Causes and Treatment of Diabetic Retinopathy
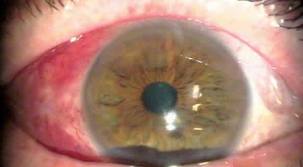
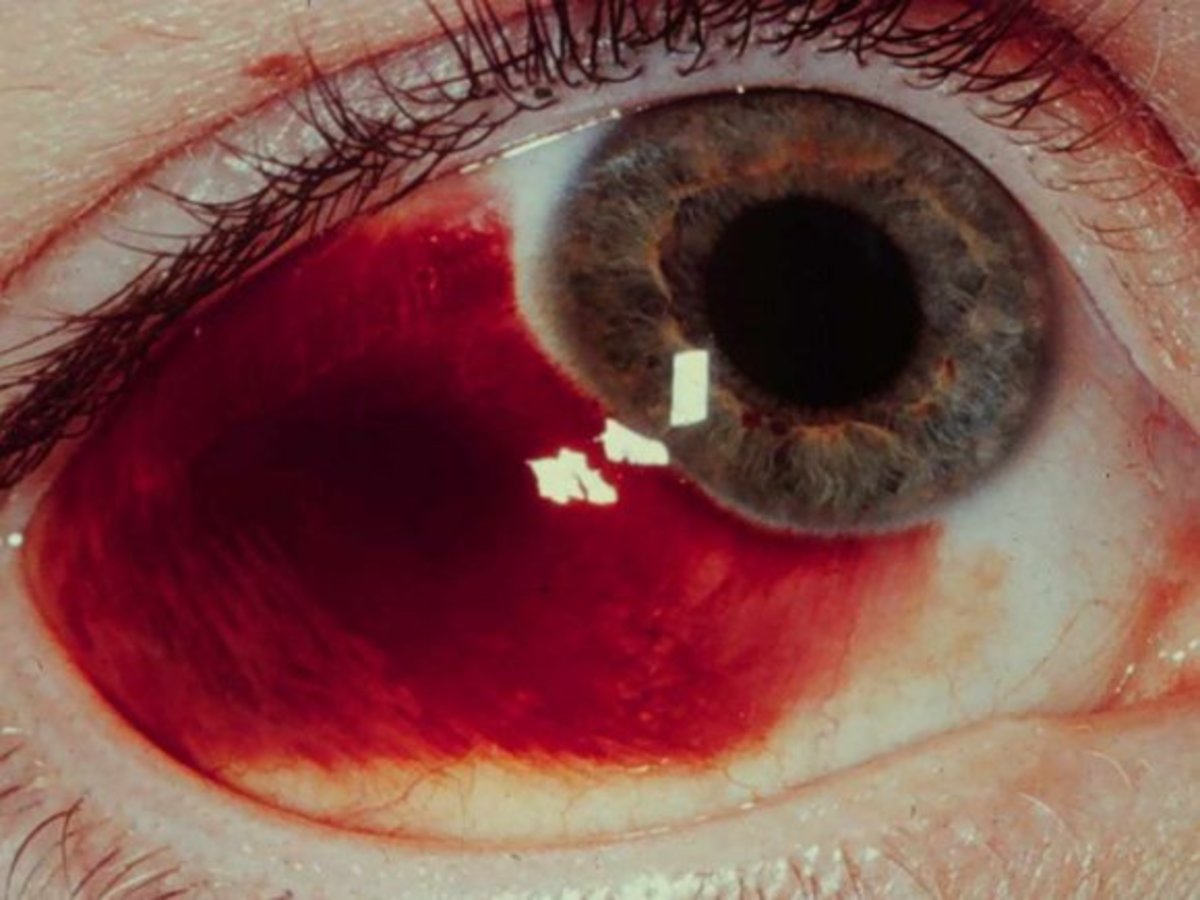
Diabetic retinopathy is characterized by deterioration of the blood vessels in the retina of each eye. Almost all people with diabetes have signs of retinal damage after living nearly 20 years with this disease.
Capillary endothelial cells are not regulated by pericytes (cells surrounding the capillaries) and will become larger and larger; there is also a basal membrane, which is 3 times thicker than normal. So there is a breakdown in the blood-retina, resulting in an alteration of endothelial junctions.
Causes
Retinopathy is usually a sign of another condition. Although many medical disorders (e.g., sickle cell anemia, lupus) can cause retinopathy, its presence is most often caused by diabetes or hypertension (high blood pressure).
Diabetic retinopathy is a complication of diabetes. Diabetes is characterized by high levels of blood sugar can damage blood vessels. The retinal vessels may lose damaged proteins and fatty acids that form deposits and eventually interfere with vision.
Hypertensive retinopathy is a complication of hypertension and usually develops over several years. High blood pressure damages blood vessels swell and contract under the influence. The blood supply to the retina is reduced and damage occurs. The blood filtration may possibly occur in the retina and cause further damage.
Symptoms and Complications
You may be able to observe any symptoms during the early stage of diabetic retinopathy. As the disease progresses, symptoms include:
Blurred vision.
Fluctuations of vision.
Blind spots.
A change in color perception.
Sudden vision loss.
Double vision.
Eye pain in more advanced cases.
A more advanced form of diabetic retinopathy, proliferative diabetic retinopathy call can lead to scarring responsible for a decrease of vision. In patients with proliferative retinopathy, new blood vessels grow on the retina and vitreous (the sticky substance between the lens and the retina). These blood vessels may swell and burst, thus causing bleeding eye damage. In some cases, blood is reabsorbed, but often separates the retina and cause blindness
Diagnosis
Diabetic retinopathy is a long-term complication of diabetes. It is imperative that a person with diabetes examines your eyes regularly, as recommended by an ophthalmologist.
The diagnosis of diabetic retinopathy and hypertensive retinopathy is approximately the same. An ophthalmologist examines the retina with an ophthalmoscope, which shines a bright light on the back of the eye. The ophthalmologist looks for signs of blood vessel dilation and micro aneurysms. The ophthalmologist also can use fluorescein angiography. A test that requires the injection of a dye into a vein in the arm before taking a series of images of the retina that detect signs of bleeding blood vessels. This technique allows us to identify the areas of the retina that bleed easily.
In the case of the hypertensive retinopathy, ophthalmologist look for small plaques cholesterol content in the blood vessels of the retina, and changes that cause thickening and narrowing.
Treatments and Prevention
The key to the treatment of retinopathy is the management of the underlying causes of this disorder.
Balancing blood sugar in a person with diabetes is critical in delaying the onset of diabetic retinopathy. Good control of diabetes is taking prescribed medication, either insulin or other antidiabetic agents, and adopts a healthy diet and exercise program.
The blood pressure control helps prevent hypertensive retinopathy. Appropriate medications reduce high blood pressure and help prevent complications. The regular practice of physical exercise, diet and other appropriate changes in lifestyle, such as quitting smoking, significantly reduce the risk of retinopathy.
Today, many retinal problems can be treated with laser. The scatter laser treatment is used for treating proliferative diabetic retinopathy. The objective is to create 1000 - 2000 retinal burns with the hope of reducing the oxygen demand of the retina, and therefore the possibility of ischemia. In the treatment of advanced diabetic retinopathy, burns are used to destroy abnormal blood vessels of the retina. This has been shown to reduce the risk of severe vision loss in eyes with risk of 50%.
The ophthalmologist dilates the pupil and applies anesthetic drops to numb the eye. During the procedure, the patient may see flashes of light. These flashes eventually may create a tingling uncomfortable for the patient. After laser treatment, patients are advised not to drive for a few hours when pupils are still dilated. Vision may be a little blurry for the rest of the day, but the eye irritation is mild
Your doctor may be of the opinion that vitrectomy is necessary if there has been a flow of blood in the vitreous and scar tissue that has formed. This procedure involves removing a portion of the vitreous body and scar tissue. Early vitrectomy is especially effective in people with diabetes mellitus, which may have an increased risk of blindness due to bleeding in the eye. Vitrectomy is often done under local anesthesia.
The doctor makes a small incision in the sclera or white of the eye. Then, a small instrument is placed in the eye to remove vitreous and insert into the eye saline. Patients can go home soon after the vitrectomy, or may be asked to stay in hospital overnight. After surgery, the eye will be red and sensitive, and patients often need to wear an eye patch for a few days or weeks to protect your eyes. Medicated eye drops are also prescribed to prevent infection.
The treatment against hypertensive retinopathy includes drugs that stabilize blood pressure, laser treatment, and sometimes the injection of drugs into the eye (e.g. Corticosteroids). , But prevention is the key to this disorder.
In patients with proliferative retinopathy, you should consult your doctor before starting any strenuous exercise because they may increase the pressure on the blood vessels of the eye and cause bleeding.