Are Patients Being Over-Diagnosed?
Your Health Care Choices

What's Wrong With Me?
When a patient goes to a doctor with an ailment, they expect a diagnosis and treatment. Many patients feel the doctor has not done his job if they do not walk out his office door with a prescription in their hand or know that one was phoned in to their pharmacy.
Because the patient's expectations are high, doctors, on one hand, feel pressured to oblige, and on the other hand, they are being accused of over-diagnosing patients. Some doctors err on the side of caution, just to be safe, and will write that prescription.
Sometimes there's no diagnosis that can be made during the visit either because the visit is too short to do all the testing involved or because a patient's symptoms could point to any number of diseases or ailments. Most physicians might want to wait until they can study all the test results.
In an era when doctors are sued for malpractice for anything, some doctors cover themselves by ordering a medication that will do the least amount of harm while they wait for test results or while considering other medical options before making a diagnosis.
For many doctors and their patients, it is a "wait and see" game -- waiting for more time to pass or for more symptoms to manifest before a name is put to their ailments.
Once a patient has a name for their disease - preferably a disease they can look up on the internet - they will leave the doctor's office much more at ease than they were when they arrived.
Every illness is not mental, but mental plays a part in every illness.
We want to know what is wrong with us, and we want a name to go with it.
A patient who hears a doctor say "I don't know what is wrong with you," might translate that to mean "He thinks I'm crazy." The patient who leaves the doctor's office with a prescription can still be in some "physical" pain, but the mental knowledge that a prescription will possibly help that pain, makes them leave with a more positive attitude, and sometimes with "less" pain symptoms.
Pick up referrals and prescriptions

Drive-through medicine
Sometimes a patient "knows" what is wrong with them and treats the primary care physician's office like a drive through window, picking up their referral for their next doctor.
Some physicians are swift to oblige and don't mind handing out referrals. Others give a thorough exam and painstakingly document their notes in the patient's chart.
Patients who self-diagnose by asking for referrals without the benefit of indepth consultation or physical examination by their primary doctor run the risk of being mis-diagnosed.
Bringing a laundry list of symptoms to a visit often swamps the physician with too many options so that he feels like he has to order a medication to cover interim time - the time between the date of the tests, the date of the results and start of the treatment plan. This can be an antibiotic, a low dose steroid, a pain medication or a placebo.
While patients are very quick to blame doctors for over-diagnosing, they have to accept part of the blame if they demand instant cures for their symptoms.

Meet My Doctor: The Internet
For most people, the internet has become their first pit stop when they are researching their symptoms. They can get hundreds of instant results and an endless sea of links to click, some of which may even contradict one another.
The internet can give you basic information regarding treatments, procedures, new medications, and even some pointers on how to choose your physician, hospital and insurance plans.
But the internet should never replace your "real" doctor.
Content On Medical Websites
Unless there are medical credentials after someone's name (MD, CRNP, etc), much of the information found on medical websites is written by lay people, government agencies, and special interest groups.
Just like on HubPages, some authors of medical articles are not medical professionals. They are writers supplying content about a particular medical subject that they have researched or have had personal experience.
Where did they get their information?
From the internet.
Are you interested in writing for a medical website?
Many websites allow laypeople to "upload and edit" any type of content to their websites, not just medical content; for example, Parkinson's Foundation, About.com, WikiDoc, most of the Wiki websites, Nature Medicine, Everyday Health, The Lancet, Yahoo Health, MedPage Today, and e-how, just to name a few. These links will lead you to the "guidelines for writers" on each website.
Writing content for medical websites can be quite lucrative. As previously stated, you don't have to be a medical professional; you just have to write like one and follow their guidelines.
How Current Is The Information?
In many cases, internet articles, reviews, testimonials, and non-scientific information are out-of-date. Before using any of the content, you should always be aware of the age of the article. In order to know, look at the website address bar while you are on some of these medical sites. They will either show the document date within the URL address or there might be a copyright or a creation date at the end of an article.
Standard disease and disorder information on websites like WebMD rarely changes from year to year unless there have been new discoveries. Articles are often three or more years behind today's date, with the exception of their "news" sections.
Some website authors think it makes them appear knowledgeable and authoritative if they cram tons of links on their articles so while you are reading, you are bombarded with alot of information. It is hard not to click on links before you finish reading the article.
When links take you to websites other than the one you were reading on, it is the rare reader who finds their way back to finish reading the original article. Websites that are over-saturated with links entice the reader to follow link after link until they are so far afield that they will never find their way back to the original article to finish reading.
Bottom Lines:
- You should never stop researching for more up-to-date information.
- Never take one website's information as gospel, no matter how reputable they are.
- Some knowledge is better than no knowledge, so always educate yourself first.
- Read about your symptoms, possible medications and their side effects - then make an appointment with your physician.
Colon Screening
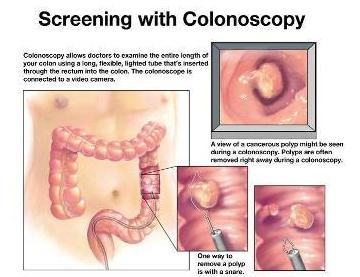
Are screenings important?
Some websites use quizzes as a pre-screening effort, similar to a community hospital's "screening day" where people go for peace of mind, or to "see if" they have disease markers.
In the last ten years, medical professionals say they are seeing more cancers in certain age brackets because they are actively screening for them within those age brackets. What about all the ages that aren't screened? Does the incidence of disease hold true for them?
Do medical tests and screenings lead to over-diagnosis?
Patient chart notes
Once a disease, a disorder or a patient's belief is noted in a patient's medical record, it is very hard to get it removed. It probably wasn't the original intention, but the information influences each doctor who has that patient under their care or each doctor who is called in as a consultant.
A diagnosis can hinder an application for life insurance or when changing medical insurance plan, for example: going from a company based group plan to a non-group medical insurance.
I don't know how many times I've read in a chart that a doctor wrote he suspected the patient had "Disease A" or "Disease B." Every doctor who reads the notes will be influenced by it. No matter what treatment or tests are ordered, the notes in the chart will always be in the back of their mind and could possibly influence how he interprets (or misinterprets) test results. It might go like this:
- One consulting doctor: "The patient has a history of bipolar disorder."
- Second consulting doctor: "Oh yes, now I remember. I read in his chart that he exhibits some paranoia due to ....."
- "Patient wants referrals to go to many specialists to rule out the stated disease."
- "The patient believes she has breast cancer but her labs and her imaging studies are normal."
When a doctor leaves notes of his speculation on a chart, whether it is true or false, it can be a death sentence for the patient.
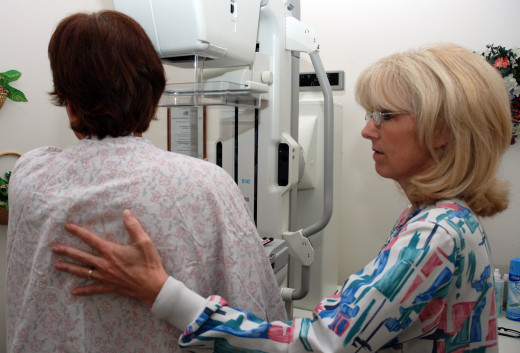
Fear vs diagnosis
Barbara, age 33. Unmarried, no children, resident of Pennsylvania. In relatively good health. Has a history of breast cancer on both sides of her family. Parents are both deceased; no siblings. No health insurance, no primary physician.
May 1999. Barbara found a lump in her left breast. An exam at the free clinic suggested it was a cyst, may be fatty tissue possibly due to her 30 pound weight gain. She somewhat agreed with the doctor's diagnosis because some days when she felt around for it, it wasn't there; other days it felt huge, like a golf ball. She was told the recommended age for a mammogram was age 40 and above, so since she didn't meet the age requirement, the test was not ordered.
January 2000. At her free clinic appointment, Barbara was seen by a different doctor who said he thought the lump was suspicious. After his exam, he said "Yes, I definitely feel a lump." He ordered a medically necessary mammogram and she got an appointment for the next day. Seven months had gone by since she first felt the lump. With all the new attention to the matter, Barbara had worked herself up so badly that she was convinced she had breast cancer.
After the mammogram, she had to wait for the clinic doctor to call her with the results. After the first week of not getting a call, she became two weeks of leaving messages but he never returned her calls. By now, she was a basket case. The next time she called, she was told due to the volume of patients that doctors didn't call patients with test results unless the test showed an abnormality. Barbara accepted that as the reason she hadn't received a phone call.
In March 2000, she started a full time job and became eligible on May 1, 2000 for the company's HMO health plan. She chose a local doctor to be her primary doctor, but couldn't get a "new patient" appointment until June 15, 2000.
Healthwise, things changed for the worse which made it unbearable to wait six weeks for her appointment. Her breast was hot to the touch and painful. She was convinced she had breast cancer. She knew her HMO insurance required a referral from a primary doctor for her to go to a surgeon for a consult. A week after making the appointment, she was beside herself with worry and called the primary's office and was able to get an earlier appointment.
As soon as the doctor entered the exam room, she blurted out that she didn't want to waste his time, she was just there to get a referral to a surgeon to treat her breast lump. She was pretty sure she had breast cancer, she just needed an appointment with a surgeon who could take care of her right away.
He insisted on doing an exam anyway, stating he couldn't give a referral without documenting some patient history. The clinic faxed over her mammogram written report, which was now 6 months old. It stated that the study was unremarkable but he did not have access to the films. After an exam, he said he wanted to try to aspirate the cyst because he felt it was probably full of fluid.
Barbara agreed and 15 minutes later, the thin small needle had a few cc's of clear fluid. He said the lump could hardly be felt now after drawing out the fluid and most likely this was just a benign cyst and nothing to worry about. He said he would send the sample to the lab to be tested. To give her peace of mind, he would order an ultrasound of her breasts, but her insurance had to approve the test first.
In her chart he noted: "patient tolerated fine needle aspiration left lateral breast, producing 1 cc clear fluid and reduction of breast cyst. Pathology report requested. Patient expressed that she was sure her breast lump was cancer. Follow up with bi-lateral breast ultrasound imaging, pending insurance approval, then re-evaluate."
Barbara's HMO would not approve the bi-lateral breast ultrasound because there was not enough medical necessity.
Three months later, Barbara's cyst was back and it was huge. She was scared to death and made a decision that would solve her problem once and for all. She chose another primary doctor. At her first appointment, she immediately asked for a referral to a surgeon. She shared her fears of going through cancer treatments due to her family history, then she told him she wanted a bi-lateral mastectomy because she believed it would reduce her risk of getting cancer.
Based on doctor's notes, patient mental status, family history and two recent mammograms, Barbara's insurance approved surgery for bi-lateral mastectomy.
Surgical summary: Bi-lateral lymph nodes and tissue pathology: no evidence of cancer cells.
Barbara was one month shy of her 35th birthday.
Opinion Poll
Knowing the outcome of Barbara's surgery and her frame of mind, fears, and family history, do you think
Autism

Mental Disorders, ADHD and Autism
Since the beginning of this century, symptoms relating to mental disorders are among the most diagnosed conditions. Patients want doctors to put a name on their symptoms, then they want a medicine to treat it.
That's easier when doctors take lots of time to evaluate or when the diagnosis is obvious, but it is not so easy when a patient pushes for instant results. Whether it is fear of being sued, losing patients, or erring on the side of caution, there are doctors who will write prescriptions or offer free samples for newer drugs they received from drug company representatives in exchange for patient feedback.
Bipolar Disorder (also known as manic depressive disorder or mania depressive disorder) is diagnosed more now in the 2000s than it ever was in the past. That could be due to the change in social attitudes, clearer criteria or better diagnostic tools. Previously, doctors played the waiting game for more symptoms to manifest before making a diagnosis, or prescribing medication and a treatment plan.
In children, an ADHD diagnosis also ranks high as an over-diagnosed condition and with good reason when you consider fast food diets and the distractions children face in everyday life. Since the late 1980s, many parents have taken the initiative to investigate underlying reasons why their children are hyperactive or have attention deficits. When they read about medication side effects, long term dependency and possible organ damage, they decided to tweak diets or create a specialized diet, and use more natural remedies in place of certain prescription medications.
Autism was never diagnosed quickly - partly because the criteria was not yet clear in the 1980s. In fact, my son, who is 29 years old as of this writing (2011), was diagnosed when he was five years old. It took nearly three years to get a definitive diagnosis for him because doctors didn't want to "label" him. However, they were fine with labeling him as ADHD, which turned out to be a misdiagnosis.
To provide input for research purposes, there were doctors who gladly shared the methods and testing procedures they used to make an Autism diagnosis. This meant providing lots of documentation, both to the medical community and to the medical insurance providers who might not have paid for the testing and post-diagnostic services at that time, but the contributions and documentation by those physicians is most of the reason why they pay for it now.
For my son, I had to do my own research to figure out what worked. There weren't many specialists and there were very few books written on the subject. If one was given a drug, it was either Ritalin or Adderall which were given out like candy. I felt he was too young and that his symptoms didn't warrant a little boy taking such hard-core drugs. I studied everything about my son's life, his interactions with family and non-family adults; his playmates and play environments; over-the-counter and prescription medications; food and sleep schedules, then I made small changes, one at a time, in his everyday environment (at home and school) and found ways to reduce the noise and "busy-ness" of his surroundings. At school, life was made easier for parents and staff by putting certain strategies in place that were consistently and successfully used at home, and using educational tools so he could continue to go to school with other children. I wrote his IEPs (Individual Education Plans) because I believe they work best when parents are in control of the content and are educated about the available free services that their child is entitled to, such as a dedicated school vehicle limited to six students to transport to and from school; having the same one-on-one aide assigned each day; and developing a specialized day schedule to promote better school attendance with less disruptions and more interaction.
Today my son is a very high-functioning 29 year old young man. He went to driving school, passed the test and obtained a drivers license. He has a full time job, picked out and made payments to pay for his own 2010 car, manages his checking and savings accounts, selects and writes out his weekly food menus then does the required food shopping. Recently he bought his first house and he is proud owner. As for medications, he takes one pill twice a day for depression. His intake journal of his daily food, vitamins and supplements is still part of his daily routine. He has also continued our practice of using redirection to steer himself away from "bad" or "unhealthy" behaviors, such as cheating on his diet by drinking soda pop or eating gluten or wheat products. Today, he admits he needs at least 75% less redirection than he did 5 years ago and I suspect as he gets older, he will no longer need to use redirection.
When I remember every time I was told to "stop looking for answers and just take him home and love him," and all those specialists who wrote in his chart "patient will never be high-functioning." I sure wish they could see him now.
He is one of the reasons why people should never say the word "never."
Screenings Poll
Do you think Screenings help to identify disease?
Does early diagnosis mean overdiagnosis?
Many doctors say they don't over-diagnose; they make what is called an early diagnosis. Documenting an early diagnosis in a patient's chart is a "cover-my-ass" maneuver which is usually subject to change as more test results come in. Early diagnoses are educated guesses.
Sometimes when a physician suspects a certain disease or disorder early on, while waiting for final test results, he will order a prophylactic medication, which is a "just to be on the safe side" type of medication.
Sometimes it is an antibiotic. But sometimes it is a placebo medication - a sugar pill - when they are afraid the real medication may influence the outcome of certain tests. Remarkably, some patients will say they feel better while taking it and others will say it didn't do a thing for them.
Timing of Tests Per Insurance Guidelines
Our insurance companies hold all the cards when it comes to tests and studies. If a patient has a colonoscopy in 2010 and presents with symptoms where a doctor might want to conduct another colonoscopy in 2011, most insurance companies will not pay for the second one. The rule of thumb is a colonoscopy every 3 years or else the patient has to pay their own expenses.
Because of being outside the time guidelines, those patients will have to endure other tests to get a diagnosis, such as upper and lower GI performed in place of the colonoscopy.
Patients are at the mercy of healthcare insurance companies when it comes to the tests they need in order to get a diagnosis. Each individual insurance company decides what tests and procedures they will pay for, how often and how much they will pay, and how much the patient will pay.
Your Private Information and Insurance Companies
In the case of making an early diagnosis, many patients will pressure a doctor to perform certain tests to "rule out" or to "make sure" that they don't have the disease they suspected they had when they walked into the doctor's office. Other patients blame doctors for ordering tests with high copays they can't afford.
It is true that the schedule of fees are set by the insurance company along with the doctor and/or healthcare facility, and often they are set at a very high rate. That is because the insurance company will only pay them so much of a percentage. When a test has a high fee or copay, it doesn't mean the cost of the test increased. By raising the cost, the doctors and health care institutions will get more compensation. Ultimately it all lies in the hands of the insurance company which tests we are permitted to have, how much they will pay and what our cash outlay will be.
Who Reads Your Medical Information?
You should be very concerned about what a doctor writes in your chart and records. In fact, you should be downright scared.
Whatever a doctor writes in a patient's chart, whether it is an early diagnosis or a suspected diagnosis, you'd be surprised that it's not only your healthcare insurance provider who reads it.
That information includes the history provided by a patient stating if their ailment is due to a prior car accident, listing surgeries and physical or mental diseases, any tests they've had in the past even if it was when they had different insurance coverage or lived in a different state, and how long they have been exhibiting their symptoms.
They can also color the way a "future" medical care provider treats you - personally, medically, and professionally. Even prospective employers have a certain amount of leeway to access what is in your records before deciding to hire you. They do have to show justifiable means as to why they want to see it, but even though we may feel it is none of their business, today it has become so commonplace. Simply stated, there are so many hands in the pot, and we don't know who they are until we are asked to sign a release form so they can request the records and go look.
I know one gentlemen who signed consents for all his past doctors to send his records to his present doctor to keep his records all in one place. He and his wife bought a house and decided to get a life insurance policy so his wife would be able to pay off the house upon his death. When he applied for $250,000 life insurance, he was given a physical exam, then he was asked to sign a consent so they could access his medical records.
Ten days later he received a letter from the insurance company stating he was uninsurable because of the array of medical tests that were performed to "rule out" certain diseases and because his cholesterol was higher than they would like to see it. The only other options he was given was to pay higher premiums in order to get the life insurance coverage he wanted.
Screenings
We hear on the news all the time that early diagnosis via screenings has saved many lives.
Cancer researchers estimate that the number is closer to 1 in 5,000 than the "many lives" we are led to believe, as we see in the video accompanying this article.
Over-diagnosis Poll
Since 2000, do you think people are being over-diagnosed with the new screenings guidelines?
Conclusion
With the high cost of medical care in the United States, many people believe that we are over-screened, over-treated and over-diagnosed.
Part of the blame rests with "screenings" and "preventative" medicine.The age ranges of screening have been changed to "look" for cancers in certain parts of the population who were not screened before.
- Does that mean there is a higher incidence of the disease?
- Or, does that mean the disease was there all along or the decreased sensitivity levels of the screenings are now picking up on it?
Part of the blame rests with the ever changing guidelines skewed to meet the lowered criteria of diseases.
- Many more people fall within the guidelines of a disease, as measured by their test results.
- What we would have considered a mild case 10 to 15 years ago is now a definite disease.
An example: As of January 2011, just 8 months ago, Harvard Medical School lists the standard for a fasting blood sugar at 126 and over.
- That means if your blood glucose measured 126 or more, you are diabetic and you will be prescribed oral medication or perhaps insulin to control your blood sugar. Clicking the Harvard link will show you the illustration.
Failure to take into consideration other blood levels like the metabolic panel and lipids panel, means treating just diabetes and not evaluating the whole picture. If it were, perhaps adjusting thyroid medication or cholesterol dosage would remedy the elevated blood sugar readings.
Steroids and statins use (cholesterol drugs) can also be the reason for a diabetic reading. It's a well known fact among medical professionals that taking statins to control cholesterol raises your blood sugar.
Simply modifying those medications along with diet and lifestyle changes can put off being dependent on insulin for years, if ever.
So, do you think we are over-diagnosed in today's world? Your comments are welcome.
This content is accurate and true to the best of the author’s knowledge and does not substitute for diagnosis, prognosis, treatment, prescription, and/or dietary advice from a licensed health professional. Drugs, supplements, and natural remedies may have dangerous side effects. If pregnant or nursing, consult with a qualified provider on an individual basis. Seek immediate help if you are experiencing a medical emergency.
© 2014 awordlover