- HubPages»
- Health»
- Diet & Weight Loss»
- Weight Loss
How to Reduce Obesity With Stomach Surgery, Bariatric or Weight Loss Bypass Surgery.
Bariatric or weight loss surgery is an operation that is performed on the stomach. It refers to a variety of procedures used to achieve excess weight loss in people who are dangerously overweight and in need of help to reduce obesity.
As the British National Health Service (NHS) consider new ways to reduce obesity, in order to stem the massive pressure on health service, bariatric or weight loss surgery is one of the measure being proposed to help prevent diseases like diabetes, estimated to have cost the the UK £9.8 billion in direct cost, this equates to 10% of the country's budget for England.
The procedures used are categorized by how they work. Weight loss or stomach bypass surgery makes changes to the digestive system, it help to reduce weight by limiting the amount of food intake, resulting in a sense of fullness sooner than before the procedure was performed. It also work by reducing the absorption of nutrients, or in some cases, it can be a combination of both.
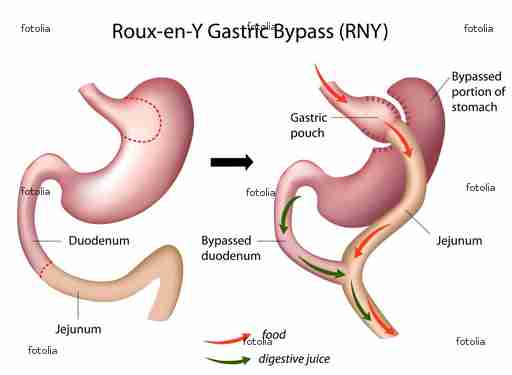
Stomach or gastric Bypass surgery
One of the most common type of bariatric surgery is the gastric bypass surgery; this procedure is the one preferred by most surgeons because it generally has fewer complications when compared to other weight loss surgeries. Gastric bypass surgery on the NHS up by 530% over the past five years, costing 85m a year according to the daily mail, August, 2012.
Gastric Bypass Surgery has two main function, Restriction, where the smaller size of the new stomach restricts the quantity of food intake.
Mal-absorption, part of the digestive system is bypassed, reducing the amount of calories absorbed from the food eaten.
The stomach is made smaller by the use of surgical staples to create a small pouch of 30 to 50 ml from the upper part of the stomach. This new pouch, is connected directly to the middle section of the small intestine, bypassing the rest of the stomach and upper part of the small intestine.
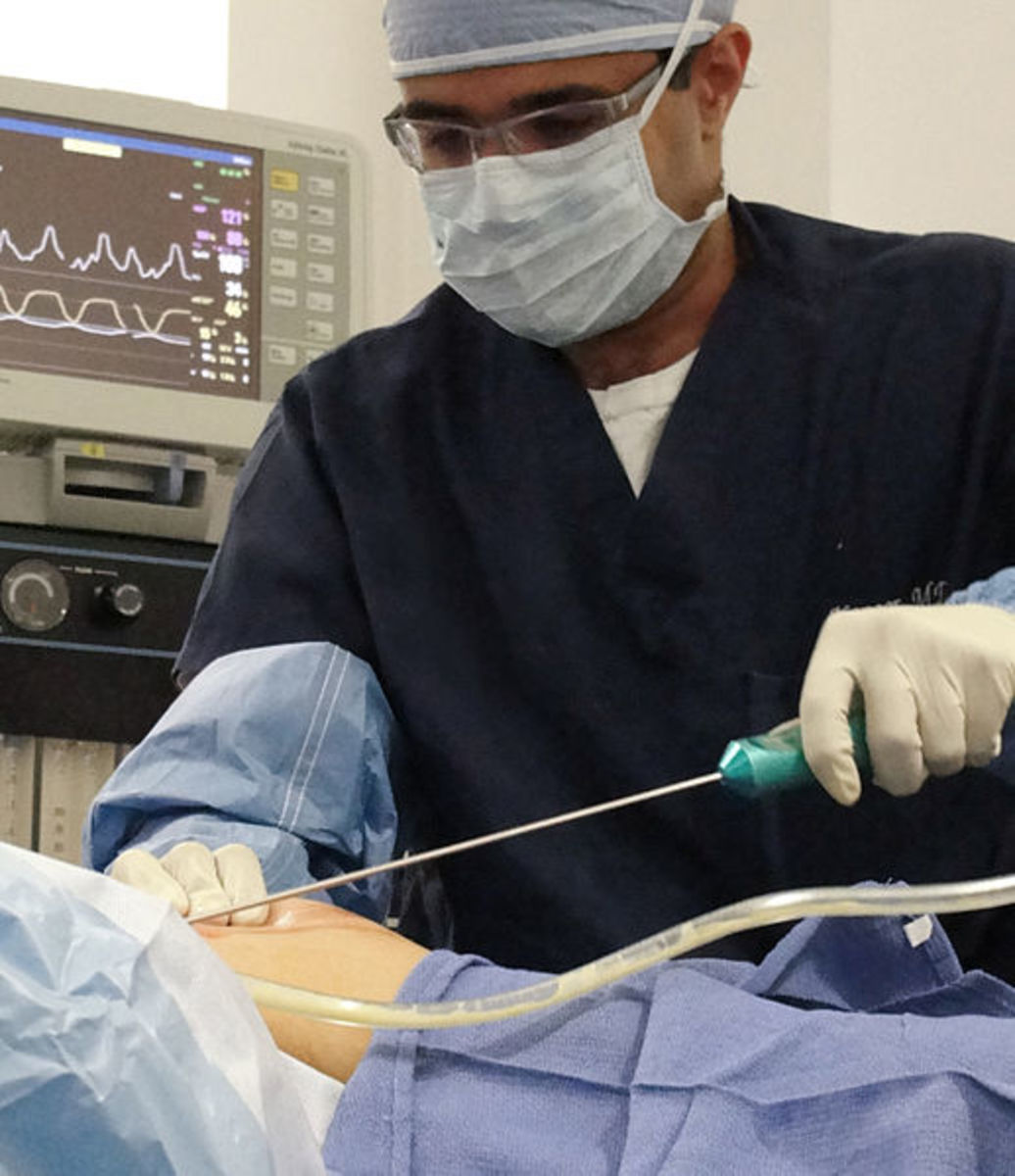
The surgical procedure is performed using laparoscopic or keyhole surgery, a small incision is made with the use of relatively small instruments, which are camera guided. Surgery is performed under full anaesthesia.
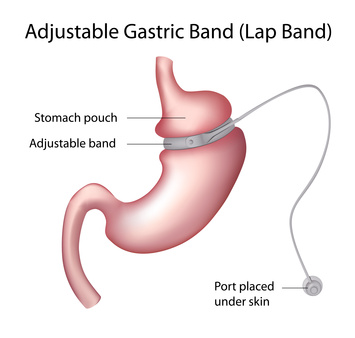
Gastric Band Surgery
Gastric banding or lap banding, are also designed to make the stomach feel fuller after eating small amount of food; it does this, by reducing the capacity of the stomach, allowing it to facilitate weight loss over a period of time.
Gastric banding is appropriate for people who are morbidly obese with a BMI above 40 kg/m 2, or with a BMI between 30 and 40 kg/m 2 and suffer from conditions that poses a serious health risk in people who have tried and failed to lose significant amount of weight conventionally, using diet and exercise.
During this procedure, an adjustable band is placed around the stomach, creating two compartments with a narrow opening between the top and bottom, allowing food to pass through slowly. The limited space left for food, quickly create a sensation of fullness.
The gastric band can be adjusted after the procedure, depending on how much and how fast weight is lost. Fluid can be inserted into the band to tighten it, known as a band fill. After gastric band surgery an overnight hospital stay may be necessary, but generally, this procedure is performed as a day case.
Gastric Sleeve Surgery (Sleeve gastrectomy)
This is more significant than having a gastric band, but it is not considered to be as major as a gastric bypass, it involve fewer changes to the digestive system. The procedure can be performed on its own or as part of a two stage procedure for patient considered to be too high risk for gastric bypass surgery, which can be done once enough weight is lost.
Gastric sleeve surgery involves reducing the size of the stomach, ¾ of the stomach is removed by dividing it. This method effectively reduces the capacity of the stomach without affecting the function. Gastric sleeve surgery can be done either through keyhole surgery or through a conventional operation with an opening in the abdomen. It is performed under a general anaesthetic and usually lasts around 2 hours, hospital stay can be between 1 to 3 days. This procedure differs from gastric band, as it is a permanent reduction in the size of the stomach and is not reversible.
Bariatric surgery is performed as a last resort; only after every effort has been made to reduce weight by eating a healthy calorie controlled balanced diet in conjunction with regular exercise.
In the UK, bariatric surgery is only available through the NHS for those people who are dangerously obese with a potential for developing life threatening conditions and for whom lifestyle changes have not worked.
Obesity
Wikipedia defined obesity as a medical condition in which excess body fat has accumulated to the extent that it may have an adverse effect on health, leading to reduced life expectancy and/or increased health problems. 1.5 million Brits are considered morbidly obese,
Obesity increases the potential for a number of diseases, a person is said to have life threatening obesity when the body mass index (BMI) reaches a level of 40 kg/m 2 or more, or have a BMI of 35 kg/m 2 and above with other serious health conditions that can be improved by losing the excess fat, such as type 2 diabetes, hypertension (high blood pressure), sleep apnoea, certain types of cancer and osteoarthritis
Since not every overweight person is suitable for weight loss surgery, there are alternatives. For people with a BMI of between 27 kg/m 2 and 35 kg/m 2, a gastric balloon insertion may be a suitable option, this procedure is non-surgical, and it must be stressed; losing weight naturally, by controlling the amount of calories and by regular exercise is always the better option, resorting to surgery only when every effort has been exhausted.
Biliopancreatic Division With Duodenal Switch (BPD-DS)
Biliopancreatic division with duodenal switch. (BPD-DS), this procedure is usually done for patients who are severely obese, the procedure is irreversible and is rarely performed. BPD-DS involves the removal of 65% to 70% of the stomach, leaving the pyloric valve intact.The remaining part of the stomach is attached to part of the small intestine. The surgery restricts intake and slow digestion and absorption.
Gatric Balloon- This procedure can also be used in morbidly obese patients who are high risk for anaesthesia and surgery, it allows them to gain a level of weight loss before Bariatric bypass surgery can be attempted.
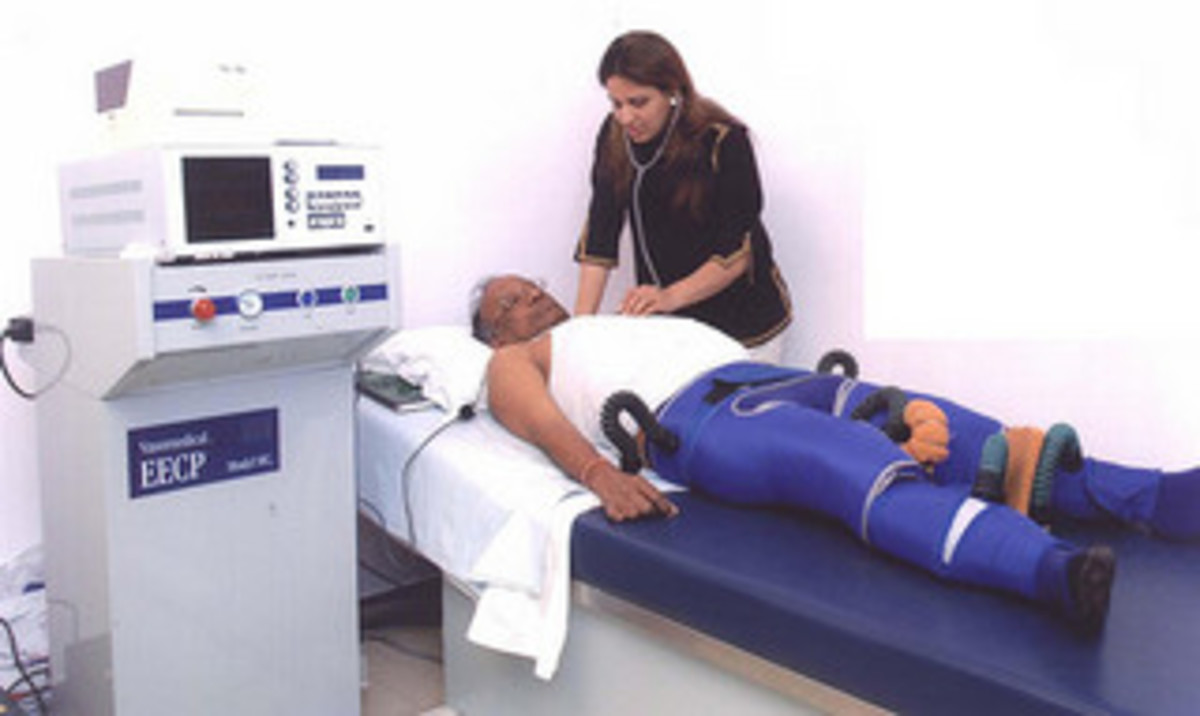
The gastric baloon is inserted into the stomach via the mouth, with the use of an endoscope, (a flexible telescope), the balloon is then partially filled with saline solution, leaving little room for food. The aim is to reduce the feeling of hunger, so that the stomach feels fuller for longer, after eating small meals. This procedure is designed to be a temporary solution to weight loss, and will usually be removed after a six month period. The gastric balloon, also known as intra-gastric balloon, helps to lose weigh without the need for surgery. The procedure is performed under sedation and takes about 20 to 30 minutes, a relatively minor procedure, but needs some time for the stomach to become accustomed to the balloon.
After the procedure, the patient may return home on the same day or following day. In a small number of cases, the stomach is unable to tolerate the balloon for the full six month period, if this occur the balloon may be removed early.
Complications from Bariatric wight loss surgery
Complication from weight loss surgery are frequent and may include:
- Death (1 in 300 patient)
- Complication from anaesthesia
- Pulmonary Embolism
- Bowel Obstruction
- Bleeding
- Nerve problems
- Hypoglycemia (low blood sugar)
- Kidney Problems
- Pneumonia ( rare, < 1% of patients)
- Venous thrombosis (blood clots in the leg)
- Incision infection
- Leak at the staple line
- Ulcer formation where small intestine joins upper part of the stomach, this is uncommon
- Hernia or weakness in incision, this may need to be repair and is less common post laparoscopic surgery
- Stricture or narrowing of the stoma (opening between the stomach and intestine) this is uncommon
- Poor absorption of certain vitamin and minerals post surgery
- Anemia due to iron or vitamin B12 deficiency
- Neurologic complications resulting from B12 deficiency
- Kidney stone disease, due to malabsorption of calcium and oxalate
- Potential bone disease due to mineral or vitamin D deficiency
- Possible dehydration, patients are unable to drink large quantities of fluids at a time after surgery.
- Conversion from laparoscopic (Keyhole) to open abdominal procedure ( 1 in 200 patients)
- Failure of weight loss (about 1 in 10 patient fail to lose adequate weight of 50% or more, of excess body weight after gastric bypass surgery)
- Too much weight loss, rare,
In conclusion; Bariatric or weight loss surgeries are growing in popularity. There were greater than 8000 of these operation performed by the NHS in 2011 with the number rising by around 10% per year. The number of people who are paying for their operation privately is unknown.
Weight loss surgery should never be seen as a quick fix; there are certain risks associated with such procedures, with significant lifestyle changes after surgery.
There should be much consideration before the decision is taken. Most surgeons, whether private or NHS, will recommend that patients attempt to lose weight through diet and exercise before surgery is considered.
Sufficient time and information should be given before surgery, with comprehensive post-op care, and access to dietary and psychological support.