema, Cystic fibrosis (mucoviscidosis), Bronchial asthma
Pathogenesis of bronchial obstruction is based on ventilation disturbances caused by etiological factor.
Classification of bronchial obstruction is based on spirography estimation of decrease of FEV1: stage 1 >= 70 %, stage 2– 50-69 %, stage 3– < 50 %.
Clinical signs of syndromes:
Bronchial spasm (paroxysmal and steady) – Expiratory dyspnoe, dry cough, dry rales. Accent of second sound on a. pulmonale, on ECG overloading of right ventricle. X-ray examination – acute enphysema. Decrease of symptoms after administration of broncholytics.
Bronchial inflammation (diffuse and local) – common symptoms of inflammation associated with pain in trachea or bronchi, cough (dry or wet), rales;
Delay of sputum – dry nonproductive cough associated with bed feeling and high temperature changes on large amount of spurum during coughing and relieve of all symptoms (lung abscess, chronic bronchitis etc.).
Obturation and compression of bronchus – Absence of ventilation in part of lung. Symptoms of lung atelectasis.
Trachea and bronchial narrowing– inspiratory dyspnoe, cough, restriction of chest movements. Symptoms of hypoventilation. Atelectasis in perspective (tumor etc.).
Bronchial drainage disturbances– based on bed function of epithelium and suppressed coughing reflex. Cough associated with wet rales. Degenerative changes in epithelium.
Bronchial mucous hypersecretion – deals with changes of neuro-humoral regulation or irritation of mucosa. In sputum: low amount of leucocytes and a lot of fluid;
Hypersensitivity of bronchus – allergic in origin and is reaction on infection or non infection factors. The main symptoms are: sneezing, cough, wheezing after contact with allergen. In sputum: eosinophylia, Sharko-Laiden crystals.
Clinical peculiarities of bronchial disorders in case of bronchitis, pneumonia, bronchial asthma, bronchoectases,tumors.
Bronchitis. There are obstructive and non obstructive bronchitis. The obstructive btonchitis is the main cause of bronchial obstruction. The most common are the syndromes of bronchial inflammation and delay of sputum. Bronchial spasm is not common.
Bronchial asthma. The main syndrom is bronchospasm with dyspnoe of expiratory type associated with allergic inflamation.
Pneumonia. In 55% of patients are bronchial disorders. Pneumonia may worse the previously persisted bronchial obstruction. The syndromes of inflammation and Delay of sputum and sometimes bronchospasm are usual.
Bronchoectases independently don’t course bronchial obstruction but frequently associates with chronic bronchitis, pneumonia or hiredetary abnormalities that course the obstruction or other syndromes.
Tumors frequently compress the bronchus. Hypoventylation, regional pneumatosis and atelectasis subsequently develops. Syndrom of obturation and compression of bronchus are frequent.
Diagnostic value of laboratory and instrumental investigations for bronchial obstruction and it peculiarities in patients with lung diseases is completely described in methodological instructions to lesson 1 in pulmonology. Its necessary to say that the most important methods of diagnostics are spirometry and peakfluorymetry. The perculiarities of diagnostics in cases of different diseases are described in chapters dedicated to this pathology either in methodological instructions or in handbooks.
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)
Clinically significant, irreversible, generalized airways obstruction associated with varying degrees of chronic bronchitis, abnormalities in small airways, and emphy sema. The designation was introduced because chronic bronchitis, small airways abnormalities, and emphysema often coexist and it may be difficult in an individ ual case to decide which is the major factor producing the airways obstruction.
When it is clear that the patient's entire disease can be explained by emphysematous changes in the lung, the diagnosis "chronic obstructive emphysema" is pre ferred to the more general designation COPD. Similarly, the diagnosis "chronic obstructive bronchitis"should be used when the obstructive abnormality is a di rect result of an inflammatory process in the airways.
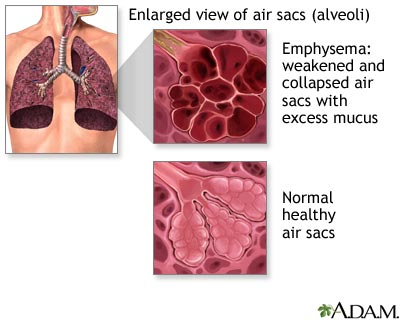
To avoid the semantic confusion often encountered in discussions of these dis orders, the following definitions are provided. Chronic bronchitis, when unquali fied, is defined as acondition associated with prolonged exposure to nonspecific bronchial irritants and accompanied by mucus hypersecretion and certain structural alterations in the bronchi.Clinically, it is characterized by chronic productive cough and is usually associated with cigarette smoking. Pulmonary emphysema is defined as enlargement of the air spaces distal to the terminal nonrespiratory bronchioles, accompanied by destructive changes of the alveolar walls. Airways obstruction is defined asincreased resistance to air flow during forced expiration. It may result from narrowing or obliteration of the airways secondary to intrinsic bronchial disease or from excessive collapse of airways during forced expiration secondary to pulmonary emphysema.
The interrelationships between chronic bronchitis, pulmonary emphysema, and COPD are depicted inFIG. 34-1. Some degree of emphysematous change is ex tremely common in the general population, but not all patients with emphysema have sufficient airways obstructive problems to be considered as having COPD. Similarly, many cigarette smokers have evidence of chronic bronchitis, but only a minority have clinically significant airways obstruction, usually associated with marked changes in the small airways of the lung. As noted in FIG. 34-1, most patients with clinically significant irreversible airways obstruction (COPD) have some combination of chronic bronchitis and emphysema. It is uncertain, however, whether this overlap results from a common causal factor or whether emphysema and chronic bronchitis predispose to one another.
Etiology
The development of chronic bronchitis, emphysema, and chronic airways ob struction appears to be determined by a balance between individual susceptibility and exposure to provocative agents.
The basic lesion of emphysema apparently results from the effect of proteolytic enzymes on the alveolar wall. Such enzymes can be released from leukocytes participating in an inflammatory process. Thus, any factor leading to a chronic inflammatory reaction at the alveolar level encourages development of emphysematous lesions. Smoking presumably plays a role due to its adverse effects on lung defense mechanisms (particularly by impairing the function of the alveolar macrophage) permitting low-grade inflammatory reactions to develop with conse quent recurrent or chronic release of leukocytic proteolytic enzymes (see Ch. 48). Fortunately, most people can neutralize such enzymes as a result of antiproteolytic activity of the «i-globulin fraction of their sera. In a rare condition known ashomozygotic antitrypsin deficiency, however, the serum antiproteolytic activity is markedly diminished. In such patients, emphysema may develop by middle age even in the absence of exposure to substances that interfere with lung defense mechanisms. In the absence of severe deficiency of ai-globulin in the serum, however, the factors which make some cigarette smokers more susceptible to develop ment of emphysema than others remain uncertain. It is also uncertain why persons with similar degrees of emphysema may have considerably varying de grees of severity of airways obstruction.
With sufficient exposure to bronchial irritants, particularly cigarette smoke, most persons develop some degree of chronic bronchitis. The lesion essential to development of severe airways obstruction is apparently located in the small air ways and may be basically different from the ordinary large airways abnormality which leads to hypersecretion of mucus in most smokers. The reason why small airways abnormalities develop in some patients with chronic bronchitis is uncer tain, but viral or bacterial pulmonary infections in childhood, an unidentified immunologic mechanism, a mildly impaired ability to inactivate proteolytic en zymes (as in heterozygotic antitrypsin deficiency), or unidentified genetic characteristics could be predisposing factors. While typical allergic bronchial asthma is not a common precursor of COPD, the exact interrelationships of these disor ders are not known.
Prevalence
COPD is a major cause of disability and death. In the USA, it is second to heart disease as a cause of disability in Social Security statistics, and reported mortality rates have been doubling about every 5 yr. Its true mortality probably exceeds that from lung cancer. Some of this increase reflects the longer survival of patients who previously would have died of bacterial pneumonia before their COPD became known. Overall, it has been estimated that COPD affects as many as 15% of older men. Symptomatic COPD affects men 8 to 10 times more often than women, presumably as a result of the more frequent, prolonged, and heavier smoking in men; however, the incidence in women is now increasing.
Pathology
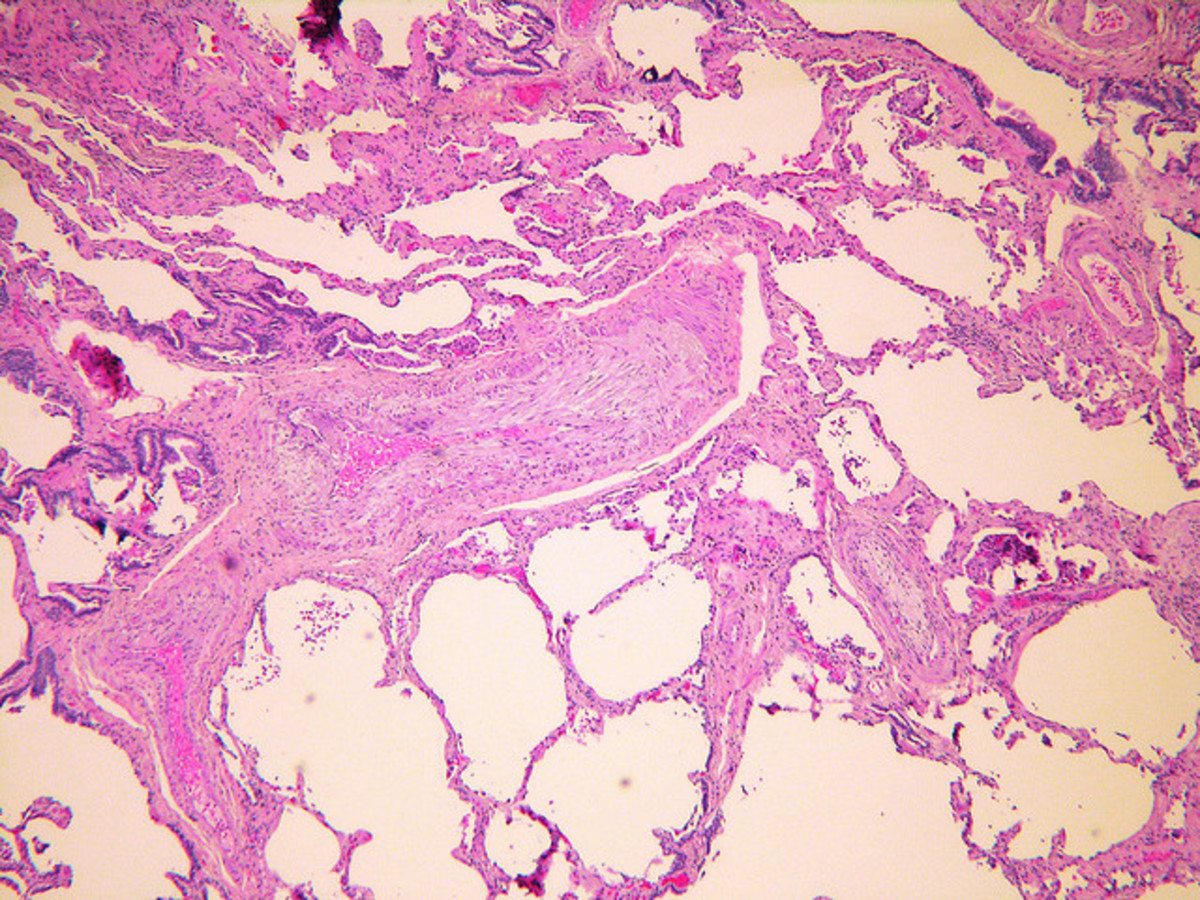
In patients with severe emphysema, the lungs are large and pale and often fail to collapse when the thorax is opened. Microscopic examination reveals "departitioning" of the lung due to loss of alveolar walls. Large bullae may be present in advanced disease. Changes may be most marked in the center of the secondary lobule (centrilobular emphysema) or more diffusely scattered throughout the lobule (panacinar emphysema). In all forms, the normal architecture is destroyed; rupture of septa results in air sacs of various sizes. The number of capillaries in the remaining alveolar walls is reduced, and the pulmonary arterial vessels may show sclerotic changes. These abnormalities lead not only to a reduction in the area of alveolar membrane available for gas exchange, but also to the perfusion of non-ventilated areas and to the ventilation of nonperfused parts of the lung; i.e., ventilation/perfusion abnormalities. They also lead to poor support of the airways of the lung, accounting for excessive collapse of airways on expiration.
In chronic bronchitis, the bronchial walls are thickened, there is mucus in the lumen, and the number of goblet cells and mucous glands is increased. There may be purulent secretions and inflammatory changes in bronchial walls and sur rounding lung parenchyma if infection is present. Such large airways changes do not account for severe airways obstruction, however, and in patients dying of COPD, narrowing or obliteration, or both, of small airways may be observed.
Right ventricular hypertrophy (cor pulmonale) is common in patients with ad vanced respiratory insufficiency.
Clinical pictures of COPD
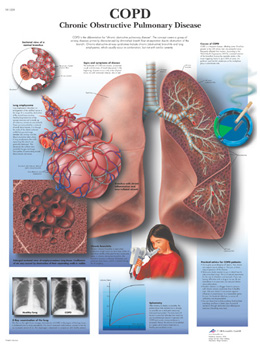

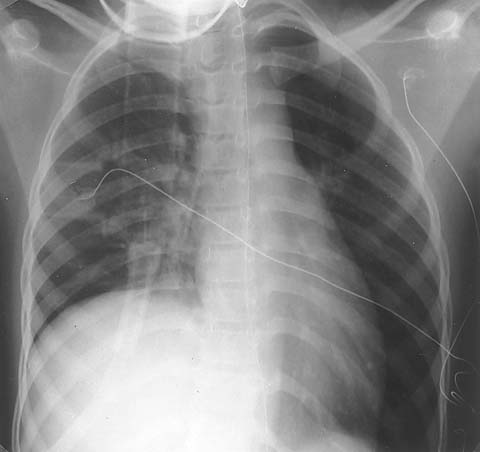
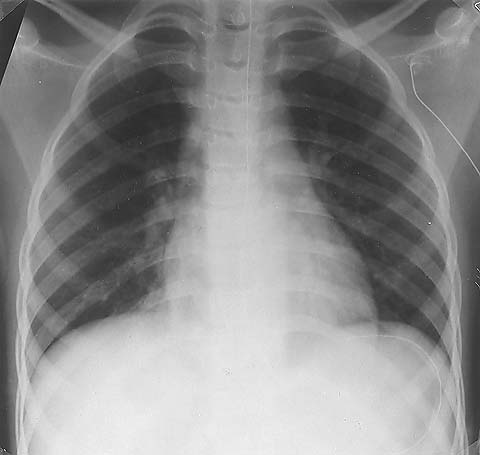
Different variants of the Chest-X-ray and showing COPD
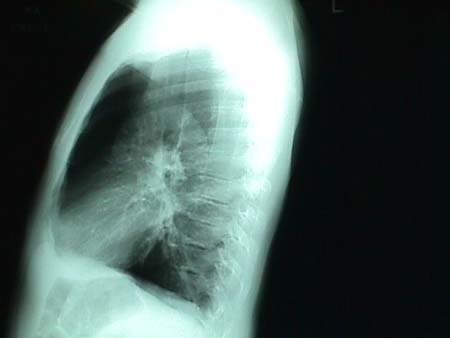
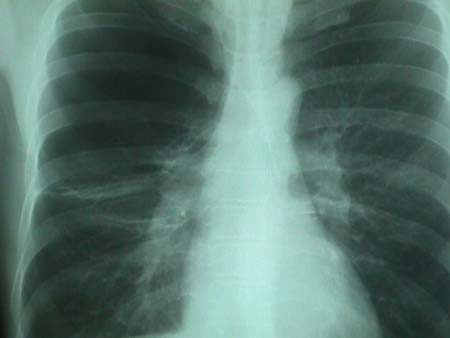
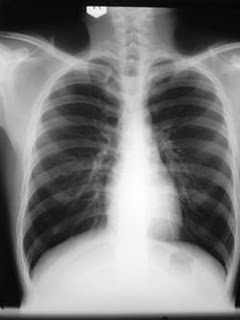
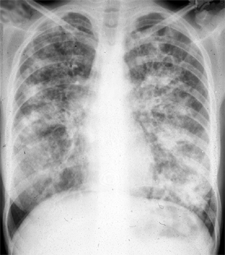
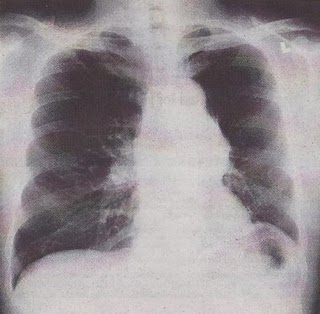
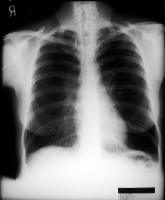
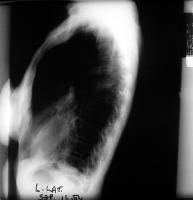
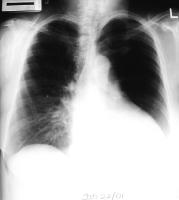
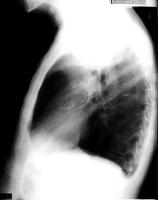
CT scans showing COPD
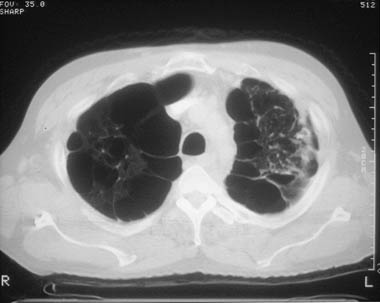
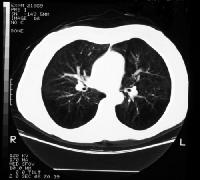
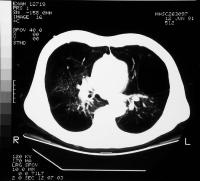
Symptoms, Signs, and X-ray Findings
COPD is thought to begin early in life, though significant symptoms and dis ability usually do not occur until middle age. Mild ventilatory abnormalities may be discernible long before the onset of significant clinical symptoms. A mild "smoker's cough" is often present many years before onset of exertional dyspnea.
Gradually progressive exertional dyspnea is the most common presenting com plaint. Patients may date the onset of dyspnea to an acute respiratory illness, but the acute infection may only unmask a preexisting subclinical chronic respiratory disorder. Cough, wheezing, recurrent respiratory infections, or, occasionally, weakness, weight loss, or lack of libido may also be initial manifestations. Rarely, initial complaints are related to congestive heart failure secondary to cor pulmo nale, patients with such complaints apparently ignoring their cough and dyspnea prior to the onset of dependent edema and severe cyanosis.
Cough and sputum production are extremely variable. The patient may admit only to "clearing his chest" on awakening in the morning or after smoking the first cigarette of the day. Other patients may have severe disabling cough. Sputum varies from a few ml of clear viscid mucus to large bronchiectasis-like quantities of purulent material.
Wheezing also varies in character and intensity. Asthma-like episodes may oc cur with acute infections. A mild chronic wheeze that is most obvious on reclining may be noted. Many patients deny having any wheeze.
The physical findings in COPD are notoriously variable, especially in early cases. A consistent abnormality is obstruction to expiratory air flow manifested by a slowing of forced expiration. To demonstrate this, the patient is asked to take a deep breath and then empty his lungs as quickly and completely as possible. Forced expiration is normally virtually complete in < 4 seconds. This test, which should be part of every routine physical examination, may be abnormal even though the patient does not complain of dyspnea.
Other findings, including bronchi, diminished vesicular breath sounds, tachy cardia, distant heart tones, and decreased diaphragmatic motion, are not consis tently present. The typical findings of gross pulmonary hyperinflation, prolonged expiration during quiet breathing, depressed diaphragm, pursed-lip breathing, stooped posture, calloused elbows from repeated assumption of the "tripod posi tion," and marked use of accessory muscles of respiration are seen only in later stages of COPD. A barrel-chested appearance is an unreliable finding since it is often noted in elderly patients without significant respiratory problems. Late in the disease, there may be frank cyanosis from hypoxemia, a plethoric appearance associated with secondary erythrocytosis, and, in patients with severe cor pulmo nale, signs of congestive heart failure. Mild, chronic, dependent edema is quite common and does not necessarily indicate heart failure. It may result from pro longed sitting, elevated intrathoracic pressures, and renal retention of salt second ary to blood gas abnormalities even in the absence of cor pulmonale. X-rayfindings are also variable. In early stages of the disease, the x-ray is often normal. Changes indicative of hyperinflation (e.g , depressed diaphragm, general ized radiolucency of the lung fields, increased retrosternal air space, and tenting of the diaphragm at the insertions to the ribs) are common and suggestive of emphysematous disease, but are not diagnostic. They may also be found in pa dents with asthma and occasionally m healthy persons Localized radioluceno with attenuation of vascular markings is a more reliable indicator of emphysema
Bullae are seen occasionally with COPD. Large bullae are generally well seen on ordinary x-rays, but small ones are more reliably detected with planograms. They may occur as part of a diffuse emphysematous process or as isolated phe nomena and thus do not necessarily indicate a generalized lung disease.
Bronchitis itself does not have a characteristic appearance on ordinary chest x-ray, but bronchogramsmay reveal cylindrical dilation of bronchi on inspiration bronchial collapse on forced expiration, and enlarged mucous ducts Prank: saccular bronchiectasis is unusual and generally occurs only in patients who have had a previous severe respiratory infection.
In patients with recurrent chest infections, a variety of nondescript postinflammatory abnormalities may be noted, such as localized fibrotic changes, hone^ combing, or contraction atelectasis of a segment or lobe.
Isotopic lung scans generally demonstrate uneven ventilation and perfusion Diagnosis COPD should be suspected in any patient with chronic productive cough or exertional dyspnea of uncertain etiology, or whose physical examination reveals evidence of slowing of forced expiration. Definite diagnosis depends on (1) demonstration of physiologic evidence of airways obstruction which persists despite intensive and maximum medical management, and (2) exclusion of any specific disease (e.g., silicosis, tuberculosis, or upper airway neoplasm) as a cause of this physiologic abnormality.
Spirometric testing reveals characteristic obstruction to expiratory air flow with slowing of forced expiration as manifested by a reduced 1-second forced expiratory volume (FEV1) and a low maximum mid-expiratory flow. Slowing of forced expiration is also evident on flow-volume curves. The vital capacity (VC) and forced vital capacity (FVC) are somewhat impaired in patients with severe disease but are better maintained than the measures of the speed of expiration. For this reason, the FEV1/VC and FEV1/FVC ratios are regularly reduced to < 60% with clinically significant COPD. This degree of abnormality should persist despite prolonged, maximal therapy before a diagnosis of COPD is considered confirmed
Maldistribution of ventilation and perfusion occurs in COPD and is manifested m several ways. An excessive physiologic dead space ventilation indicates that there are areas of the lung in which ventilation is high relative to blood flow (a high ventilation/perfusion ratio), resulting in "wasted" ventilation. Physiologic shunting indicates the presence of alveoli with reduced ventilation in relation to blood flow (a low ventilation/perfusion ratio) which allows some of the pulmonary blood flow to reach the left heart without becoming fully oxygenated, resulting in hypoxemia. In late stages of the disease, overall alveolar underventilation with hypercapnia occurs, aggravating any hypoxemia present due to physiologic shunting. Chronic hypercapnia is usually well compensated, and pH levels are close to normal.
The pattern of physiologic abnormality in an individual case depends to some extent on the relative severity of intrinsic bronchial disease and anatomic emphy sema. Diffusing capacity is regularly reduced in patients with severe anatomic emphysema, but is more variable in patients with airways obstruction associated with predominant intrinsic bronchial disease. In patients with severe emphysema. resting hypoxemia is usually mild and hypercapnia does not occur until terminal stages of the illness. In these patients, cardiac output may be quite low, but frank pulmonary hypertension and cor pulmonale are usually late developments. In patients with airways obstruction associated primarily with an intrinsic bronchial disorder, severe hypoxemia and hypercapnia may be noted relatively early. Such patients usually have a well-maintained cardiac output and tend to develop severe pulmonary hypertension with chronic cor pulmonale. The residual volume (RV) and total lung capacity (TLC) are markedly elevated in emphysematous patients, while pulmonary hyperinflation may be relatively slight in bronchitic COPD, but the ratio of RV to TLC tends to be elevated in both types of disease.
Detailed lung function measurements help to determine the severity of emphy sema and intrinsic bronchial disease in an individual case, but are rarely needed for ordinary clinical evaluation. With severe emphysema, pressure-volume curves show a characteristic loss of recoil and increased compliance. Airways resistance measurements made in the body plethysmograph tend to reflect the severity of intrinsic bronchial narrowing.
In a few cases with severe emphysema but little bronchitis or with severe ob structive bronchitis but little, if any, emphysema, it is possible to distinguish emphysematous type (Type A) disease frombronchial type (Type B) disease on the basis of clinical and physiologic findings (see TABLE 1). Unfortunately, most patients appear to have a "mixed" syndrome.
Specific parenchymal lung diseases which may lead to airways obstruction can usually be excluded by chest x-ray. Upper airway lesions (generally associated with stridor) and localized bronchial obstructions (often associated with a local ized wheeze) must also be excluded. It is particularly important to exclude pri mary cardiac disease with congestive failure as a cause of the patient's respiratory insufficiency. A normal or small cardiac silhouette on chest x-ray is characteristic of COPD prior to development of frank cor pulmonale, but is most unusual in patients who are dyspneic as a result of a cardiac disorder.
CLINICAL TYPES OF CHRONIC OBSTRUCTIVE PULMONARY DISEASES
Emphysematous (Type A)
Age at diagnosis: 55-75
Cough onset: Often after onset of dyspnea
Sputum: Scanty, mucoid
Recurrent infections: Occasional
Chest x-ray: Normal or emphysematous
Pulmonary artery pressure: Normal or slightly high
Chronic cor pulmonale: unusual
Lung compliance: Normal or high
Recoil pressure: Low
Airways resistance: Near normal
Pulmonary overdistention: Marked
Diffusing capacity: Low
Chronic hypercapnia: Unusual
Chronic hypoxemia: Mild or moderate
Bronchial (TypeB)
Age at diagnosis: 45-65
Cough onset: Usually before onset of dyspnea
Sputum: Copious, purulent
Recurrent infections: Frequent
Chest x-ray: Normal or fibrotic
Pulmonary artery pressure: Often very high
Chronic cor pulmonale: Common
Lung compliance: Normal or low
Recoil pressure: Normal or high
Airways resistance: Elevated
Pulmonary overdistention: Mild or moderate
Diffusing capacity: Variable
Chronic hypercapnia: Common
Chronic hypoxemia: Often severe
Homozygotic antitrypsin deficiency should be suspected when there is a family history of obstructive airways disease, or when emphysema occurs in a woman, a relatively young man, or a nonsmoker. The diagnosis may be confirmed by mea suring serum antitrypsin levels or by specific phenotyping.
Course and Prognosis
Some reversal of airways obstruction and considerable symptomatic improve ment can often be obtained initially, but the long-term prognosis is less favorable in patients with persistent obstructive abnormality. After initial improvement, the FEV1 generally falls 50 to 75 ml/yr, which is 2 to 3 times the rate of decline expected from aging alone. There is a concomitant slow progression of exertional dyspnea and disability. The course is punctuated by acute symptomatic exacerba tions, generally related to superimposed bronchial infections.
Prognosis is closely related to the severity of expiratory slowing. When the FEV1 exceeds 1.25 L, the 10-yr survival rate is about 50%; when the FEV, is 1 L, the average patient survives about 5 yr; when there is very severe expiratory slowing (FEV1 about 0.5 L), survival for > 2 yr is unusual, particularly if the patient also has chronic hypercapnia or demonstrable cor pulmonale.
Treatment
Therapy does not result in cure, but provides symptomatic relief and controls potentially fatal exacerbations. It may also slow progression of the disorder, though this is unproved. Treatment is directed at alleviating conditions which cause symptoms and excessive disability (e.g., infection, bronchospasm, bronchial hypersecretion, hypoxemia, and unnecessary limitation of physical activity).
Infection: An attempt should be made to clear purulent sputum with a broad-spectrum antibiotic (e.g., tetracycline 250 mg q.i.d. for 10 days), the course re peated promptly at the first sign of recurrent bronchial infection or sputum purulence. Ampicillin or cephalothin may be used to treat severe exacerbations Regular courses of a broad-spectrum antibiotic are indicated in patients with frequent infectious exacerbations.
Bronchospasm: The degree of reversibility of airways obstruction can be as sessed only by a vigorous and prolonged therapeutic trial of bronchodilators.
Corticosteroids have a very limited role in treating COPD, but a trial of these agents may be required to prove conclusively that the airways obstruction is not a result of potentially reversible bronchospasm. This is especially true when there is a past history suggesting asthma, eosinophilia, fluctuations in the severity of air ways obstruction, or a good immediate response to inhalation of a bronchodilator. If a corticosteroid trial (e.g., prednisone 30 to 40 mg every morning for 3 wk) is undertaken, its usefulness should be documented by objective improvement w spirometric tests before long-term corticosteroid therapy is recommended, al which time the lowest maintenance dose which sustains improvement is used. In some patients, alternate-day therapy can be used for maintenance.
Bronchial secretions: Adequate systemic hydration is essential to prevent 10-spissation of secretions. In some patients bronchial hygiene may also be improved by inhalation of mist, postural drainage, and chest physical therapy, particularly following bronchodilator inhalation. Saturated solution of potassium iodide 10 drops in H20 t.i.d. is used by some physicians in an attempt to thin bronchial secretions. Despite their wide use, IPPB machines have not been shown to im prove the patient's ability to raise secretions or to affect favorably the overall condition of ambulatory patients with COPD.
Hypoxemia: Severe chronic hypoxemia, often associated with hypercapnia, accentuates pulmonary hypertension and leads to development of cor pulmonale in patients with COPD. Recurrent cardiac failure may develop and necessitate long-term 02 therapy. Low flow (1 to 2 L/min) 02 therapy via nasal prongs for 15 h or more/day (including sleeping hours) may be effective in reversing pulmonary hypertension and improving cardiac status. Around-the-clock 02 supplementation has been shown to be preferable for patients with severe chronic hypoxemia (arte rial O2 tensions consistently < 55 mm Hg at rest) and appears to prolong survival. When instituting long-term O2 therapy, it is important to monitor the blood gas responses. No more O2 should be given than is needed to raise the arterial 02 tension to 55 mm Hg. One should also be sure that chronic 02 therapy does not lead to a progressive rise in C02 tension as a consequence of removing hypoxic ventilatory drive; in fact, this has rarely proved to be an important problem.
Even in patients without severe cor pulmonale, O2 may be needed to correct severe exertional hypoxemia when the patient is started on a graded exercise program. Use of 02 for symptomatic relief of dyspnea without verification of severe hypoxemia, however, is unjustified and potentially dangerous.
Hypercapnia: Patients with rapidly developing or worsening hypercapnia re quire immediate hospitalization and intensive therapy, but chronic well-compen sated hypercapnia is generally well tolerated and requires no specific therapy.
Heart failure: The most important measure for controlling heart failure second ary to cor pulmonale is correction of excessive hypoxemia. Diuretic therapy and controlled sodium intake are important adjuncts. Digitalis must be used cau tiously, if at all, since digitalis intoxication readily occurs in patients with COPD, probably as a result of fluctuating blood gas and electrolyte abnormalities.
Exercise tolerance: Prolonged inactivity leads to excessive disability in patients with COPD. As long as there is no severe cardiac disease, it is important to maintain a regular exercise program. This can usually be prescribed directly by the physician. If the patient is severely disabled, however, the program may be more effective if supervised by a trained physical therapist. The exercise program should have a specific meaningful goal (e.g., walking to the store, golfing) and should train those muscles needed for this specific activity. Breathing "exercises" (breathing training) may have a place in treating anxious patients who develop an excessively rapid ventilatory rate during exertion, but such exercises have not been shown to improve ventilatory capacity.
Depression: Periods of severe depression or marked anxiety are frequent in patients with COPD. A vigorous therapeutic program and an enthusiastic physi cian are most helpful. A nihilistic attitude toward management of this disease is inexcusable. The patient must understand the nature of the disease and the goals and expectations of therapy.
Exacerbations: Treat promptly; e.g., if sputum becomes purulent, prescribe a course of broad-spectrum antibiotics and a more intensive program of bronchodilation and bronchial hygiene (see above). Patients with increasing hypoxemia or hypercapnia should be hospitalized promptly for intensive therapy. Sedatives and hypnotics should always be avoided in patients with COPD, particularly during exacerbations, since they increase the risk of acute ventilatory failure
More on COPD



Complications, classification by severity and Treatment
Complications
Acute Bronchitis, Pneumonia, Pulmonary thromboembolism, and concomitant left Ventricular failure may worsen otherwise stable COPD. Pulmonary hypertension, Cor Pulmonale, and chronic respiratory failure are common advanced COPD. Spontaneous Pneumothorax occurs in a small fraction of patients with emphysema. Hemophysis may result from chronic bronchitis or may signal bronchogenic carcinoma.
Classification of COPD (by severity)
This classification is based on stage and severity.
1. Mild- FEV1<80%, FEV1/FVC <70%. As a rule, chronic cough with sputum usually occurs in this stage.
2. Moderate- 50%<FEV1<80%. FEV1/FVC<70%. Symptoms are more significant, presence of dyspnea during physical activity and exacerbation occur.
3. Severe- 30%<FEV1<50%. FEV1/FVC<70%. Symptoms in this stage cause worsening of Life quality.
4. Very severe- FEV1<30%. FEV1/FVC<70% and Chronic renal failure occurs.
Treatment
Principles of treatment
I. Increasing of intensity of treatment in correlation with COPD severity.
II. Permanent basis therapy.
III. Individual sensitivity of patients to different medicines leads to necessity of permanent control
IV. Inhaled medicines are useful
Inhaled Cholynolytics
I. SHort action- (Ipratropium bromide, Berodual H) has more slowly beginning but longer action than B2- agonists.
II. Prolonged action- (Thyotropium bromide, spiriva) is active for 24 hours.
Inhaled Broncholytics
I. B-agonists of short action (salbutamol, fenoterol)- fast beginning of action, but duration is 4-6 hours.
II. B2-agonists of prolonged action (Salmeterol, Formoterol) are active for 12 hours.
Methylxantines
Theophylines of prolonged action are useful- Teopec, Teotard etc.
Glucocorticosteroids
Glucocorticosteroids are useful for permanent basis therapy for patients with COPD III- IV stages and basically, inhaled types are used. Prednisome may be used only during exacerbation and is not recommended for basis therapy. Examples of such are Beclomethasone, Budesonid, FLucasone). Seretid is Glucocorticosteroids + Salmeterol, which is used in patients with III- IV stages of COPD and often exacerbations in anamnesis.
Management
Management of Chronic Obstructive Pulmonary Diseases in all severity involves; avoidance of risk factors (smoking cessation, reduction of indoor pollution, reduction of occupational exposure etc) and also influenza vaccination.
I. Stage 0: CHaracterized by chronic symptoms of cough and sputum. No spirometric abnormalities. The recommended treatment is smoking cessation.
II. Stage 1 (Mild COPD): The recommended treatment is administration of short-acting bronchodilator as needed.
III. Stage 2 (Moderate COPD): Recommended treatment is the administration of the following; short acting bronchodilator as needed; regular treatment with one or more long-acting bronchodilators and as well rehabilitation.
IV. Stage 3 (Severe COPD): Recommended treatment is short-acting bronchodilator as needed; regular treatment with one or more long-acting bronchodilators, inhaled glucocorticosteroids if repeated exacerbations occur and also rehabilitation.
V. Stage IV (Very severe COPD): Recommended treatment is by the administration of short-acting bronchodilator as needed. Regular treatment with one or more long-acting bronchodilators. Also administration of inhaled glucocorticosteroids if repeated exacerbations occur. Complications as well should be treated appropriately and long term oxygen therapy should be administered if respiratory failure occurs. Surgical options could as well be considered.
Acknowledgement and Contributors







sources
- Alsaeedi A, Sin DD, McAlister FA. The effects of inhaled corticosteroids in chronic obstructive pulmonary disease: a systematic review of randomized placebo-controlled trials. Am J Med. Jul 2002;113(1):59-65.
- Anthonisen NR. Prognosis in chronic obstructive pulmonary disease: results from multicenter clinical trials. Am Rev Respir Dis. Sep 1989;140(3 Pt 2):S95-9.
- Anthonisen NR, Connett JE, Kiley JP. Effects of smoking intervention and the use of an inhaled anticholinergic bronchodilator on the rate of decline of FEV1. The Lung Health Study. JAMA. Nov 16 1994;272(19):1497-505.
- Belman MJ, Botnick WC, Shin JW. Inhaled bronchodilators reduce dynamic hyperinflation during exercise in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. Mar 1996;153(3):967-75.
- Brenes GA. Anxiety and chronic obstructive pulmonary disease: prevalence, impact, and treatment. Psychosom Med. Nov-Dec 2003;65(6):963-70.
- Burrows B, Bloom JW, Traver GA. The course and prognosis of different forms of chronic airways obstruction in a sample from the general population. N Engl J Med. Nov 19 1987;317(21):1309-14.
- Casaburi R, Mahler DA, Jones PW. A long-term evaluation of once-daily inhaled tiotropium in chronic obstructive pulmonary disease. Eur Respir J. Feb 2002;19(2):217-24.
- Chapman KR. Therapeutic algorithm for chronic obstructive pulmonary disease. Am J Med. Oct 21 1991;91(4A):17S-23S.
- Davis RM, Novotny THE. The epidemiology of cigarette smoking and its impact on chronic obstructive pulmonary disease. Am Rev Respir Dis. Sep 1989;140(3 Pt 2):S82-4.
- Donohue JF, van Noord JA, Bateman ED. A 6-month, placebo-controlled study comparing lung function and health status changes in COPD patients treated with tiotropium or salmeterol. Chest. Jul 2002;122(1):47-55.
- Dunn WF, Nelson SB, Hubmayr RD. Oxygen-induced hypercarbia in obstructive pulmonary disease. Am Rev Respir Dis. Sep 1991;144(3 Pt 1):526-30.
- Fabbri LM, Luppi F, Beghe B. Update in chronic obstructive pulmonary disease 2005. Am J Respir Crit Care Med. May 15 2006;173(10):1056-65.
- Ferguson GT, Cherniack RM. Management of chronic obstructive pulmonary disease. N Engl J Med. Apr 8 1993;328(14):1017-22.
- Fletcher C, Peto R. The natural history of chronic airflow obstruction. Br Med J. Jun 25 1977;1(6077):1645-8.
- Halbert RJ, Natoli JL, Gano A. Global burden of COPD: systematic review and meta-analysis. Eur Respir J. Apr 12 2006.
- Karpel JP, Kotch A, Zinny M. A comparison of inhaled ipratropium, oral theophylline plus inhaled beta-agonist, and the combination of all three in patients with COPD. Chest. Apr 1994;105(4):1089-94.
- Lopez-Majano V, Dutton RE. Regulation of respiration during oxygen breathing in chronic obstructive lung disease. Am Rev Respir Dis. Aug 1973;108(2):232-40.
- Mannino DM, Watt G, Hole D. The natural history of chronic obstructive pulmonary disease. Eur Respir J. Mar 2006;27(3):627-43.
- McKay SE, Howie CA, Thomson AH. Value of theophylline treatment in patients handicapped by chronic obstructive lung disease. Thorax. Mar 1993;48(3):227-32. [Medline].
- O''Donnell DE, Sanii R, Anthonisen NR. Effect of dynamic airway compression on breathing pattern and respiratory sensation in severe chronic obstructive pulmonary disease. Am Rev Respir Dis. Apr 1987;135(4):912-8.
- O''Donnell DE, Hernandez P, Aaron S. Canadian Thoracic Society COPD Guidelines: summary of highlights for family doctors. Can Respir J. May-Jun 2003;10(4):183-5.
- O''Donnell DE, Parker CM. COPD exacerbations . 3: Pathophysiology. Thorax. Apr 2006;61(4):354-61.
- O''Donnell R, Breen D, Wilson S. Inflammatory cells in the airways in COPD. Thorax. May 2006;61(5):448-54.
- Papi A, Luppi F, Franco F. Pathophysiology of exacerbations of chronic obstructive pulmonary disease. Proc Am Thorac Soc. May 2006;3(3):245-51.
- Pauwels R. Global initiative for chronic obstructive lung diseases (GOLD): time to act. Eur Respir J. Dec 2001;18(6):901-2.
- Peto R, Speizer FE, Cochrane AL. The relevance in adults of air-flow obstruction, but not of mucus hypersecretion, to mortality from chronic lung disease. Results from 20 years of prospective observation. Am Rev Respir Dis. Sep 1983;128(3):491-500.
- Petty TL, Finigan MM. Clinical evaluation of prolonged ambulatory oxygen therapy in chronic airway obstruction. Am J Med. Aug 1968;45(2):242-52.
- Postma DS, Sluiter HJ. Prognosis of chronic obstructive pulmonary disease: the Dutch experience. Am Rev Respir Dis. Sep 1989;140(3 Pt 2):S100-5.
- Prigmore S. End-of-life decisions and respiratory disease. Nurs Times. Feb 14-20 2006;102(7):56, 59, 61.
- Ram FS, Rodriguez-Roisin R, Granados-Navarrete A. Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2006;CD004403.
- Rutten FH, Cramer MJ, Lammers JW. Heart failure and chronic obstructive pulmonary disease: An ignored combination?. Eur J Heart Fail. Mar 10 2006.
- Sanders C. The radiographic diagnosis of emphysema. Radiol Clin North Am. Sep 1991;29(5):1019-30.
- Schachter EN. Cilomilast. Drugs Today (Barc). Apr 2006;42(4):237-47.
- Sutherland ER, Martin RJ. Airway inflammation in chronic obstructive pulmonary disease: comparisons with asthma. J Allergy Clin Immunol. Nov 2003;112(5):819-27; quiz 828.
- Thurlbeck WM. Pathophysiology of chronic obstructive pulmonary disease. Clin Chest Med. Sep 1990;11(3):389-403.
- Thurlbeck WM. Overview of the pathology of pulmonary emphysema in the human. Clin Chest Med. Sep 1983;DA - 19840127(3):337-50.
- Tsoumakidou M, Siafakas NM. Novel insights into the aetiology and pathophysiology of increased airway inflammation during COPD exacerbations. Respir Res. May 22 2006;7(1):80.
- Ulrik CS. Efficacy of inhaled salmeterol in the management of smokers with chronic obstructive pulmonary disease: a single centre randomised, double blind, placebo controlled, crossover study. Thorax. Jul 1995;50(7):750-4.
- Vestbo J. Clinical assessment, staging, and epidemiology of chronic obstructive pulmonary disease exacerbations. Proc Am Thorac Soc. May 2006;3(3):252-6.
- Vincken W, van Noord JA, Greefhorst AP. Improved health outcomes in patients with COPD during 1 yr''s treatment with tiotropium. Eur Respir J. Feb 2002;19(2):209-16.
- Weitzenblum E, Sautegeau A, Ehrhart M. Long-term oxygen therapy can reverse the progression of pulmonary hypertension in patients with chronic obstructive pulmonary disease. Am Rev Respir Dis. Apr 1985;131(4):493-8.