Anthrax (Wool Sorter’s Disease): Epidemiology, Pathology, Clinical Manifestations, Diagnosis, Treatment And Prevention
Bacillus Anthracis
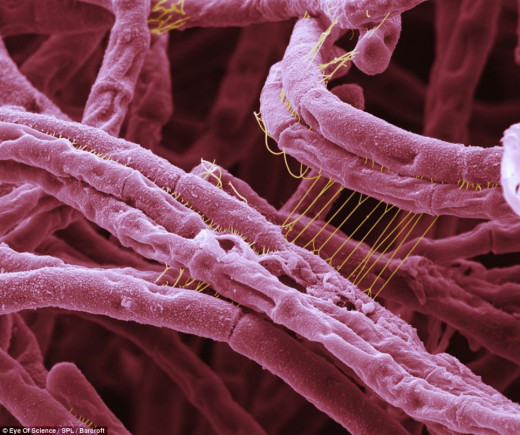
Epidemiology And Pathology Of Anthrax
Anthrax is a disease of animals which is transmitted to man either directly or through infected animal products and caused by Bacillus anthracis. The organism occurs as the bacillus in tissues. They form spores which are resistant to heat and ordinary disinfectants, and can survive for long periods. Spores play the major role in transmission. The organisms produce an exotoxin which causes toxemia and death in severe cases. The toxin can be neutralized by specific antiserum.
Epidemiology: The disease is prevalent throughout the world but only rarely seen in places like India, Ghana, Nigeria and West Africa. Household animals are commonly infected and they form the reservoir. Man acquires the disease while handling infected animals or contaminated wool, hide, hair or other such materials. The common modes of entry of the spores or bacilli are abrasions in the skin, ingestion of infected milk or meat, and inhalation of the spores.
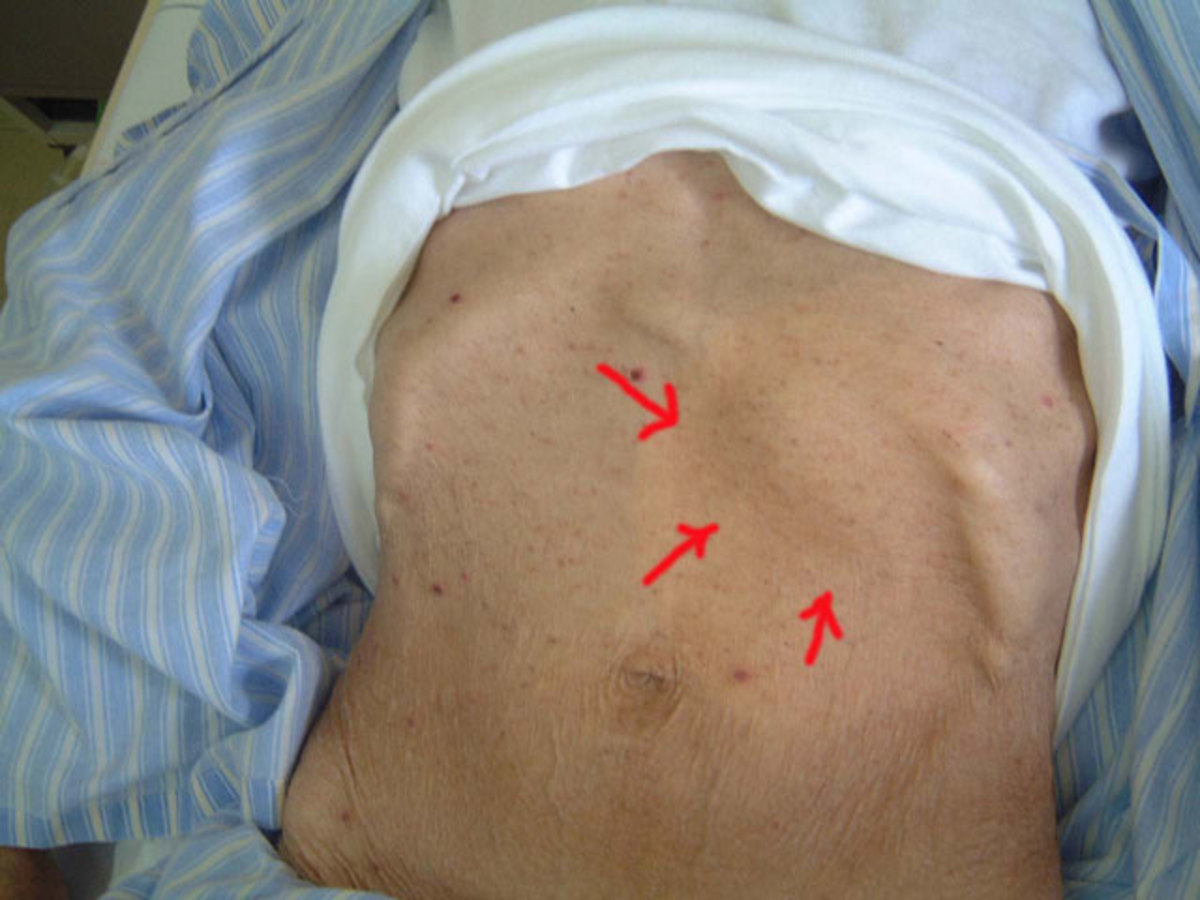
Pathology and pathogenesis: The disease may present as cutaneous anthrax (malignant pustule), pneumonia, meningitis or as the gastrointestinal form. Cutaneous anthrax follows inoculation of anthrax spores which germinate, multiply and produce toxins. This results in hemorrhagic edema, necrosis and infiltration by inflammatory cells. The polypeptide capsule of B. anthracis protects from phagocytosis. The bacillus spreads to the other parts of the body through the regional lymph nodes. At autopsy, the organism can be demonstrated in the blood vessels, lymph nodes and parenchyma of various organs. All affected tissues show hemorrhagic edema. Pneumonia and meningitis may occur. An attack of anthrax generally produces permanent immunity.
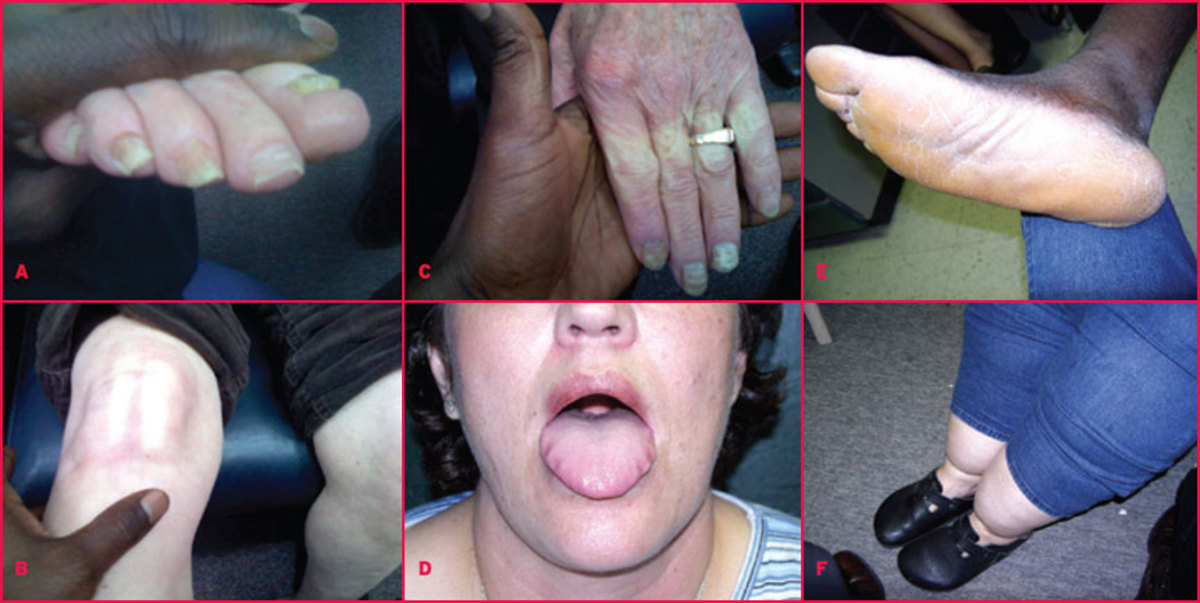
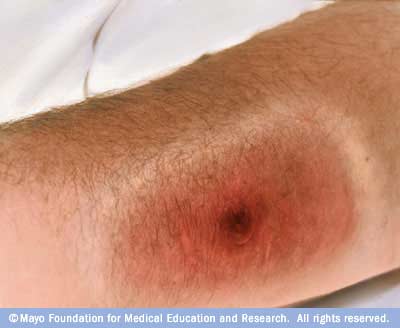
Cutaneous Manifestation Of Anthrax
Clinical Presentations And Diagnosis of Anthrax
Clinical Manifestations
Malignant pustule develops as a small papule after an incubation period of 2 to 5 days. It vesiculates and the vesicle is surrounded by erythema and induration. The vesicle becomes black and an escharis formed with a well demarcated ulcer. The term malignant edema is usef for cutanoue anthrax associated with gross local edema, multiple bullae, induration and systemic illness.
Pulmonary form: Anthrax spores or organisms on entering the respiratory tract produce anthrax pneumonia (wool sorter’s disease). It begins as a mild respiratory infection, but soon the condition worsens. Respiratory distress and cyanosis develop. The sputum is hemorrhagic. Roxemia is severe and death usually occurs within 24 hours.
The gastrointestinal form: This develops 2 to 5 days after ingestion of contaminated meat. It is characterized by fever, nausea, vomiting, abdominal pain, hematemesis and rarely diarrhea. Toxemia may occur.
Meningitic form: Cutanoeus, pneumonic or gastrointestinal anthrax may be complicated by meningitis. The CSF is hemorrhagic. Mortality is very high.
Diagnosis
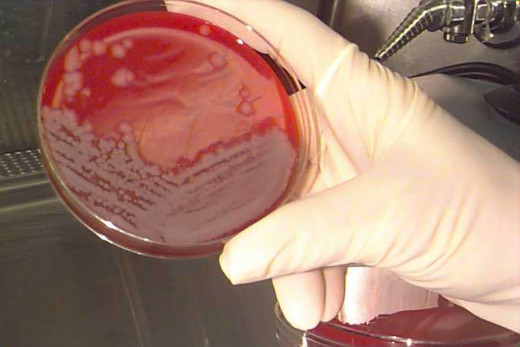
Clinical suspicion is absolutely necessary for early diagnosis. The organism can be demonstrated by Gram- staining of the vesicular fluid. Blood culture may be positive in bacteremic cases. Polymorph leucocytosis is common. Cerebrospinal fluid may be hemorrhagic in anthrax meningitis and the bacilli may be demonstrable. Serum antibody titer can be detected by an agar gel precipitation inhibition test. A four -fold rise in titer confirms the diagnosis.
Differential diagnosis: Anthrax has to be differentiated from other pustular and punched out lesions with gross edema. These include tularemia, lymphogranuloma venereum, catscratch disease, rat bite fever, bubonic plague, glanders and typhus fevers. Marked local induration with pitting edema around the eschar, but without lymphangitis and lymphadenitis are characteristic of cutaneous anthrax. Pulmonary anthrax has to be distinguished from other forms of pneumonia. Anthrax meningitis may be mistaken for subarachnoid hemorrhage but CSF studies are diagnostic and CSF yields causative organism.
The Bacillus Anthracis Culture
Treatment of Anthrax
Penicillin, tetracycline, erythromycin, chloramphenicol and streptomycin are all effective but the drug of choice is penicillin. Penicillin G is given in a dose of 500,000 units every six hours for 5 to 7 days. An alternative drug is tetracycline, 2g per day in 4 divided doses.
Prevention: The disease can be prevented in those at risk by proper health education and surveillance. A vaccine prepared from Bacillus anthracis containing the alum precipitated toxoid is available to protect susceptible people. The course consists of 3 injections given intramuscularly at 6 weeks and 6 months intervals. Booster doses are required annually.
© 2014 Funom Theophilus Makama