Cats and Infections Cause Alzheimer’s Disease. Hobbies and Heart Problems help reduce it.
Cats and Alzheimer
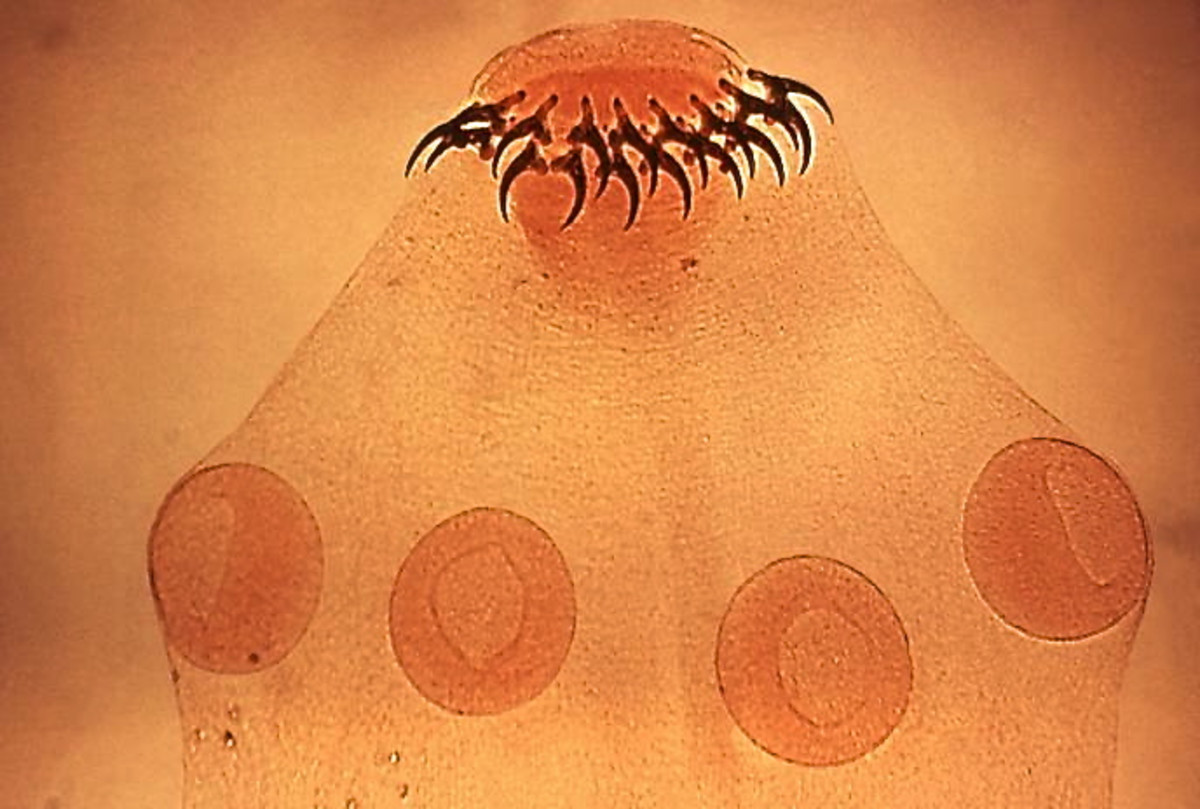
It has been suggested that a parasite carried by cats could cause Alzheimer’s disease. Toxoplasmosa gondii gets into the body from used cat litter and then travels to the brain. Once there it causes chemical changes affecting memory and learning. Up to a third of people in Britain carry the parasite in their bloodstream. The discovery suggests Britain’s ten million cats could in some cases be the source of the incurable illness.
Michael Sukhdeo, editor of the Journal of Parasitology states that it is highly plausible T. gondii may be linked to Alzheimer's disease, 'given that the parasite likes to live in the brain'. T.gondii is considered one of the most prevalent pathogens in the world. The commonly-found parasite inhabits 50 percent of living organisms. It lives inside the intestines of warm-blooded animals, but particularly thrives in cats. Humans can ingest the parasite by eating contaminated meat or water, or coming into contact with cat feces while cleaning out the kitty litter. Therefore having a cat in the yard, instead of your house could be a good solution. Exposure to cat feces can lead to toxoplasmosis, which has devastating effects in people with weakened immune systems. Infected healthy people can experience flu-like symptoms, though many experience no symptoms at all.
White Cat Under Guard of Alzheimer

Hobbies reduce Alzheimer’s risk
People who take part in leisure activities in 40s and 50s are less likely to develop dementia, study says.
People with higher blood pressure are at much lower risk of developing dementia. It is possible that this is because they die younger and it is a race to disease or death.
There is currently no effective treatment for millions suffering from Alzheimer’s and dementia. One U.S. expert said it was “highly plausible” the cat parasite was linked to Alzheimer’s disease. But scientists from Alzheimer’s Research UK have dismissed the Iranian study on mice. They said there was “no evidence” to suggest humans are similarly affected. Dr Rosa Sancho, from Alzheimer’s Research UK, said: “Some research suggests infections in general can ramp up the immune system and contribute to brain damage in Alzheimer’s. “But there is no conclusive evidence a particular infectious agent or parasite is responsible for the disease. “There is no evidence it has a similar effect in people.” Alzheimer’s and dementia affect around 850,000 Brits. And the number is forecast to hit one million in under a decade and two million by 2051. There is no effective treatment, with current medications only help slow down the symptoms.
Infections Cause Alzheimer
Living next to a main road dramatically raises your chance of getting dementia. This is possibly due to infections being more common in reduced immune systems in humans.
Previously, researchers assumed that the protein—beta amyloid—was just a junk molecule that piled up. And efforts to cure Alzheimer’s focused on clearing out clogs and banishing beta amyloid from the brain. But a new study conducted using mice and worms suggests that the protein clumps are actually microbial booby traps, sturdy proteinaceous snares intended to confine invading microbes and protect the brain.
The findings, published in the journal Science Translational Medicine, suggest that Alzheimer’s may result from the brain’s effort to fight off infections. While that hypothesis is controversial and highly speculative at this point, it could dramatically alter the way researchers and doctors work to treat and prevent the degenerative disease.
The findings are “fascinating,” Colin Masters, a neuroscientist at the University of Melbourne in Australia, told Science. But because the study was carried out in mice and worms, the findings are “very contrived in the sense that they don't bear a direct relationship to what we see in the human condition.”.
Still, the findings have many scientists intrigued, and some say they make a lot of sense. For instance, past research had found that people who developed Alzheimer’s had increased levels of antibodies to herpes virus, suggesting past infections. But the idea that herpes caused Alzheimer’s seemed far-fetched, Michael Weiner, an Alzheimer’s disease neuroimaging researcher at the University of California, San Francisco, told the New York Times. He said that the new data provides a plausible explanation as well as being “interesting and provocative.”.
In the study, researchers at Harvard injected a lethal dose of bacteria into the brains of mice genetically engineered to overproduce amyloid beta—a model for studying Alzheimer’s disease—as well as normal mice. Overnight, the Alzheimer’s model mice developed protein plaques similar to those seen in people with the disease. At the center of each plaque was a single bacterial cell. The control mice, on the other hand, didn’t form plaques and died faster.
In worms called Caenorhabditis elegans, another model organism, researchers saw similar results. Extra amyloid in the worms’ guts prolonged their life after infection with bacteria and yeast.
The root cause of Alzheimer’s, a progressive disease that as of 2013 affects some 5 million Americans, is still not completely understood. Researchers know that hallmarks of the disease are tiny balls of plaque that accumulate in Alzheimer’s patients’ brains.
But how and why they form was still pretty much a mystery. Now, researchers at Harvard University, made a surprising finding: Proteins in the brain leftover from fighting off common infections like from a virus or a bacteria, clump together and create the plaque that is ubiquitously found in Alzheimer’s patients. The new research, published yesterday in the journal Science, could pave the way to more precise research on how to stop or prevent the disease.
When infections enter our bodies, our immune systems kick into gear and generate proteins called beta amyloids that encircle the virus or bacterium, killing it and stopping the infection from spreading. Afterwards, the beta amyloid shells that trapped the infection are left and create little balls of plaque.
While this process happens throughout the body, our blood brain barrier attempts to prevent the infections from entering our brains. But in many older people, this barrier becomes leaky, allowing bacteria and other agents into the brain. There beta amyloids fight them off, leaving behind the little balls of plaque--the hallmark of Alzheimer’s disease.
The researchers tested this idea out in neurons grown in a petri dish as well as in mice and fruit flies. First they confirmed that beta amyloid did indeed have a role in fighting off infections. Then, they found that mice without these amyloid proteins succumbed to common infections that could have been fought off. This new finding helps to explain why many people with Alzheimer’s often have more antibodies to the herpes virus, than people without the disease.
But if everyone is constantly bombarded by infections, why do only some people develop Alzheimer’s? Researchers think that some people over produce beta amyloid proteins, making them more likely to develop these plaques. Similarly, some people’s immune systems are better at getting rid of those balls of plaques than others, according to The New York Times. These differences may have to do with having different versions of certain genes already identified in Alzheimer’s, like ApoE4.
The next step, according The Times, is to study the brains of people with and without the disease, to look for microbes found in plaque. Once researchers better understand how and why the plaque is remaining in the brain, they might be able to find ways to prevent it.
/ Science Translational Medicine The beta amyloid proteins capturing the Candida albicans infection in a petri dish. The root cause of Alzheimer’s, a progressive disease that as of 2013 affects some 5 million Americans, is still not completely understood. Researchers know that hallmarks of the disease are tiny balls of plaque that accumulate in Alzheimer’s patients’ brains. But how and why they form was still pretty much a mystery. Now, researchers at Harvard University, made a surprising finding: Proteins in the brain leftover from fighting off common infections like from a virus or a bacteria, clump together and create the plaque that is ubiquitously found in Alzheimer’s patients. The new research, published yesterday in the journal Science, could pave the way to more precise research on how to stop or prevent the disease. When infections enter our bodies, our immune systems kick into gear and generate proteins called beta amyloids that encircle the virus or bacterium, killing it and stopping the infection from spreading. Afterwards, the beta amyloid shells that trapped the infection are left and create little balls of plaque. While this process happens throughout the body, our blood brain barrier attempts to prevent the infections from entering our brains. But in many older people, this barrier becomes leaky, allowing bacteria and other agents into the brain. There beta amyloids fight them off, leaving behind the little balls of plaque--the hallmark of Alzheimer’s disease. Researchers think it’s this process, of fighting off common infections, that could be causing Alzheimer’s. The researchers tested this idea out in neurons grown in a petri dish as well as in mice and fruit flies. First they confirmed that beta amyloid did indeed have a role in fighting off infections. Then, they found that mice without these amyloid proteins succumbed to common infections that could have been fought off. This new finding helps to explain why many people with Alzheimer’s often have more antibodies to the herpes virus, than people without the disease. But if everyone is constantly bombarded by infections, why do only some people develop Alzheimer’s? Researchers think that some people over produce beta amyloid proteins, making them more likely to develop these plaques. Similarly, some people’s immune systems are better at getting rid of those balls of plaques than others, according to The New York Times. These differences may have to do with having different versions of certain genes already identified in Alzheimer’s, like ApoE4. The next step, according The Times, is to study the brains of people with and without the disease, to look for microbes found in plaque. Once researchers better understand how and why the plaque is remaining in the brain, they might be able to find ways to prevent it.
The root cause of Alzheimer’s, a progressive disease that as of 2013 affects some 5 million Americans, is still not completely understood. Researchers know that hallmarks of the disease are tiny balls of plaque that accumulate in Alzheimer’s patients’ brains. But how and why they form was still pretty much a mystery. Now, researchers at Harvard University, made a surprising finding: Proteins in the brain leftover from fighting off common infections like from a virus or a bacteria, clump together and create the plaque that is ubiquitously found in Alzheimer’s patients. The new research, published yesterday in the journal Science, could pave the way to more precise research on how to stop or prevent the disease. When infections enter our bodies, our immune systems kick into gear and generate proteins called beta amyloids that encircle the virus or bacterium, killing it and stopping the infection from spreading. Afterwards, the beta amyloid shells that trapped the infection are left and create little balls of plaque. While this process happens throughout the body, our blood brain barrier attempts to prevent the infections from entering our brains. But in many older people, this barrier becomes leaky, allowing bacteria and other agents into the brain. There beta amyloids fight them off, leaving behind the little balls of plaque--the hallmark of Alzheimer’s disease. Researchers think it’s this process, of fighting off common infections, that could be causing Alzheimer’s. The researchers tested this idea out in neurons grown in a petri dish as well as in mice and fruit flies. First they confirmed that beta amyloid did indeed have a role in fighting off infections. Then, they found that mice without these amyloid proteins succumbed to common infections that could have been fought off. This new finding helps to explain why many people with Alzheimer’s often have more antibodies to the herpes virus, than people without the disease. But if everyone is constantly bombarded by infections, why do only some people develop Alzheimer’s? Researchers think that some people over produce beta amyloid proteins, making them more likely to develop these plaques. Similarly, some people’s immune systems are better at getting rid of those balls of plaques than others, according to The New York Times. These differences may have to do with having different versions of certain genes already identified in Alzheimer’s, like ApoE4. The next step, according The Times, is to study the brains of people with and without the disease, to look for microbes found in plaque. Once researchers better understand how and why the plaque is remaining in the brain, they might be able to find ways to prevent it.
Do you have a cat?
Do you have a cat?
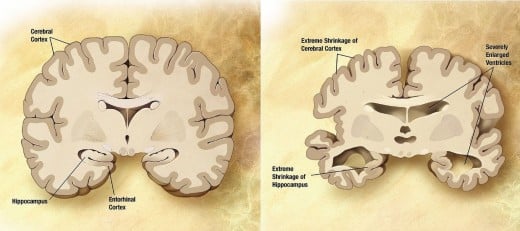
Two brains.
References
Alzheimer's Disease May Result From Past Brain Infections. (2017). Retrieved on April 12, 2017, from http://articles.mercola.com/sites/articles/archive/2016/06/09/alzheimers-disease-brain-infection.aspx.
Brain infections may spark Alzheimer's, new study suggests | Ars .... (2017). Retrieved on April 12, 2017, from http://arstechnica.com/science/2016/05/brain-infections-may-spark-alzheimers-new-study-suggests/.
Common Infections Might Be Causing Alzheimer's Disease | Popular .... (2017). Retrieved on April 12, 2017, from http://www.popsci.com/common-infections-might-be-causing-alzheimers-disease-study-suggests.
CAT's poop could give you Alzheimer's, warn scientists | Daily Mail (2017). Retrieved on April 12, 2017, from http://www.dailymail.co.uk/health/article-4156708/Could-CAT-s-poop-Alzheimer-s.html.
The Link Between Alzheimer's, Cinnamon, and Vitamins. (2017). Retrieved on April 12, 2017, from http://articles.mercola.com/sites/articles/archive/2013/06/13/alzheimers-dementia-treatment.aspx.
UK's ten million moggies could be source of Alzheimer's disease as .... (2017). Retrieved on April 12, 2017, from https://www.thesun.co.uk/living/2707597/uks-ten-million-moggies-could-be-source-of-alzheimers-disease-as-scientists-find-link-between-cat-litter-and-the-incurable-illness/.