Better Diagnosis and Treatment of Lyme Disease, Part 2: Assessing Credibility
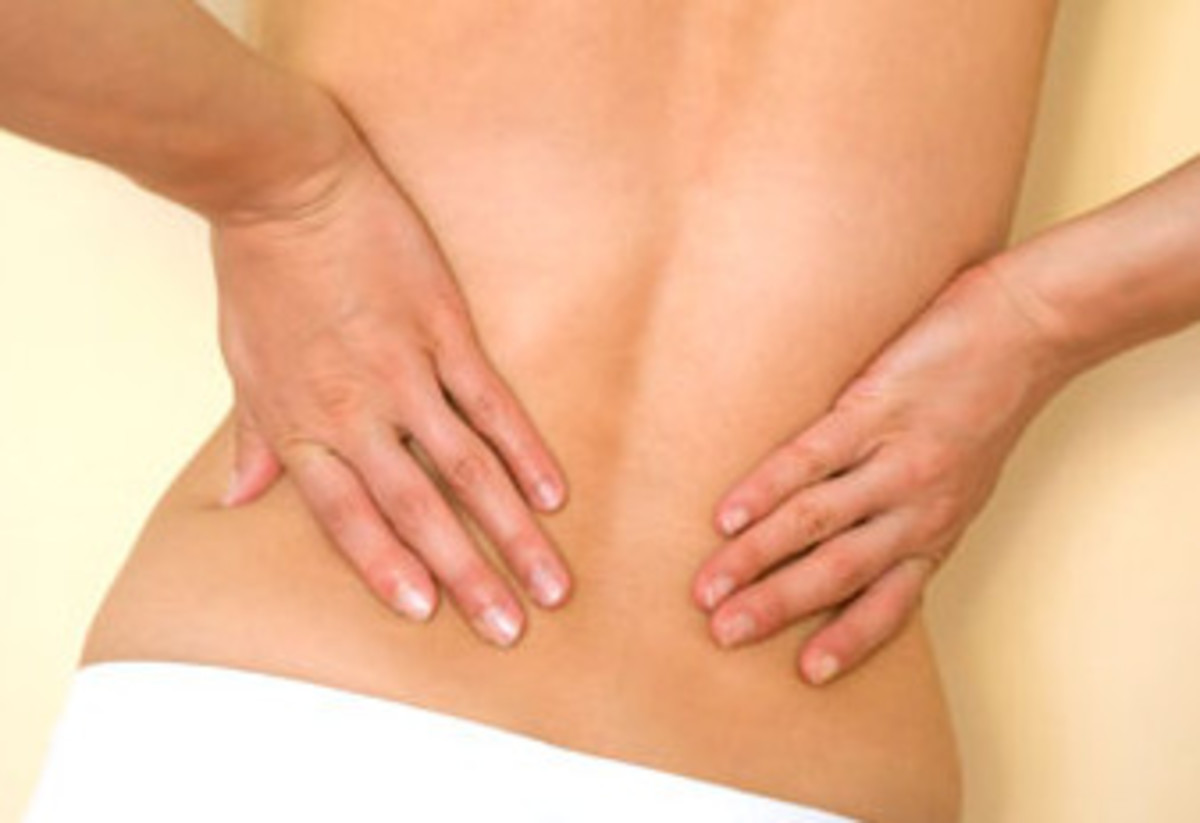
![Clockwise from top left: B. burdorferi. By CDC [Public domain], via Wikimedia Commons; 'Typical' B. burgdorferi spirochete (E) and 'Colony' form (F). By J.Miklossy, S.Kasas, A. Zurn, S, McCall, S.Yu and P. McGeer; B. thieleri. By Alan Walker. Clockwise from top left: B. burdorferi. By CDC [Public domain], via Wikimedia Commons; 'Typical' B. burgdorferi spirochete (E) and 'Colony' form (F). By J.Miklossy, S.Kasas, A. Zurn, S, McCall, S.Yu and P. McGeer; B. thieleri. By Alan Walker.](https://usercontent2.hubstatic.com/11996747_f520.jpg)
The 'purpose and need' for this series arises from dangerous misinformation and pervasive myths that do not give patients or doctors the full view of Lyme Disease.
As described in the first post of this series, there are several major areas of disagreement, especially pertaining to the diagnosis and treatment of Lyme Disease, that have polarized patient groups and medical professionals for decades.
Lyme Politics Versus Lyme Logic
Identifying the politics and problems can sometimes make a given author, patient, or advocacy group sound a bit like a conspiracy theorist. I will admit that since I was unfamiliar with the topic at the time, I actually had at least a tiny bit of this impression the first time I viewed the excellent documentary Under Our Skin. After all, why would infectious disease doctors go to such great lengths to discount patients?
However, it only took a few minutes of digging (after finishing the film) to find that the problematic language highlighted in the film was included in my state's treatment protocols.
As a Biologist, the logic behind the protocols was quite disturbing, and contradicting scientific literature was abundant in medical and other scientific journals.
Scientific Uncertainty and Best Available Science
Several sources I'd trusted during my three years of diagnosis were expressing dangerous and outdated information, and a number of what I considered highly reputable institutions and agencies failed to note any uncertainty or disagreement and failed to include numerous relevant studies and sources in each of the areas I later became aware were controversial.
As a government agency Biologist, I was pretty blown away, since the standards I am held to include discussing all relevant science. If something is not credible or applicable, even that has to be documented. I had previously taken for granted that other agencies, such as the CDC, were subject to the same standards.
Controversies include, but are not limited to, basic science, persistence, diagnosis, and treatment of Lyme Disease.
Obstacles, Dangers, and Impacts...
Regarding Misinformation
This series does not suggest that you should take the word of patients on faith, either, without further review. But in many instances, you will see the questions, problems, uncertainties, and disagreements more clearly in the writings of patients and advocates because they have been personally harmed by the policies and information.
If you aren't aware of the problematic issues, you may not see them identified on medical or agency websites, and won't find triggers or disclosures leading you to compare facts. What you don't know could hurt you by leading to:
- Misdiagnosis
- Accepting inaccurate test results
- Delayed treatment
- Long-term impairment
Regarding Treatment
If you have or suspect Lyme Disease and your symptoms persist beyond initial treatment or if for any reason you are not immediately diagnosed, you will have a very hard time receiving treatment from an insurance-covered, main-stream physician.
There are many layers to this issues and many reasons why this is the case. At the risk of oversimplifying these issues, reasons include:
- Misguided use of surveillance protocols as diagnosis protocols (though not intended for this use);
- Lack of awareness that Lyme is a clinical diagnosis;
- Inadequate and inaccurate laboratory tests;
- Use of two tiered testing system that has not been revisited in twenty years (with a first tier that results in false negatives from 65-85% of the time);
- Widely contested current protocols that limit Lyme treatment and insurance coverage to 28 days;
- The risk of losing medical licenses for applying professional discretion in the treatment of Lyme;
- Prevalent myths and misinformation about Lyme Disease, including erroneous beliefs about distribution and vectors
- Lack of awareness of the infections that often accompany Lyme Disease and can cause treatment to fail if not also effectively identified and treated.
Knowing what to watch for (in terms of misinformation in addition to symptoms) and having a strategy for assessing credibility will help you if you suspect Lyme, ever contract Lyme in the future, or want to be informed about these issues in general, or to be better informed as your state considers mitigating through legislation.
Assessing Credibility ~ Lyme-specific Questions
Typical credentials and reputations don't cut the mustard in assessing who's sharing the whole story on Lyme Disease, and who is aware of the whole picture.
There's no way to fully know the background or biases of a blogger, a Hubber, a journalist, or even an agency or professional medical organization when it comes to this topic.
Considerable skepticism is advised, so please consider a few starting questions and red flags before accepting information on this illness.
Does the source disclose and highlight areas of disagreement?
This may seem like an obvious question, but I did not have a reason to doubt the agency major medical institution information I was reading. I believed what I read and it sounded logical because I didn't know what was being omitted.
I saw hints of disagreement, but missed what I now realize (in the context of ongoing debates) were very disparaging dismissals of concerns without due diligence (meaning full disclosure of the alternate conclusions, evidence, and research, as would typically be required by law from a federal agency with science-based responsibilities and mandates).
If both sides of the issues are not mentioned, be wary. As stated earlier, the fact that there is controversy is indisputable and relevant to note. If not noted, the source is most likely excluding scientific evidence, not just alternate perspectives (examples will be plentiful in following hubs).
Willy Burgdorfer Addresses Controversy (Discovered the Lyme Disease bacterial causal agent; born 1932, died Nov. 17, 2014)
Does the statement really make logical sense?
Remembering the simple tenets of argument papers from high school English, and the basic tenets of science from any level of education will guide you to the enormous logical problems here, once you know where the disagreements lie.
Example: My state "does not have" Lyme because no cases (according to state agencies) have been contracted here, yet doctors are instructed to consider Lyme only if a patient has traveled. Ergo, no cases have been contracted here, and until a case is contracted here, the cases contracted here are not Lyme. I wish I were exaggerating, but here's an example in an editorial from a Montana doctor.
Location of My Tick Bite in 2010
A statement may sound logical, but what's the evidence?
This one often depends on knowing where the controversies lie, because you can't easily know what it is you don't know. But several simple sounding points really warrant better evidence, or in many cases, any evidence, to support them. There may be times when it's available but not provided, but in any other realms of science, it would be.
Example: The lack of Lyme in certain areas is usually predicated on the lack of deer ticks. The first problem with this is that multiple other species such as black flies, sand fleas, mosquitoes, etc. (supported by peer reviewed research, as discussed in detail in later hubs in this series) transmit Lyme Disease to humans.
But, if we assume for the sake of argument that deer ticks are a necessary component of Lyme Disease occurrence, what proves that deer ticks are absent in a given location? Extensive surveys would be required to provide any degree of certainty. Positive occurrences are shown on a CDC map, but survey effort is not displayed. In areas such as my state and surrounding states, the gaps in occurrences are also gaps in survey effort, at least that I can find record of or that entomologists I know are aware of. Survey effort would need to be disclosed in order for that map to indicate (but would not prove) that deer ticks might be absent.
Absence of proof is not proof of absence (a basic tenet of biology, particularly applicable to survey effort). You have no indication of presence or absence if you are not looking.
North Dakota (adjacent to Montana) claimed not to have deer ticks or Lyme Disease, until Entomologists recently looked in 9 locations (a minimal sample size for a state level survey) and found deer ticks carrying Lyme disease at multiple survey locations. When they didn't look, they didn't find it. When they looked, they found it.

What are the author's affiliations?
Agencies tend to quote agencies, but not always. If you become familiar with facts from the CDC (many are grossly inaccurate, but we'll get to that) you will see only these facts reflected on the sites of most medical institutions, infectious disease doctors, most state agencies, and any groups influenced by the Infectious Disease Society of America (IDSA, more on that later as well). Look at citations and note the dates and the relatively small number of citations, for cross reference later with the long lists of better studies from the same time periods as well as the past decade that you will find on sites such as Lymedisease.org and universities that are (independently) studying Lyme Disease.
Similarly, be watchful of groups with names that imply patient affiliations, but facts and members that match CDC and IDSA very precisely, with no mention of controversies or alternate views and no actual evidence of any patient involvement.
Alternately, NIH and some state agencies reflect inadequacies and uncertainties about Lyme testing, diagnosis, treatment and acknowledge research that other agencies do not. I may not agree with some of their conclusions to date, but the higher regard for available science and disclosure of uncertainty give me more confidence in their information.
Researches, Lyme doctors, and Lyme groups that are truly speaking for Lyme patients, in my experience, tend to be pretty up front about the disagreements and uncertainties and tend to pose more questions. They may sound over-zealous, but at least it remains clear that there are alternate views to learn about.

What is the nature of the author's training or direct experience?
You will quickly see that being a doctor does not make one an expert on this topic, particularly in the absence of specific training and direct experience. This can mean research or treating patients, but still apply the above questions to decide, as this is not always enough.
Even personal experiences with Lyme can leave a doctor (or patient, as discussed later) less than fully informed if he or she were treated right away, as they have no personal knowledge of the symptoms, ambiguities, and procedural obstacles many years into this illness.
Lyme Literate Doctors (LLMD's or ND's if naturopaths) are those who are able to see beyond red tape and treat patients adaptively and gain experience and knowledge that usually makes them advocates as well, which shows in what they have to say. Sadly it also leads them to be pursued by the authors of the protocols that keep many patients misdiagnosed, because patient-specific, Lyme-specific treatment can be out of keeping with these protocols.

Additional Purpose and Need For This Series
Numerous medical and agency websites still state a number of misleading things about Lyme Disease that have been extensively refuted by research, which can be dangerous for patients trying to figure out what they have---the misleading information sends a lot people in the wrong direction.
In addition to institutional websites, authors without direct experience of the disease (ranging from bloggers to mainstream media) repeat matching information without knowing (and/or not disclosing adequately) how much disagreement there is, even on just the 'basic' aspects of this disease. One incorrect source can be used across a broad range of websites, much like how rumors spread.
A recent example, for context, has been some misleading articles on Hub Pages from an author new to the Lyme Disease article category. Authors are entitled to their own perspectives, but there is no indication in these popular articles of the enormous debate surrounding these issues. The perspectives shared are counter to most of the articles on Hub Pages, and run counter to the experiences of patient authors here and elsewhere.
Had I read and believed the statements in that Hub prior to diagnosis, I would be gravely misled in ways that would reduce my chances of receiving adequate care.
I listed some of the inconsistencies and troubling statements in Part 1, and will address them in detail in Part 3. But this phenomenon is not isolated to Hub Pages or any venue, so they serve as a good example of the need to assess credibility.
Specific Examples
- The author defines Lyme Disease through the use of surveillance criteria in the place of diagnostic criteria---which the surveillance criteria even state was not their intended use.
- The author states that testing catches 20-30% of cases in the first month and the remaining 70-80% of cases after that. This is not supported in the literature. The first rung of the current two-tiered testing system (the ELISA) has a laboratory-reported false negative rate ranging from 65 to 85% (meaning that up to 85% of infected patients will receive falsely negative results).
Lyme Disease is a clinical diagnosis that a doctor can make based on clinical criteria. The diagnosis is not precluded by lack of laboratory confirmation.
A reader would gain the opposite impression from the recent Hub, as from many articles and websites.
A patient could be dissuaded from pursuing adequate treatment and care.
Hubs and Information To Come
There could be any number of topics needfully covered in this series, but in general, I expect the next few hubs to cover roughly the following (with the expectation that topics and order will adaptively evolve):
Part 1--Introduction to Dangerous Misinformation
Part 2— Assessing Credibility
Part 3— Science Refutes Common Myths
Part 4—Inadequacies of Testing and Interpretation (Intro to "Dearborn" and IDSA)
Part 5—Diversity of Symptoms and Patient Presentation